- Research Article
- Abstract
- Traumatic Brain Injury - Causes
- Traumatic brain injury-Incidence
- Traumatic Brain Injury - Diagnosis
- Trajectory of mTBI
- Symptoms Prognosis of Traumatic Brain Injury
- Diagnosis Symptomatology of TBI
- Hormones and TBI
- How does hypoglycemia impair cognition?
- Can you Enhance Cognitive Performance in Alzheimer’s?
- References
Mild Traumatic Brain Injury, Hibernation, Type 2 Diabetes Common Etiopathophysiology Biomarkers and Function
Cheryl A Frye*, Luciana F Lembo and Jennifer Torgenson
Comprehensive Neuropsychological Services, USA
Submission: October 8, 2022; Published: January 17, 2023
*Corresponding author: Cheryl A Frye, Comprehensive Neuropsychological Services, 490 Western Avenue, Albany, NY 12203, USA
How to cite this article: Cheryl A Frye, Luciana F Lembo, Jennifer T. Mild Traumatic Brain Injury, Hibernation, Type 2 Diabetes Common Etiopathophysiology Biomarkers and Function. Curre Res Diabetes & Obes J 2023; 16(3): 555937.DOI: 10.19080/CRDOJ.2023.16.555937
- Research Article
- Abstract
- Traumatic Brain Injury - Causes
- Traumatic brain injury-Incidence
- Traumatic Brain Injury - Diagnosis
- Trajectory of mTBI
- Symptoms Prognosis of Traumatic Brain Injury
- Diagnosis Symptomatology of TBI
- Hormones and TBI
- How does hypoglycemia impair cognition?
- Can you Enhance Cognitive Performance in Alzheimer’s?
- References
Abstract
The link between diabetes and traumatic brain injury (TBI) is an area worthy of exploration. TBI is caused by bumps, blow, jolt, or penetrating injury to the head. Even mild (mTBI) and moderate TBI frequently results in chronic cognitive, emotional and behavioral symptoms, which impact long-term outcome and functioning. Traumatic brain injury is associated with neuroendocrinopathies including hypothalamic, pituitary, adrenal, gonadal (HPAG axis), pancreatic and other hormonal dysfunctions. Increases in cortisol, cholesterol, and weight gain that can occur with some TBI can all survivors may contribute to Metabolic Syndrome and Type II diabetes. In addition, many patients with TBI find physical activity, proper eating and sleeping difficult. They also often experience anxiety and stress, which contribute to hormonal dysregulation. Taking a proactive approach in lifestyle to avoid becoming diabetic and careful monitoring to address issues can improve the quality of life of patients with TBI and prevent the likelihood of developing metabolic syndrome and Type II diabetes. We also show endocrine data of several different species in different phases or types of hibernation which can be informative.
Keywords: Diabetes; Traumatic brain injury; Hormonal dysregulation; Type II diabetes; Metabolic syndrome; Chronic cognitive; Emotional and behavioral symptoms
- Research Article
- Abstract
- Traumatic Brain Injury - Causes
- Traumatic brain injury-Incidence
- Traumatic Brain Injury - Diagnosis
- Trajectory of mTBI
- Symptoms Prognosis of Traumatic Brain Injury
- Diagnosis Symptomatology of TBI
- Hormones and TBI
- How does hypoglycemia impair cognition?
- Can you Enhance Cognitive Performance in Alzheimer’s?
- References
Traumatic Brain Injury - Causes
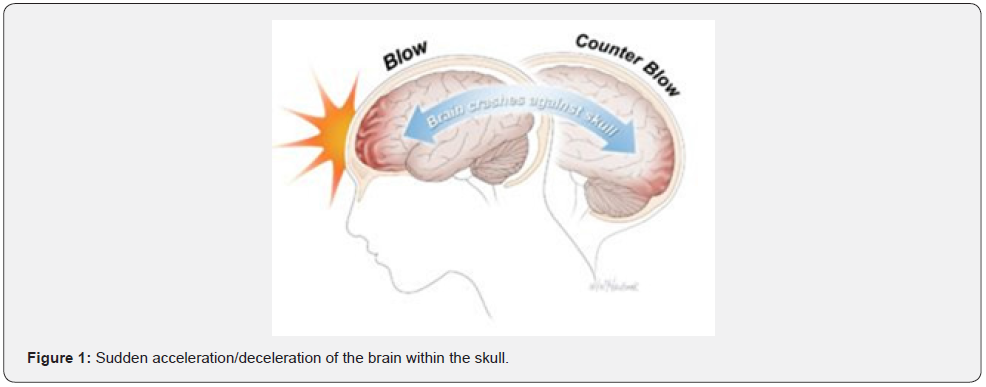
Traumatic brain injury (TBI) is caused by bumps, blow, jolt, or penetrating injury to the head. Brain injuries occur in motor vehicle or bicycle crashes, in sports and industrial accidents. They may be sustained from whiplash, falls, assaults, or loud blasts injuries, or long periods of exposure to loud blasts at unexpected intervals. The common all-cause effect of TBI is prevalent, disabling and treatment- resistant conditions due to focal impact to the head and/or sudden acceleration/deceleration of the brain within the skull (Figure 1). Shaken baby syndrome, falls, surgeries gone wrong or delayed, following pressure, blood or blockage of the brain, due to strokes, viruses, or injuries to the eye (or other body parts) can also produce TBI injuries. If not fatal, they. They are often life-changing and require the same kind of aggressive diagnosis and proper treatment that occurs with heart attacks and strokes. The first step in the treatment of intracranial brain injury is to recognize when it has occurred so that stroke medications, such as troponin, can be used in the 3-hour window of a non-bleeding stroke, as necessary and appropriate.
- Research Article
- Abstract
- Traumatic Brain Injury - Causes
- Traumatic brain injury-Incidence
- Traumatic Brain Injury - Diagnosis
- Trajectory of mTBI
- Symptoms Prognosis of Traumatic Brain Injury
- Diagnosis Symptomatology of TBI
- Hormones and TBI
- How does hypoglycemia impair cognition?
- Can you Enhance Cognitive Performance in Alzheimer’s?
- References
Traumatic brain injury-Incidence
Traumatic brain injury is extremely prevalent in the U.S. and is associated with substantial morbidity and functional impairment. In New York State, people that have brain injuries and are present at hospitals exceeds the national average and is around 550 persons a day. Nation-wide of the two and a half million emergency department visits 87% were treated and released another 11% were hospitalized and discharged 2% died from their traumatic brain injuries. These numbers do not account for those who do not receive medical care who had outpatient or office-based visits or who receive care at federal facilities. The Department of Defense data revealed that from 2000 through 2011, 235,046 service members or approximately 5% of the 5.5 million who served in the Army, Air Force, Navy, and Marine Core or diagnosed with a TBI. These data were from the CDC and IH Department of Defense invitation VA leadership panel in 2013. These numbers are clearly under reports of the incidence of traumatic brain injury. Many people are in denial that they have a traumatic brain injury and do not seek care. Others do not seek care because they do not have the resources for it. Lastly those who are in motor vehicle accidents often do not seek care because of complications surrounding car insurance and liability issues or nationality status.
- Research Article
- Abstract
- Traumatic Brain Injury - Causes
- Traumatic brain injury-Incidence
- Traumatic Brain Injury - Diagnosis
- Trajectory of mTBI
- Symptoms Prognosis of Traumatic Brain Injury
- Diagnosis Symptomatology of TBI
- Hormones and TBI
- How does hypoglycemia impair cognition?
- Can you Enhance Cognitive Performance in Alzheimer’s?
- References
Traumatic Brain Injury - Diagnosis
The severity of TBI can be classified as mild, moderate, or severe based upon the individuals’ clinical presentation. Results of positive imaging tests, such as CAT scans or MRI’s can be the definitive of a traumatic brain injury. However, negative tests on such scans do not indicate that there is no TBI. Some of the inherent challenges with TBI is that damage to the brain is often not evident on imaging with CAT scans or MRIs. CAT scans are used to evaluate whether there has been compression of the brain, such that some of these sulci are compromised, whether there has been a midline shift, or a brain bleed has occurred. MRIs are also limited. They only show large changes in the brain. They do not reveal damage caused by axonal shearing, which is a major cause of injury in TBI. PET scans can evaluate axonal shearing, but they are so expensive or of limited availability that they are not typically utilized to evaluate TBIs. In the absence of definitive damage on a scan, evaluation by a neuropsychologist is needed for diagnosis of TBI.
- Research Article
- Abstract
- Traumatic Brain Injury - Causes
- Traumatic brain injury-Incidence
- Traumatic Brain Injury - Diagnosis
- Trajectory of mTBI
- Symptoms Prognosis of Traumatic Brain Injury
- Diagnosis Symptomatology of TBI
- Hormones and TBI
- How does hypoglycemia impair cognition?
- Can you Enhance Cognitive Performance in Alzheimer’s?
- References
Trajectory of mTBI
Mild (mTBI) and moderate to severe TBI, frequently results in chronic cognitive, emotional and behavioral symptoms, which impact long-term outcome and functioning. These numbers will be increasing, because of covid, which has effects on the pons to alter breathing on the brain. We have already seen post-covid patients presenting with mTBI. Moderate TBI patients have difficulty ambulating, transferring and toileting. Severe TBI cases are of individuals who are bedridden, on catheters, and have a limited capacity to communicate.
- Research Article
- Abstract
- Traumatic Brain Injury - Causes
- Traumatic brain injury-Incidence
- Traumatic Brain Injury - Diagnosis
- Trajectory of mTBI
- Symptoms Prognosis of Traumatic Brain Injury
- Diagnosis Symptomatology of TBI
- Hormones and TBI
- How does hypoglycemia impair cognition?
- Can you Enhance Cognitive Performance in Alzheimer’s?
- References
Symptoms Prognosis of Traumatic Brain Injury
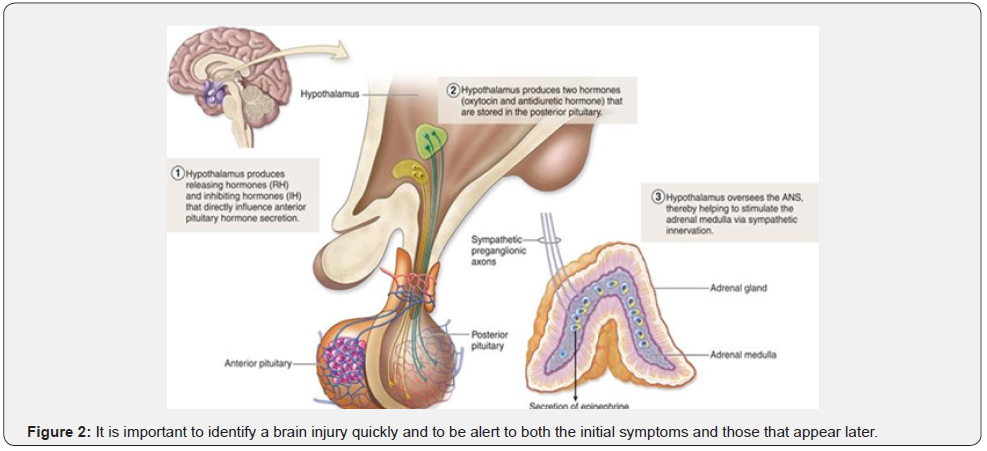
In the following pages, we list some of the symptoms a brain injury typically shows, first those that are likely to appear at the time of the injury, then those that may appear later. It should be noted that brain injuries are highly individualized. As such, the symptoms will vary widely from person to person. Healing in brain injury takes time, for some months and others’ years. Failure to appreciate this and forcing individuals back to their normal life activities before they are ready can severely retard their progress in recovery. It is important to identify a brain injury quickly and to be alert to both the initial symptoms and those that appear later (see Figure 2).
- Research Article
- Abstract
- Traumatic Brain Injury - Causes
- Traumatic brain injury-Incidence
- Traumatic Brain Injury - Diagnosis
- Trajectory of mTBI
- Symptoms Prognosis of Traumatic Brain Injury
- Diagnosis Symptomatology of TBI
- Hormones and TBI
- How does hypoglycemia impair cognition?
- Can you Enhance Cognitive Performance in Alzheimer’s?
- References
Diagnosis Symptomatology of TBI
In the following pages, we list the symptoms a brain injury typically shows, first those that are likely to appear at the time of the injury, then those that may appear later. It should be noted that brain injuries are highly individualized. As such, the symptoms will vary widely from person to person. Healing in brain injury takes time for some months and there other years. Failure to appreciate this and forcing individuals back to their normal life activities before they are ready can severely retard their progress. It is important to identify a brain injury quickly and to be alert to both the initial symptoms and those that appear later. Some of the inherent challenges with TBI is that damage to the brain is often not evident on imaging with CAT scans or MRIs, so functional determinations are necessary. The further, the common symptomatology, such as headache, seizures, motor disorders, sleep disorders, dizziness, visual disturbances, ringing in the ears, mood changes, and cognitive, memory, and speech and sleep difficulties— resemble symptoms of post-traumatic stress disorder (PTSD), which is often co-morbid with TBI. Some of the symptoms unique to TBI are persistent headaches, ringing in the ears, and sensitivity to light. Another challenge of TBI is that people often do not look different. So, it is hard for the individual with TBI and the people around them to adjust to profound changes associated with TBI. These, and other factors, may be associated with an increased vulnerability to certain psychological disorders, possibly accounting for the high rate of such disorders and suicide among survivors. The remainder of this article will focus on our work on people with mTBI (primary injury), who develop metabolic syndrome or Type 2 diabetes as a secondary injury in a subset of such individuals, and an interesting model of it (Figure 3).

Brain Injuries occur in motor vehicle or bicycle crashes, in sports and industrial accidents. They may be sustained from whiplash, falls, assaults, or loud blasts. If not fatal, they are often life-changing and require the same kind of aggressive diagnosis and proper treatment that occurs with heart attacks and strokes. The first step in the treatment of brain injury is to recognize when it has occurred. In the following pages, we list the symptoms a brain injury typically shows, first those that are likely to appear at the time of the injury, then those that may appear later. It should be noted that brain injuries are highly individualized. As such, the symptoms will vary widely from person to person. Healing in brain injury takes time for some months and thers years. Failure to appreciate this and forcing individuals back to their normal life activities before they are ready can severely retard their progress. It is important to identify a brain injury quickly and to be alert to both the initial symptoms and those that appear later.
- Research Article
- Abstract
- Traumatic Brain Injury - Causes
- Traumatic brain injury-Incidence
- Traumatic Brain Injury - Diagnosis
- Trajectory of mTBI
- Symptoms Prognosis of Traumatic Brain Injury
- Diagnosis Symptomatology of TBI
- Hormones and TBI
- How does hypoglycemia impair cognition?
- Can you Enhance Cognitive Performance in Alzheimer’s?
- References
Hormones and TBI
Traumatic brain injury is associated with neuroendocrineo pathies including hypothalamic, pituitary, adrenal, gonadal (HPAG axis), pancreatic and other hormonal dysfunctions. Indeed, prior to the development of current technologies to image the brain, one of the means by which traumatic brain injuries were defined was by verifying long term dysfunction of the endocrine axis a year following brain insult, which occurs in 30-80% of persons with TBI. Some of the challenges facing individuals with mild traumatic brain injury include a list of up to 137 symptoms which focus on physical, cognitive, and emotional challenges, which are largely due to effects of hormonal targets. Neuroendocrine dysfunction and TBI share 12 overlapping symptoms.
At the 2015 Brain Injury Association of New York State annual congress, held at the Marriot Hotel in Latham NY, Gary Bussey was the keynote speaker. He is in many ways a personification of someone with an mTBI. He can function in the world, but it is challenging for him in some ways; for example, emotional regulation and self-awareness can be difficult. During each session, questionnaires were left for participants with varying interests. The questionnaires focused on the individual’s level of TBI, the duration since their TBI, how they were functioning, the physical, cognitive and emotional symptoms associated with TBI, and the degree to which individual’s perceived their symptoms impaired their daily life. Of all 137 TBI symptoms, 12 symptoms had a Cronbach’s alpha chrone back alpha statistical loading of greater than 0.80, and another set of 8 particular symptoms had Cronbach’s alpha score above 0.85 concordance. They all corresponded with symptoms of neuroendocrine dysfunction. Physical symptoms were fatigue/lethargy, appetite changes, and weight changes. Cognitive symptoms were problems with shortterm memory and concentration. Emotional regulation symptoms were anxiety and depression. Changes in libido did not achieve this level of significance. It should be noted that a tell-tale factor in determining TBI in the first opportunity to test individuals, 3 months after injury, is that sexual dysfunction has been reported in every man and woman with a mTBI that my clinic has diagnosed. The reasons were for both performance and motivational dysfunction. It is so endemic in the disorder that most people have never been asked about it, or associated it with their injury, and those with mTBI typically do not report this symptom unless it is explicitly asked. The majority of my patients were never asked about ED post TBI and were highly relieved to know this was due to pituitary dysfunction and they could be treated by a urologist (Figure 4).
During a traumatic brain injury, which is typically due to a blow to the head or a blast injury, the brain tethered to the spinal cord and skull brain generally stays in place and the skull moves around the brain causing damage, including contra-cous impact to the brain and movement of the pituitary, which is held on by a nerve net to the hypothalamus. Of the patients in our clinic, those who are type 1 diabetics type, long prior to their TBI, demonstrate the greatest least variance in blood sugar levels, A1C, cortisol, and plasma neurosteroids cholesterol. Many more patients (33%) have become diabetic after their TBI. Those who become Type II diabetics are typically associated with the development of a lifestyle in which they become like “bears” in terms of their phenotype, behavior, metabolism and endocrinopathies. They eat sparsely and only when food is made available to them at home; they engage in very little physical activity; if able to they will spend a significant amount of time sleeping; they gain weight gain, develop metabolic syndrome and type 2 diabetes. Other patients with mild TBI, who are able to maintain some level of activity and remain on a daily schedule of eating, exercise, cognitive and social engagement, (we call “squirrels”) do not seem develop type 2 diabetes. However, they do typically experience an increase in cholesterol levels usually between 50 and 75ng/mL higher than prior to their injury. Many are encouraged to take cholesterol lowering medications, which are contra-indicated in mTBI, due to their amnestic effects. Further, cholesterol goes up with TBI because it is a necessary building block for the brain. However, if cholesterol levels (over 250 in are excessive they have to be treated).
It is a well-known fact that Drs. Robert Flint (St. Rose) and Dr. Ewan McNay (UAlbany) have shown that having a little sugar boost will increase boost cognitive performance; however, we have not seen this in our “bear” TBI ENT patients. There is a candy jar in the check in room filled with Lifesaver peppermints in individual wrapped packages. Those bears who have a mint do not do better on cognitive tasks than bears that do not have a mint. However, squirrels that have a mint do perform better than those that do not have a mint. Hibernation is an adaptation for mammals which is characterized by severely reduced energy needs (i.e., lower metabolism and body temperature) in times when resources may be limited, such as in the Artic during winter (Barnes, 1989). As such, it may be akin to what we see in some of our patients with TBI, who have metabolic syndrome, Type II diabetes, and amotivation syndrome and cannot do much other than sleep and the minimum ADL’s (Figure 5).

Hibernation is thought to have some conserved physiological mechanisms across different species. For example, there is increased tau phosphorylation in the brains of hibernating species, such as black bears (Ursus americanus), during torpor compared to arousal. Black bears’ hibernation is characterized by a metabolic rate that drops to about 25% of the euthermic condition and maximum reductions in body temperature to 30°C. These findings pose the question: what is the role of blood sugar levels, A1C, cortisol, and cholesterol, in hibernation and such model systems of stress?
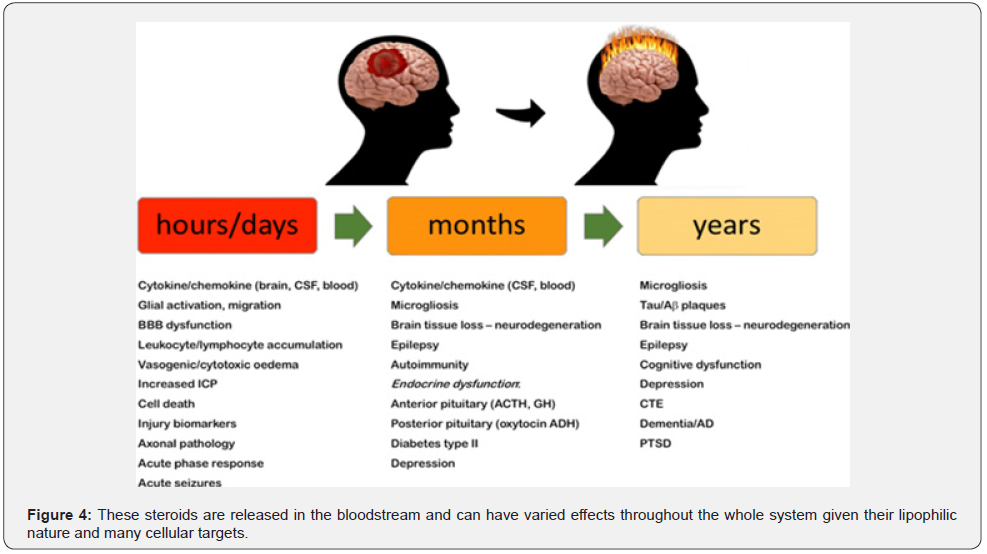
The classic notion about hormones, such as sex and stress steroids, is that they are molecules produced by glands in the periphery, under control from central nervous system input and tropic factors, in specific contexts. These steroids are released in the bloodstream and can have varied effects throughout the whole system given their lipophilic nature and many cellular targets. In the brain, ovarian progesterone is converted by the 5alpha-reductase enzyme to dihydroprogesterone (DHP), which is then converted to allopregnanlone by the 3alpha-hydroxysteroid dehydrogenase enzyme. Estradiol, from the ovaries, enhances the effects of these enzymes and can increase central allopregnanolone levels [1-3]. Some of the functional effects of sex and stress steroids from the periphery are those involved in reproduction, growth, and stress responding.
There is another class of steroids referred to as neurosteroids because they can be produced de novo in the brain. Stressors, ranging from foots hock to social challenges, mating, maternal behavior can increase levels of these neurosteroids (e.g. allopregnanolone) [4-11]. Moreover, administering allopregnanlone to female rats reduces their stress responses to an acute physical challenge (e.g. restraint; [6]). As such, these data suggest that neurosteroids may inhibit the stress response and restore sympathetic tone. Clearly, this could have adaptive significance beyond this described situation in adult rodents. It has been proposed that high levels of allopregnanolone during pregnancy and birth may have protective effects (e.g., reduce effects of anoxia) as well as produce a state of quiescence in the pregnant female and developing offspring [12-19].
What might be the mechanism by which neurosteroids, like allopregnanlone, have such effects to quell HPA responses? Allopregnanlone binds at high affinity to a specific binding site on GABA receptors, which are ubiquitous and can strongly contribute to inhibitory tone in the central nervous system. Indeed, these inhibitory effects in the brain (which we now understand to occur at least in part via GABA), were exploited with use of progesterone and its metabolites, like allopregnanlone, as surgical anesthetics [20]..Therefore, it is of interest what the hormonal profile of hibernating mammals is during different states (torpor, emergence from torpor, and arousal). We have assessed levels of metabolic, stress hormones, allopregnanolone and prohormones that typically co-vary with allopregnanolone (estradiol and progesterone). The role of stress hormones for allopregnanolone’s effects was assessed. As was hormone-mediated trophic factor (BDNF).
(Neuro)steroids can have protective effects and can enhance neural plasticity. In support, administration of estradiol, progesterone, and allopregnanolone can have beneficial effects in whole animal models of aging and neuronal compromise (i.e., seizure, cortical contusion, ischemia, and diabetic neuropathy models [2,21-30]. Moreover, allopregnanolone levels are lower among people with Alzheimer’s Disease versus controls or those with age-related dementia. A similar pattern of lower levels of allopregnanolone has been observed in a mutant mouse model of Alzheimer’s Disease which co-overexpresses mutant forms of amyloid precursor protein (APPswe) and presenilin [31]. Of interest, is the extent to which some of the differences in tau expression and phosphorylation (one hallmark of Alzheimer’s Disease) as well as synaptic changes, and protection from insults such as stroke, observed in hibernating animals, such as black bears, may reflect these protective or trophic effects of neurosteroids. As such, in the proposed experiments, one marker of neural plasticity, Brain-derived Neurotrophic Factor (BDNF, which can be measured in peripheral tissues, such as blood, as a proxy of brain levels) was determined in black bears in different states of hibernation: torpor, emergence from torpor and arousal.
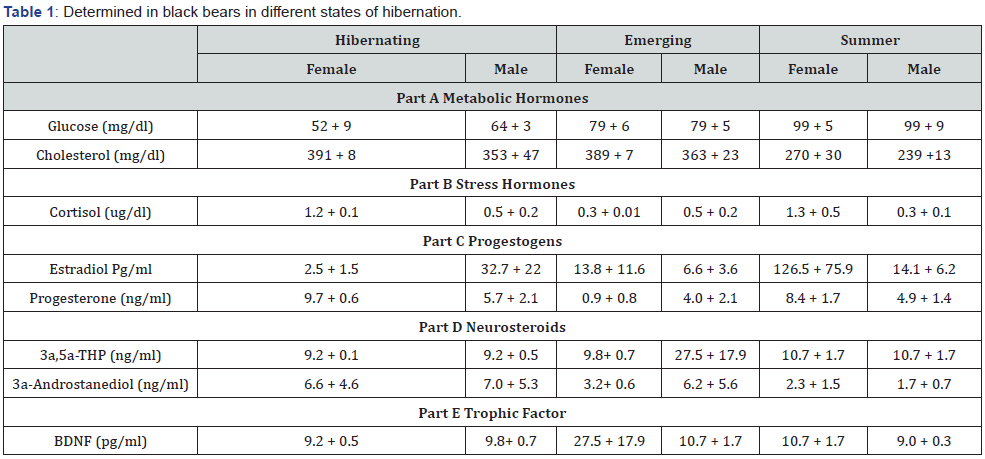
We observed the following results (Table 1).
a) Glucose levels were lower in hibernation (58 + 6) > < emergence (79 + 6) < > summer (99 + 7).
b) Cholesterol was higher during hibernation (372 + 27) and emergence (375 + 15) than in summer (255 + 22).
c) Cortisol was higher in females (1.3 + 0.3), than males (0.4 + 0.2) except during emergence (0.3 + 0.01), when it was at nadir.
d) Estradiol was lowest among females in hibernation (2.5 + 1.5) emergence 13.8 + 11.6 summer (126.5 + 75.9).
e) Progesterone was lower among emerging females (0.9 + 0.8) summer (8.4 + 1.7) hibernation (9.7 + 0.6); males did not vary by season (4.8 + 1.8).
f) Allopregnanolone was lower among hibernating (9.2 + 0.1) < emerging (9.8+ 0.7) < summer (10.7 + 1.7) female than male bears (15.8 + 6.7).
g) 3a-diol levels were lower during summer (2.0 + 1.3) >emergence (4.8 + 3.1)> hibernation (6.8 + 4.9) bears
h) BDNF levels were highest during emergence (19.1 + 9.8), summer (9.8 + 1.0) hibernation (9.5 + 0.6)
i) These data support that there may be sex-specific endocrine effects associated with emergence from hibernation among Ursus americanus. There were differences in metabolic, stress, sex and neurosteroid, as well as plasticity markers associated with emergence. We have observed similar differences among people with a subset of people with mTBI, who develop Type 2 diabetes as a result of weight gain and/or inactivity. Together, these finding suggest that development of metabolic syndrome and associated glucose dysregulation, cholesterol, sex and neurosteroids and trophic factors akin to hibernation or emergence may be biomarkers of mTBI associated with amotivational syndrome. This may allow better monitoring and treatment of such individuals. This is necessary because it has already been established that metabolic factors in brain function, links between type 2 Diabetes and Alzheimer’s, and the role of insulin in brain function, the hippocampus relies on insulin signaling, and measurement of the cognitive impact of recurrent hypoglycemia. McNay web site 1 Insulin affects spatial working memory.
Researchers inhibited GluT4-mediated glucose uptake and found that glucose utilization in the dorsal hippocampus of male rats during a hippocampally-mediated spatial working memory task. The data obtained suggested functional hippocampal GluT4 is not required for baseline hippocampal cognitive processing, but cognitive enhancement by supra-baseline insulin does. Thus, demonstrating the key role of GluT4 in transducing precognitive effects of elevated hippocampal insulin.
- Research Article
- Abstract
- Traumatic Brain Injury - Causes
- Traumatic brain injury-Incidence
- Traumatic Brain Injury - Diagnosis
- Trajectory of mTBI
- Symptoms Prognosis of Traumatic Brain Injury
- Diagnosis Symptomatology of TBI
- Hormones and TBI
- How does hypoglycemia impair cognition?
- Can you Enhance Cognitive Performance in Alzheimer’s?
- References
How does hypoglycemia impair cognition?
Cognition is impaired during hypoglycemia, but restoration of euglycemia is associated with improved hippocampally mediated memory. Increased glucocorticoid signaling during recurrent hypoglycemia produced changes in the dorsal hippocampus associated with hippocampus-dependent contextual learning. In addition to supporting cognition, these changes may reduce damage caused by repeated exposure to hypoglycemia.
- Research Article
- Abstract
- Traumatic Brain Injury - Causes
- Traumatic brain injury-Incidence
- Traumatic Brain Injury - Diagnosis
- Trajectory of mTBI
- Symptoms Prognosis of Traumatic Brain Injury
- Diagnosis Symptomatology of TBI
- Hormones and TBI
- How does hypoglycemia impair cognition?
- Can you Enhance Cognitive Performance in Alzheimer’s?
- References
Can you Enhance Cognitive Performance in Alzheimer’s?
Dyshomeostasis in zinc and copper have been observed in Alzheimer’s disease to cause profound cognitive impairment. Insulin therapy has been shown to enhance cognitive performance, but recent data suggests this may be due to the inclusion of zinc in insulin formation. Researchers looked to the spatial working memory of Sprague Dawley rats and found hippocampal zinc and copper, as well as plasma copper increased with age, but plasma zinc decreased. Zinc supplementation improved cognitive performance, suggesting its use in cognitive impairment disorders.
Obesity and type 2 diabetes are both associated with decreased metabolism in the brain. Researchers found lower levels of glucose in the brains of individuals with obesity and type 2 diabetes. The authors of the study believe this may be why these individuals have an increased risk of developing eating disorders and Alzheimer’s.
Insulin resistance, which can be caused by obesity and physical inactivity, is linked to a rapid decline in cognitive abilities. Both diabetic and non-diabetic patients with insulin resistance showed an accelerated cognitive decline in memory and executive function. Researchers used a drug, 2-DG, to mimic the ketogenic diet in rats. Neuroscientists were able to prevent the development of epileptic activity in mice following a traumatic brain injury, suggesting a change in metabolism is key to its therapeutic effects. These findings suggest that there is a bidirectional relationship between glucose, diabetes and traumatic brain injury and the manifestations of their neuroendocineopathies. This is similar to what has been reported in other neurodegenerative disorders such as epilepsy, Alzheimer’s and multiple sclerosis dementia.
We are interested in exploring the role of these changes in steroid levels in a natural model of stress and how this relates to brain plasticity. Neuropsychiatric disorders, such as depression, are considered to be highly stress-sensitive and impacted by circadian/seasonal effects. Moreover, neurosteroids play a role in depression. Progestogens can decrease depressive-like behavior among young and aged female rats or mice [32-37]. Men and women diagnosed with depression have lower levels of allopregnanolone in cerebrospinal fluid, and levels of allopregnanolone are increased with treatment with antidepressants, such as the selective serotonin reuptake inhibitors [38]. It has been proposed that depression may be related to the health of plasticity-prone areas of the brain, such as the hippocampus. Efficacy of antidepressant treatments has been associated with ability to enhance neural plasticity [39]. The notion is that by investigating metabolic, (neuro)steroids and BDNF in hibernating animals, important information about the role of these factors for stress-related and mTBI models will be elucidated.
- Research Article
- Abstract
- Traumatic Brain Injury - Causes
- Traumatic brain injury-Incidence
- Traumatic Brain Injury - Diagnosis
- Trajectory of mTBI
- Symptoms Prognosis of Traumatic Brain Injury
- Diagnosis Symptomatology of TBI
- Hormones and TBI
- How does hypoglycemia impair cognition?
- Can you Enhance Cognitive Performance in Alzheimer’s?
- References
References
- Morganti-Kossmann MC, Semple BD, Hellewell SC, Bye N, Ziebell JM (2019) The complexity of neuroinflammation consequent to traumatic brain injury: from research evidence to potential treatments. Acta Neuropathol 137(5): 731-755.
- Langlois JA, Rutland-Brown W, Wald MM (2006) The epidemiology and impact of traumatic brain injury: a brief overview. J Head Trauma Rehab 21: 375-378.
- Gean AD, Fischbein NJ (2010) Head trauma. Neuroimaging Clin N Am 20(4): 527-556.
- Faul M (2010) Traumatic brain injury in the United States: emergency department visits, hospitalizations, and deaths, 2002–2006.
- Greve MW, Zink BJ (2009) Pathophysiology of traumatic brain injury. Mount Sinai J N Y 76: 97-104.
- Cheng YJ, Karavolas HJ (1973) Conversion of progesterone to 5 alpha-pregnane-3,20-dione and 3 alpha-hydroxy-5 alpha-pregnan-20-one by rat medical basal hypothalami and the effects of estradiol and stage of estrous cycle on the conversion. Endocrinology 93(5): 1157-1162.
- Frye CA, Rhodes ME (2005) Estrogen-priming can enhance progesterone's anti-seizure effects in part by increasing hippocampal levels of allopregnanolone. Pharmacol Biochem Behav 81(4): 907-916.
- Frye CA, Vongher JM (1999) 3alpha,5alpha-THP in the midbrain ventral tegmental area of rats and hamsters is increased in exogenous hormonal states associated with estrous cyclicity and sexual receptivity. J Endocrinol Invest 22(6): 455-464.
- Barbaccia ML, Roscetti G, Trabucchi M, Purdy RH, Mostallino MC, et al. (1997) The effects of inhibitors of GABAergic transmission and stress on brain and plasma allopregnanolone concentrations. Br J Pharmacol 120(8): 1582-1588.
- Frye CA (2006) Progestins influence motivation, reward, conditioning, stress, and/or response to drugs of abuse. Pharmacol Biochem Behav 86(2): 209-219.
- Frye CA (2009) Neurosteroids' effects and mechanisms for social, cognitive, emotional, and physical functions. Psychoneuroendocrinology 34(Suppl 1): S143-161.
- Guo AL, Petraglia F, Criscuolo M, Ficarra G, Nappi RE, et al. (1995) Evidence for a role of neurosteroids in modulation of diurnal changes and acute stress-induced corticosterone secretion in rats. Gynecol Endocrinol 9(1): 1-7
- Patchev VK, Shoaib M, Holsboer F, Almeida OF (1994) The neurosteroid tetrahydroprogesterone counteracts corticotropin-releasing hormone-induced anxiety and alters the release and gene expression of corticotropin-releasing hormone in the rat hypothalamus. Neuroscience 62(1): 265-271.
- Patchev VK, Hassan AH, Holsboer DF, Almeida OF (1996) The neurosteroid tetrahydroprogesterone attenuates the endocrine response to stress and exerts glucocorticoid-like effects on vasopressin gene transcription in the rat hypothalamus. Neuropsychopharmacology 15(6): 533-440.
- Patchev VK, Almeida OF (1996) Gonadal steroids exert facilitating and "buffering" effects on glucocorticoid-mediated transcriptional regulation of corticotropin-releasing hormone and corticosteroid receptor genes in rat brain. J Neurosci 16(21): 7077-7084.
- Purdy RH, Morrow AL, Moore PH Jr, Paul SM (1991) Stress-induced elevations of gamma-aminobutyric acid type A receptor-active steroids in the rat brain. Proc Natl Acad Sci U S A 88(10): 4553-4557.
- Brunton PJ, Russell JA (2011) Neuroendocrine control of maternal stress responses and fetal programming by stress in pregnancy. Prog Neuropsychopharmacol Biol Psychiatry 35(5): 1178-1191.
- Frye CA, Bayon LE (1999) Prenatal stress reduces the effectiveness of the neurosteroid 3 alpha,5 alpha-THP to block kainic-acid-induced seizures. Dev Psychobiol 34(3): 227-234.
- Herbison AE (2001) Physiological roles for the neurosteroid allopregnanolone in the modulation of brain function during pregnancy and parturition. Prog Brain Res 133: 39-47.
- Hirst JJ, Palliser HK, Yates DM, Yawno T, Walker DW (2008) Neurosteroids in the fetus and neonate: potential protective role in compromised pregnancies. Neurochem Int 52(4-5): 602-610.
- Nguyen PN, Ross Young I, Walker DW, Hirst JJ (2004) Allopregnanolone in the brain and blood after disruption of the hypothalamic-pituitary-adrenal axis in fetal sheep. J Endocrinol 182(1): 81-88.
- Paris JJ, Frye CA (2011) Gestational exposure to variable stressors produces decrements in cognitive and neural development of juvenile male and female rats. Curr Top Med Chem 11(13): 1706-1713.
- Paris JJ, Brunton PJ, Russell JA, Walf AA, Frye CA (2011) Inhibition of 5α-reductase activity in late pregnancy decreases gestational length and fecundity and impairs object memory and central progestogen milieu of juvenile rat offspring. J Neuroendocrinol 23(11): 1079-1090.
- Paris JJ, Walf AA, Frye CA (2011) Cognitive performance of middle-aged female rats is influenced by capacity to metabolize progesterone in the prefrontal cortex and hippocampus. Brain Res1379: 149-163.
- Selye H (1941) On the Hormonal Activity of a Steroid Compound. Science 94(2430): 94.
- Asbury ET, Fritts ME, Horton JE, Isaac WL (1998) Progesterone facilitates the acquisition of avoidance learning and protects against subcortical neuronal death following prefrontal cortex ablation in the rat. Behav Brain Res 97(1-2): 99-106
- Cervantes M, González-Vidal MD, Ruelas R, Escobar A, Moralí G (2002) Neuroprotective effects of progesterone on damage elicited by acute global cerebral ischemia in neurons of the caudate nucleus. Arch Med Res 33(1): 6-14.
- Charalampopoulos I, Alexaki VI, Tsatsanis C, Minas V, Dermitzaki E, et al. (2006) Neurosteroids as endogenous inhibitors of neuronal cell apoptosis in aging. Ann N Y Acad Sci 1088: 139-152.
- Ciriza I, Carrero P, Azcoitia I, Lundeen SG, Garcia-Segura LM (2004) Selective estrogen receptor modulators protect hippocampal neurons from kainic acid excitotoxicity: differences with the effect of estradiol. J Neurobiol 61(2): 209-221.
- Frye CA, Walf AA (2008) Progesterone to ovariectomized mice enhances cognitive performance in the spontaneous alternation, object recognition, but not placement, water maze, and contextual and cued conditioned fear tasks. Neurobiol Learn Mem 90(1): 171-177.
- Leonelli E, Bianchi R, Cavaletti G, Caruso D, Crippa D, et al. (2007) Progesterone and its derivatives are neuroprotective agents in experimental diabetic neuropathy: a multimodal analysis. Neuroscience 144(4): 1293-1304.
- Nilsen J, Brinton RD (2002) Impact of progestins on estrogen-induced neuroprotection: synergy by progesterone and 19-norprogesterone and antagonism by medroxyprogesterone acetate. Endocrinology 143(1): 205-212.
- Roof RL, Duvdevani R, Braswell L, Stein DG (1994) Progesterone facilitates cognitive recovery and reduces secondary neuronal loss caused by cortical contusion injury in male rats. Exp Neurol 129(1): 64-69.
- Sayeed I, Guo Q, Hoffman SW, Stein DG (2006) Allopregnanolone, a progesterone metabolite, is more effective than progesterone in reducing cortical infarct volume after transient middle cerebral artery occlusion. Ann Emerg Med 47(4): 381-389.
- Frye CA, Walf AA (2008) Effects of progesterone administration and APPswe+PSEN1Deltae9 mutation for cognitive performance of mid-aged mice. Neurobiol Learn Mem 89(1): 17-26.
- Frye CA, Walf AA, Rhodes ME, Harney JP (2004) Progesterone enhances motor, anxiolytic, analgesic, and antidepressive behavior of wild-type mice, but not those deficient in type 1 5 alpha-reductase. Brain Res 1004(1-2): 116-124.
- Frye CA, Sumida K, Dudek BC, Harney JP, Lydon JP, et al. (2006) Progesterone's effects to reduce anxiety behavior of aged mice do not require actions via intracellular progestin receptors. Psychopharmacology (Berl) 186(3): 312-322.
- Frye CA, Rhodes ME (2006) Infusions of 5alpha-pregnan-3alpha-ol-20-one (3alpha,5alpha-THP) to the ventral tegmental area, but not the substantia nigra, enhance exploratory, anti-anxiety, social and sexual behaviours and concomitantly increase 3alpha,5alpha-THP concentrations in the hippocampus, diencephalon and cortex of ovariectomised oestrogen-primed rats. J Neuroendocrinol 18(12): 960-975.
- Frye CA, Walf AA (2004) Hippocampal 3alpha,5alpha-THP may alter depressive behavior of pregnant and lactating rats. Pharmacol Biochem Behav 78(3): 531-540.






























