Quality of Life Outcomes After 3 Years of Bariatric Surgery: Comparison of Roux-En-Y Gastric Bypass and One Anastomosis Gastric Bypass
Alfonso Ballester R*, Kasyanchuk I, Mora-Oliver I, Kraus Fischer G, Martí Fernández R, Lapeña Rodríguez M, Cassinello Fernández N and Ortega Serrano J
General Surgery Department, University of Valencia, Spain
Submission: February 13, 2023; Published: March 13, 2023
*Corresponding author: Raquel Alfonso Ballester, General Surgery Department, Clinic University Hospital of Valencia. Avda. Blasco Ibáñez, 17. 46010-Valencia, Spain
How to cite this article: Alfonso Ballester R, Kasyanchuk I, Mora-Oliver I, Kraus Fischer G, Martí Fernández R, et al. Quality of Life Outcomes After 3 Years of Bariatric Surgery: Comparison of Roux-En-Y Gastric Bypass and One Anastomosis Gastric Bypass. Curre Res Diabetes & Obes J 2023; 16(3): 555940.DOI: 10.19080/CRDOJ.2023.16.555940
Abstract
Background: Laparoscopic One Anastomosis Gastric Bypass and Laparoscopic Roux-en-Y gastric Bypass are two of the most common bariatric techniques. We compared quality of life in both procedures, assessing pre-operative and long term post-operative differences in quality of life, physical activity level and psychosocial functioning in patients undergoing bariatric surgery.
Methods: A prospective cohort study including obese patients undergoing either Laparoscopic One Anastomosis Gastric Bypass or Laparoscopic Roux-en-Y gastric Bypass. The Moorehead-Ardelt Quality of Life Questionnaire II and Gastrointestinal Quality of Life Index (GIQLI) questionnaires were administered at 3 months preoperatively and 3 years after surgery, while the third, the Bariatric Analysis and Reporting Outcome System (BAROS), was administered only postoperatively.
Results: A total of 41 patients were included in the study. Statistically significant differences were found between the Moorehead-Ardelt Quality of Life Questionnaire II and QIGLI scores taken at both time points, across the entire cohort (p= 0.001 and p= 0.001, respectively); and between the results taken at 3 years postoperatively in the BAROS test (p= 0.001) for the entire cohort. There were no significant differences between Laparoscopic One Anastomosis Gastric Bypass and Laparoscopic Roux-en-Y gastric Bypass groups in the questionnaire scores (Moorehead-Ardelt Quality of Life Questionnaire II: p=0.526, QIGLI: p=0.990 and BAROS: p=0.753).
Conclusions: Bariatric surgery improves quality of life in operated patients, without significant differences between Laparoscopic One Anastomosis Gastric Bypass and Laparoscopic Roux-en-Y gastric Bypass techniques. Patients undergoing bariatric surgery develop higher physical activity levels, and long-term improvements in the psychosocial domain are observed over time.
Keywords: Bariatric surgery; Quality of life tests; One anastomosis gastric bypass; Roux-en-y gastric bypass
Abbreviations: DMI: Diabetes Mellitus; COPD: Chronic Obstructive Pulmonary Disease; QoL: Quality of Life; BMI: Body Mass Index; BAROS: Bariatric Analysis and Reporting Outcome System; IWQol: Impact of Weight on Quality of Life; GIQLI: Gastrointestinal Quality of Life Index; LRYGB: Laparoscopic Roux-en-Y Gastric Bypass; LOAGB: Laparoscopic One Anastomosis Gastric Bypass; HBA1C: Glycated Hemoglobin
Background
Obesity is a health problem with a great number of associated comorbidities, such as type II diabetes mellitus (DMII), high blood pressure, dyslipidemia and chronic obstructive pulmonary disease (COPD) [1]. Combined with excess weight, these conditions reduce the quality of life (QoL) of patients with obesity in both physical and psychosocial domains.
Excess weight affects not only physical but also psychosocial health, in the form of low self-esteem, depression, and anxiety, as well as difficulty performing daily life activities and finding employment due to physical appearance and social isolation, among other factors [2,3]. Obesity therefore results in multiple economic, social and personal dysfunctions, and when assessing QoL in patients with obesity, it is necessary to take into account both physical and psychosocial domains. The physical sphere can be assessed using anthropometric parameters such as abdominal circumference, weight and body mass index (BMI), in addition to parameters that determine related conditions such as diabetes, dyslipidemia or hypertension.
After bariatric surgery, patient QoL improves not only in the physical but also in the psychological domain, in perceptions of both self and environment [4]. There are multiple questionnaires that include assessment of both spheres, such as the Bariatric Analysis and Reporting Outcome System (BAROS), Impact of Weight on Quality of Life (IWQol), and Gastrointestinal Quality of Life Index (GIQLI), among others [5-7].
Laparoscopic Roux-en-Y gastric bypass (LRYGB) has classically been considered the preferred procedure in terms of weight loss and resolution of associated medical complications and is the most widely used malabsoptive procedure. Laparoscopic One Anastomosis Gastric Bypass (LOAGB), the second most commonly performed mixed procedure, is a viable alternative that achieves good weight loss results and minimal postoperative complications [8,9]. The two techniques have been compared in terms of percentage total weight loss, and resolution of DM2, high blood pressure and other comorbidities [10-12] with similar results, but data in QoL are scarce in the published literature. However, although they are very similar techniques, there are variations between the two that may cause differences in QoL, especially in the gastrointestinal area, such as the greater length of the biliopancreatic loop or the biliary reflux. Our experience with LOAGB is that if biliary reflux appears, it is mainly in the first 3 postoperative months, improving and disappearing along the first postoperative year. Moreover, both techniques lead to changes in the way the patient approaches food, so they start postoperatively with liquids and progressively solid meals are introduced. They are teached to properly chew well before swallowing each meal, and slow down while eating. In the first year they all go through a complete behavior change.
The purpose of our study is to investigate any potential differences in QoL in patients undergoing either LRYGB or LOAGB.
Methods
A prospective consecutive cohort single-center study was carried out in patients undergoing LRYGB or LOAGB for obesity between February 2018 and December 2019. A total of 41 patients were included. The study was submitted and approved by the Clinic University Hospital of Valencia INCLIVA ethics committee. All patients signed the written informed consent for the study participation.
As the main technique in our institution, LRYGB was performed as the primary surgical procedure, except in patients >55 years with associated metabolic syndrome (especially with poor glycemic control), in whom LOAGB was performed. Exclusion criteria were drug or alcohol addiction, severe mental disorder, age under 18 or over 65 years and advanced malignant pathology. Diabetes remission was defined by normoglycemia and glycated hemoglobin (HBA1C) levels below 6%, in the absence of glucose-lowering medications for at least 1 year [13]. All surgery was performed by three members of a highly specialized bariatric unit of a tertiary hospital. Institutional board approval was obtained.
The questionnaires used were BAROS [4], GIQLI [6] and M-A QoLQII [14]. The GIQLI and M-A QoLQII tests were completed preoperatively, while the BAROS test was used postoperatively only. All the tests were distributed at 1 month, 3 months, 1 year and 3 years after surgery.
The GIQLI questionnaire assesses patient QoL by providing information on general QoL aspects as well as accompanying digestive symptoms, which allows researchers to differentiate whether the QoL improvement is overall or at the expense of any of its constituent aspects. It comprises 36 questions divided into five domains: gastrointestinal symptoms (19 questions), physical dysfunction (7 questions), emotional dysfunction (5 questions), social dysfunction (4 questions) and effects of medical treatment (1 question).
The M-A QoLQII test consists of 6 questions aimed at evaluating mood, ability to enjoy physical activity and social encounters, ability to work, sexual activity and attitude towards food. Like the GIQLI, it allows us to determine preand postoperative differences, and also differences according to technique used. It is simple, user friendly and quick, which increases patient response rates. The BAROS questionnaire is only applicable after surgery. It analyzes outcomes of comorbidities, percentage of total weight loss, postoperative medical and surgical complications, need for reoperation and patient QoL. The associated comorbidities analyzed were DMII, arterial hypertension, dyslipidemia, COPD and osteoarthropathy.
A descriptive analysis was performed, and quantitative variables were tested for normality with the Shapiro-Wilk test. Qualitative data were expressed as n (%) and quantitative data as median (95% confidence intervals). For quantitative variables that met the criteria of normality and homoscedasticity, we applied parametric tests such as Student’s T for independent or paired samples. For quantitative variables that did not meet the normality criterion, non-parametric tests were used, such as the U-Mann-Whitney test for independent samples and the Wilcoxon test for paired samples. To assess the outcome of comorbidities over time, the McNemar test was applied for paired samples. Statistical analysis was carried out with IBM SPSS Statistics Version 26 for Windows. P<0.05 was considered statistically significant.
Results
After applying the exclusion criteria, a final study cohort of 41 patients was defined, of which 14 (34.14%) were male and 27 females. LRYGB was performed in 21 patients and LOAGB in 20. The average patient age was 53 years (range, 37–65). In the LOAGB group, all patients were over 55 years of age. In contrast, in the LRYGB group, 9 patients were over 50 years, and 12 patients were under 50. Statistically significant differences therefore existed between the two surgical techniques in terms of patient age ranges (p-value= 0.000). Average baseline BMI was 44.14 kg/m2 (±5.31 kg/m2). After a follow-up of 36 months, it was 29.15 kg/m2 (±5.56 kg/m2).
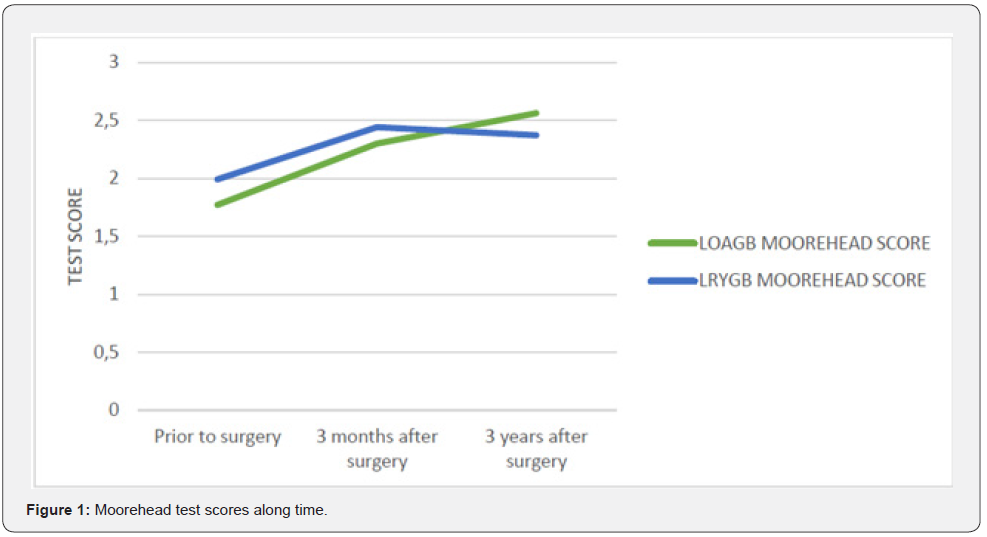
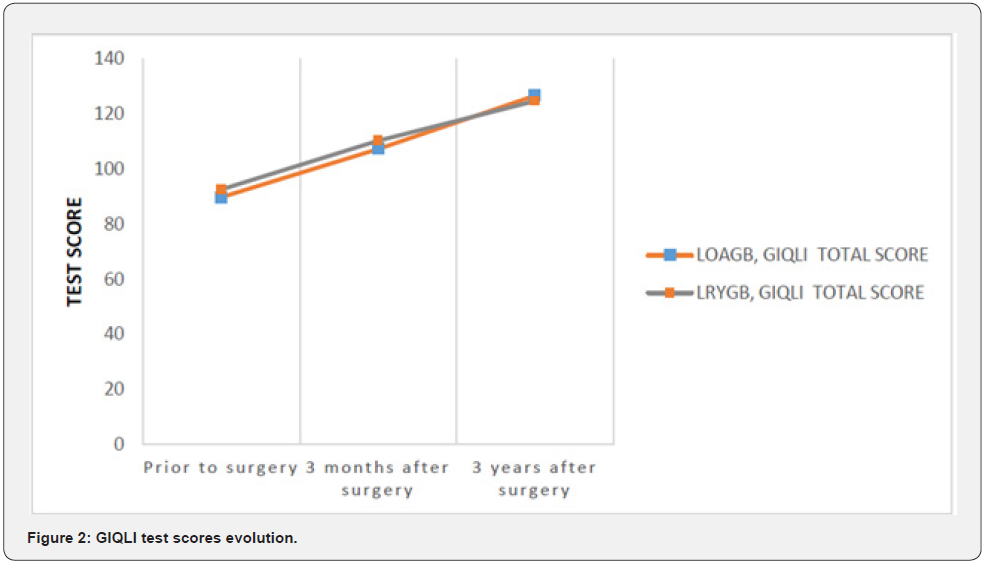
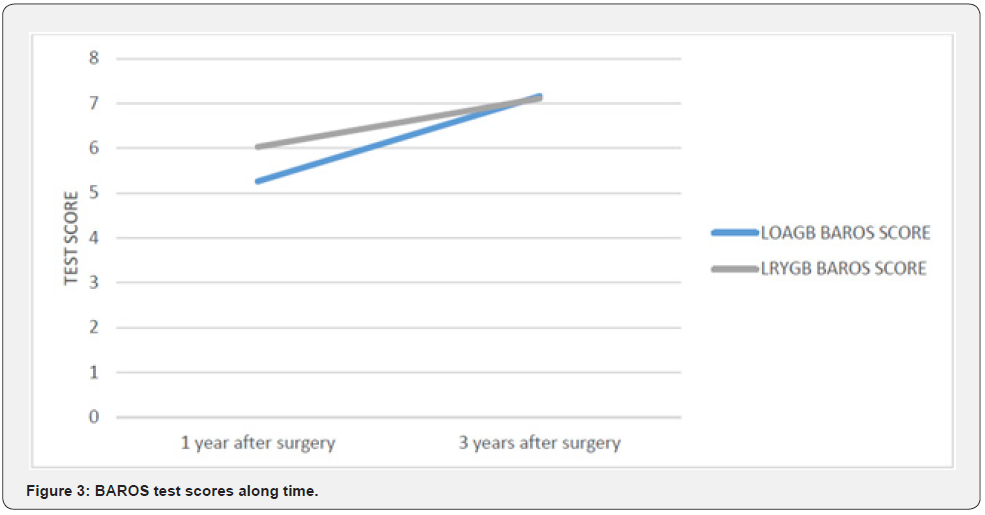
Percentage of total weight loss was calculated for both groups, revealing no statistically significant differences between the LOAGB and LRYGB groups (p= 0.657). The mean percentage of excess weight loss was 67.99% (± 21.23%); specifically, 67.69 (± 18.89%) in the LOAGB group and 68.27 (± 23.71%) in the LRYGB group. We compared M-A QoLQII and GIQLI test scores obtained at 3 months and 3 years after surgery with the results prior to surgery, finding statistically significant differences: (p=0.001, p=0.001), respectively (Figure 1 & 2). Statistically significant differences were also found between the results taken at 1 year and 3 years after surgery for the BAROS test (p 0.001) figure 3.
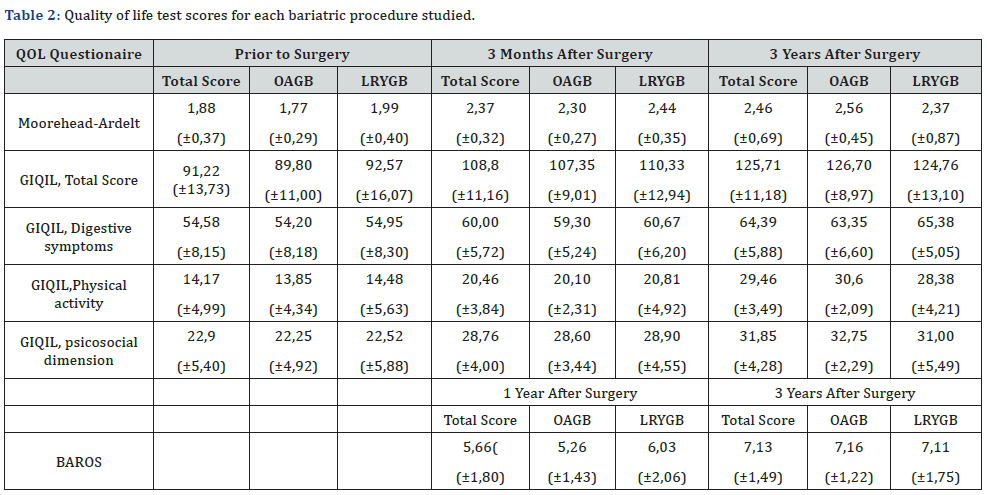
Comparing the two procedures (LOAGB and LRYGB), no significant between- group differences were found in any of the three QoL tests; M-A QoLQII (p = 0.526), BAROS (p = 0.753) and GIQLI (p = 0.990), respectively (Table 1 & Figure 4-6). When comparing comorbidities before and after surgery, associated medical problems varied across the study period (Table 2). No statistically significant differences were observed between procedures in terms of weight loss, QoL improvement or resolution of comorbidities, with the exception of DM2 and dyslipidemia resolution, which was slightly higher in the LRYGB group (p= 0.048 and p= 0.014, respectively). A total of 14 patients (34.14%) were treated for or showed signs of depression. Analyzing the presence of depression in the two groups, we noted statistically significant differences in the proportion of patients with depression (p= 0.037), which was far higher in patients operated using the LOAGB (71.4%, 10 patients) than LRYGB technique (28.6%, 4 patients). This can be due to a possible selection bias because LOAGB group had elder patients and with poorer health condition, which can lead to a higher level of depression.
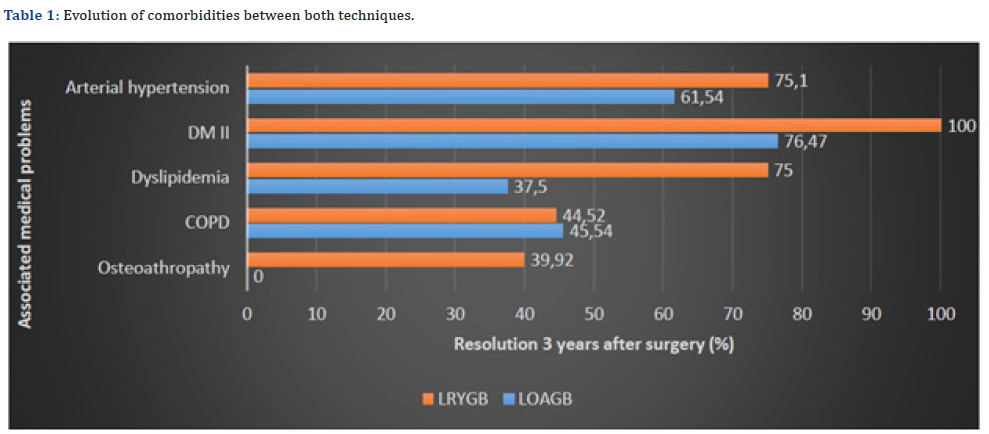
Results are shown in percentages (%)
QoL: Quality of Life
Discussion
Numerous publications have shown QoL improvement in patients undergoing bariatric surgery in the short term, at average time points of between 3 months and 1 year, but the number of studies evaluating patient outcomes over time and in the long term is limited [15-17]. According to the results obtained in our study, scores differed between the three QoL questionnaires used, comparing pre and post- operative data, and confirm an improvement at long-term QoL follow-up in patients undergoing bariatric surgery compared to their situation prior to surgery. This QoL improvement evolves over time, with differences also found between the scores obtained at short term and long term. In line with similar studies, our findings therefore underline the importance of long-term follow-up via QoL questionnaires of patients undergoing bariatric surgery, to enable standardized between-group comparisons with defined criteria [18,19].
Percentage of excess weight lost is among the essential parameters to assess the effectiveness of bariatric surgery [20,21]. Both surgical techniques used in our study achieve an adequate percentage of excess weight loss, as evidenced by mean weight and BMI outcomes of participating patients. LRYGB is the current gold standard of bariatric surgery, while LOAGB is under study as an equally effective alternative with fewer technical requirements [22,23]. Statistical analysis of results with the two surgical procedures failed to yield sufficient differences between the two, leading to the conclusion that both achieve an optimal decrease in excess weight, QoL improvement and resolution of comorbidities.
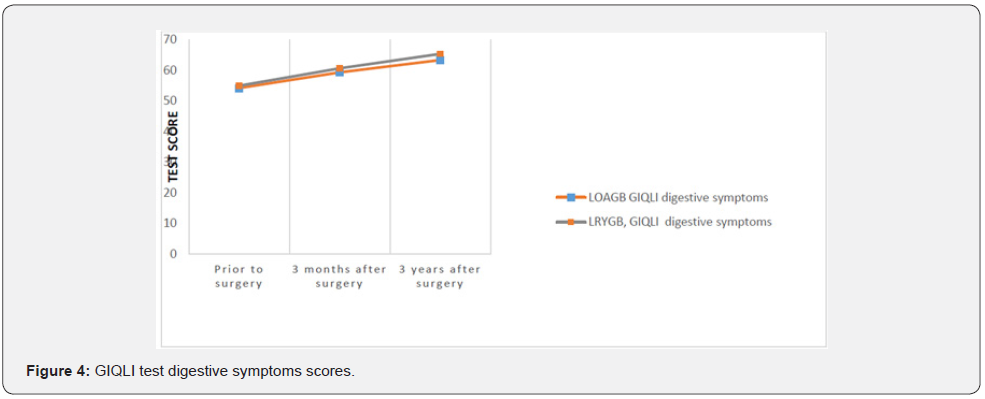
Undergoing bariatric surgery involves great changes for patients, who must adapt to a new way of eating due to the inability to consume large amounts of food or heavy meals without experiencing frequent digestive symptoms such as nausea, vomiting, diarrhea or early satiety. It is therefore important to evaluate patient suitability for new eating plans by assessing the accompanying digestive symptoms that may occur in the long term. In our study, we observed that the GIQLI digestive symptoms scores are different from patients’ previous situation and also compared to results obtained in the short term. In the clinical interview, many patients confirmed these changes over time and the long learning curve regarding food intake after undergoing surgery.
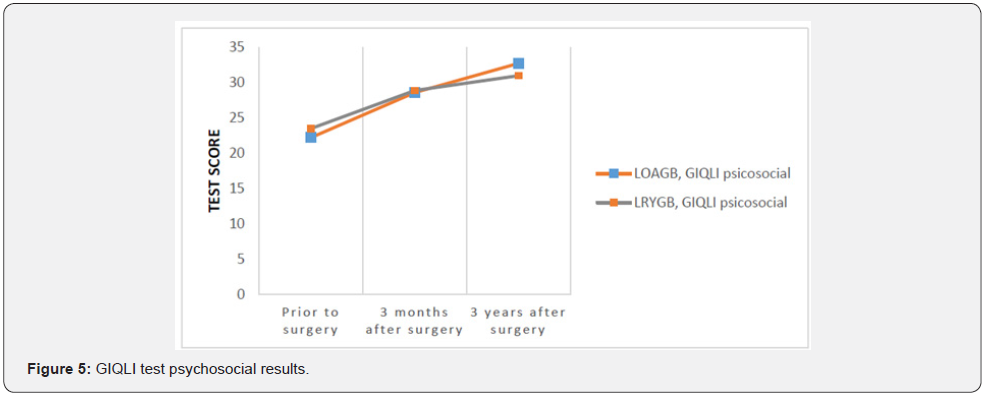
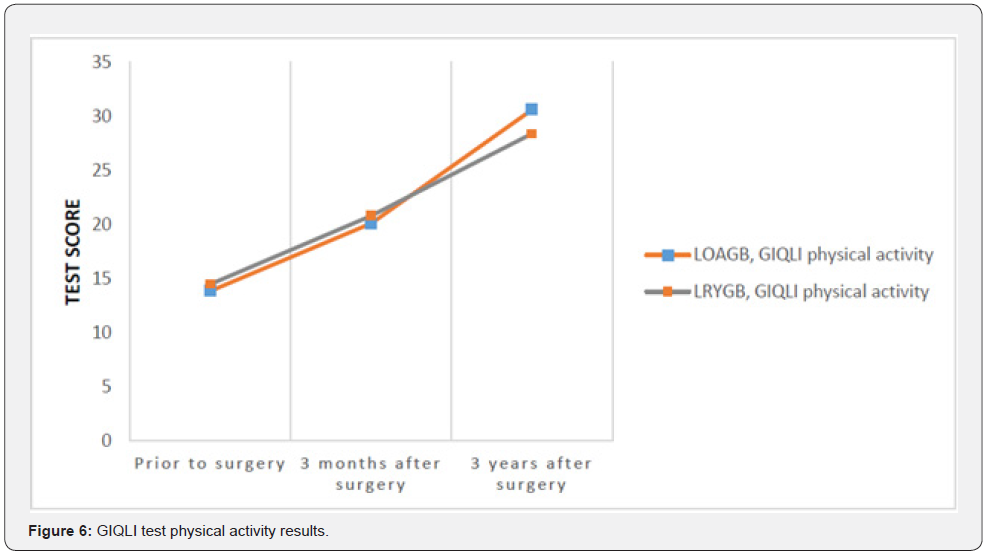
As regards physical activity, drastic weight reduction results in greater agility and endurance, with substantial improvements compared with patients’ preoperative status [15]. This change not only facilitates performing physical exercise aimed at weight loss, but also brings positive changes in daily activities, such as climbing stairs, and greater agility at work and home, among others. In the psychosocial domain, we observed long-term improvements and progress over time compared to short term results, with no evident differences between the two surgical procedures. When interpreting these results, it is important to take into account the prevalence of anxious-depressive syndrome and the context of the current COVID-19 pandemic. During clinical interview many patients reported feeling a higher degree of sadness related to SARS-COV2, concern due to slight weight gain because of increased inactivity, and a greater degree of anxiety about food.
We found noteworthy changes in self-esteem and perception of environment over follow-up. However, many patients have substantial excess skin which has a negative effect on selfesteem and sexual and physical activity. Multiple studies have shown that patients who undergo excess skin removal after bariatric surgery report greater and more enduring satisfaction with surgery than those who have not undergone this procedure [24,25]. In relation to comorbidities in the long term, we found a significant improvement in all those studied, but without perceiving an evident change in osteoarthropathy. This could be explained by the fact that many of the comorbid diseases patients presented with were chronic or rheumatological. Note that the LOAGB group includes older patients than the LRYGB, resulting in long and chronic osteoarthropathy in some patients and therefore less marked improvement after surgery. This same factor could also have impacted on DM2 and dyslipidemia, showing worse results in the older, LOAGB group than in the LRYGB group because of the chronic course of the two medical conditions. This statistical bias is a limitation of our study that should be taken into account.
Conclusions
Bariatric surgery is the most effective long-term therapeutic method for patients with obesity, since it brings great QoL changes in both physical and psychosocial domains, while also resolving many comorbidities associated with obesity, and these results are maintained over time. QoL questionnaires are crucial to be able to carry out between-group comparisons across time in these domains. Up to 60% of patients report QoL improvement in the psychosocial sphere in terms of anxiety and depression compared to their status prior to surgery. This is a general improvement, related to decrease in BMI, since neither surgery type, age or sex significantly affected improvement or resolution of these complications. The improvements in QoL are greater in the physical than in the mental sphere, due to the influence of baseline psychological state prior to surgery in each patient, which exerted a greater effect in the younger age groups. Therefore, it is important to take patient age into account when making generalized analyzes of the results.
Numerous publications have shown a QoL improvement in patients undergoing bariatric surgery in the short term, between 3 months and a year, but few studies have evaluated this in the long term. In our work, differences in scores obtained were observed in the three QoL questionnaires across all different study time points, across the entire sample, but not between the two groups. This seems to confirm an improvement in longterm QoL in operated patients compared to their preoperative condition. This change evolves over time, as differences are found between scores obtained in the short and long term.
Declarations
Ethics approval and consent to participate: All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/ or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study was submitted and approved by the Clinic University Hospital of Valencia INCLIVA ethics committee. All patients signed the written informed consent for the study participation.
Availability of Data and Materials
All data and material are kept in our institutional database.
Competing Interests
We declare we have no competing interests.
Funding
No institutional funding has been needed for this study.
References
- Expert panel report (2013) Guidelines for the management of overweight and obesity in adults. Obesity 22: S41-S410.
- S Kasen, P Cohen, H Chen, A Must (2008) Obesity and psychopathology in women: A three-decade prospective study. International Journal of Obesity 32(3): 558-566.
- Luppino, Floriana S (2010) Overweight, obesity, and depression: a systematic review and meta-analysis of longitudinal studies. Archives of general psychiatry 67(3): 220-229.
- Sierżantowicz R, Lewko J, Hady HR, Kirpsza B, Trochimowicz L, et al. (2017) Effect of BMI on quality of life and depression levels after bariatric surgery. Adv Clin Exp Med 26(3): 491-496.
- Oria HE, Moorehead MK (1998) Bariatric analysis and reporting outcome system (BAROS). Obes Surg 8(5): 487-499.
- Manwaring J, Wilfley D (2010) The Impact of Weight on Quality of Life Questionnaire. In: Preedy VR, Watson RR, (Eds.), Handbook of Disease Burdens and Quality of Life Measures. Springer, New York, USA, p. 209-225.
- Quintana JM (2001) Traducción y validación del Índice de Calidad de Vida Gastrointestinal (GIQLI). Rev Esp Enferm Dig 93(11): 693-699.
- Bruzzi M, Rau C, Voron T, Guenzi M, Berger A, et al. (2015) Single anastomosis or mini-gastric bypass: long-term results and quality of life after a 5-year follow-up. Surg Obes Relat Dis 11(2): 321-326.
- Wang FG, Yan WM, Yan M, Song MM (2018) Outcomes of Mini vs Roux-en-Y gastric bypass: A meta-analysis and systematic review. Int J Surg 56: 7-14.
- Robert M, Philippe Espalieu, Elise Pelascini, Robert Caiazzo, Adrien Sterkers, et al. (2019) Efficacy and safety of one anastomosis gastric bypass versus Roux-en-Y gastric bypass for obesity (YOMEGA): a multicentre, randomised, open-label, noninferiority trial. Lancet 393(10178): 1299-1309.
- Magouliotis DE, Tasiopoulou VS, Tzovaras G (2019) One Anastomosis Gastric Bypass Versus Roux-en-Y Gastric Bypass for Morbid Obesity: an Updated Meta-Analysis. Obes Surg 29(9): 2721-2730.
- Poublon N, Chidi I, Bethlehem M, Kuipers E, Gadiot R, et al. (2020) One anastomosis gastric bypass vs. Roux- en-Y gastric bypass, remedy for insufficient weight loss and weight regain after failed restrictive bariatric surgery. Obes Surg 30(9): 3287-3294.
- Buse JB, Caprio S, Cefalu WT, Antonio Ceriello, Stefano Del Prato, et al. (2009) How do we define cure of diabetes? Diabetes Care 32(11): 2133-2135.
- Moorehead MK, Ardelt-Gattinger E, Lechner H, Oria HE (2003) The validation of the Moorehead-Ardelt Quality of Life Questionnaire II. Obes Surg 13(5): 684-692.
- Julia C, C Ciangura, L Capuron, J-L Bouillot, A Basdevant, et al. (2013) Quality of life after Roux-en-Y gastric bypass and changes in body mass index and obesity-related comorbidities. Diabetes Metab 39(2): 148-154.
- Dreber H, Thorell A, Reynisdottir S, Hemmingsson E (2019) Health-Related Quality of Life 5 Years After Roux-en-Y Gastric Bypass in Young (18-25 Years) Versus Older (≥ 26 Years) Adults: A Scandinavian Obesity Surgery Registry Study. Obes Surg 29(2): 434-443.
- Piotr Major, Tomasz Stefura, Błażej Dziurowicz, Joanna Radwan, Michał Wysocki, et al. Quality of Life 10 Years After Bariatric Surgery. Obes Surg 30(10): 3675-3684.
- Castanha CR, Castanha AR, Belo GQMB, Lacerda RMR, Vilar L (2018) Evaluation of quality of life, weight loss and comorbidities of patients undergoing bariatric surgery. Rev Col Bras Cir 45(3): e1864.
- Queiroz C, Sallet JA, DE Barros E Silva PG, Queiroz LD, Pimentel JA, et al. (2017) Application of BAROS' questionnaire in obese patients undergoing bariatric surgery with 2 years of evolution. Arq Gastroenterol 54(1): 60-64.
- Larrad A, Sánchez Cabezudo C (2004) Indicadores de calidad en cirugía bariátrica y criterios de éxito a largo plazo. Cir Esp 75(3): 301-304.
- Al Harakeh AB, Larson CJ, Mathiason MA, Kallies KJ, Kothari SN (2011) BAROS results in 700 patients after laparoscopic Roux-en-Y gastric bypass with subset analysis of age, gender, and initial body mass index. Surg Obes Relat Dis 7(1): 94-98.
- Carbajo M, Ortiz J, García C, Pérez M, Guadalupe O, Castro J (2008) Bypass gástrico laparoscópico de una sola anastomosis (BAGUA) asistido con brazo robótico: Técnica y resultados en 1,126 pacientes. Rev Mex Cir Endoscop 9(1): 6-13.
- Carbajo MA, Luque-de-León E, Jiménez JM, Ortiz-de-Solórzano J, Pérez- Miranda M, et al. (2017) Laparoscopic One-Anastomosis Gastric Bypass: Technique, Results, 26 and Long-Term Follow-Up in 1200 Patients. Obes Surg 27(5): 1153-1167.
- Tremp M, Delko T, Kraljević M, Zingg U, Rieger UM, et al. (2015) Outcome in body-contouring surgery after massive weight loss: A prospective matched single-blind study. J Plast Reconstr Aesthet Surg 68(10): 1410-1416.
- Cai A, Maringa L, Hauck T, Boos AM, Schmitz M, et al. (2020) Body Contouring Surgery Improves Physical Activity in Patients After Massive Weight Loss-a Retrospective Study. Obes Surg 30(1): 146-153.






























