The Leptin-to-Adiponectin Ratio in Inflammation
Jamie Rausch PhD11, Kaitlyn Horne BSN1, Jodi C McDaniel2
1Indiana University Fort Wayne, School of Nursing, USA
2Ohio State University, College of Nursing, USA
Submission: May 3, 2024; Published: May 15, 2024
*Corresponding author: Jamie Rausch RN, Indiana University Fort Wayne, School of Nursing, Indiana, USA
How to cite this article: Jamie Rausch PhD, Kaitlyn Horne BSN, Jodi C McDaniel. The Leptin-to-Adiponectin Ratio in Inflammation. Curre Res Diabetes & Obes J 2023; 17(3): 555964.DOI: 10.19080/CRDOJ.2023.17.555964
Abstract
Leptin and adiponectin are adipokines that have been shown to mediate the relationship between systemic inflammation and chronic diseases. However, the inconsistent reporting of leptin and adiponectin data by previous studies hinders the pooling of data across studies for cross-population comparisons or meta-analyses. As such, the aims of this brief are to (1) encourage researchers in the area of systemic inflammation to include standardized measures of leptin and adiponectin and the leptin to adiponectin ratio in future studies, and (2) recommend standardized reporting methods. Following standardized measurement and reporting methods will increase the likelihood that new data generated can be compared across studies and thus, knowledge about the impact of these adipokines on inflammation regulation can be advanced.
Keywords: Leptin; Adiponectin; Adipokines; Inflammation; Human studies
Abbreviation: CRP: C-Reactive Protein; LAR: Leptin-to-Adiponectin Ratio; TNF: Tumor Necrosis Factor; IL: Interleukin; ALR: Adiponectin-to-Leptin Ratio. EIA: Enzyme Immunometric Assay; ELISA: Enzyme Linked Immunoassay; IFMA: Immuno Flouro Metric Assay; QIA: Quantikine immunoassay; RIA: Radioimmunoassay
Introduction
Chronic systemic inflammation is associated with an increased risk for and a more rapid progression of multiple chronic diseases, including cardiovascular disease, diabetes mellitus, and kidney disease [1-6]. Identifying biomarkers and molecular contributors of chronic systemic inflammation early in its course may allow for earlier implementation of efficacious treatments, to prevent tissue and system damage, and thus reduce long-term disease ramifications [3]. Currently, the acute phase inflammatory biomarker c-reactive protein (CRP) is used in research and clinical practice [7-10] to help predict chronic disease and to guide treatment [11]. However, multiple factors, including certain medications, nutritional supplements, and acute injuries can cause CRP levels to be highly variable and unreliable [12].
Leptin and adiponectin are adipokines (hormones) made and released from adipose tissue that are involved in inflammation regulation. For example, leptin can activate various signal transduction cascades that result in the release of a host of other inflammatory mediators [13]. Leptin has been shown to have mostly pro-inflammatory actions, including up-regulating CRP, while adiponectin has been shown to have primarily anti- inflammatory actions, including down-regulating CRP [14-20]. Therefore, leptin and adiponectin are inflammatory biomarkers that may be more sensitive than CRP for detecting inflammatory status in clinical and research settings. Moreover, some studies have shown that the leptin-to-adiponectin ratio (LAR) has a higher diagnostic accuracy in detecting an inflammatory profile than leptin or adiponectin alone [21-24]. As such, the purpose of this brief report is to emphasize the importance of standardized assessment and reporting of leptin, adiponectin, and the LAR in future studies to facilitate more accurate comparisons across studies and data synthesis.
Background
Leptin and adiponectin are hormones made and released by adipocytes in adipose tissue that current literature describes as being mediators of inflammation and influencers of chronic diseases [25-29]. Leptin and adiponectin can be detected in tissue samples [30] however, they are most frequently measured in blood samples for clinical studies [29,31]. The proinflammatory actions of leptin are varied and include 1) inducing monocytes and macrophages to synthesize eicosanoids, 2) triggering of natural killer cell cytotoxicity, 3) stimulating chemotaxis in neutrophils, 4) activating proinflammatory cytokine production in B cells, and 5) promoting Th1-cell immune responses (Th1 cells secrete tumor necrosis factor (TNF)-α, lymphotoxin, and interleukin (IL)-2) [19,32-35]. Conversely, the anti-inflammatory actions of adiponectin include inhibiting the production of proinflammatory cytokines, such as TNF-α and IL-6 by some immune cells (e.g., monocytes) [14,15,19,36,37]. Additionally, some studies report that adiponectin promotes the production of anti-inflammatory cytokines such as IL-10 [38,39].
The LAR has recently been identified as an important indicator of the collective actions of leptin and adiponectin and thus may be a more accurate biomarker of systemic inflammation than leptin or adiponectin alone [36,40,41]. While higher LARs have been shown to signify greater systemic inflammation and lower LARs have been shown to indicate less systemic inflammation [42,43], reference values have not yet been established.
Reporting Issues and Recommendations
There are several issues regarding the reporting of leptin and adiponectin in clinical trials. First, clinical studies assessing systemic inflammation often omit leptin and adiponectin as outcome measures or measures only one of these biomarkers [44-47]. A recent systematic review indicated that not only is the omission of these adipokines in clinical studies a concern, but in the majority of studies that quantified leptin and adiponectin, the LAR was not reported and therefore was not included in the analyses.[29] We recommend including leptin, adiponectin, and the LAR as outcome measures of inflammation in future studies focusing on the causes and treatments of chronic systemic inflammation.
Second, although leptin and adiponectin data, similar to other biomarker data, are often skewed and analyzed on a transformed scale, [48] a systematic review found that studies rarely included a description of the data transformation technique that was used [29]. Not knowing the data transformation technique used can make it difficult to compare results across studies and to pool data for meta-analyses. We recommend a standardized data transformation technique that involves a two-step process to normalize skewed data [49]. Transforming the variable into a percentile rank that results in a uniform distribution is step one. In the second step, step one results are modified using an inversenormal transformation, guided by the mean and standard error of the original variable. This two-step process will transform any data set to a normal distribution with the same mean and standard error of the original data [49].
Third, there is variability in the unit of measurement of leptin and/or adiponectin reported by previous studies. Although the most frequently used measurement unit for leptin reported by previous studies is ng/ml, [24,50-53], mcg/l, [54] and pg/ml have been reported by other studies [55]. Similarly, the most commonly used measurement unit for adiponectin is mcg/ml, [24,45-47,50- 54,56], however ng/ml, [57,58] mg/ml, [59,60] pg/ml, [55] and mg/L have also been used [44,61]. We recommend that the standardized measurement unit for leptin be ng/ml and the mcg/ ml should be used for adiponectin. given that they have been the reporting units most frequently used by previous studies.
Fourth, some previous studies including leptin and adiponectin assessments have reported the adiponectin-to-leptin ratio (ALR), [62,63] while others have reported the LAR [41,42,64-66]. We recommend using the more commonly reported LAR versus the ALR. High levels of the ALR indicate less inflammation, while high levels of the LAR indicate more inflammation. Using LAR, instead of ALR, would allow for the natural association of values being indicative of a higher pro-inflammatory status. When the LAR is reported, it is often calculated by dividing leptin (ng/ml) by adiponectin (mcg/ml) [24,31]. We recommend continuing this practice in future studies.
Methods used for Measuring Leptin and Adiponectin
Information was taken from a systematic review by Rausch et al. (2020) with author approval [29]. Leptin and adiponectin have been measured using various methods. The 31 studies included in the systematic review reported the following methods for reporting leptin and adiponectin.[29] Several studies did not report the methods used for measuring leptin and adiponectin [29]. Moreover, it is unclear how much variation occurs between the different methods used.
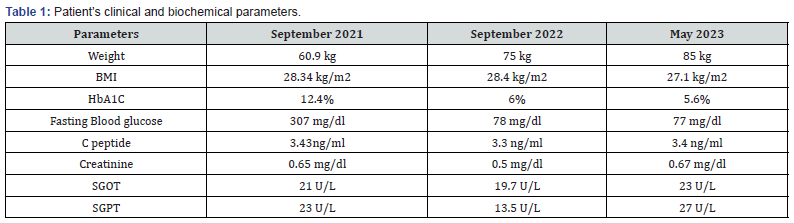
Fifth, complicating the ability to accurately compare levels of leptin and adiponectin across human studies is that the methods used to quantify these adipokines in previous studies have varied widely [29] Table 1. Given that it is still unclear if all methods for quantifying leptin and adiponectin yield similar results, additional studies are needed to make this determination.
Finally, various previous human studies have measured leptin and adiponectin in plasma/serum, saliva, hair, and/or urine [30,31,64-74]. There may be methods that would allow the comparison of levels of leptin and adiponectin across sample types, but additional studies are needed to explore this possibility. Using non-invasive methods to collect samples from sources other than blood to quantify leptin and adiponectin would allow researchers to analyze data from very young participants and compare them to other age groups. Moreover, parents may be more inclined to allow their children to participate in research studying inflammation across the lifespan if noninvasive methods for sample collection were used.
Conclusion
Taken together, to improve the accuracy of comparing leptin and adiponectin data across human studies, we recommend researchers investigating systemic inflammation consider including leptin, adiponectin, and the LAR as outcome variables in future studies, use a standardized transformation technique for skewed data (and report same), and report leptin and adiponectin data in standardized measurement units. Over the last 20+ years, information about how leptin and adiponectin influence inflammation regulation has increased. Yet, there is still much to be learned about how to use these important adipokines to guide disease diagnostics and treatment.
Financial Support
The authors received no financial support for the research, authorship, and/or publication of this article.
Author Contributions
JR conceived the presented idea and wrote the manuscript. JM, and KH gave substantial feedback and assisted in manuscript writing and reviewing.
Conflict of Interest
The authors declare there are no conflicts of interest.
References
- Furman D, Campisi J, Verdin E, Pedro CB, Sasha T, et al. (2019) Chronic inflammation in the etiology of disease across the life span. Nat Med 25(12): 1822-1832.
- Tahergorabi Z, Khazaei M, Moodi M, Chamani E (2016) From obesity to cancer: a review on proposed mechanisms. Cell Biochem Funct 34(8): 533-545.
- Franceschi C (2014) Chronic inflammation (inflammaging) and its potential contribution to age-associated diseases. J Gerontol A Biol Sci Med Sci 69(Suppl 1): S4-S9.
- Tabas I, Glass CK (2013) Anti-inflammatory therapy in chronic disease: challenges and opportunities. Sci 339(6116): 166-172.
- Ehlers S, Kaufmann SH (2010) Infection, inflammation, and chronic diseases: consequences of a modern lifestyle. Trends Immunol 31(5): 184-190.
- Garcia-Rio F, Miravitlles M, Soriano JB, Luis M, Enric DT, et al. (2010) Systemic inflammation in chronic obstructive pulmonary disease: a population-based study. Respir Res 11(1): 63.
- Babaei Z, Moslemi D, Parsian H, Khafri S, Pouramir M, et al. (2015) Relationship of obesity with serum concentrations of leptin, CRP and IL-6 in breast cancer survivors. J Egypt Natl Cancer Inst 27(4): 223-229.
- Badimon L, Peña E, Arderiu G, Teresa P, Mark S, et al. (2018) C-Reactive Protein in Atherothrombosis and Angiogenesis. Front Immunol 9: 430.
- Bastard JP, Maachi M, Lagathu C, Min Ji K, Martine C, et al. (2006) Recent advances in the relationship between obesity, inflammation, and insulin resistance. Eur Cytokine Netw 17(1): 4-12.
- Bisoendial RJ, Kastelein JJP, Levels JHM, Jaap JZ, Bas van den B, et al. (2005) Activation of inflammation and coagulation after infusion of C-reactive protein in humans. Circ Res 96(7): 714-716.
- Del Giudice M, Gangestad SW (2018) Rethinking IL-6 and CRP: Why they are more than inflammatory biomarkers, and why it matters. Brain Behav Immun 70: 61-75.
- Nehring SM, Amandeep G, Patel BC (2019) C Reactive Protein (CRP). In: StatPearls. StatPearls Publishing.
- Perrotta F, Scialò F, Mallardo M, Giuseppe S, Vito D, et al. (2023) Adiponectin, Leptin, and Resistin Are Dysregulated in Patients Infected by SARS-CoV-2. Int J Mol Sci 24(2): 1131.
- Ait Eldjoudi D, Cordero Barreal A, Gonzalez-Rodríguez M, et al. (2022) Leptin in Osteoarthritis and Rheumatoid Arthritis: Player or Bystander? Int J Mol Sci 23(5): 2859.
- Najafi A, Mohammadi I, Sadeghi M, Brühl AB, Sadeghi-Bahmani D, et al. (2022) Evaluation of Plasma/Serum Adiponectin (an Anti-Inflammatory Factor) Levels in Adult Patients with Obstructive Sleep Apnea Syndrome: A Systematic Review and Meta-Analysis. Life (Basel) 12(5): 738.
- De Rosa S, Cirillo P, Pacileo M, Di Palma V, Paglia A, et al. (2009) Leptin stimulated C-reactive protein production by human coronary artery endothelial cells. J Vasc Res 46(6): 609-617.
- Hribal ML, Fiorentino TV, Sesti G (2014) Role of C Reactive Protein (CRP) in Leptin Resistance. Curr Pharm Des 20(4): 609-615.
- Singh P, Hoffmann M, Wolk R, Shamsuzzaman ASM, Somers VK (2007) Leptin induces C-reactive protein expression in vascular endothelial cells. Arterioscler Thromb Vasc Biol 27(9): e302-307.
- Fantuzzi, Mazzone (2014) Adipose Tissue and Adipokines in Health and Disease. 2nd Humana Press.
- Ouchi Walsh (2007) Adiponectin as an anti-inflammatory factor. Clin Chim Acta. 380(1): 24-30.
- Sardu C, D’Onofrio N, Torella M, Portoghese M, Loreni F, et al. (2019) Pericoronary fat inflammation and Major Adverse Cardiac Events (MACE) in prediabetic patients with acute myocardial infarction: effects of metformin. Cardiovasc Diabetol 18(1): 126.
- Canas JA, Damaso L, Altomare A, Killen K, Hossain J, Balagopal PB (2012) Insulin resistance and adiposity in relation to serum β-carotene levels. J Pediatr 161(1): 58-64.
- Angın Y, Arslan N, Kuralay F (2014) Leptin-to-adiponectin ratio in obese adolescents with nonalcoholic fatty liver disease. Turk J Pediatr 56(3): 259-266.
- Jacobo-C, Valdés-R, Guadarrama-L, Pardo-M, Martínez-C, et al. (2017) Effect of n-3 Polyunsaturated Fatty Acid Supplementation on Metabolic and Inflammatory Biomarkers in Type 2 Diabetes Mellitus Patients. Nutrients 9(6): 573.
- Andrade-Oliveira V, Câmara NOS, Moraes-Vieira PM (2015) Adipokines as Drug Targets in Diabetes and Underlying Disturbances. J Diabetes Res 2015: 681612.
- Antuna-Puente B, Feve B, Fellahi S, Bastard JP (2008) Adipokines: the missing link between insulin resistance and obesity. Diabetes Metab 34(1): 2-11.
- Gairolla, Kler, Modi, Khurana (2017) Leptin and adiponectin: pathophysiological role and possible therapeutic target of inflammation in ischemic stroke. Rev Neurosci 28(3): 295-306.
- Kwaifa IK, Bahari H, Yong YK, Noor SM (2020) Endothelial Dysfunction in Obesity-Induced Inflammation: Molecular Mechanisms and Clinical Implications. Biomolecules 10(2): 291.
- Rausch J, Gillespie S, Orchard T, Tan A, McDaniel JC (2021) Systematic review of marine-derived omega-3 fatty acid supplementation effects on leptin, adiponectin, and the leptin-to-adiponectin ratio. Nutr Res 85: 135-152.
- Batury VL, Tam FI, Hellerhoff I, Marie LW, Katrin B, et al. (2023) Hair-Based Assessment of Sex Steroid Hormones in Patients with Anorexia Nervosa. Metabolites 13(1): 21.
- Rausch JA, Gillespie S, Orchard T, Tan A, McDaniel JC (2021) Secondary data analysis investigating effects of marine omega-3 fatty acids on circulating levels of leptin and adiponectin in older adults. Prostaglandins Leukot Essent Fatty Acids 170: 102302.
- Abella V, Scotece M, Conde J, Pino J, Angel Gonzalez-Gay A, et al. (2017) Leptin in the interplay of inflammation, metabolism and immune system disorders. Nat Rev Rheumatol 13(2): 100-109.
- Dagogo-Jack (2015) Leptin Regulation and Clinical Applications. Springer International Publishing.
- La Cava (2017) Leptin in inflammation and autoimmunity. Cytokine 98: 51-58.
- Bennett JE, Dolin R, Blaser MJ (2015) Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 8th edition. Elsevier/Saunders.
- Litwack (2012) Adiponectin. Elsevier/Academic Press.
- Scotece M, Conde J, Lopez V, Lago F, Pino J, et al. (2014) Adiponectin and leptin: new targets in inflammation. Basic Clin Pharmacol Toxicol 114(1): 97-102.
- Ganzetti G, Campanati A, Offidani A (2015) Non-alcoholic fatty liver disease and psoriasis: So far, so near. World J Hepatol 7(3): 315-326.
- Wulster-Radcliffe MC, Ajuwon KM, Wang J, Christian JA, Spurlock ME (2004) Adiponectin differentially regulates cytokines in porcine macrophages. Biochem Biophys Res Commun 316(3): 924-929.
- Ayina CNA, Endomba FTA, Mandengue SH, Jean Jacques NN, Laurent Serge EN, et al. (2017) Association of the leptin-to-adiponectin ratio with metabolic syndrome in a sub-Saharan African population. Diabetol Metab Syndr 9: 66.
- Golbahar J, Das NM, Al-Ayadhi M, Gumaa K (2012) Leptin-to-adiponectin, adiponectin-to-leptin ratios, and insulin are specific and sensitive markers associated with polycystic ovary syndrome: a case-control study from Bahrain. Metab Syndr Relat Disord 10(2): 98-102.
- Chen VCH, Chen CH, Chiu YH, Lin TY, Li FC, et al. (2018) Leptin/Adiponectin ratio as a potential biomarker for metabolic syndrome in patients with schizophrenia. Psychoneuroendocrinology 92: 34-40.
- Zhang M, Cheng H, Zhao X, Dongqing H, Yinkun Y (2017) Leptin and Leptin-to-Adiponectin Ratio Predict Adiposity Gain in Nonobese Children over a Six-Year Period. Child Obes Print 13(3): 213-221.
- Allaire J, Couture P, Leclerc M, Amélie C, Johanne M, et al. (2016) A randomized, crossover, head-to-head comparison of eicosapentaenoic acid and docosahexaenoic acid supplementation to reduce inflammation markers in men and women: the Comparing EPA to DHA (ComparED) Study. Am J Clin Nutr 104(2):280-287.
- Gammelmark, Madsen, Varming K, Lundbye-C, Schmidt (2012) Low-dose fish oil supplementation increases serum adiponectin without affecting inflammatory markers in overweight subjects. Nutr Res 32(1): 15-23.
- Koh KK, Quon MJ, Shin KC, Lee Y, Ichiro S, et al. (2012) Significant differential effects of omega-3 fatty acids and fenofibrate in patients with hypertriglyceridemia. Atherosclerosis 220(2): 537-544.
- Krantz MJ, Havranek EP, Pereira RI, Beaty B, Mehler PS, et al. (2015) Effects of omega-3 fatty acids on arterial stiffness in patients with hypertension: a randomized pilot study. J Negat Results Biomed 14: 21.
- Wang CY, Feng Z (2023) A Flexible Method for Diagnostic Accuracy with Biomarker Measurement Error. Mathematics 11(3): 549.
- Templeton (2011) A Two-Step Approach for Transforming Continuous Variables to Normal: Implications and Recommendations for IS Research. Commun Assoc Inf Syst p. 28.
- Guebre-Egziabher F, Debard C, Drai J, Laure D, Sandra P, et al. (2013) Differential dose effect of fish oil on inflammation and adipose tissue gene expression in chronic kidney disease patients. Nutrition 29(5): 730-736.
- Itariu BK, Zeyda M, Hochbrugger EE, Angelika N, Gerhard P, et al. (2012) Long-chain n-3 PUFAs reduce adipose tissue and systemic inflammation in severely obese nondiabetic patients: a randomized controlled trial. Am J Clin Nutr 96(5): 1137-1149.
- Ito R, Satoh-Asahara N, Yamakage H, Yousuke S, Shinji O, et al. (2014) An increase in the EPA/AA ratio is associated with improved arterial stiffness in obese patients with dyslipidemia. J Atheroscler Thromb 21(3): 248-260.
- Krebs JD, Browning LM, McLean NK, Rothwell JL, Mishra GD, et al. (2006) Additive benefits of long-chain n-3 polyunsaturated fatty acids and weight-loss in the management of cardiovascular disease risk in overweight hyperinsulinaemic women. Int J Obes 30(10): 1535-1544.
- Haidari F, Mohammadshahi M, Borsi SH, Haghighizadeh MH, Malgard S (2014) Comparison of Essential Fatty Acid Intakes and Serum Levels of Inflammatory Factors between Asthmatic and Healthy Adults: A Case- Control Study. Iran J Allergy Asthma Immunol 13(5): 335-342.
- Patel JV, Lee KW, Tomson J, Dubb K, Hughes EA, et al. (2007) Effects of omega-3 polyunsaturated fatty acids on metabolically active hormones in patients post-myocardial infarction. Int J Cardiol 115(1): 42-45.
- Huerta AE, Prieto-Hontoria PL, Sainz N, Martinez JA, Moreno-Aliaga MJ (2016) Supplementation with alpha-Lipoic Acid Alone or in Combination with Eicosapentaenoic Acid Modulates the Inflammatory Status of Healthy Overweight or Obese Women Consuming an Energy-Restricted Diet. J Nutr 146(4): 889S-896S.
- Poreba M, Mostowik M, Siniarski A, Renata GW, Krzysztof Piotr M, et al. (2017) Treatment with high-dose n-3 PUFAs has no effect on platelet function, coagulation, metabolic status or inflammation in patients with atherosclerosis and type 2 diabetes. Cardiovasc Diabetol 16(1): 50.
- Spencer M, Finlin BS, Unal R, Beibei Z, Andrew JM, et al. (2013) Omega-3 Fatty Acids Reduce Adipose Tissue Macrophages in Human Subjects with Insulin Resistance. Diabetes 62(5): 1709-1717.
- Masson S, Marchioli M, Mozaffarian D, Roberto B, Valentina M, et al. (2013) Plasma n-3 polyunsaturated fatty acids in chronic heart failure in the GISSI-Heart Failure Trial: Relation with fish intake, circulating biomarkers, and mortality. Am Heart J 165(2): 208.
- Mizia-Stec K, Haberka M, Mizia M, Artur C, Klaudia G, et al. (2011) N-3 Polyunsaturated fatty acid therapy improves endothelial function and affects adiponectin and resistin balance in the first month after myocardial infarction. Arch Med Sci 7(5): 788-795.
- Harving F, Svensson M, Flyvbjerg A, Erik BS, Kaj AJ, et al. (2015) n-3 polyunsaturated fatty acids and adiponectin in patients with end-stage renal disease. Clin Nephrol 83(5): 279-285.
- Becerril S, Rodríguez A, Catalán V, Beatriz R, Amaia M, et al. (2023) Sex- and Age-Dependent Changes in the Adiponectin/Leptin Ratio in Experimental Diet-Induced Obesity in Mice. Nutrients 15(1): 73.
- Frühbeck G, Catalán V, Rodríguez A, Beatriz R, Sara B, et al. (2019) Adiponectin-leptin Ratio is a Functional Biomarker of Adipose Tissue Inflammation. Nutrients 11(2): 454.
- Larsen MA, Isaksen VT, Moen OS, Wilsgaard L, Remijn M, et al. (2018) Leptin to adiponectin ratio - A surrogate biomarker for early detection of metabolic disturbances in obesity. Nutr Metab Cardiovasc Dis 28(11): 1114-1121.
- Chou HH, Hsu LA, Wu S, Teng MS, Sun YC, et al. (2014) Leptin-to-Adiponectin Ratio is Related to Low Grade Inflammation and Insulin Resistance Independent of Obesity in Non-Diabetic Taiwanese: A Cross-Sectional Cohort Study. Acta Cardiol Sin 30(3): 204-214.
- López-Jaramillo P, Gómez-Arbeláez D, López-López J (2020) Relationship among the leptin-to-adiponectin ratio, systemic inflammation, and anisocytosis: a plausible pathophysiological mechanism of a novel cardiovascular risk marker. Kardiol Pol 78(5): 381-382.
- Aydin S, Halifeoglu I, Ozercan IH, Fazilet E, Nermin K, et al. (2005) A comparison of leptin and ghrelin levels in plasma and saliva of young healthy subjects. Peptides 26(4): 647-652.
- Duffles LF, Hermont AP, Abreu LG, Pordeus IA, Silva TA (2019) Association between obesity and adipokines levels in saliva and gingival crevicular fluid: A systematic review and meta-analysis. J Evid-Based Med 12(4): 313-324.
- Hua Y, Herder C, Kalhoff H, Anette EB, Jonas E, et al. (2020) Inflammatory mediators in the adipo-renal axis: leptin, adiponectin, and soluble ICAM-1. Am J Physiol Renal Physiol 319(3): F469-F475.
- Meriç P, Özçaka Ö, Ceyhan-Öztürk B, Akcal A, Nalbantsoy A, et al. (2018) Salivary Adiponectin and Leptin Levels are Increased in Women with Gestational Diabetes Mellitus and Gingival Inflammation. Oral Health Prev Dent 16(6): 541-547.
- Sharifian M, Shohadaee S, Esfandiar N, Mohkam M, Dalirani R, et al. (2015) Serum and Urine Leptin Concentrations in Children Before and After Treatment of Urinary Tract Infection. Iran J Kidney Dis 9(5): 374-378.
- Thanakun S, Watanabe H, Thaweboon S, Izumi Y (2013) An effective technique for the processing of saliva for the analysis of leptin and adiponectin. Peptides 47: 60-65.
- Tvarijonaviciute A, Castillo C, Ceron JJ, Martinez-Subiela S, Tecles F, et al. (2017) Leptin and NGF in saliva of patients with diabetes mellitus type 2: A pilot study. J Oral Pathol Med Off Publ Int Assoc Oral Pathol Am Acad Oral Pathol 46(9): 853-855.
- Yaturu S, Reddy RD, Rains J, Jain SK (2007) Plasma and urine levels of resistin and adiponectin in chronic kidney disease. Cytokine 37(1): 1-5.






























