The Study of Gut Microbiota Pattern in Anorexia Nervosa Patients
Taha Anbara*
Department of Surgery, Erfan Niayesh Hospital, Iran
Submission: November 22, 2022; Published: December 19, 2022
*Corresponding author: Taha Anbara MD, General and laparoscopic surgeon, Department of Surgery, Erfan Niayesh Hospital, PC 1476919491, No. 17, Bahar Intersection, Imam Hossein St., after Kabiri Tameh Blvd., Niayesh Gharb Highway, Tehran, Iran
How to cite this article: Anbara T. The Study of Gut Microbiota Pattern in Anorexia Nervosa Patients. Curre Res Diabetes & Obes J 2022; 16(2): 555934.DOI: 10.19080/CRDOJ.2022.16.555934
Abstract
Introduction: Anorexia nervosa (AN) is a common eating disorder associated with weight, physiology and the gut microbiome. The main aim of this study was to gather taxonomical profile changes of intestinal bacteria in patients who suffer from AN and suggest possible treatment and prevention approaches for future studies.
Method: We had a review of the literature published between 2000 and 2021 in the databases of Web of Science, PubMed and the Scopus through the main keywords including eating disorders, anorexia nervosa, probiotic, microbiota, microbiome, gut pattern, and gut-brain axis.
Results: Based on reports, a reduction in gut bacteria richness such as enriched Coriobacteriaceae, which is implicated in lipid metabolism, Clostridium clusters, Roseburia, archaea, and Methanobrevibacter smithii in subjects were significantly higher compared to control groups.
Conclusion: This study provided evidences of intestinal dysbiosis in AN patients and sheds light on possible treatment and prevention approaches for AN patients such as nutritional interventions considering paraprobiotics, postbiotics, probiotics and prebiotics or dietary supplements as an important component for AN therapy.
Keywords: Anorexia nervosa; Eating disorders; Gut microbiome; Treatment
Abbreviations: AN: Anorexia Nervosa; BN: Bulimia Nervosa; GLP-1: Glucagon-like Peptide-1; SCFAs: Short Chain Fatty Acids; GABA: Gamma-Aminobutyric Acid; FMT: Fecal Microbiota Transplantation
Introduction
Human eating disorders such as anorexia nervosa (AN) is an increasing psychiatric disorder among citizens of modern societies [1,2] and is characterized by a series of psychological behaviors and clinical variables such as extreme dietary restriction resulting in a sustained low weight, imbalanced homeostasis energy, impaired brain and reduced gut function in patients [3].
Prevalence of eating disorders increased globally from 3.4% to 7.8% from 2000 to 2018 [4]. However eating disorders are traditionally considered to affect mainly women, men represent a growing proportion of subjects suffering from AN and bulimia nervosa (BN) [2,4]. Based on recent studies, around 1.5% of people suffer from AN in the world [5-7].
As far as the impact of eating disorders on health is concern, due to direct influence of an eating disorder, one person dies every hour [8], which AN is the deadliest mental illness caused by malnutrition among eating disorders with 56 times higher incidence of suicide attempts [9]. In addition, Mood disorders, such as major depression, anxiety disorders, obsessive-compulsive disorder, post-traumatic stress disorder, resulting in substance use disorder [10], beside electrolyte abnormalities, and organ damages including heart attacks, kidney failures, the gut problems, neurological disorders and reduction in total volume of brain are the most frequent health risks of such eating disorders [11,12]. The recent reports claim that abnormal composition of the intestinal microbiome may be a crucial factor supporting cachexia of AN patients [13,14]. We aim to gather the most recent surveys on the changes in the gut microbiome composition in AN patient and the role of the intestinal bacteria in the pathogenesis of AN. In addition, we tried to gather possible treatment and prevention approaches for AN patient. For this purpose, a review of the literature published between 2000 and 2021 in the databases of Web of Science, PubMed and the Scopus has been performed by importing keywords: eating disorders, anorexia nervosa, probiotic, microbiota, microbiome, gut pattern, and gutbrain axis.
The Gut Brain Axis: Definition, and Functions
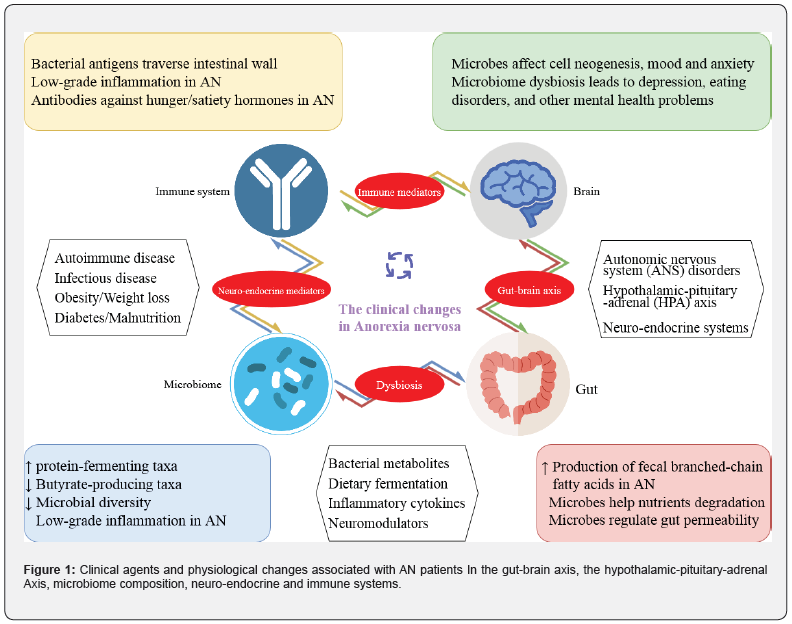
The gastrointestinal tract colonized with the gut microbiome [15], referring to the bidirectional communication between the gut and the brain [16], which is crucial in mental health. Importance of gut microbiota have been illustrated on weight gain [17], digestive system, immune system, appetite hormones and autoantibody against them in have been reported in previous studies [18]. The gut-brain axis uses neural, immune, hormonal and microbial factors messages for the communication between the gut and the brain [2,17]. For instance, L cells, and endocrine cells, which release PYY, glucagon-like peptide-1 (GLP-1) and GLP-2, are stimulated by short chain fatty acids (SCFAs), which are generated by particular microbes [19,20]. SCFAs stimulate L cells via activating G protein coupled receptors such as Gpr41 [21]. One the other side, gut-derived hormones are undeniable links between the gut microbiome and physiological responses [22]. Furthermore, the taxonomic profile of the gut bacteria influences the profile of metabolites in the brain [15]. The gut microbiome is also able to generate neurotransmitters and neuromodulators such as 5-hydroxytryptamine, dopamine noradrenaline, acetylcholine, gamma-aminobutyric acid (GABA) [17]. Numerous intestinal microbes including Lactobacillus, Bacteroides, Helicobacter pylori, Escherichia coli and Candida species contain proteins that have amino acid sequences identical to these appetite-regulating peptides [23]. The circulating levels of autoantibodies against alpha-melanocyte-stimulating hormone, which are increased in AN, correlate with the psychobehavioural abnormalities of these eating disorders [24]. Figure 1 illustrates more details on the clinical agents and physiological changes involved in the communications between the gut microbiome and brain in AN patients.
The Role of the Gut Microbiota in AN
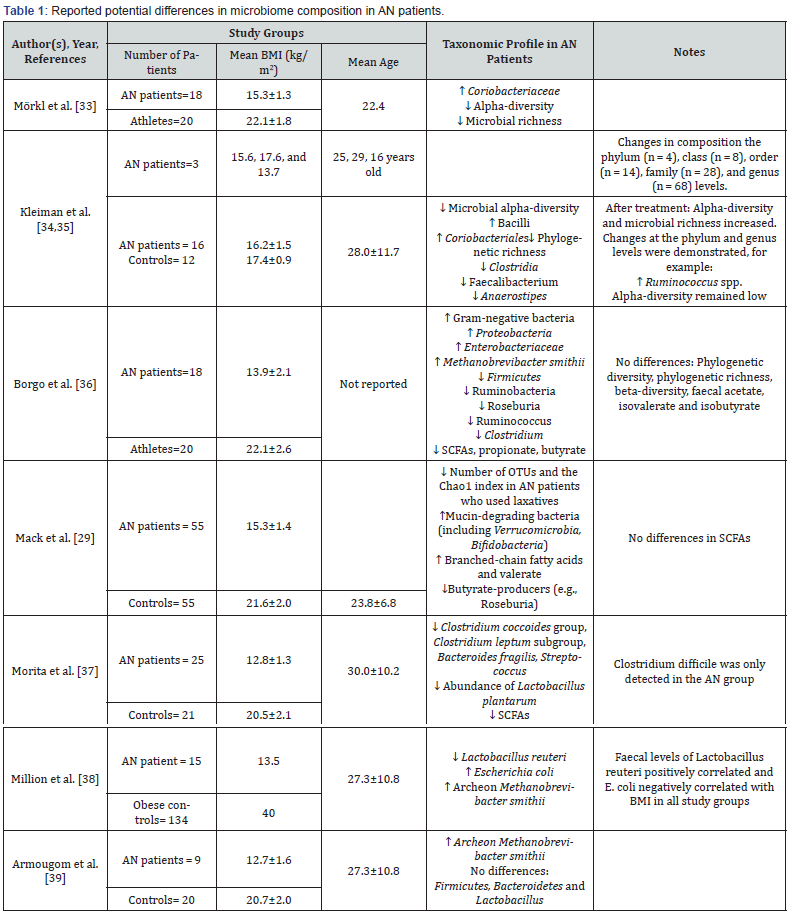
The intestinal microbiota control the formation of IgG and IgA autoantibodies against neuropeptides involved in appetite control including lpha-melanocyte-stimulating hormone, NPY, PYY, agouti-related protein, ghrelin, leptin and some other neuropeptides/peptides [23,25,26]. Researchers reported a reduction in gut bacteria richness in AN subjects, in which the enriched Coriobacteriaceae was significantly dominant [27]. Coriobacteriaceae colonize the human gastrointestinal tract and are implicated in lipid metabolism [28]. Moreover, the taxa corresponding to various Clostridium clusters, Roseburia, archaea, and Methanobrevibacter smithii in an subjects were significantly higher compared to control groups [29,30]. Methanobrevibacter smithii is most abundant bacteria in the intestines of people with malnutrition, which enables them to effectively metabolize nutrients to calories [30]. In addition, Bacteroides and Firmicutes bacteria and those archaea species enhance the fermentation yield of indigestible fiber contents to SCFAs [31], which play a critical role in neuro-immunoendocrine regulation [32]. Table 1 presents studies related to the taxonomical profile changes in AN patient. There are conceivable reasons for a synergistic effect of the gut microbiota in AN patient. In addition, several antidepressants may have antimicrobial effects [40], which could indeed be responsible for the paradoxical results that studies have found in AN patient. More studies are required to find out in more detail the influence of intestinal bacteria on prescription of antidepressant medications in AN patient.
Possible Therapeutic Approaches for AN Patients
Unfortunately, the above-mentioned abnormalities do not translate as yet for effective methods of treatment for AN patient. However, the knowledge about the gut-brain interaction in AN patients is constantly growing and the results are very promising so far, the findings are not precise in some sections and many questions remain unanswered that must be clarified before any recommendations for AN treatment and prevention. On the other hand, dietary behavior is an important factor affecting the gut microbiome composition, the clinical impacts of diet, which are typically made quickly in patients with AN, should be examined in more detail. The nutritional interventions considering paraprobiotics, postbiotics, probiotics and prebiotics or dietary supplements could become an important additional component of multimodal AN therapy in the future. As far as fecal microbiota transplantation (FMT) as a treatment approach for AN is concern, a patient who had been suffering for 2years was able to gain weight of 6.3kg and led to the improvement of gut barrier function after FMT from a healthy control subject of normal weight [41]. Furthermore, in another patient, decreased the fungal alpha diversity, bacterial species richness and enhanced gut microbiome evenness in the patient were observed [42]. Overall, the relatively young research field of gut-brain interaction in the context of AN appears extremely promising. It might help to also consider AN and its underlying mechanisms from a nutritional and microbiome-gut-brain-axis perspective in the existing biopsychosocial model. Appropriately specifically developed individual nutritional therapeutic interventions could complement the previous multimodal therapy.
Conclusion
In this review article, we gathered the most recent published surveys on the changes of taxonomic profile of microbiome composition in AN patient and the possible approaches for treatment and prevention of heating disorders considering diet supplements, probiotics, probiotics, postbiotics, and paraprobiotics as well as the outcomes on FMT in AN patients.
References
- Trinh S, Kogel V, Voelz C, Schlösser A, Schwenzer C, et al. (2021) Gut microbiota and brain alterations in a translational anorexia nervosa rat model. J Psychiatr Res 133: 156-165.
- Tabasi M, Anbara T, Siadat SD, Khezerloo JK, Elyasinia F, et al. (2020) Socio-demographic Characteristics, Biochemical and Cytokine Levels in Bulimia Nervosa Candidates for Sleeve Gastrectomy. Arch Iran Med 23(1).
- Leyrolle Q, Cserjesi R, Mulders MDGH, Zamariola G, Hiel S, et al. (2021) Specific gut microbial, biological, and psychiatric profiling related to binge eating disorders: A cross-sectional study in obese patients. Clin Nutr 40(4): 2035-2044.
- Galmiche M, Déchelotte P, Lambert G, Tavolacci MP (2019) Prevalence of eating disorders over the 2000-2018 period: a systematic literature review. Am J Clin Nutr 109(5): 1402-1413.
- Kazdin AE, Fitzsimmons‐Craft EE, Wilfley DE (2017) Addressing critical gaps in the treatment of eating disorders. Int J Eat Disord 50(3): 170-1
- Hudson JI, Hiripi E, Pope Jr HG, Kessler RC (2007) The prevalence and correlates of eating disorders in the National Comorbidity Survey Replication. Biol Psychiatry 61(3): 348-358.
- Aykut MK, Bilici S (2021) The relationship between the risk of eating disorder and meal patterns in University students. Eat Weight Disord Anorexia. Bulim Obes 1-9.
- Abraham S, Llewellyn-Jones D (2001) Eating disorders: The facts. Oxford University Press, USA.
- Bulik CM, Thornton L, Pinheiro AP, Plotnicov K, Klump KL, et al. (2008) Suicide attempts in anorexia nervosa. Psychosom Med 70(3): 378-383.
- Tagay S, Schlottbohm E, Reyes-Rodriguez ML, Repic N, Senf W (2014) Eating disorders, trauma, PTSD, and psychosocial resources. Eat Disord 22(1): 33-49.
- Titova OE, Hjorth OC, Schiöth HB, Brooks SJ (2013) Anorexia nervosa is linked to reduced brain structure in reward and somatosensory regions: a meta-analysis of VBM studies. BMC Psychiatry 13(1): 1-11.
- Himmerich H, Kan C, Au K, Treasure J (2020) Pharmacological treatment of eating disorders, comorbid mental health problems, malnutrition and physical health consequences. Pharmacol Ther 107667.
- Butler MJ, Perrini AA, Eckel LA (2021) The Role of the Gut Microbiome, Immunity, and Neuroinflammation in the Pathophysiology of Eating Disorders. Nutrients 13(2): 500.
- Ghenciulescu A, Park RJ, Burnet PWJ (2021) The Gut microbiome in Anorexia nervosa: friend or foe? Front Psychiatry 11: 1463.
- Madison AA, Kiecolt-Glaser JK (2021) The gut microbiota and nervous system: Age-defined and age-defying. In: Seminars in Cell & Developmental Biology. Elsevier.
- Kheirvari M, Dadkhah Nikroo N, Jaafarinejad H, Farsimadan M, Eshghjoo S, et al. (2020) The advantages and disadvantages of sleeve gastrectomy; clinical laboratory to bedside review. Heliyon 6(2): e03496.
- Tabasi M, Ashrafian F, Khezerloo JK, Eshghjoo S, Behrouzi A, et al. (2019) Changes in Gut Microbiota and Hormones After Bariatric Surgery: a Bench-to-Bedside Review. Obes Surg.
- Fetissov SO (2017) Role of the gut microbiota in host appetite control: bacterial growth to animal feeding behaviour. Nat Rev Endocrinol 13(1): 11.
- Alhabeeb H, AlFaiz A, Kutbi E, AlShahrani D, Alsuhail A, et al. (2021) Gut Hormones in Health and Obesity: The Upcoming Role of Short Chain Fatty Acids. Nutrients 13(2): 481.
- Ronveaux CC, Tomé D, Raybould HE (2015) Glucagon-like peptide 1 interacts with ghrelin and leptin to regulate glucose metabolism and food intake through vagal afferent neuron signaling. J Nutr [Internet]. 145(4): 672-680.
- Xiong Y, Miyamoto N, Shibata K, Valasek MA, Motoike T, et al. (2004) Short-chain fatty acids stimulate leptin production in adipocytes through the G protein-coupled receptor GPR41. Proc Natl Acad Sci 101(4): 1045-1050.
- B Herpertz-Dahlmann B, Seitz J, Baines J (2017) Food matters: how the microbiome and gut-brain interaction might impact the development and course of anorexia nervosa. Eur Child Adolesc Psychiatry 26(9): 1031-1041.
- Fetissov SO, Sinno MH, Coëffier M, Bole-Feysot C, Ducrotté P, et al. (2008) Autoantibodies against appetite-regulating peptide hormones and neuropeptides: putative modulation by gut microflora. Nutrition 24(4): 348-359.
- Roubalová R, Procházková P, Papežová H, Smitka K, Bilej M, et al. (2020) Anorexia nervosa: Gut microbiota-immune-brain interactions. Clin Nutr 39(3): 676-684.
- Gorwood P, Blanchet-Collet C, Chartrel N, Duclos J, Dechelotte P, et al. (2016) New insights in anorexia nervosa. Front Neurosci 10: 256.
- Pichard C, Laviano A, Meguid MM (2008) Of autoantibodies and single nucleotide polymorphisms: A brave new world? Curr Opin Clin Nutr Metab Care 11(4): 398-399.
- Mörkl S, Lackner S, Müller W, Gorkiewicz G, Kashofer K, et al. (2017) Gut microbiota and body composition in anorexia nervosa inpatients in comparison to athletes, overweight, obese, and normal weight controls. Int J Eat Disord 50(12): 1421-1431.
- Clavel T, Charrier C, Braune A, Wenning M, Blaut M, et al. (2009) Isolation of bacteria from the ileal mucosa of TNFdelta ARE mice and description of Enterorhabdus mucosicola nov., sp. nov. Int J Syst Evol Microbiol 59(7): 1805-1812.
- Mack I, Cuntz U, Grämer C, Niedermaier S, Pohl C, et al. (2016) Weight gain in anorexia nervosa does not ameliorate the faecal microbiota, branched chain fatty acid profiles and gastrointestinal complaints. Sci Rep 6(1): 1-16.
- Walker A (2007) Say hello to our little friends. Nat Rev Microbiol 5(8): 572-573.
- Hoffmann C, Dollive S, Grunberg S, Chen J, Li H, et al. (2013) Archaea and fungi of the human gut microbiome: correlations with diet and bacterial residents. PLoS One 8(6): e66019.
- Mörkl S, Lackner S, Müller W, Gorkiewicz G, Kashofer K, et al. (2017) Gut microbiota and body composition in anorexia nervosa inpatients in comparison to athletes, overweight, obese, and normal weight controls. Int J Eat Disord 50(12): 1421-1431.
- Kleiman SC, Glenny EM, Bulik‐Sullivan EC, Huh EY, Tsilimigras MCB, et al. (2017) Daily changes in composition and diversity of the intestinal microbiota in patients with anorexia nervosa: a series of three cases. Eur Eat Disord Rev 25(5): 423-42
- Susan C Kleiman, Hunna J Watson, Emily C Bulik-Sullivan, Eun Young Huh, Lisa M Tarantino, et al. (2015) The Intestinal Microbiota in Acute Anorexia Nervosa and during Renourishment: Relationship to Depression, Anxiety, and Eating Disorder Psychopathology. Psychosom Med 77(9): 969-981.
- Borgo F, Riva A, Benetti A, Casiraghi MC, Bertelli S, et al. (2017) Microbiota in anorexia nervosa: The triangle between bacterial species, metabolites and psychological tests. PLoS One 12(6).
- Chihiro Morita, Hirokazu Tsuji, Tomokazu Hata, Motoharu Gondo, Shu Takakura, et al. (2015) Gut Dysbiosis in Patients with Anorexia Nervosa. PLoS One 10(12):
- Million M, Angelakis E, Maraninchi M, Henry M, Giorgi R, et al. (2013) Correlation between body mass index and gut concentrations of Lactobacillus reuteri, Bifidobacterium animalis, Methanobrevibacter smithii and Escherichia coli. Int J Obes 37(11): 1460-1466.
- Fabrice Armougom, Mireille Henry, Bernard Vialettes, Denis Raccah, Didier Raoult (2009) Monitoring bacterial community of human gut microbiota reveals an increase in Lactobacillus in obese patients and Methanogens in anorexic patients. PLoS One 4(9): e7125.
- Silva YP, Bernardi A, Frozza RL (2020) The role of short-chain fatty acids from gut microbiota in gut-brain communication. Front Endocrinol (Lausanne) 11: 25.
- González-Pérez A, Rodríguez LAG (2005) Breast cancer risk among users of antidepressant medications. Epidemiology 16(1): 101-105.
- Navarro-Tapia E, Almeida-Toledano L, Sebastiani G, Serra-Delgado M, García-Algar Ó, et al. (2021) Effects of microbiota imbalance in anxiety and eating disorders: probiotics as novel therapeutic approaches. Int J Mol Sci 22(5): 2351.
- Prochazkova P, Roubalova R, Dvorak J, Tlaskalova-Hogenova H, Cermakova M, et al. (2019) Microbiota, microbial metabolites, and barrier function in a patient with anorexia nervosa after fecal microbiota transplantation. Microorganisms 7(9): 338.






























