Screening for Oral Diseases among Diabetic Patients: The Unmet Need of Emerging Importance
Irosha Perera1, Sajith Siyambalapitiya2, Noel Somasundaram3 and Manosha Perera4
11Preventive Oral Health Unit, National Dental Hospital (Teaching), Colombo
22Endocrinology Unit, North Colombo Teaching Hospital, Sri Lanka
33Endocrinology Unit, National Hospital Sri Lanka, Sri Lanka
44Alumnus School of Dentistry and Oral Health, Griffith University, Sri Lanka
Submission: September 10, 2022; Published: September 16, 2022
*Corresponding author: Irosha Perera, Preventive Oral Health Unit, National Dental Hospital (Teaching) Sri Lanka, Ward Place, Colombo 7, Sri Lanka
How to cite this article: Irosha P, Sajith S, Noel S, Manosha P. Screening for Oral Diseases among Diabetic Patients: The Unmet Need of Emerging Importance. Curre Res Diabetes & Obes J 2022; 16(1): 555929.DOI: 10.19080/CRDOJ.2022.16.555929
Abstract
Periodontitis the chronic inflammatory disease of the periodontium and tooth supporting structures garnered recognition as the sixth complication of diabetes mellitus. There is evidence for the bi-directional relationship between diabetes and periodontal disease extended to optimal glycaemic control. Sri Lanka is a lower-middle-income developing country currently grappling with a major economic crisis and a high burden of non- communicable- diseases including diabetes. Oral health is often a neglected aspect of diabetic patients. Against such a backdrop, this short report explores the emerging need for screening of diabetic patients for oral diseases as a routine practice.
Keywords: Periodontitis; Chronic inflammatory disease; Periodontium; Optimal glycaemic control; Oral health; Diabetes; Glycaemic control
Introduction
Diabetes mellitus denotes a challenging multidimensional public health problem and in Sri Lanka with prevalence ranging from 18.6% to 6.8 % among ≥20-year-old-adults [1]. Periodontitis, the chronic disease of the tooth supporting structures is considered to be the 6th complication of diabetes and a main cause for tooth loss. Diabetic patients are at 2.8-fold elevated risk of progressing into periodontitis [2] and 4.2-fold increased risk of having alveolar bone loss than their non-diabetic counterpart [2]. More often poor oral hygiene status is associated with the high burden of periodontitis among diabetic patients.
Evidence is emerging on the bi-directional relationship between glycaemic control and periodontal disease status among diabetics. For example, recent systematic review and meta-analysis, based on 7 randomized-controlled-clinical trials revealed that there was a reduction of glycated haemoglobin (H1AC) 0.48 (95% CI 0.18-0.78) among the intervention group who received non-surgical treatment for periodontal disease compared to the non-intervention group over a minimum follow- up period of 3 months [3]. Screening of diabetic patients for oral disease is not being practiced in Sri Lanka. Against this backdrop, present short report focuses on main findings of screening diabetic patients for oral hygiene as a proxy for their existing periodontal disease.
Methods
A rapid assessment of a convenience sample of 40 diabetic patients attended a selected diabetic clinic at NHSL was conducted. Data were collected at the waiting area of the diabetic clinic using an interviewer administered, pre-tested, brief-data collection form. Clinical data were extracted from clinic records. Simplified debri index component of simplified oral hygiene index (Green & Vermillion, 1964) was used to assess oral hygiene status [4]. The data were entered and analysed using SPSS-21 Statistical Software Package. Approval was obtained from Director General NHSL and Consultant Endocrinologists via the Director, National Dental Hospital (Teaching) (NDHTSL) Sri Lanka.
Results
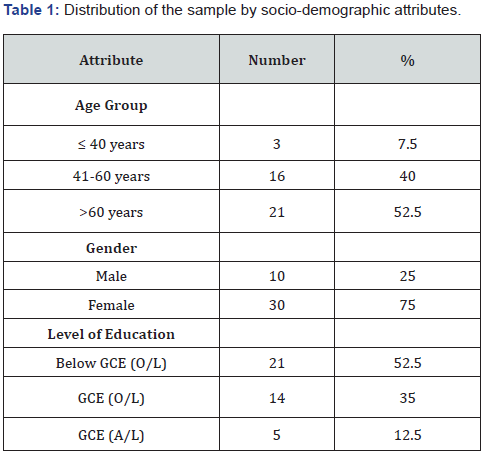
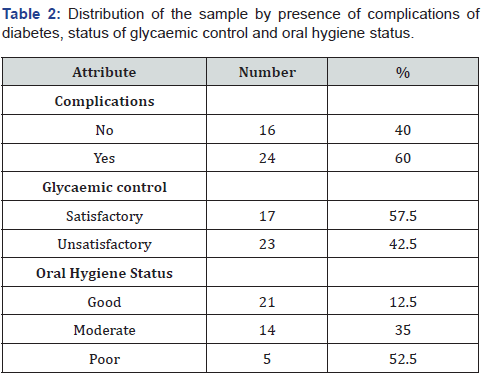
The overwhelming majority comprised of female diabetic patients (75%) of which 40% were aged 41-60 years and 52.5% were aged above 60 years. Their mean age was 57.95 years ± 11.2 years. 52.5% had levels of education below GCE (O/L). The mean ± SD duration of living with diabetes after diagnosis was 61.73 ± 92.47 months (around 6 years). Importantly, the majority (57.5%) demonstrated unsatisfactory glycaemic control status by fasting blood sugar level [80–130mg/dl (4.4–7.2mmol/L)] assessed most recently. Moreover, 60% had complications of diabetes ie. neuropathy, retinopathy, cardiovascular disease and nephropathy. Furthermore, 52.5% were identified as having poor oral hygiene status.
Discussion
Present assessment provides baseline data of a purposive sample of diabetic patients attended a selected diabetic clinic of NHSL. The overwhelming majority of diabetic patients were older females of low educational attainment (Table 1). Despite being diagnosed as having diabetes for past 6 years or more, the majority reported less optimal glycaemic control and consequent complications of diabetes (Table 2). One of vital plausible reasons could be poor adherence to regular physical exercise by diabetic patients as reported by some studies despite being an inherent component of diabetes management [5]. The oral hygiene status of the diabetic patients (a surrogate indicator of their periodontal disease status) was a cause of concern as it was moderate to poor among the great majority (Table 2). As reported by previous studies, self-reported diabetes was an independent risk for periodontitis among Sri Lankan adults [6]. The high burden of periodontal disease among diabetic patients in Sri Lankan context was reported by other studies [7].
The National Dental Hospital (Teaching) Sri Lanka (NDHTSL) is the premier multispecialty, tertiary care public dental hospital in the country possessing a fully-fledged Preventive Oral Health Unit (POHU) to offer services for diabetic patients. Hence, an intervention was planned to screen diabetic patients for oral health status and refer them to POHU for dietary & life-style modification counselling, brushing instructions and demonstration, full mouth scaling, restorations, fluoride gel application, necessary referrals for further management and follow up of care.
Conclusion
In conclusion, our findings clearly demonstrate poor oral hygiene status of diabetic patients compounded by their poor glycaemic control and complications of diabetes. They may paint the general portrait of the picture of oral hygiene status among diabetic patients attending public hospitals in Sri Lanka with potential implications on their disease condition. Therefore, screening for oral diseases with referrals to oral health care seems an unmet need of emerging importance for diabetic patients.
References
- Kutulanda P, Rathnapala DAV, Sheriff R, Mathews DR (2011) Province and ethnic specific prevalence of diabetes among Sri Lankan adults. Sri Lanka Journal of Diabetes Endocrinology and Metabolism 1: 2-7.
- Emrich LJ, Shlossman M, Genco RJ (1991) Periodontal disease in non-insulin-dependent diabetes mellitus. J Periodontol 62(2): 123-131.
- Teshome A, Yitayeh A (2017) The effect periodontal therapy in glycemic control and fasting plasma glucose level in type 2 diabetic patients: systematic review and meta-analysis. BMC Oral Health 17(1): 31.
- Green JC, Vermillion JR (1964) The simplified oral hygiene index. J Am Dent Assoc 68: 7-13.
- Wellapuli N, Ekanayake L (2017) Risk factors for chronic periodontitis in Sri Lankan adults: a population based case–control study. BMC Res Notes 10: 460.
- Preshaw PM, de Silva N, McbCracken GI, Fernando DJ, Dalton CF, et al. (2010) Compromised periodontal status in an urban Sri Lankan population with type 2 diabetes. J Clin Periodontol 37(2): 165-171.
- Siyambalapitiya S, Gunathilake G, Perera I (2012) Exercise: an essential component in diabetes management. Sri Lanka Journal of Diabetes, Endocrinology and Metabolism 2: 57-60.






























