Elderly HbA1c Goals and Complications
Zofia Dice-Cholodzinski and Ronny Priefer*
Massachusetts College of Pharmacy and Health Sciences University, USA
Submission: November 09, 2022; Published: November 21, 2022
*Corresponding author: Ronny Priefer, Massachusetts College of Pharmacy and Health Sciences University, Boston, MA, USA
How to cite this article: Zofia Dice-C, Ronny P. Elderly HbA1c Goals and Complications. Curre Res Diabetes & Obes J 2022; 16(2): 555931.DOI: 10.19080/CRDOJ.2022.16.555931
Abstract
Background and Aims: Setting HbA1c goals for elderly patients guides the intensity of their therapy and can be extremely difficult. Creating individualized goals and plans is vital to help achieve the best quality of life for these patients.
Methods: Varying diabetes guidelines were assessed. PubMed was used to find studies and articles discussing HbA1c targets in elderly patients with diabetes, along with consequences of intensive versus standard treatment. Guidelines from around the world were found through their individual websites.
Results: Elderly patients with diabetes are not often studied exclusively and many studies present conflicting evidence to support various HbA1c goals. While many guidelines suggest an individualized approach in practice, many healthcare professionals lean towards stricter HbA1c goals for elderly patients with diabetes.
Conclusions: This review summarizes how the various guidelines and trials used by the guidelines as well as independent studies impact various HbA1c goals for elderly patients with diabetes.
Keywords: Diabetes; Elderly; HbA1c; Hypoglycemia; Hyperglycemia
Introduction
Diabetes in the elderly community is a growing concern. As of 2019, it was estimated that 19% of individuals aged 65-99 have diabetes worldwide and that concern is even more prevalent in North America and the Caribbean [1]. Diabetes itself is arduous to treat, however among the elderly, this is even more challenging. All too often, these patients have multiple comorbid conditions and thus require a myriad of medications [2]. Additionally, more barriers to achieving glycemic control in the elderly are present compared to those that are younger. If diabetes is not treated adequately, many micro and macrovascular complications may arise leading to hospitalization. Diabetes also puts patients at a higher risk of developing stroke, myocardial infarction, heart failure, and other cardiac events such as coronary artery disease, arrhythmias, and peripheral artery disease. While these outcomes can be minimized, if the glycemic treatment is too intense, severe hypoglycemia can lead to falls, cognitive decline, and has been correlated with increased mortality [3,4]. In recent years, there has been more documentation showing more hospitalization for hypoglycemia compared to hyperglycemia among this older age group [5]. Many studies have acknowledged that those experiencing frequent severe hypoglycemia episodes have more adverse events such as falls, cognitive decline and a lower quality of life [6]. Furthermore, in older patients with multiple comorbidities, studies found that the improvement of cardiovascular outcomes was negligible with intense treatment [7]. Balancing the management of hyperglycemia, while preventing hypoglycemia and other complications, is a particularly challenging task among the elderly.
Current American Diabetes Association (ADA) Diabetes Guidelines recommend an HbA1c goal of 7.0-7.5% for those with good cognitive function and minimal comorbid conditions. For those with comorbid conditions and cognitive impairment the goal is 8.0-8.5%. The ADA Guidelines also recommend an individualized approach to glycemic control for the elderly [8]. While these guidelines have specific recommendations and also suggest an individualized approach it can be challenging for both the patient and the healthcare provider to actually implement these said recommendations. Unfortunately, due to this challenge, many elderly patients are still over treated and have glycemic goals that are often too intense for their conditions and needs [9]. Four major studies, Action to Control Cardiovascular Risk in Diabetes (ACCORD), Action in Diabetes and Vascular Disease: Preterax and Diamicrone Modified Release Control Evaluation (ADVANCE), Glucose Control and Vascular Complications in Veterans with type 2 Diabetes (VADT), and the United Kingdom Prospective Diabetes Study (UKPDS), coupled with the aforementioned guidelines, provide the most up-to-date information that practitioners can use when making decisions regarding glycemic goals for all diabetes patients. The ACCORD, ADVANCE, and VADT trials included patients over the age of 65 enrolled while the UKPDS did not but their findings are utilized when making decisions regarding elderly patients The ACCORD trial specifically found that intense therapy and lowering of HbA1c may increase mortality for some patients and it was thought this may be attributed to severe hypoglycemia. We know that hypoglycemia is common in elderly patients with diabetes and this trial suggests that if patients HbA1c is lowered too much there could be negative outcomes [10].
In addition, while many guidelines recommend an individualized approach there is minimal discussion regarding the actual implementation of such an approach. Many elderly patients with diabetes actually have differing goals than their providers regarding their diabetes when considering long-term benefits of intense treatment versus the treatment burden especially if they have a shorter life expectancy. One survey done by the University of Chicago showed while some elderly patients may prefer minimizing adverse effects and treatment burden others may prefer increasing life expectancy and minimizing long-term complications. Depending on patients’ goals, practitioners should create individualized treatment plans that help achieve the care preferred by the patient [11]. There are many benefits to having professionals discuss patient goals with their patients instead of going solely based on guidelines. Some studies found that when an individualized approach was used it saved money and helped prevent polypharmacy and overtreatment [2,12]. While diabetes treatment within the elderly community has been studied, there is a clear need to increase general knowledge regarding this topic. Herein, is a review of guidelines regarding diabetes in the elderly and a discussion of the consequences of not individualizing glycemic goals for elderly patients with diabetes.
Guidelines
American diabetes association guidelines
One of the main diabetes guidelines used in the used in the U.S.A. is the ADA Guidelines. The ADA Guidelines HbA1c target for generally healthy young individuals is to have an HbA1c level below 7%. Additionally, for generally healthy elderly patients with diabetes, with minimal comorbid conditions, the target is set at less than 7.0-7.5%. Conversely, for patients with comorbid conditions or cognitive impairment the goals are elevated to 8.0-8.5%. These guidelines have made recommendations for relaxing HbA1c goals for elderly patients and focus on a more individualized approach, as well as discussed strategies and rationale for goal and treatment adjustments [9].
American association of clinical endocrinology guidelines
In contrast, the American Association of Clinical Endocrinology (AACE) guidelines are very strict and suggest elderly diabetic patients that are generally healthy should follow the same goal as younger patients, of having an HbA1c level below 6.5%. However, the guidelines do recognize that patients with more medications or those that are frail can have less stringent goals [13].
Endocrine society clinical practice guidelines
The Endocrine Society guidelines does not provide specific glycemic targets as it states that evidence for specifics is lacking. However, the guidelines do recommend that patients over 65 years old with diabetes should have outpatient treatment regimens specifically designed to minimize hypoglycemia. There also is a mention of pushing glycemic targets to focus on overall health and management strategies [14].
American college of physicians
The American College of Physician Clinical Guidelines first emphasize the need for personalized targets focused on patient preference, life expectancy, treatment burden, and costs of care. These Guidelines just have a general glycemic target range of 7-8% for most patients with Type 2 diabetes mellitus (T2DM) due to the inconsistency in further benefit below 7 in many trials. Additionally, these guidelines even recommend de-intensify pharmacotherapy in patients with HbA1c below 6.5% [15].
National institute of health and care excellence
The National Institute of Health and Care Excellence Guidelines emphasize discussing and agreeing upon an individual target and maintaining it unless there are adverse effects such as hypoglycemia. Then the guidelines split goal targets into various groups. The first group is those using only lifestyle and diet changes or medications that do not cause hypoglycemia and their target is below 6.5%. For those on hypoglycemic medications their target becomes less than 7%. Then the guidelines recommend relaxing goals further for patients that are elderly, reduced life expectancy, high risk of hypoglycemia and falls, or significant comorbidities [16].
International diabetes federation guidelines
The International Diabetes Federation (IDF) categorizes patients into three categories: Functionally Independent, Functionally Dependent, and End of Life Care. The HbA1c goal of Functionally Independent is 7.0-7.5%, while those that are Functionally Dependent have a goal that is slightly raised to 7.0-8.0%. If the patient has dementia or is classified as frail, their goal is to maintain a level less than 8.5%. Lastly, if the patient is receiving End of Life Care, the key target is to avoid symptomatic hyperglycemia. These guidelines also recommend an individualized approach based on comorbidity, functional status, risk of hypoglycemia, and microvascular complications [17].
Japanese geriatric diabetes guidelines
The Japanese Geriatric Diabetes Guidelines are even more specific with their three categories of patients. The first category is patients with intact cognitive function and no impairment of activities of daily living. These guidelines further separate patients into those on medications that can induce hypoglycemia such as insulin, sulfonylureas, or glinides, and those that are not. For those that are on a hypoglycemic-inducing medication, an HbA1c goal of less than 7.5% is suggested for those younger than 75 and 8.0% if older. For those that are not, their HbA1c goal should be below 7.0%. The second category includes patients with mild cognitive impairment or dementia but no major impairment of daily living. For those on hypoglycemic-inducing medication, their HbA1c goal is less than 8.0% and less than 7.0% if they are not. The final category includes patients with moderate dementia or impairment of activities of daily living or multiple comorbidities. For those that are on a hypoglycemic medication, their HbA1c goal is <8.5% while those that are not should be <8.0% [18].
European society of cardiology/European association for the study of diabetes guidelines
The European Society of Cardiology/European Association for the Study of Diabetes Guidelines is even more lenient by having a goal of less than 8.0 % for those with moderate comorbid conditions or less than 9.0% for patients with more conditions. For healthy elderly diabetic patients, the main goal is to stay below 7.0%. However, these guidelines do acknowledge the need for further research in this population, specifically including the adverse events related to polypharmacy [19].
Department of veterans affairs/department of defense
One of the most specific guidelines is from the US Department of Veterans Affairs and Department of Defense. Here, the patients are split into three categories. Those with no comorbidity and over ten years of life expectancy, those with a major comorbidity and a five-to-ten-year life expectancy, and end of life care. Each category is further split by microvascular complications. For patients with no comorbidity and mild microvascular complications the HbA1c goal is <7.0%. If they have more microvascular complications, then the goal is less than 8.0%. However, if there are significant complications the goal is further raised to be less than 9.0%. For those patients with a major comorbidity and little microvascular complications the goal is less than 8.0%, while with multiple microvascular complications the goal is less than 9.0%. If the patient categorized as in end-of-life care, the goal is simply to be less than 9.0% [20,21].
International association of gerontology and geriatrics and European diabetes working party for older people and international task force of experts in diabetes guidelines
The International Association of Gerontology and Geriatrics and European Diabetes Working Party for Older People and International Task Force of Experts in Diabetes guidelines have more generalized goals. These guidelines are only split into healthy versus frail patients. Healthy elderly patients have a goal to be below 7.5 % while for frail individuals there is a goal of below 8.5% [21,22].
Diabetes Canada Clinical Practice Guidelines
Finally, the Diabetes Canada Clinical Practice Guidelines separates elderly patients by status to either functionally independent, dependent, frail with or without dementia, and end of life. Functionally independent are patients that have a greater than 10-year life expectancy and thus should be treated similar to younger patients with diabetes and thus have an HbA1c goal of less than 7.0%. Functionally dependent patients are those with orthostasis or limited life expectancy and have a goal of less than 8.0%. Frail patients with or without dementia are defined as elderly patients with a high risk of hypoglycemia due to polypharmacy, comorbidities, or impaired renal function and have a more liberal goal of 8.5%. Lastly, those patients on end-oflife care do not have an HbA1c goal but aim to avoid symptomatic hyperglycemia or hypoglycemia. These guidelines also separate those taking insulin and sulfonylureas from those that do not, since these medications have a higher risk of hypoglycemia and patients taking them will subsequently have a lower HbA1c. For those not taking these medications the goals are as stated above but for those taking them that are functionally dependent the goal is between 7.1 and 8.0%, while for those that are frail with or without dementia it is between 7.1 and 8.5%. Those that are functionally independent or in end-of-life care, the goals remain the same. The Canadian guidelines also emphasize the need to create goals based on functional status and that most elderly in general should fall in a goal between 7.0 and 8.0 [23].
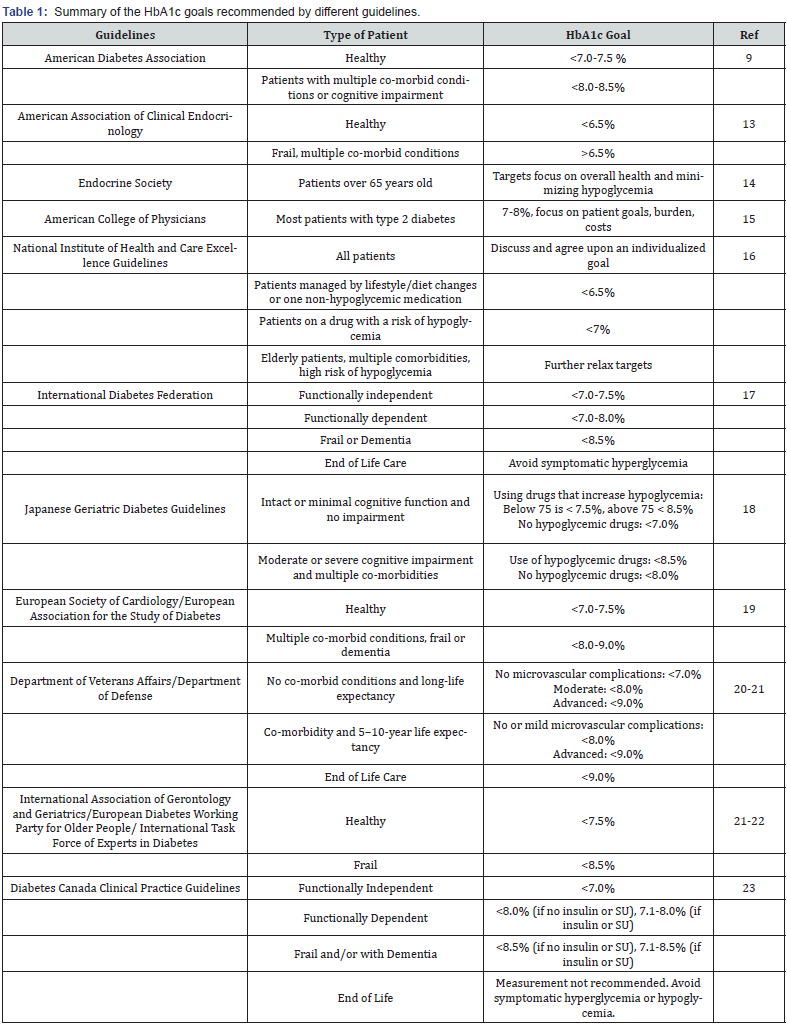
While many of these guidelines acknowledge the need for individualized treatment, many elderly patients still receive goals that are not individualized or too strict (Table 1), and subsequently many hospitalizations in elderly diabetic patients occur partially due to too strict glucose control goals [5,24].
Glycemic Target Trial Studies
UKPDS trial
As mentioned earlier, four major studies (UKPDS, ACCORD, ADVANCE, and VADT) helped form the guidelines for treating elderly patients with diabetes (Table 2). The UKPDS trail is one of the oldest and biggest trails with over 7000 participants ranging at an age of 25-65 [25]. After undergoing a 3-month dietary control, patients that had a fasting blood glucose level between 108 – 270 mg/dL were placed into either conventional treatment, which at the time was diet control, or intensive control, which consisted of a sulfonylurea or insulin. If the patient was overweight (having 120% of ideal body weight) they were given metformin. The study revealed that those that had intensive therapy for 10 years led to a 9% reduction in risk for a diabetes related endpoint and 24% reduction in risk for microvascular complications. For overweight patients the reduction in risk for a diabetes related endpoint was 21% and diabetes related death was 30% after 10 years of therapy. However, for some endpoints, including risk of microvascular disease and myocardial infarction, the benefit was only seen with long-term treatment, so it may limit the applicability to individuals with shorter-life expectancy. Although this trial did not include elderly (patients over 65), the findings are still used by practitioners and integrated into practice guidelines due to the lack of trials in this population [26].
ACCORD trial
The ACCORD trial consisted of participants ranging in the age of 40-79. The study separated the participants into two arms: intensive treatment and standard treatment. Those in the intensive arm aimed for a lower HbA1c goal (<6.0%) while the standard arm aimed for a broader HbA1c goal (7.0-7.9%). After seven years, the intensive arm was halted early, due to increased mortality in comparison to the standard arm (HR 1.22). Prior to stopping, the intensive arm had higher incidences of severe hypoglycemic events requiring medical assistance (HMA) or any assistance (HA). Although the study found that the increased mortality rate could not be attributed to severe hypoglycemia alone, it did find that for those that did not have previous occurrences of HMA were at greater risk of death in the intensive arm. However, in patients with a previous HMA event the risk of death was greater in the standard arm [27]. Despite previous trails, including UKPDS, which concluded that intensive glucose control leads to reduced microvascular outcomes [26], the ACCORD trail revealed the opposite. Patients enrolled in the intensive arm did not see a significant improvement in their microvascular outcomes in comparison to their standard arm counterparts [7]. A limitation with the ACCORD trial was the fact that the study mainly included younger patients, thus making it difficult to apply to the elderly population [27]. The ACCORD trial did support the generation of guidelines pushing for an individualized approach to glucose control among all patients.
Advance trial
The ADVANCE trial had similar outcomes as the aforementioned ACCORD. In this trial, all patients were over 55 years of age with a diagnosis of Type 2 diabetes at the age of 30 or older. The patients were separated into an intensive treatment group targeting an HbA1c goal below 6.5% and a standard treatment group based on local guidelines. This study found that intensive glucose control led to increased rates of severe hypoglycemia and hospitalization. However, in contrast to ACCORD trial, the ADVANCE trial found no significant difference in mortality between the groups [28]. In addition, while other studies showed a reduction of macrovascular events with intensive control [27], the ADVANCE trial could not support this claim with statistical significance [29]. The trial did show that severe hypoglycemia was associated with increased micro and macrovascular events as well as death. It was concluded that the adverse outcomes were associated more with incidences of hypoglycemia, rather than intensive glucose control. The trial showed the need for further studies discussing the relationship between severe hypoglycemia and vascular outcomes [30].
VADT trial
The VADT trial is another major trial that included veterans with an average age of 60, an average HbA1c of 9.2%, and approximately 11 years with diabetes. Much like the ACCORD study, the participants were either assigned to an intensive or standard glucose control groups [31]. After a 5-year follow-up, the intensive arm did not show any benefit over standard with respect to retinopathy, neuropathy, and nephropathy. but did show a reduction in the progression of both albumin excretion and macroalbuminuria [32]. At the 10-year follow-up, the intensive arm participants maintained a higher eGFR, and at a 15-year follow-up, they were less likely to develop composite renal outcomes. In terms of retinopathy, the intensive glucose participants that were younger than 55 saw a reduction, however those above 70 years of age saw an increase in this adverse outcome. The trial acknowledged the benefit of intensive glucose control long term; however, it may not be suited for patients with multiple comorbid conditions and for elderly with short life spans [33].
Table 2 provides an overview of the data from these trials discussed. One disclaimer about these trials is that many of them are older and did not implement newer agents, with less risk of hypoglycemia, which are considered as part of the 1st line treatment regimens today for certain patient populations.

Consequences of Strict Glycemic Targets
Hypoglycemia
While these the previously mentioned trials guide practitioners in creating goals and treatment plans for the elderly population. However, even though many guidelines and trials push practitioners towards more liberal HbA1c targets for elderly patients, some studies have shown that many times elderly patients have than HbA1c goals that may be too stringent and can lead to many adverse effects [11]. One major adverse effect when HbA1c is lowered is that often patients have more instances of hypoglycemia. The elderly population is more at risk for hypoglycemia. When these elderly patients had intensive glucose lowering therapy, they had even more instances of severe hypoglycemia [34]. One cross sectional study of elderly and nonelderly patients with diabetes found that those with a lower HbA1c had a higher prevalence of instances of hypoglycemia and that those on insulin and multiple forms of therapy were also at a higher chance of these events [35]. An analysis of the ACCORD trial showed those on intensive therapy had a 3.14% annual incidence of hypoglycemia while those on standard therapy only had 1.03% incidence and those that were older only gained risk every year older, they got [36]. However, one study of elderly patients with diabetes found no association between different HbA1c levels and duration of hypoglycemia. This study also found that maybe the type of insulin administration was to blame and that using once a day basal insulin over multiple daily administrations lowered the risk of hypoglycemia rather than correlating it to a specific HbA1c level [37]. One qualitative study that conducted interviews of patients that had hypoglycemic events, reported that many said they felt that they were over treated and on too many medications. They felt that their practitioners where too strict and this led to their hypoglycemia [38]. One study on trends of hospitalizations for hyperglycemia versus hypoglycemia found that from 1999- 2011 the rates of hospitalization for hyperglycemia were declining while the rates for hypoglycemia were increasing [5]. This varying evidence shows the need for further research regarding the correlation between HbA1c level and risk of hypoglycemia in elderly patients with diabetes.
Falls
Another issue arises when elderly patients are put on intensive glucose control regimens in attempts to control their glucose levels is that, they are put at more risk for physical falls due to the hypoglycemia. In the elderly population, falls are a major cause of morbidity and mortality. Patients with diabetes are known to be frailer and at a higher at risk for falls, so it is even more important to prevent falls in this population [39]. In one study, the risk of falling doubled for elderly patients with diabetes that had a hypoglycemic episode [40]. In a different retrospective study discussing the correlation between glycemic control and falls, the results concluded that elderly patients, regardless of frailty status that had an HbA1c below 7, were at increased risk for falling. Looking at the frail population and comparing those with an HbA1c above and below 7; 58% of those in the higher HbA1c group had a fall incident compared to 77% in the lower HbA1c group. In the non-frail group, 12% of patients fell with an HbA1c above 7, while 30% fell for those with an HbA1c below 7. This evidence points towards looser glycemic control in both frail and non-frail elderly patients [41]. However, there is a debate, as other studies did not find this correlation between lower HbA1c levels and falls [42]. One study found that only those using insulin that had an HbA1c level below 6 were at risk for falls, while those on other medications for diabetes were not [43].
Cardiovascular events (macrovascular)
Cardiovascular events are another complication associated with poorly managed HbA1c levels. Macrovascular events include the development of coronary artery disease, peripheral artery disease, or stroke while microvascular events include diabetic neuropathy, nephropathy, or retinopathy.. One prospective study in patients with diabetes over 70 years found a higher incidence of cardiovascular events in those with an increased HbA1c level though the study did not assess the effect of glucose control on these HbA1c levels [44]. While the UKPDS trial demonstrated no difference in macrovascular events when comparing intensive versus standard glucose control [45], in an extended follow up of the VADT trail, a 17% reduction in major cardiovascular outcomes was found for intensive arm of the trial compared to the standard [46]. The ADVANCE trial suggested that reducing HbA1c levels might improve cardiovascular outcomes but did not have enough power. So, the trial could not show a significant effect of intensive glucose control on major cardiovascular events [25]. A long-term follow-up of the ACCORD trial on the other hand also found no significant reduction in major cardiovascular events after 5 years. When creating HbA1c goals for elderly patients, the benefit of intensive treatment on cardiovascular events must be assessed based on individual considerations, such as life expectancy and burden of this type of treatment.
Cardiovascular events (microvascular)
There is contrasting evidence on whether intensive glucose control prevents these microvascular outcomes from occurring. The UKPDS trial saw a 25% reduction in microvascular events for intensive treatment in comparison to the standard [45]. However, a long-term follow up study of the UKPDS trial admitted that much of the risk reduction of microvascular disease could only be seen with extended follow up and not short-term [23]. Meanwhile, in the VADT trial, there was no significant reduction in microvascular complications (retinopathy, nephropathy, and neuropathy), besides one significant reduction in worsening albumin excretion [30].
Quality of life and expense
Some other important considerations include the cost and the treatment burden on the patient. In a survey conducted in elderly patients with diabetes, it was found that many patients thought that intensive treatment could worsen their quality of life. While individualized treatment is recommended by guidelines for many elderly patients with diabetes, one survey, found that doctors favored more intensive treatment [11]. A different study found that in older patients the improvement in quality adjusted life years was significantly lower as age increased. There also was an impact of patient’s perception of treatment and many patients that had a high treatment burden (mainly those on intensive insulin treatment) did not see a noticeable risk reduction for end stage renal disease, vision loss, amputation, or myocardial infarction when lowering the patients HbA1c by 1% [47]. Regarding hypoglycemic events often associated with intensive glucose control, patients found the experience to be very unpleasant and admitted that it affected their adherence to their glucose lowering medications [48]. When comparing individualized control and intensive control, one study found that individualized control saved over $10,000 per person, as often there were less medication costs. While overall the strategy led to lower lifeexpecting years, it led to increased quality of life, cost-savings, and less hypoglycemic episodes [49].
Mortality
Two retrospective cohort studies assessed the relationship between HbA1c levels and mortality. The results revealed a U-shaped curve suggesting both those with either low (below 7.0) and high HbA1c’s (above 9.0) had increased incidence of mortality [50,51]. Another study of elderly patients in Canada found that those with intensive glucose control were more likely to be hospitalized or die over patients with conservative control regardless of the medication they were taking [52]. As with the aforementioned falls, many studies offer different views. For example, one follow-up to the ACCORD trail suggests that there is greater risk of mortality for high vs lower HbA1c levels when discussing only the intensive treatment group [53]. Another study that discussed the ACCORD trial, found that more patients in the intensive treatment group died, than those in the standard arm [31]. Other studies agree that intensive glucose control in the elderly leads to increased mortality, but also agree that high HbA1c levels contribute to said mortality.
Conclusion
HbA1c goals in the elderly are extremely difficult to create and these guidelines and studies show the need for individualized goals. The main studies originally used for the previous guidelines can be conflicting and often do not have statistical significance for their implementation. While the UKPDS trial found no significant risk reduction in microvascular outcomes, the ADVANCE trial found a decrease in microvascular events among the intensive group. Both the ACCORD and ADVANCE trials found a significant risk of hypoglycemia in the intensive treatment groups of their respective studies. Even though these trials are the are utilized in the development of guidelines, the UKPDS only includes patients up to 65 years of age while with ACCORD it was up to 79, again demonstrate inconsistency in their studies. The number of large, randomized studies that include elderly patients with diabetes is very limited, however this population continues to grow. It is imperative that future investigations focus on this group. Many of the discussed trails do not provide clear evidence for healthcare practitioners to set proper individualized HbA1c goals for patients.
Historically, even after guidelines started to consider different targets, elderly patients continued to receive low HbA1c goals even after complaints about hypoglycemia and other adverse effects associated with decreased glucose levels [54]. Part of the issue when setting goals is the consequences of having a too low or too high HbA1c such as risk of hypoglycemia and falls. Conversely, if levels are too high there is a risk of microvascular and macrovascular complications, although this is mainly seen long term. For some elderly patients, this potential benefit may not be useful since their life expectancy may be less than the complication onset. Studies considering elderly found that quality of life decreases on both ends of the spectrum whether their HbA1c is too high or too low. These studies also demonstrated that patient preference makes a difference especially in the elderly. The expense and adverse effects of intensive control were often too much for patients and they prefer to have a less intensive glucose treatment. New studies of this population need to reassess whether practice has changed as the guidelines evolved to include more guidance focused on the particular needs and issues pertaining to elderly patients with diabetes to help provide a clearer understanding for healthcare providers to use when creating individualized goals for their patients.
Acknowledgements
The authors wish to thank the School of Pharmacy at the Massachusetts College of Pharmacy and Health Sciences University for financial support of this project.
References
- Sinclair A, Saeedi P, Kaundal A, Karuranga S, Malanda B, et al. (2020) Diabetes and global ageing among 65-99-year-old adults: Findings from the International Diabetes Federation Diabetes Atlas, (9th), Diabetes Res Clin Pract 162: 108078.
- Peron EP, Ogbonna KC, Donohoe KL (2015) Antidiabetic medications and polypharmacy. Clin Geriatr Med 31(1): 17-27.
- Saito N, Toyoda M, Ono M, Kaneyama N, Kimura M, et al. (2020) Importance of the Evaluation of Renal Function for the Prevention of Hypoglycemia in Elderly Diabetes Patients. Tokai J Exp Clin Med 45(3): 139-143.
- Huang ES, Laiteerapong N, Liu JY, John PM, Moffet HH, et al. (2014) Rates of complications and mortality in older patients with diabetes mellitus: the diabetes and aging study. JAMA Intern Med 174(2): 251-258.
- Lipska KJ, Ross JS, Wang Y, Inzucchi SE, Minges K, et al. (2014) National trends in US hospital admissions for hyperglycemia and hypoglycemia among Medicare beneficiaries, 1999 to 2011. JAMA Intern Med 174(7): 1116-1124.
- Redekop WK, Koopmanschap MA, Stolk RP, Rutten GE, Wolffenbuttel BH, et al. (2002) Health-related quality of life and treatment satisfaction in Dutch patients with type 2 diabetes. Diabetes Care 25(3): 458-463.
- Connor OPJ, Ismail BF (2011) Near-Normalization of Glucose and Microvascular Diabetes Complications: Data from Accord and Advance. Ther Adv Endocrinol Metab 2(1): 17-26.
- American Diabetes Association (2021) 6. Glycemic Targets: Standards of Medical Care in Diabetes-2021. Diabetes Care 44(Suppl 1): S73-S84.
- Hoogwerf BJ (2008) Action to Control Cardiovascular Risk in Diabetes Study Group. Does intensive therapy of type 2 diabetes help or harm? Seeking accord on ACCORD. Cleve Clin J Med 75(10): 729-737.
- Bonds DE, Miller ME, Bergenstal RM, Buse JB, Byington RP, et al. (2010) The association between symptomatic, severe hypoglycaemia and mortality in type 2 diabetes: retrospective epidemiological analysis of the ACCORD study. BMJ 340: b4909.
- Chin MH, Drum ML, Jin L, Shook ME, Huang ES, et al. (2008) Variation in treatment preferences and care goals among older patients with diabetes and their physicians. Med Care 46(3): 275-286.
- Basu S, Shankar V, Yudkin JS (2016) Comparative effectiveness and cost-effectiveness of treat-to-target versus benefit-based tailored treatment of type 2 diabetes in low-income and middle-income countries: a modelling analysis. Lancet Diabetes Endocrinol 4(11): 922-932.
- Garber AJ, Handelsman Y, Grunberger G, Einhorn D, Abrahamson MJ, et al. (2020) Consensus statement by the american association of clinical endocrinologists and american college of endocrinology on the comprehensive type 2 diabetes management algorithm - 2020 executive summary. Endocr Pract 26(1): 107-139.
- Derek L, Geert JB, Susan SB, Felipe FC, Boris D, et al. (2019) Treatment of Diabetes in Older Adults: An Endocrine Society Clinical Practice Guideline. The Journal of Clinical Endocrinology & Metabolism 104(5): 1520-1574.
- Amir Q, Timothy JW, Devan K, Horwitch C, Barry MJ, et al. (2018) Hemoglobin A1c Targets for Glycemic Control with Pharmacologic Therapy for Nonpregnant Adults with Type 2 Diabetes Mellitus: A Guidance Statement Update from the American College of Physicians. Ann Intern Med 168: 569-576.
- (2015) Type 2 diabetes in adults: Management: Guidance. Type 2 diabetes in adults: management.
- Dunning T, Sinclair A, Colagiuri S (2014) New IDF guideline for managing type 2 diabetes in older people. Diabetes Research and Clinical Practice 103(3): 538-540.
- Araki E, Goto A, Kondo T, Noda M, Noto H, et al. (2020) Japanese Clinical Practice Guideline for Diabetes 2019. J Diabetes Investig 11(4): 1020-1076.
- Cosentino F, Grant PJ, Aboyans V, Bailey CJ, Ceriello A, et al. (2019) 2019 ESC guidelines on diabetes, pre-diabetes, and cardiovascular diseases developed in collaboration with the EASD. European Heart Journal 41(2): 255-323.
- Tschanz MP, Watts SA, Colburn JA, Conlin PR, Pogach LM (2017) Overview and Discussion of the 2017 VA/DoD Clinical Practice Guideline for the Management of Type 2 Diabetes Mellitus in Primary Care. Fed Pract 34(Suppl 8): S14-S19.
- Bansal N, Dhaliwal R, Weinstock RS (2015) Management of diabetes in the elderly. Med Clin North Am 99(2): 351-377.
- Sinclair A, Morley JE, Rodriguez ML, Paolisso G, Bayer T, et al. (2012) Diabetes mellitus in older people: position statement on behalf of the International Association of Gerontology and Geriatrics (IAGG), the European Diabetes Working Party for Older People (EDWPOP), and the International Task Force of Experts in Diabetes. J Am Med Dir Assoc 13(6): 497-502.
- Diabetes Canada Clinical Practice Guidelines Expert Committee. (2018) Diabetes Canada 2018 Clinical Practice Guidelines for the Prevention and Management of Diabetes in Canada. Can J Diabetes 42(Suppl 1): S1-S326.
- Budnitz DS, Lovegrove MC, Shehab N, Richards CL (2011) Emergency hospitalizations for adverse drug events in older Americans. N Engl J Med 365(21): 2002-2012.
- Adler AI, Stevens RJ, Manley SE, Bilous RW, Cull CA, et al. (2003) Development and progression of nephropathy in type 2 diabetes: the United Kingdom Prospective Diabetes Study (UKPDS 64). Kidney Int 63(1): 225-232.
- Holman RR, Paul SK, Bethel MA, Matthews DR, Neil HA (2008) 10-year follow-up of intensive glucose control in type 2 diabetes. N Engl J Med 359(15): 1577-1589.
- Lipska KJ, Krumholz H, Soones T, Lee SJ (2016) Polypharmacy in the Aging Patient: A Review of Glycemic Control in Older Adults with Type 2 Diabetes. JAMA 315(10): 1034-1045.
- Gerstein HC, Miller ME, Byington RP, Goff DC, Bigger JT, et al. (2008) Action to Control Cardiovascular Risk in Diabetes Study Group. Effects of intensive glucose lowering in type 2 diabetes. N Engl J Med 358(24): 2545-2559.
- Patel A, MacMahon S, Chalmers J, Neal B, Billot L, et al. (2008) Advance Collaborative Group. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Engl J Med 358(24): 2560-2572.
- Zoungas S, Patel A, Chalmers J, Galan BE, Li Q, et al. (2010) Severe hypoglycemia and risks of vascular events and death. N Engl J Med 363(15): 1410-1418.
- Skyler JS, Bergenstal R, Bonow RO, Buse J, Deedwania P, et al. (2009) Intensive glycemic control and the prevention of cardiovascular events: implications of the Accord, Advance, and VA Diabetes Trials: a position statement of the American Diabetes Association and a Scientific Statement of the American College of Cardiology Foundation and the American Hsinclaeart Association. J Am Coll Cardiol 53(3): 298-304.
- Duckworth W, Abraira C, Moritz T, Reda D, Emanuele N, et al. (2009) Glucose control and vascular complications in veterans with type 2 diabetes. N Engl J Med 360(2): 129-139.
- Tran K, Reaven P (2020) Review of the veteran affairs diabetes trial: Lessons learned. Rev Endocr Metab Disord 21(4): 537-546.
- Freeman J (2019) Management of hypoglycemia in older adults with type 2 diabetes. Postgrad Med 131(4): 241-250.
- Miller CD, Phillips LS, Ziemer DC, Gallina DL, Cook CB, et al. (2001) Hypoglycemia in patients with type 2 diabetes mellitus. Arch Intern Med 161(13): 1653-1659.
- Miller ME, Bonds DE, Gerstein HC, Seaquist ER, Bergenstal RM, et al. (2010) The effects of baseline characteristics, glycaemia treatment approach, and glycated haemoglobin concentration on the risk of severe hypoglycaemia: post hoc epidemiological analysis of the ACCORD study. BMJ 340: b5444.
- Munshi MN, Slyne C, Segal AR, Saul N, Lyons C, et al. (2017) Liberating A1C goals in older adults may not protect against the risk of hypoglycemia. J Diabetes Complications 31(7): 1197-1199.
- Pasciak WE, Berg DN, Cherlin E, Fried T, Lipska KJ (2021) Qualitative analysis of reasons for hospitalization for severe hypoglycemia among older adults with diabetes. BMC Geriatr 21(1): 318.
- Yanase T, Yanagita I, Muta K, Nawata H (2018) Frailty in elderly diabetes patients. Endocr J 65(1): 1-11.
- Kachroo S, Kawabata H, Colilla S, Shi L, Zhao Y, et al. (2015) Association between hypoglycemia and fall-related events in type 2 diabetes mellitus: analysis of a U.S. commercial database. J Manag Care Spec Pharm 21(3): 243-253.
- Nelson JM, Dufraux K, Cook PF (2007) The relationship between glycemic control and falls in older adults. J Am Geriatr Soc 55(12): 2041-2044.
- Chiba Y, Kimbara Y, Kodera R, Tsuboi Y, Sato K, et al. (2015) Risk factors associated with falls in elderly patients with type 2 diabetes. J Diabetes Complications 29(7): 898-902.
- Schwartz AV, Vittinghoff E, Sellmeyer DE, Feingold KR, Rekeneire N, et al. (2008) Diabetes-related complications, glycemic control, and falls in older adults. Diabetes Care 31(3): 391-396.
- Orozco BD, Navarro PJ, Cebrián CAM, Guisasola FA, Miana CE, et al. (2020) The influence of hemoglobin A1c levels on cardiovascular events and all-cause mortality in people with diabetes over 70 years of age. A prospective study. Prim Care Diabetes 14(6): 678-684.
- (1998) Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). UK Prospective Diabetes Study (UKPDS) Group Lancet 352(9131): 837-853.
- Hayward RA, Reaven PD, Wiitala WL, Bahn GD, Emanuele NV, et al. (2015) Follow-up of Glycemic Control and Cardiovascular Outcomes in Type 2 Diabetes. N Engl J Med 373(10): 978.
- Vijan S, Sussman JB, Yudkin JS, Hayward RA (2014) Effect of patients' risks and preferences on health gains with plasma glucose level lowering in type 2 diabetes mellitus. JAMA Intern Med 174(8): 1227-1234.
- Nicolucci A, Pintaudi B, Rossi MC, Messina R, Dotta F, et al. (2015) The social burden of hypoglycemia in the elderly. Acta Diabetol 52(4): 677-685.
- Laiteerapong N, Cooper JM, Skandari MR, Clarke PM, Winn AN, et al. (2018) Individualized Glycemic Control for U.S. Adults with Type 2 Diabetes: A Cost-Effectiveness Analysis. Ann Intern Med 168(3): 170-178.
- Currie CJ, Peters JR, Tynan A, Evans M, Heine RJ, et al. (2010) Survival as a function of HbA(1c) in people with type 2 diabetes: a retrospective cohort study. Lancet 375(9713): 481-489.
- Huang ES, Liu JY, Moffet HH, John PM, Karter AJ (2011) Glycemic control, complications, and death in older diabetic patients: the diabetes and aging study. Diabetes Care 34(6): 1329-1336.
- Lega IC, Campitelli MA, Austin PC, Na Y, Zahedi A, et al. (2021) Potential diabetes overtreatment and risk of adverse events among older adults in Ontario: a population-based study. Diabetologia 64(5): 1093-1102.
- Riddle MC, Ambrosius WT, Brillon DJ, Buse JB, Byington RP, et al. (2010) Epidemiologic relationships between A1C and all-cause mortality during a median 3.4-year follow-up of glycemic treatment in the Accord trial. Diabetes Care 33(5): 983-990.
- Mahoney GK, Henk HJ, McCoy RG (2019) Severe Hypoglycemia Attributable to Intensive Glucose-Lowering Therapy Among US Adults with Diabetes: Population-Based Modeling Study, 2011-2014. Mayo Clin Proc 94(9): 1731-1742.






























