Appraisal of an Oral Health Care Programme to Improve Oral Health Status of Diabetic Patients: Evidence from Sri Lanka
Dhanitha Thabrew1, Irosha Perera2*, Suranga Dolamulla3, Dushan Baddage1 and Manosha Perera4
1Oral & Maxillofacial Unit D, National Dental Hospital, Sri Lanka
2Preventive Oral Health Unit, National Dental Hospital, Sri Lanka
3Directorate of Laboratory Services, Ministry of Health, Sri Lanka
4Alumnus School of Dentistry and Oral Health, Griffith University, Sri Lanka
Submission: November 18, 2022; Published: December 02, 2022
*Corresponding author: Irosha Perera, Preventive Oral Health Unit, National Dental Hospital (Teaching) Sri Lanka, Ward Place, Colombo 7, Sri Lanka
How to cite this article: Dhanitha T, Irosha P, Suranga D, Dushan B, Manosha P. Appraisal of an Oral Health Care Programme to Improve Oral Health Status of Diabetic Patients: Evidence from Sri Lanka. Curre Res Diabetes & Obes J 2022; 16(2): 555932.DOI: 10.19080/CRDOJ.2022.16.555932
Abstract
Sri Lanka is a low-income country currently grappling with an unprecedented economic crisis and a rising burden of non-communicable diseases dominated by diabetes and pre-diabetes. The economic crisis has negatively impacted once strong public health care system of the country which offered free of-charge services. Therefore, optimal management of diabetic complications through healthy lifestyle habits has become more important than ever before. The bi-directional relationship of diabetes and periodontal diseases is well-known but not translated into clinical practices in diabetic management. In general, the oral health statuses of diabetic patients are often neglected in providing comprehensive diabetic care across the globe. Consequently, diabetic patients carry a high burden of oral diseases that could interfere with their optimal glycemic control and aggravate diabetic complications. Against this backdrop, this short report aims to appraise the service delivery of an oral health programme of a premier, multispecialty tertiary care public dental hospital in Sri Lanka to improve the oral health status of a group of diabetic patients.
Keywords: Diabetic complications; Oral health; Chronic inflammatory; Glycaemic control
Introduction
Sri Lanka is a developing country currently grappling with an unprecedented economic crisis which has impacted negatively on public health care delivery [1] and a rising burden of diabetes and pre-diabetes [2]. The public health delivery model of the country that offered health care services, treatment, medicines and investigations free of charge at the point of service delivery gained recognition as efficient, effective and pro-poor [3,4]. Government expenditure as a share of GDP has remained static but low around 1.7% during the period from 2013 to 2016 [3]. This was relatively low by regional standards which were constrained attributed to very low levels of government revenue whilst out-of-pocket expenditure (OOPE) accounted for about 40% of total health expenditure [4]. However, prevailing economic crisis and its negative impact has resulted in many impediments in availability of and accessibility to drugs and investigations delivered by public sector.
There is convincing evidence rising diabetes burden in Sri Lanka. The age-sex standardized prevalence (95% confidence interval) of diabetes for Sri Lankans aged >or= 20 years was 10.3% (9.4-11.2%) [males 9.8% (8.4-11.2%), females 10.9% (9.7-12.1%) [2]. Thirty-six per cent (31.9-40.1%) of all diabetic subjects were previously undiagnosed. Diabetes prevalence was higher in the urban population compared with rural [16.4% (13.8-19.0%) vs. 8.7% (7.8-9.6%) [2]. The prevalence of overall, urban and rural pre-diabetes was 11.5% (10.5-12.5%), 13.6% (11.2-16.0%) and 11.0% (10.0-12.0%), respectively. Overall, 21.8% (20.5-23.1%) presented with some form of dysglycaemia [2]. The projected diabetes prevalence for the year 2030 was 13.9%. Therefore, one in five adults in Sri Lanka deemed having either diabetes/ pre-diabetes whilst one-third of them being undiagnosed [2]. The prevalence of diabetes mellitus in Jaffna district (Northern Sri Lanka) was 16.4% (95% CI: 13.3- 19.9); in males 19.6% (95% CI: 14.6-25.4) and in females 13.9% (95% CI: 10.1-18.5). Of the diabetics, 27.4% were previously undiagnosed [5]. A more recent study conducted among Colombo urban population revealed an overall prevalence rate of 27.6% (95% CI: 23.7-31.4). The prevalence rate of diabetes among 18-40-year-olds was 12.4% (95% CI: 6.4 -18.4), 36.1% (95% CI: 29.8 – 42.4) among 41 – 60-year-olds and 48.3% (95% CI: 40.7 – 55.8) among those who were aged >60. Pre-diabetes was detected in 30.3% (95% CI 25.9- 34.8) of the population (with either an HbA1c of 5.7-6.4%, FPG of 110-125 mg/dl or 2 Hr PPG of 140-199 mg/dl). Cumulative prevalence of diabetes and prediabetes in the population was as high as 57.9% [6].
The high burden of periodontitis among diabetic patients and the bi-directional relationship between both diseases is well-established [7,8]. Periodontitis, the chronic inflammatory polymicrobial disease of the periodontium and tooth supporting structures, is linked to diabetes in two ways. Patients with poorly controlled diabetes are at a three-to-four-fold risk to develop severe periodontitis [7-9]. On the other hand, there is evidence to suggest that high proportion and severity of periodontitis and increased inflamed surface area of the periodontium is linked to poor glycaemic control and microvascular complications [10]. A study conducted among 285 individuals with type 2 diabetes mellitus in urban Sri Lanka revealed a compromised periodontal status compared with non-diabetic controls [11,12].
Recent systematic review and a meta-analysis reported an increased risk for diabetic complications including microvascular, macrovascular and death in the presence of periodontal disease [13]. Higher risks for diabetic retinopathy (odds ratios: 2.8-8.7), neuropathy (3.2-6.6), nephropathy (1.9-8.5), cardiovascular complications (1.28-17.7) and mortality (2.3-8.5) were reported for people with diabetes with periodontitis compared to those with diabetes who have no periodontitis [13]. However, such evidence has not transformed to clinical practices in comprehensive management of diabetes even in developed countries. Against this backdrop, this short report aims to appraise the service delivery of an oral health programme of a premier, multispecialty tertiary care hospital in Sri Lanka to improve the oral health status of a group of diabetic patients.
Methodology
A pilot project was conducted in 2019 Preventive in selected diabetes clinics of National Hospital Sri Lanka (NHSL) which is the premier, multispecialty, tertiary care teaching hospital in the country. Dental Surgeons attached to the Preventive Oral Health Unit of National Dental Hospital (Teaching) Sri Lanka, which is the premier, multispecialty, tertiary care public dental hospital in Sri Lanka. The findings of the rapid oral health status assessment conducted among randomly selected 40 diabetic patients attended those clinics Oral Health Unit of National Dental Hospital (Teaching) Sri Lanka were published previously. Without interfering with patient care services busy, crowded diabetic conducts few outreach oral health programmes for patients attending selected diabetic clinics of NHSL, patients were attended while they were seated at the waiting area. Brief awareness of importance of better oral health for diabetic patients was done, followed by rapid oral health screening and referral of diabetic patients to the Preventive Oral Health Unit. As two hospitals are located in close proximity, patients were allowed to make their visits to oral health care whilst attending to diabetic care.
Once the diabetic patients attended the Preventive Oral Health Unit, they were provided with a thorough oral health examination, tailored oral health awareness, oral hygiene advice, dietary advice and required dental treatment. A special data collection form was filled each diabetic patient, comprising basic socio-demographic information, data on medical condition, tooth brushing and dietary habits and oral health status pertaining to dental caries, oral hygiene status and periodontal health status.
Scaling was provided at the POHU, with fluoride gel applications, simple fillings and uncomplicated extractions of teeth with poor prognosis. Dental treatment was provided based on the level glycaemic control of the patients and considering presence of diabetic complications and presence of other comorbidities. Those who need endodontic treatment and specialized surgical treatment were referred to Restorative Dental Units and Oral & Maxillofacial Units. Patient statistics were extracted from the diabetic patient data base of Preventive Oral Health Unit, for the period from June to December 2019 and patient attendance from January to October 2022.
Main Outcome Measures
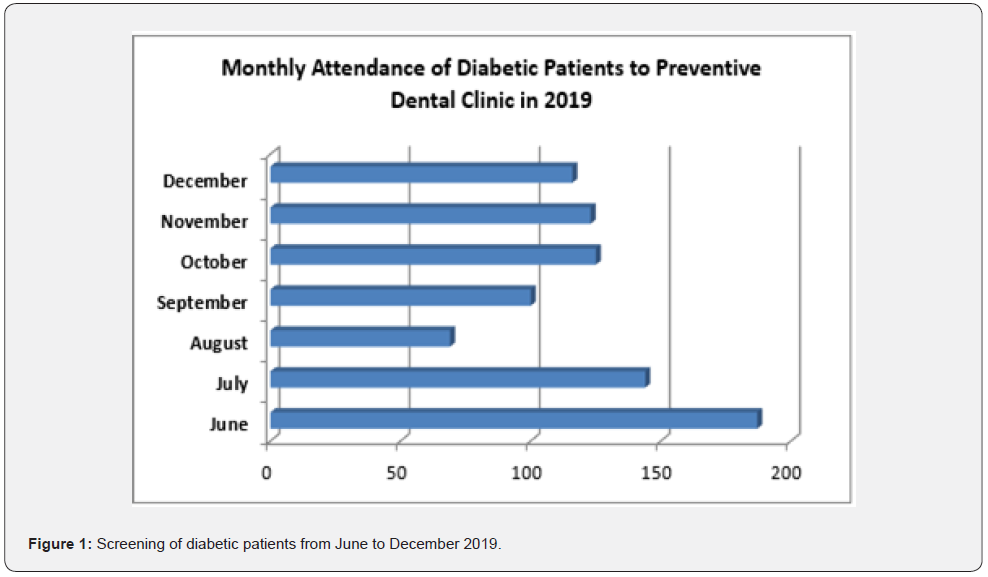
Screening statistics of diabetic patients attended selected diabetic clinics of NHSL, from June to December 2019 is depicted in figure 1. The total number of programmes conducted was 30 that screened a total of 864 diabetic patients. Of 864 diabetic patients whom were screened 413 were referred for oral health care at Preventive Oral Health Unit of National Dental Hospital. Of them, only 201 diabetic patients attended the preventive dental clinic.
Referral Rate 413/864x100= 47.8
Compliance Rate 201/413x100=48.6
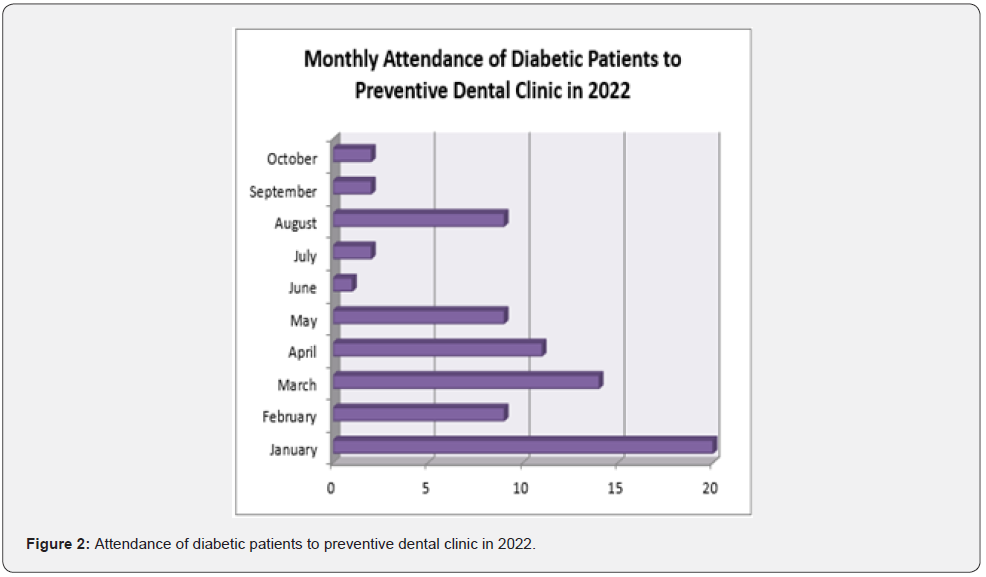
Therefore, the referral rate was 47.8% and compliance rate was 48.6% among diabetic patients. As shown in figure 2, the number of diabetic patients attended the preventive dental clinic up to October in the year of 2022, ranged from 20 to 1 whilst the total number was 77.
Discussion
Oral health gained recognition as a neglected domain of routine diabetic care [9]. Despite, high prevalence of oral conditions such as dry mouth, periodontitis, dento-alveolar infections, oral candidiasis etc. among diabetic patients, little is known about oral health care provided in diabetic settings. There is convincing evidence of lack of interest among diabetic care providers on oral health diabetic patients, predominantly attributed to time constraints and lack of oral health knowledge [15]. Similarly, the knowledge bi-directional relationship of diabetes and periodontal diseases and the importance of oral health for improved diabetic outcomes among diabetic patients is far from satisfactory [16-18]. Against this backdrop, the oral health programme for diabetic patients conducted by the preventive oral health unit of National Dental Hospital (Teaching) Sri Lanka could be considered as a commendable endevour.
Sri Lanka is currently grappling with a dollar crisis stemming from devastating economic crisis that has negatively impacted on public health care delivery [1]. The public health care delivery model of the country that offered general and specialized health carefree of charge at the point of service delivery, has now become crippled with resource constraints and drug shortages. The routine diabetic care provided by diabetic clinics in public hospitals, as revealed by a study conducted in 2000, included measuring blood glucose levels, testing for proteinuria and screening for hyperlipidaemia, hypertension, and eye disease [19]. Referral for oral health screening has never been a part of such care in Sri Lanka, like many other developing and developed countries across the world [9]. The same study revealed that with the availability of three doctors, the average consultation time was four minutes per patient. The average score for knowledge regarding management and complications, obtained from analysis of the questionnaire, was 5.3 out of a maximum of 9.0 points. According to authors, as emerged from the findings, the quality of care of diabetic patients did not meet the standards that should be expected. Lack of good organization and poor planning of resource utilization were identified as major causes [19]. However, over crowdedness of diabetic clinic adding a high burden of limited numbers of service providers could be another important reason for less optimal quality of care. An increase in funding was suggested by the authors for implementing the improvements suggested [19]. Nevertheless, prevailing economic crisis with persistent drug shortages and health staff shortages could have further reduced the quality of diabetic care provided by public hospitals in Sri Lanka.
Our previous assessment reported poor oral hygiene status of a group of 40-diabetic patients attended diabetic clinic of NHSL compounded by their poor glycaemic control and complications of diabetes [20]. Further, there is evidence of comprised periodontal health status of Sri Lankan patients. Therefore, referral of diabetic patients for oral health care has become a neglected necessity. However, our findings revealed only less than 50% compliance for oral health care. The Western Province of Sri Lanka has the highest prevalence of diabetes mellitus (DM) (18.6%) in the country, nevertheless, previous studies found a significant gap in diabetic retinopathy screening service uptake [21]. Lack of knowledge of both the condition and the need for screening were identified as key barriers to access those services. Socio-cultural factors in the family environment, economic reasons and institutional factors also emerged as important barriers. Service-related factors such as long waiting times at the eye-clinic and discomfort from the procedure were among other identified barriers [21]. Therefore, when such findings are applied to improving the compliance for referral for oral health care, provision of prompt and non-invasive preventive oral health care for diabetic patients comprising customized oral hygiene and brushing instructions, dietary counseling, professional fluoride application, simple fillings, ultrasonic scaling etc. have the potential to harness to improve patients’ compliance. However, convincing the diabetic patients on the bi-directional relationship of diabetes and oral health underpinned by periodontal health status and importance of good oral health status for optimal glycaemic need hard effort and tailored approaches in Sri Lankan socio-cultural context.
Our findings demonstrate marked reductions in attendance of diabetic patients at the preventive dental clinic in 2022, compared to 2019. The Covid-19 global pandemic that affected Sri Lanka with a breakdown of routine health care services in the years of 2020 and 2021 could be a plausible explanation for this reduction. COVID-19 pandemic negatively impacted preventive oral health care service utilization by high-risk groups, whilst raising the proportion of emergency visits due to aggravated dental diseases to preventive dental clinic [14]. The oral health programme for diabetic patients conducted by the preventive oral health unit was interrupted at many occasions in those years. Staff shortages and lack of commitment were other reasons for engagement in regular physical exercises has been identified as an essential element of Sri Lankan diabetes management [22]. Similarly, maintaining good oral hygiene and accessing oral health care should be made causes for concern among diabetic patients. Despite, inconclusive evidence on effect of periodontal treatment on glycemic control and systemic inflammation in patients with type 2 diabetes and periodontitis, a recent meta-analysis and systematic review revealed that scaling and root planning has an impact on metabolic control and systemic inflammation of type 2 diabetic patients [23]. Nevertheless, further research warranted on long-term effects in this regard [24], in different settings.
Conclusion
In conclusion, our findings demonstrate the existence of an oral health programme for diabetic patients offered by a premier, multispecialty tertiary care public dental hospital in low-income country currently grappling with an unprecedented economic crisis. However, our findings highlight the need for a dedicated staff to conduct oral health programmes for diabetic patients and the necessity for convincing diabetic patients to maximally comply with referral for oral health care. This would be a challenging task indeed in the context of economic crisis and resultant resource constraints in public health services and public dental services in Sri Lanka.
References
- Matthias AT, Jayasinghe S (2022) Worsening economic crisis in Sri Lanka: impacts on health. Lancet Glob Health 10(7): e959.
- Katulanda P, Constantine GR, Mahesh JG, Sheriff R, Seneviratne RD, et al. (2008) Prevalence and projections of diabetes and pre-diabetes in adults in Sri Lanka--Sri Lanka Diabetes, Cardiovascular Study (SLDCS). Diabet Med 25(9): 1062-1069.
- Rajapaksa L, De Silva P, Abeykoon A, Somatunga L, Sathasivam S, et al. (2021) Sri Lanka health system review. World Health Organization Regional Office for South-East Asia, New Delhi, India.
- Smith O (2018) “Sri Lanka: Achieving Pro-Poor Universal Health Coverage without Health Financing Reforms”. Universal Health Coverage Study Series No. 38, World Bank Group, Washington, DC, USA.
- Amarasinghe S, Balakumar S, Arasaratnam V (2015) Prevalence and risk factors of diabetes mellitus among adults in Jaffna District. Ceylon Med J 60(3): 107-110.
- Somasundaram NP, Ranathunga I, Gunawardana K, Ediriweera DS (2019) High prevalence of diabetes mellitus in Sri Lankan urban population – data from Colombo urban study. Sri Lanka Journal of Diabetes Endocrinology and Metabolism 9(2): 8-15.
- Deschner J, Haak T, Jepsen S, Kocher T, Mehnert H, et al. (2011) Diabetes mellitus und Parodontitis. Wechselbeziehung und klinische Implikationen. Ein Konsensuspapier [Diabetes mellitus and periodontitis. Bidirectional relationship and clinical implications. A consensus document]. Internist (Berl) 52(4): 466-477.
- Lalla E, Papapanou PN (2011) Diabetes mellitus and periodontitis: a tale of two common interrelated diseases. Nat Rev Endocrinol 7: 738-748.
- Dale J, Lindenmeyer A, Lynch E, Sutcliffe P (2014) Oral health: a neglected area of routine diabetes care? Br J Gen Pract 64(619): 103-104.
- Anil K, Vadakkekuttical RJ, Radhakrishnan C, Parambath FC (2021) Correlation of periodontal inflamed surface area with glycemic status in controlled and uncontrolled type 2 diabetes mellitus. World J Clin Cases 9(36): 11300-11310.
- De Silva NT, Preshaw PM, Taylor JJ, Jayaratne SD, Heasman PA, et al. (2006) Periodontitis: a complication of type 2 diabetes in Sri Lankans. Diabetes Res Clin Pract 74(2): 209-210.
- Preshaw PM, de Silva N, McCracken GI, Fernando DJ, Dalton CF, et al. (2010) Compromised periodontal status in an urban Sri Lankan population with type 2 diabetes. J Clin Periodontol 37(2): 165-171.
- Nguyen ATM, Akhter R, Garde S, Scott C, Twigg SM, et al. (2020) The association of periodontal disease with the complications of diabetes mellitus. A systematic review. Diabetes Res Clin Pract 165: 108244.
- Perera I, Herath C, Perera M, Gajanayake C (2022) Pinch of Prevention in Pounds of Troubles: Utilization of Preventive Oral Health Care Services by High-Risk Children and Other Target Groups Amidst Covid- 19 Milieu. Inter Ped Dent Open Acc J 7(2).
- Poudel P, Griffiths R, Wong VW, Arora A, George A (2017) Knowledge and practices of diabetes care providers in oral health care and their potential role in oral health promotion: A scoping review. Diabetes Res Clin Pract 130: 266-277.
- Leite RS, Marlow NM, Fernandes JK, Hermayer K (2013) Oral health and type 2 diabetes. Am J Med Sci 345(4): 271-273.
- Poudel P, Griffiths R, Wong VW, Arora A, Flack JR, et al. (2018) Oral health knowledge, attitudes and care practices of people with diabetes: a systematic review. BMC Public Health 18(1): 577.
- Siddiqi A, Zafar S, Sharma A, Quaranta A (2020) Awareness of Diabetic Patients Regarding the Bidirectional Association between Periodontal Disease and Diabetes Mellitus: A Public Oral Health Concern. J Contemp Dent Pract 21(11): 1270-1274.
- Mulgirigama A, Illangasekera U (2000) Study of the quality of care at a diabetic clinic in Sri Lanka. J R Soc Promot Health 120(3): 164-169.
- Perera I, Siyambalapitiya S, Somasundaram N, Perera M (2022) Screening for Oral Diseases among Diabetic Patients: The Unmet Need of Emerging Importance. Curre Res Diabetes & Obes J 16(1): 555929.
- Piyasena MMPN, Murthy GVS, Yip JLY, Gilbert C, Peto T, et al. (2019) A qualitative study on barriers and enablers to uptake of diabetic retinopathy screening by people with diabetes in the Western Province of Sri Lanka. Trop Med Health 47: 34.
- Siyambalapitiya S, Gunathilake G, Perera I (2012) Exercise: an essential component in diabetes management. Sri Lanka Journal of Diabetes, Endocrinology and Metabolism 2: 57-60.
- Baeza M, Morales A, Cisterna C, Cavalla F, Jara G, et al. (2020) Effect of periodontal treatment in patients with periodontitis and diabetes: systematic review and meta-analysis. J Appl Oral Sci 28: e20190248.
- Ndjidda Bakari W, Diallo AM, Danwang C, Nzalie RNT, Benoist HM (2021) Long-term effect of non-surgical periodontal treatment on glycaemic control in patients with diabetes with periodontitis: a systematic review and meta-analysis protocol. BMJ Open 11(2): e043250.






























