Family Social Support Perceptions and Medication Adherence among Elderly Diabetics in a Tertiary Health Institution in Lagos, Nigeria
Ayonote, Uzoramaka Angela1*, Akujuobi, Obianuju Mirian2 and Ogbonna, Adaobi Nneamaka1
1Department of Family Medicine, Lagos University Teaching Hospital, Nigeria
2Department of Counselling Psychology, Yorkville University, Canada
Submission: July 13, 2022; Published: July 21, 2022
*Corresponding author: Ayonote Uzoramaka Angela, Department of Family Medicine, Lagos University Teaching Hospital, Lagos, Nigeria
How to cite this article: Ayonote, U A, Akujuobi, O M, Ogbonna, A N. Family Social Support Perceptions and Medication Adherence among Elderly Diabetics in a Tertiary Health Institution in Lagos, Nigeria. Curre Res Diabetes & Obes J 2022; 16(1): 555927.DOI: 10.19080/CRDOJ.2022.16.555927
Abstract
Background: The perception of family support is pivotal in improving the health and wellbeing of elderly individuals through adherence to medication especially among diabetics. This study investigated the relationship between perceptions of family social support and medication adherence among individuals living with diabetes attending the outpatient clinics of the Lagos University Teaching Hospital (LUTH).
Methodology: This was a cross sectional, hospital-based study carried out among 199 randomly selected elderly diabetic patients receiving care in LUTH. Data including sociodemographic information, medication use, and procurement were obtained using an interviewer-administered semi-structured questionnaire. Perceived family social support was assessed and scored using the Perceived Social Support from Family Scale (PSS-Fa) and categorized as ‘strong’ (scores ≥ 11), ‘weak’ (scores 7-10) and ‘none’(scores≤6) while medication adherence was measured using the Morisky medication adherence scale (MMS-8). Medication adherence was rated high (score = 8), medium (scores= 6–7) and low (scores≤5). Association between perceived support and medication adherence was investigated by Chi-square test. Level of significance was p-value<0.05.
.Results: The mean age of the participants was 68.6 ± 6.7 years. The proportion of the participants who had strong, weak and no perceived family support were 92.5%, 3.5% and 4.0% respectively. Over two-thirds of participants (72.9%) reported family as responsible for providing funds to procure their medications while almost a quarter (23.6%) bought their medications by themselves. Only 2 (1.0%) participants relied on medical insurance to procure their medications. Almost half (49.7%) of them had high levels of medication adherence. Significant association existed between perceived family social support and medication adherence ( X2 = 7.626; p-value = 0.027).
Conclusion: Most participants had strong perceived family social support which was significantly associated with medication adherence. We recommend the routine assessment of family social support when dealing with geriatric patients as can improve medication adherence and ultimately better outcome of care.
Keywords: Geriatric; Elderly; Social support; Diabetic; Nigeria
Abbreviations: LUTH: Lagos University Teaching Hospital; PSS-Fa: Perceived Social Support from Family Scale; MMS-8: Morisky Medication Adherence Scale; DM: Diabetes Mellitus; OOP: Out-of-Pocket; GOPC: General Outpatient Clinic; LASUTH: Lagos State University Teaching Hospital; OOUTH: Olabisi Onabanjo University Teaching Hospital; UCH: University College Hospital; MSPSS: Multidimensional Scale of Perceived Social Support
Introduction
For elderly individuals experiencing health challenges to successfully adapt to managing ill-health, the family serves as a primary support unit [1,2]. The way in which an individual perceives support from the family with regards to the disease condition which is being experienced could have both positive or negative impacts on the treatment outcome.3 Perceived family support has been described as the subjective assessment made by an individual about the level of provision of different forms of emotional and instrumental services and assistance from family members [3]. A positive perception of family support has been associated with improved adherence to treatment and favorable outcomes in chronic diseases. This is more important for the elderly who may require support from family due to decline in functional status that occurs as they grow older [4,5] as well as due to the occurrence of non-communicable diseases such as diabetes mellitus which has been described as a major cause of morbidity and mortality among the elderly [6,7].
Diabetes mellitus (DM) is a metabolic disease characterized by hyperglycaemia resulting from deranged physiological mechanisms that control insulin secretion, insulin action, or both [8,9]. It has been reported that long term exposure to hyperglycaemia is a causative factor of long-term damage and failure of major organs [8,9]. It is a chronic debilitating disease with rising prevalence worldwide and is also a leading cause of non-traumatic amputations, blindness, and end-stage renal disease [10]. Reports have been made that have associated increasing age as a significant risk factor for diabetes considering that the prevalence of DM has increased over time with age and the highest prevalence has been reported among those aged between 60 and 79 years [11-15]. As at 2017, as much as 3.2 million deaths have been known to occur among the elderly due to complications of DM despite huge global investments to manage the condition among the elderly [16]. The financial strain associated with the management of diabetes mellitus is marked among the elderly living in developing countries like Nigeria where as much as 70 – 90% of the population personally make payments for their medical care by direct out-of-pocket (OOP) mechanism due to poor access to health insurance [17-19].
The need for support especially in terms of instrumental (physical/ financial/ material) and emotional (affection/ attention/ love) support to individuals (especially the elderly) nursing illnesses cannot be over-emphasized [20,21]. Family members are key sources of both forms of support considering that they provide instrumental support by financing hospital bills and cost of medications; helping patients schedule and keep clinic appointments; assistance and reminder with medications [22]. They also provide comfort and encouragement when the patients face distress or frustration over the long course of their diabetes care [22]. Informational support is another form of social support which involves providing advice, guidance, and suggestions to help solve problems [23]. A large proportion of the elderly especially within developing countries lack these forms of support [24]. A study in Ghana revealed that a large proportion of the elderly live alone, receiving inadequate support from their families [25]. Low level of family social support among the elderly persons with DM has also been reported in Libya [26]. Reports have also been made in South-south Nigeria regarding low levels of family support to elderly persons with only 21.9% of elderly patients reporting that they received the support they needed from their families [27]. A study in South-Eastern Nigeria has however reported better availability of family support to elderly patients than younger ones [28].
Apart from receiving social support, studies have also shown that adherence to medication regimens among this group of individuals is crucial to achieving successful treatment outcomes [29,30]. Medication adherence is defined as the extent to which a person’s behaviour such as taking medications or adapting to life-style modifications, corresponds with the recommendations from health care providers [30,31]. Considering that several studies have found that increasing age is a significant risk factor for diabetes [32-35] and that adherence to medication impacts on glycaemic control among elderly diabetic patients, it is crucial that all possible avenues be explored to promote good medication adherence among them. The achievement of good glycaemic control in diabetic patients especially in the elderly is most times hampered by certain challenges including having to take daily medications, combination of different medication regimens as well as frequent needle pricks in certain cases [29,30].These challenges coupled with the reduced capacity for self-care, cost of medications and lack of family support among elderly individuals, have been pinpointed as being contributory to instances of poor adherence and poor glycaemic control among individuals in this age group especially within developing countries [29,30].
Most studies on diabetes have been found to interestingly focus on the middle aged and young adults with paucity of such data among the elderly who form a major proportion of diabetics [36]. In developing countries, there is an increasing number of elderly patients lacking both the physical and financial capacity to care for themselves. Authors have shown evidence that the presence of family support can have a two-way effect of either having an influence or no influence on medication adherence in elderly diabetics [28,37]. Considering the rising prevalence of DM among the elderly who require high level of care and support due to the complexity of treatment regimens, as well as high rates of complications, the perception of family support and medication adherence among the elderly individuals living with diabetes is a source of concern and an area to be studied to provide necessary solutions. This study was thus conducted to assess the level of perceived family social support and how it impacts on medication adherence among elderly diabetic patients receiving care at a tertiary health care facility in Nigeria. The information generated from this study has provided a basis to advocate for incorporation of family support into the care for the elderly in order to achieve improved clinical outcomes.
Materials And Methods
This was a hospital-based cross-sectional study carried out at the Lagos University Teaching Hospital (LUTH), Idi-Araba, Lagos state The General Outpatient Clinic (GOPC) of the department of Family Medicine as well as the Endocrinology Clinic were utilized as the study sites for data collection. The study population consisted of elderly diabetic patients aged 60 years and above who had been on follow up at these clinics in LUTH for a minimum of six months [38]. Also, the six-item cognitive impairment test was used to objectively exclude patients having manifestations of cognitive impairment in order to ensure that the recruited population would be able to provide reliable answers to questions asked in the study instrument [39,40].
The sample size of 199 was calculated using the formula for calculating sample size for single proportions: [n = (Z2pq)/d2] [41]. The prevalence (p) of good adherence among elderly patients (≥ 60years) with diabetes (41%) was used for the calculation [38]. Sample size adjustment using 10% for possible missing or incomplete data was factored into the calculation. The formula to correct for finite population when a study population is less than 10,000 nf = [n/1+(n/N)] was also applied.
Study participants were recruited from both the GOPC and Endocrinology clinics using a systematic random sampling technique. Based on the proportion of patients’ attendance at each clinic, 15.6% of the sample size for this study was recruited from the GOPC (15.6% of 199 = 31.04 ≈ 32; rounded to the nearest whole person) while 84.4% of the sample size was recruited from the Endocrinology clinic (84.4% of 199 = 167.9 ≈ 168); over the study period of 12 weeks. The sampling interval was determined as follows: At GOPC: in order to recruit 3 patients per week out of 5 patients that attend the clinic per week, the sampling interval was 5/3 = 1.6 ~ 1. At the Endocrinology clinic: in order to recruit 14 patients out of 27 patients that attended the clinic per week the sampling interval was = 27/14 = 1.9 ~ 2.
The first participant for the day at the endocrinology clinic was selected through paper ballot between the first 2 patients that arrived at the clinic. The patient that picked “yes” was taken as the index participant. Thereafter, every second patient after the index patient was recruited for the study. This process was repeated every clinic day until the required sample size was recruited. At the GOPC using a sampling interval of 1 as previously calculated, the first patient that met the inclusion criteria was recruited, thereafter participants were recruited consecutively (sampling interval of 1) until the required number for that week (3 patients per week) was completed. Identification stickers were attached to the case file of every participant recruited until the study was completed in order to prevent duplication.
Two research assistants who helped in collection of data were trained by the research team two hours daily for three days before the commencement of the study. They were chosen based on their background medical knowledge and previous experience as research assistants. They were trained on greeting, creating a rapport, ensuring a comfortable and private environment, explanation of the data collection process, obtaining informed consent, administering the questionnaire. A semi-structured, interviewer administered questionnaire was used to collect data on the socio-demographic characteristics, perceived family social support and medication adherence characteristics of the respondents. Perceived family social support was assessed using the Perceived Social Support from Family Scale (PSS-Fa). This is a validated 20-item tool with an alpha coefficient of 0.90 which has been used in other studies [32,34,42]. A pre-test of the study questionnaire was conducted to check for the applicability of the questionnaire. It involved nineteen patients aged 60 years and above (10% of sample size) at the general outpatient and Diabetic clinic of Lagos State University Teaching Hospital (LASUTH), Ikeja, Lagos. Modifications were made, where necessary, for difficulty observed in answering certain questions.
Respondents answered ‘yes’, ‘no’ or ‘don’t know’ to each question with the positive responses scored as 1 and each negative answer was scored 0 [32]. Some of the questions had reversed scoring that is, a negative answer was scored 1 while a positive answer was scored 0 [32]. The maximum obtainable score was 20 while the minimum score was 0. Scores ≥ 11 suggested ‘strong perceived family support’, scores 7 to 10 suggested ‘weak perceived family support’ while scores less than or equal to 6 suggested ‘no perceived family support’ [32]. Medication adherence was assessed using the eight-item Morisky Medication Adherence Scale (MMAS-8). The responses to the first seven items were either ‘Yes’ or ‘No’ where a score of 0 was assigned for a ‘Yes’ response and 1 for a ‘No’ response. The exception to this was seen in items 5 and 8 where a ‘Yes’ response in item 5 attracted a score of 1 and a ‘No’ response attracted a score of 0. The response for the 8th item was scored based on a five-point Likert scale. A response indicating ‘never/rarely’ attracted a score of 1 while choosing any of the other options on the scale attracted a score of 0. All scores obtained were summed up to a total score, which ranged from 0 to 8. The total score for each participant indicated the level of their adherence to medications. A score of 8 signified high adherence, 6-7 medium adherence while a score of 5 and below signified low adherence [43].
Each completed questionnaire was cross-checked for completeness by the researcher after every interview. The data obtained was entered serially into Statistical package for Social Sciences IBM version 23 was used for data entry and analysis. Descriptive statistics (frequencies and percentages) was used to describe the socio-demographic characteristics of the respondents, their perceived family support and medication adherence categories. The results obtained were presented using frequency tables or charts. The association between perceived family social support and medication adherence was analyzed using the Chi squared test (or the Fisher’s exact test where one or more cells had expected frequency <5). The logistic regression analytical test was also used to determine predictor relationship between variables. The level of statistical significance was set at p < 0.05. Approval for this study was granted by the Health Research and Ethics Committee of LUTH. A written informed consent was obtained from each participant at recruitment into the research. The privacy of participants was maintained, and all information obtained were kept confidential. Detected health problems were also explained to the participants with their consent and the questionnaires were safely and securely stored. Immediate results were discussed, and appropriate education provided to the participants. The participants were also informed that their participation in the study was completely on a voluntary basis and that they could withdraw from the study at any time they chose as it would not affect their care.
Results
Sociodemographic characteristics, medication use and procurement among participants
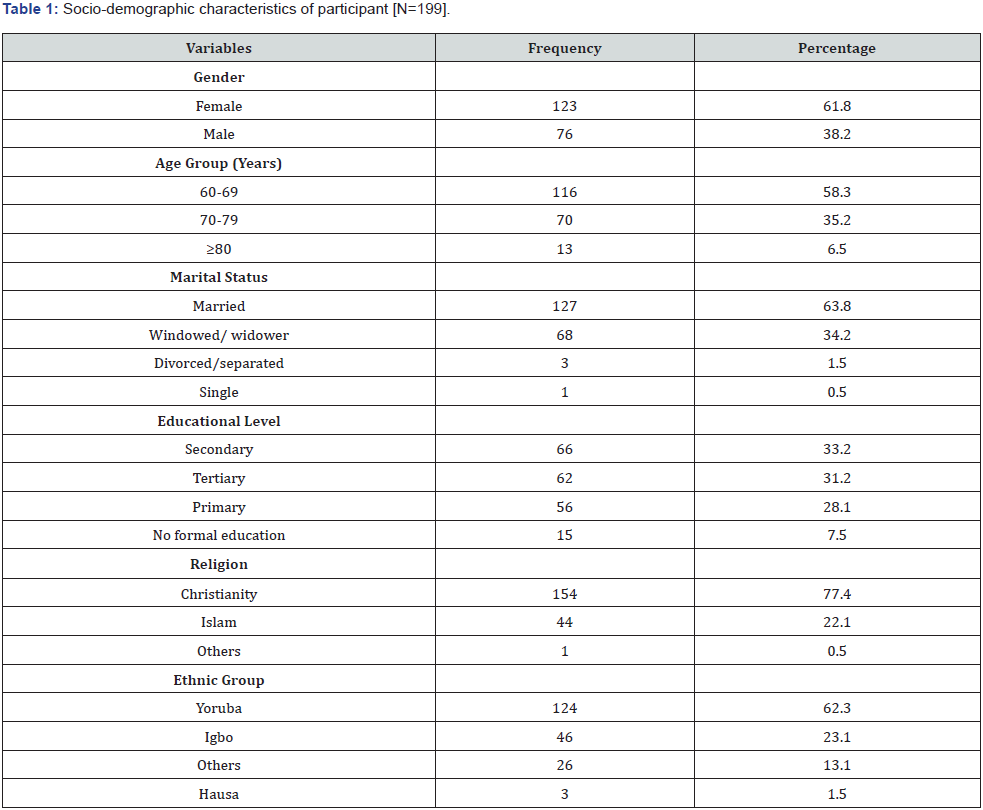
Table 1 shows the sociodemographic characteristics of the participants. The mean age of participants was 68.6±6.7 years. Majority 116(58.3%) were in the age group 60-69 years, were married 127(63.8%) and had mostly obtained secondary 66 (33.2%) and tertiary level of education 62(31.2%). Most participants were Christians (77.4%) and 124 participants (62.3%) were of the Yoruba ethnic extraction.
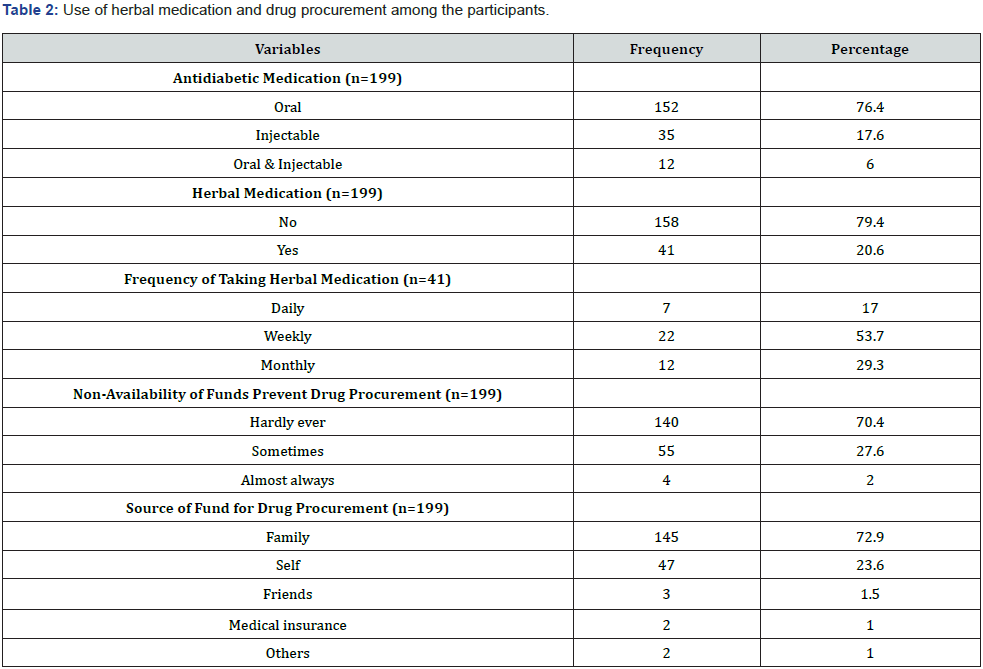
Table 2 shows the type of antidiabetic medications used by the participants as well as use of herbal concoctions. Regarding this,152 participants (76.4%) used oral anti-diabetic medications, 35 participants (17.6%) used injectable, and 12 participants (6.0%) used both oral and injectable. As much as 140 participants (70.4%) reported having availability of funds for procuring their medication while only four participants (2.0%) reported that non-availability of funds almost always prevented them from procuring their drugs. As much as 145 participants (72.9%) believed their families were responsible for providing funds to procure their medications while almost a quarter (23.6%) bought their medications by themselves.
Pattern of perceived family social support among the participants
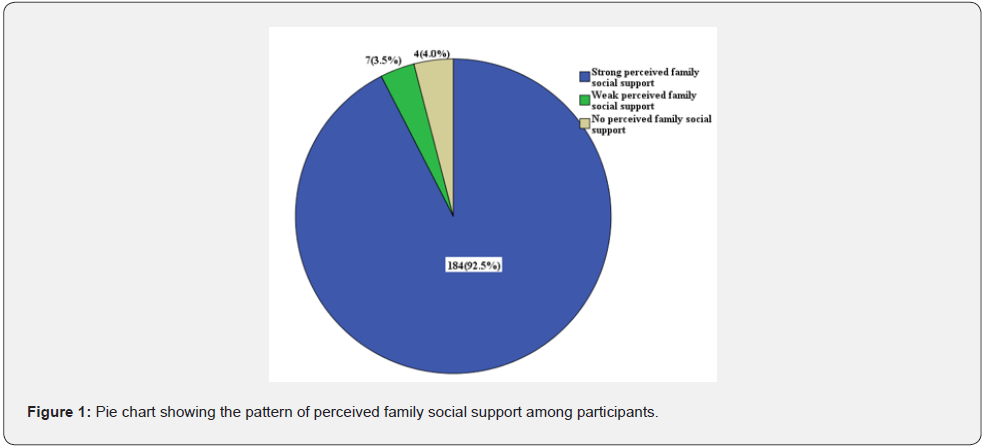
Figure 1 shows the pattern of perceived family social support among the participants. About 9 in 10 participants (92.5%) had strong perceived family social support while 7 (3.5%) had weak perception of family social support and 8 (4.0%) had no perception of family social support.
Pattern of medication adherence among the participants
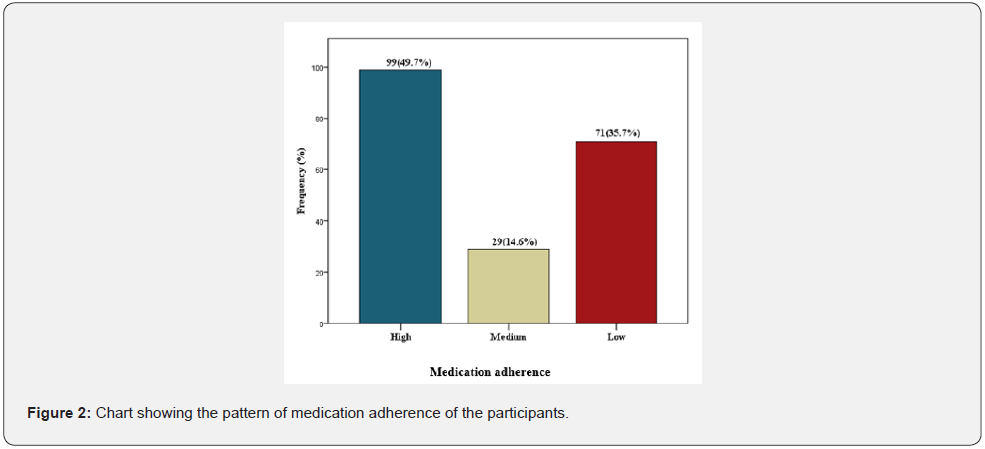
Figure 2 shows the pattern of medication adherence among the participants. Almost half (49.7%) of the participants were found to have high level of medication adherence while 14.6% had medium level of medication adherence and 35.7% had low level of medication adherence.
Association between perceived family support and medication adherence
Table 3 shows the association between perceived family social support and medication adherence. It was observed that 95 participants (51.6%) who had a strong perception of family support had high adherence to their medication meanwhile, six out of the eight participants (75.0%) who had no perception of family support had low adherence to medications. A larger proportion of participants who had weak family social support also had low adherence to their medication, strong perceived family support was also associated with high medication adherence. These associations were statistically significant (ꭓ2=7.63, p-0.027). Table 3 also shows that the absence of perceived family support is an independent predictor of low medication adherence. Participants who had no family support had five times odds (OR=5.785; 95%CI=1.931-24.597) of having low medication adherence compared to those who had strong perception of family support.
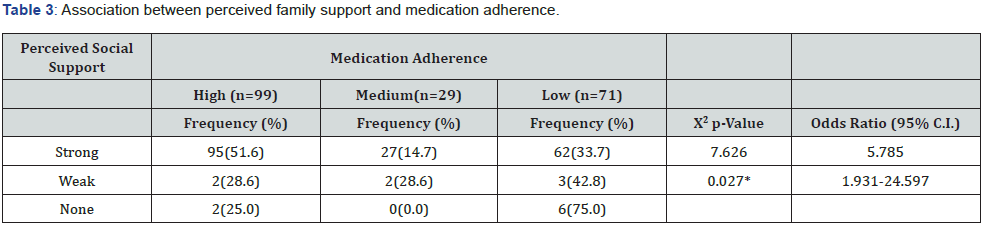
X2= Chi-square; *Significant p ≤0.05; Fishers exact was used where cells are <5; 95% C.I. = 95% Confidence Interval
Discussion
This present study showed that the perception of family support among the participants was high as most of them reported a strong perception of family support. Also, a statistically significant association was found to exist between perceived family support and medication adherence. This finding of high levels of perception of family social support could be as a result of this study being a hospital-based study and more of the patients with good support were being encouraged to present at the clinic. The finding of high prevalence of strong family support in this study was similar to findings of Timi-Oladapo and those of Iloh & Amadi [28,44] who reported prevalence of 99% and 77.5% respectively. These similarities can be attributed to the fact that both studies were hospital based and also the use of the same instrument (perceived social support-family scale- PSSFa) for assessing family support in the study by Timi-Oladapo. The implication of this finding brings to fore the positive impact which perception of family support would have on adherence and treatment outcome among elderly individuals with chronic diseases especially diabetes [3].
This notwithstanding, the findings of this study disagreed with the findings of a study conducted in South-south Nigeria where it was reported that only 21.9% of the elderly participants reported good family support [27]. The difference in the prevalence reported in both studies could be attributed to the community-based nature of the study. More so, the result of this study was also in contrast with the report of Ojewale et al. [45] who found that only 59.9% of their participants reported having good family support. This was not as high as what was obtained in the present study and the difference may be attributed to the differing study areas of both studies as well as differences in culture. Ojewale’s study was done at two locations in Southwestern Nigeria- the University College Hospital (UCH), Oyo State and Olabisi Onabanjo University Teaching Hospital (OOUTH) in Ogun State, while the present study was conducted in a teaching hospital located in Lagos State. Each of these study locations may have their unique characteristics that may have influenced the results. The difference in the results could also be due to the age category of the participants used for the different studies. Ojewale recruited participants aged 18 years and above while this study was focused only on the elderly. A larger proportion of the younger participants in the study by Ojewale et al may have been able to care for themselves and may not have had the need to rely on their family, unlike the elderly who in most cases require more support and care from their family members [4,5].
Other studies have also presented differing views in contrast to what was found in this present study [38,46,47]. These studies reported prevalence of high perceived family social support to be 43.3% [38], 48.8% [46] and 43.8% [47] respectively. The reasons for these differences could have been as a result of a number of factors including the consideration of younger age groups in these studies as against this present study that focused on the elderly. Another reason was because of the kind of instrument used to assess perceived social support in the study by Affusim and Francis which was the multidimensional scale of perceived social support (MSPSS) as against the use of the perceived social support-family scale (PSS-Fa) instrument in this present work. This thus leaves no doubt of the need to conduct more of these studies that are focused on the elderly population which is necessary to ensure inclusiveness of this age group of individuals to receive quality health care, attain improved health outcomes as well as ensure an improved quality of life [46,47].
Regarding the significant association found to exist between perceived family support and medication adherence in the present study, those who had no perceived family support were found to be five times more likely to have poor medication adherence than those who had strong perceived family support. The implication of this finding points to the beneficial effects which having strong perceived family support has on achieving optimal medication adherence among elderly individuals managed for diabetes mellitus. This finding is supported by those of Dehdari & Dehdari [48] in Iran who reported an association between the presence of good family support and medication adherence. Olowookere et al. [40] also found a significant association between both variables. The participants in their study who reported having good family support were shown to have better adherence to their medication compared to those with poor family support [49].
Despite the positively-associated finding between perceived family support and medication adherence as well as other supporting evidence, the findings of Anene-Okeke et al. [36] were different. They found that the presence of family support had no impact on medication adherence and this difference may be attributed to the different socio-demographic characteristics of the participants in their study compared to the present study. The largest proportion of the participants in Anene-Okeke et al. [36] study had received primary level of education while, majority of the participants in this study had received secondary and tertiary level of education. This may have been a reason why they seemed to adhere better to their medication considering that they were educated enough to understand the importance of medication adherence in contrast to participants in Anene-Okeke et al. [36] study. Additionally, the different methods used in assessing perceived family support in the studies maybe have contributed to the difference in results. This contrasting study used the diabetes family behavioral checklist to measure family support while the perceived social support-family scale was used to assess perceived family support in this study. Another possible reason for the difference in results could have also been the type of social support (instrumental versus emotional) that was actually perceived by the participants in each study [37].
Despite these differences, more of the evidence however points to the fact that when individuals have good perception of family support in terms of emotional, informational, or instrumental support; they tend to have better adherence to their medications [50,51].
Conclusion
The provision of family social support was perceived as being strong among elderly diabetic individuals receiving care at the Lagos University Teaching Hospital in Lagos State, Nigeria. It was recommended that family physicians and other health care provider of/for the elderly should routinely assess the perception of family support among elderly patients in clinical practice, in order to advocate for better support for the elderly. This is because diabetes care is often multi-faceted, and the day-to-day management could be overwhelming for the elderly. Policies that promote health insurance and financial aids for the elderly should also be formulated and implemented in order to reduce the financial burden of treatment among elderly individuals.
References
- Grossman BR, Magana S (2016) Introduction to the special issue Family support of persons with disabilities across the life course. Journal of Family Social Work 19(4): 237-251.
- Mayberry LS, Osborn CY (2012) Family support, medication adherence, and glycemic control among adults with type 2 diabetes. Diabetes Care 35(6): 1239-1245.
- Amiya RA, Poudel KC, Poudel-Tandukar K, Pandey BD, Jimba M (2014) Perceived family support depression and suicidal ideation among people living with HIV/AIDS. A cross-sectional study in the Kathmandu Valley Nepal PLoS ONE 9(3): e90959.
- Hartmann M, Bäzner E, Wild B, Eisler I, Herzog W (2010) Effects of interventions involving the family in the treatment of adult patients with chronic physical diseases A meta- analysis. Psychother Psychosom 79(3): 136-148.
- Shrestha S, Poudel KC, Poudel-Tandukar K, Kobayashi J, Pandey BD, et al. (2014) Perceived family support and depression among people living with HIV/AIDS in the Kathmandu Valley, Nepal. Journal of the International Association of Providers of AIDS care (JIAPAC) 13(3): 214-222.
- Mini GK, Thankappan KR (2017) Pattern correlates and implications of non-communicable disease multi-morbidity among older adults in selected Indian states a cross-sectional study. BMJ Open 7(3): e013529.
- (2013) United Nations, Department of Economic and Social Affairs, Population Division. World Population Ageing. ST/ESA/SER.A/348, 2013. Available at http://www.un.org/en/development/desa/population/publications/pdf/ageing/WorldPopulationAgeing2013.pdf Accessed on 16/12/19.
- Kharroubi AT, Darwish HM (2015) Diabetes mellitus the epidemic of the century. World J Diabetes 6(6): 850-867.
- Dal-Canto DE, Ceriello A, Rydén L, Ferrini M, Hansen TB, et al. (2019) Diabetes as a cardiovascular risk factor an overview of global trends of macro and micro vascular complications. European Journal of Preventive Cardiology 26(2): 25-32.
- Dieren SV, Beulens JW, Van-der Schouw YT, Grobbee DE, Nealb B (2010) The global burden of diabetes and its complications An emerging pandemic. European Journal of Cardiovascular Prevention & Rehabilitation 17(Suppl 1): S3-8.
- Guariguata L, Whiting DR, Hambleton I, Beagley J, Linnenkamp U, et al. (2014) Global estimates of prevalence of diabetes in adults for 2013 and projections to 2035. Diabetes Res Clin Pract 103(2): 137-149.
- Uloko AE, Musa BM, Ramalan MA, Gezawa ID, Puepet FH, et al. (2018) Prevalence and risk factors for diabetes mellitus in Nigeria A systematic review and meta-analysis. Diabetes Therapy 9(3): 1307-1316.
- Sabir AA, Balarabe S, Sani AA, Isezuo SA, Bello KS, et al. (2017) Prevalence of diabetes mellitus and its risk factors among the suburban population of Northwest Nigeria. Sahel Med J 20(4): 168-172.
- Arugu G M, Maduka O (2017) Risk factors for diabetes mellitus among adult residents of a rural District in Southern Nigeria Implications for prevention and control. Niger J Clin Pract 20(12): 1544-1549.
- Coetzee A, Beukes A, Dreyer R, Solomon S, Van-Wyk L, et al. (2019) The prevalence and risk factors for diabetes mellitus in healthcare workers at Tygerberg hospital Cape Town South Africa A retrospective study. Journal of Endocrinology Metabolism and Diabetes of South Africa 24(3): 77-82.
- (2017) International diabetes federation. IDF Diabetes atlas 8th edition. Available at www.diabetesatlas.org. Accessed on 16/12/19.
- Aregbeshola BS, Khan SM (2018) Out-of-pocket payments catastrophic health expenditure and poverty among households in Nigeria 2010. Int J Health Policy Manag 7(9): 798-806.
- Oyibo PG (2011) Out-of-pocket payment for health service Constraints and implications for government employees in Abakaliki Ebonyi State South-East Nigeria. Afr Health Sci 11(3): 481-485.
- Etobe UE, Etobe EI (2015) The national health insurance scheme and its implication for elderly care in Nigeria. International Journal of Science and Research 4(2): 128-132.
- Santos VD, Pedrosa SC, Aquino PD, Lima IC, Cunha GH, et al. (2018) Social support of people with HIV/AIDS The social determinants of health model. Revista Brasileira de Enfermagem 71(Suppl 1): 625-630.
- Scheurer D, Choudhry N, Swanton KA, Matlin O, Shrank W (2012) Association between different types of social support and medication adherence. American Journal of Managed Care 18(12): 461-467.
- Pamungkas RA, Chamroonsawasdi K, Vatanasomboon P (2017) A systematic review Family support integrated with diabetes self-management among uncontrolled type II diabetes mellitus patients. Behavioural Sciences 7(3): 62.
- Strom JL, Egede LE (2012) The impact of social support on outcomes in adult patients with type 2 diabetes A systematic review. Current Diabetes Reports 12(6): 769-781.
- Dai Y, Zhang CY, Zhang BQ, Li Z, Jiang C, et al. (2016) Social support and the self-rated health of older people A comparative study in Tainan Taiwan and Fuzhou Fujian province. Medicine 95(24): e3881.
- Aboagye E, Agyemang OS, Tjerbo T (2014) Elderly demand for family-based care and support Evidence from a social intervention strategy. Global Journal of Health Science 6(2): 94-104.
- Fattah-Badr S, Elmabsout A, Denna I (2014) Family support, malnutrition and barriers to optimal dietary intake among elderly diabetic patients in Benghazi Libya. J Community Med Health Educ 4(2): 1-6.
- Okumagba PO (2011) Family support for the elderly in Delta State Nigeria. Stud Home Comm Sci 5(1): 21-27.
- Iloh GU, Amadi AN (2018) Family support, medication adherence and glycaemic control among ambulatory type 2 diabetic Nigerians in a primary care clinic in Eastern Nigeria. J Health Res Rev 5(2): 71-77.
- Yap AF, Thirumoorthy T, Kwan YH (2016) Medication adherence in the elderly. Journal of Clinical Gerontology and Geriatrics 7(2): 64-67.
- Bazargan M, Smith J, Yazdanshenas H, Movassaghi M, Martins D (2017) Non-adherence to medication regimens among older African-American adults. BMC Geriatr 17(1): 163.
- Lam WY, Fresco P (2015) Medication adherence measures An Overview. BioMed Research International 2015: 217047.
- Uloko AE, Musa BM, Ramalan MA, Gezawa ID, Puepet FH, et al. (2018) Prevalence and risk factors for diabetes mellitus in Nigeria A systematic review and meta-analysis. Diabetes Therapy 9(3): 1307-1316.
- Sabir AA, Balarabe S, Sani AA, Isezuo SA, Bello KS, et al. (2017) Prevalence of diabetes mellitus and its risk factors among the suburban population of Northwest Nigeria. Sahel Med J 20(4): 168-172.
- Arugu GM, Maduka O (2017) Risk factors for diabetes mellitus among adult residents of a rural District in Southern Nigeria: Implications for prevention and control. Niger J Clin Pract 20(12): 1544-1549.
- Coetzee A, Beukes A, Dreyer R, Solomon S, Van-Wyk L, et al. (2019) The prevalence and risk factors for diabetes mellitus in healthcare workers at Tygerberg hospital, Cape Town, South Africa A retrospective study. Journal of Endocrinology Metabolism and Diabetes of South Africa 24(3): 77-82.
- Odume BB, Ofoegbu OS, Aniwada EC, Okechukwu EF (2015) The influence of family characteristics on glycaemic control among adult patients with type 2 diabetes mellitus attending the general outpatient clinic national hospital Abuja Nigeria. South African Family Practice 57(6): 347-352.
- Anene-Okeke CG, Adibe MO, Ukwe CV, Aguwa CN (2019) The impact of family support on medication adherence and glycemic control of type 2 diabetes outpatients in a Nigerian tertiary hospital. J Pharm Sci Therap 5(1): 295-300.
- Egunjobi AO, Ojo OS, Malomo SO, Sogunle PT (2018) Medication adherence and perceived family support among patients with type 2 diabetes mellitus seen at a primary care clinic in Southwest Nigeria. Nigerian Journal of Family Practice 9(2): 21-31.
- O'Sullivan D, O'Regan NA, Timmons S (2016) Validity and reliability of the 6-item cognitive impairment test for screening cognitive impairment: A review. Dementia and Geriatric Cognitive Disorders 42(1-2): 42-49.
- Apóstolo JL, Paiva DD, Silva RC, Santos EJ, Schultz TJ (2018) Adaptation and validation into Portuguese language of the six-item cognitive impairment test (6CIT). Aging & Mental Health 22(9): 1184-1189.
- Charan J, Biswas T (2013) How to calculate sample size for different study designs in medical research. Indian J Psychol Med 35(2): 121-126.
- Procidano ME, Heller K (1983) Measures of perceived social support from friends and from family Three validation studies. Am J Community Psycho 11(1): 1-24.
- Morisky DE, Ang A, Krousel-Wood M, Ward HJ (2008) Predictive validity of a medication adherence measure in an outpatient setting. Journal of Clinical Hypertension 10(5): 348-354.
- Timi-Oladipo AO (2017) Association between family support and glycaemic control in elderly type 2 diabetics attending the outpatient clinic of university of Ilorin teaching hospital, Ilorin Nigeria. Faculty of Family Medicine. Available at: https://www.dissertation.npmcn.edu.ng/index.php/FMCFM/article/view/217/1844.
- Ojewale LY, Oluwatosin AO, Fasanmade AA, Odusan O (2019) A survey on patients' characteristics perception of family support and diabetes self-management among type 2 diabetes patients in South-West Nigeria. Nursing Open 6(2): 208-215.
- Affusim CC, Francis E (2018) The influence of family/social support on adherence to diabetic therapy. International Journal of Advances in Scientific Research and Engineering 4(5): 71-80.
- Osuji NA, Ojo OS, Malomo SO, Sogunle PT, Egunjobi AO, et al. (2018) Relationship between glycaemic control and perceived family support among people with type 2 diabetes mellitus seen in a rich kinship network in South-West Nigeria. Family Medicine and Community Health 6(4): 168-177.
- Dehdari L, Dehdari T (2019) The determinants of anti-diabetic medication adherence based on the experiences of patients with type 2 diabetes. Archives of Public Health 77: 21.
- Olowookere AJ, Olowookere SA, Talabi AO, Etonyeaku AC, Adeleke OE (2015) Perceived family support and factors influencing medication adherence among hypertensive patients attending a Nigerian tertiary hospital. Ann Trop Med Public Health 8(6): 241-245.
- Yakaryılmaz FD, Öztürk ZA (2017) Treatment of type 2 diabetes mellitus in the elderly. World Journal of Diabetes 8(6): 278-285.
- Ijoma UN, Unaogu NN, Onyeka TI, Nwatu CB, Onyekonwu CL, et al. (2019) Health-related quality of life in people with chronic diseases managed in a low-resource setting – A study from Southeast Nigeria. Niger J Clin Pract 22(9): 1180-1188.






























