Effect of body mass index on Disease progression in Chronic Hepatitis B Patients
Lamiaa Mobarak*
National Hepatology and Tropical Medicine Research Institute, Egypt
Submission: June 25, 2018;Published: January 08, 2019
*Corresponding author: Lamiaa Mobarak, National Hepatology and Tropical Medicine Research Institute, 10 kasr Al-Ainy street, Cairo, Egypt
How to cite this article: Lamiaa Mobarak. Effect of body mass index on Disease progression in Chronic Hepatitis B Patients Curre Res Diabetes & Obes J. 2019; 9(3): 555761. DOI:10.19080/CRDOJ.2019.09.555761
Abstract
Background and study aim: In recent years the burden of obesity and metabolic syndrome has been increasing. These diseases are associated with increased risk for chronic hepatitis B virus infection as well as worsened outcomes. The aim of this study was to investigate the association between obesity, defined according to body mass index, and hepatitis B viral load and fibrosis stage among chronic hepatitis B Egyptian patients.
Methods: We performed a retrospective study on 50 patients with chronic hepatitis B virus infection at National Hepatology and Tropical Medicine Research Institute, Cairo, Egypt. The essential outcomes were laboratory tests, ultrasonography, and liver biopsy. Data analysis was used to reveal whether high BMI was a variable related to disease progression.
Results: A total of 50 HBsAg seropositive participants. All patients were classified into two groups according to BMI (non-obese, <30 kg/m2; and obese, ≥30 kg/ m2). Obese patients ≥30 kg/m2 were at higher risk for elevated serum levels of ALT (P=0.5) and for lower serum levels of HBV DNA (P=0.08). Bright liver, liver cirrhosis, and splenomegaly were higher in obese patients than in non-obese. A1 was the commonest among obese and non-obese (74.1% and 91.3%) respectively. Also, F1 was the commonest among obese and non-obese (66.7% and 56.5%) respectively. No statistically significant difference was detected between obesity and fibrosis stage.
Conclusion: Subjects with body mass index ≥30 kg/m2 were at higher risk for elevated serum levels of ALT and for lower serum levels of HBV DNA and possible liver cirrhosis based on ultrasonographic findings. We did not find association between obesity and stage of fibrosis.
Keywords: Hepatitis B virus; Body mass index; Liver biopsy; Liver fibrosis; Chronic liver disease; Obesity; Fatty liver disease; Steatosis; Metabolic risk factors; Hepatitis B; Liver disease
Abbreviations: HBV: Hepatitis B Virus; CLD: Chronic Liver Disease; NAFLD: Non-Alcoholic Fatty Liver Disease; CBC: Complete Blood Picture; AST: Aspartate Aminotransferase; ALT: Alanine Aminotransferase; AFP: Alpha Fetoprotein; PCR: Polymerase Chain Reaction; BMI: Body Mass Index; SD: Standard Deviation; HCC: Hepatocellular Carcinoma; MS: Metabolic Syndrome
Introduction
Chronic hepatitis B virus (HBV) infection leads to progressive liver fibrosis and is the leading cause of chronic liver disease (CLD) [1,2]. Furthermore, as the incidence of obesity rises in the general population, non-alcoholic fatty liver disease (NAFLD) is also emerging as a disease of significant concern. NAFLD affecting more than 30% of adults in developed countries [3]. Coexistent steatosis is common in chronic hepatitis B infection and is also strongly associated with more advanced liver disease [4].
Obesity is one of metabolic risk factors associated with NAFLD that have recently emerged as potential cofactors in the development of fibrosis in cases of chronic HCV and HBV [5-7].
Consequently, the evaluation of hepatic fibrosis is highly important in the management of patients with CLD. In spite of certain limitations, histological assessment is the classic method to determine the extent of hepatic fibrosis [8]. As such, we used liver biopsy in the present study, to investigate the relationship between obesity and the risk of liver disease progression in chronic hepatitis B infection among this special patient group.
Aim of the work
Was to examine whether obesity according to body mass index was associated with higher hepatitis B viral load and more progressive disease in chronic hepatitis B Egyptian patients.
Patients and methods
Patients: This retrospective study included 50 patients with chronic hepatitis B presented to the out-patient clinics of the National Hepatology and Tropical Medicine Research Institute, Cairo, Egypt. Diagnosis of HBV was based on detection of HBsAg and quantitative HBV DNA by PCR. Patients with malignancy, decompensated liver disease, Patients with HIV infection or hepatitis B and C co-infection and presence of absolute contraindication for liver biopsy were excluded from this study. An informed written consent was obtained from all patients in the study and according to the Declaration of Helsinki.
Data collection: All patients were subjected to basic laboratory tests including: Complete blood picture (CBC), Aspartate aminotransferase (AST), Alanine aminotransferase (ALT), serum albumin, total bilirubin, INR, Alpha fetoprotein (AFP), hepatitis seromarkers for HCV (anti HCV) and for hepatitis B virus (HBV); (HBsAg, anti HBc and anti HBs) using ELISA technique. HBV DNA was tested by quantitative polymerase chain reaction (PCR).
The following clinical parameters were recorded: age, sex, and body mass index (BMI). Ultrasound guided liver biopsies were performed. Fibrosis was staged according to the METAVIR scoring system from F0 to F4 as: F0 (no fibrosis), F1 (mild fibrosis without septa), F2 (moderate fibrosis with few septa), F3 (severe fibrosis with numerous septa without cirrhosis) and F4 (cirrhosis) [9]. All patients were classified into two BMI groupings (non-obese, <30 kg/m2; obese, ≥30 kg/ m2).
Statistical analysis
Numerical data were presented as means±standard deviation (S.D), while categorical data were presented as number (percent). The Mann-Whitney U test and the Chi-square test were used when appropriate. Statistical significance was considered if P value was less than or equal 0.05.
Result
The study was conducted on 50 chronic hepatitis B patients. They presented to the outpatient clinic of the National Hepatology and Tropical Medicine Research Institute, Cairo, Egypt.
The mean age of obese patients was 39.9+ 7.2 years, while the mean age of non-obese patients was 33.2+ 10.9 years, with a statistical significance (P=0.02). There was male predominance in both groups, without a statistical significance in relation to sex (P=0.3). Regarding the laboratory results, the significant difference was confined to hemoglobin which was significantly higher in obese than in non-obese patients (P=0.02). ALT level was elevated in obese patients compared with non-obese without a significant difference (P=0.5).
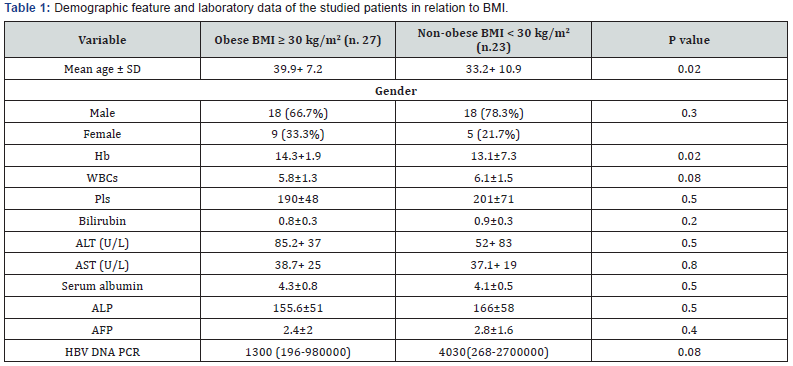
Obese patients (BMI ≥ 30 kg/m2) had lower HBV DNA PCR than in non-obese, however, did not show a statistical significance (P=0.08) (Table 1).
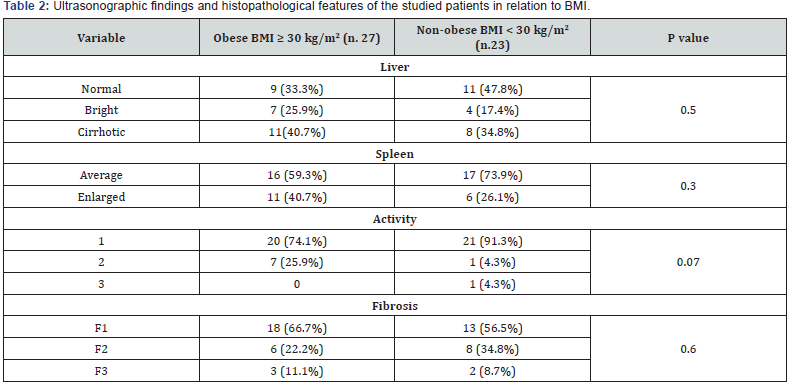
The ultrasound findings showed that bright liver, liver cirrhosis, and splenomegaly were higher in obese patients than in non-obese. There was not a statistical significance in abdominal ultrasonographic findings between both groups. A1 was the commonest among obese and non-obese (74.1% and 91.3%) respectively. Also, F1 was the commonest among obese and non-obese (66.7% and 56.5%) respectively. No statistically significant difference was detected between obesity and fibrosis stage (Table 2).
Discussion
Chronic hepatitis B virus (HBV) infection is a challenging disease worldwide [10]. It is well-known that HBV infection is a main risk factor for hepatic fibrosis, cirrhosis and hepatocellular carcinoma (HCC) [11-14]. It is significant to exactly predict the stage of liver fibrosis progression in chronic viral hepatitis patients, which has significant implications for prognosis and treatment [15].
Metabolic syndrome (MS) involves three characteristics of the following: dyslipidemia, an impaired fasting glucose metabolism, hypertension or central obesity [15,16].
It is vastly known that hepatitis C virus infection might increase the risk of metabolic syndrome and diabetes mellitus [17,18]. HBV and its relationship with metabolic syndrome have also become a focus of research [19]. In the current study, we investigated whether obesity, according to body mass index, was associated with higher hepatitis B viral load and more progressive disease in chronic hepatitis B Egyptian patients.
There are only few studies regarding the relationships of chronic hepatitis B infection with obesity. In the present study we did not find any association between chronic hepatitis B infection and obesity, as Obese patients (BMI ≥ 30 kg/m2) had lower HBV DNA PCR than in non-obese, however, it did not show a statistical significance (P=0.08). This is consistent with previous studies [20,21] which found that extreme obesity was associated with low HBV viral load and was a significant predictor of HBsAg seroclearance in chronic hepatitis B patients. This may be a reason why HBV patients with higher BMI had less fatty liver. Jinjuvadia et al, [22] observed among patients with chronic HBV infection, a lower odd of having central obesity.
The relationship between chronic HBV infection, and abnormal liver function, is complex. Patients with chronic HBV infection have a higher risk of abnormal liver function, such as elevated ALT levels [10]. Previous studies have also confirmed the predictive role of an elevated ALT level with an increased incidence of metabolic syndrome [23,24], and it is consistent with the present study as ALT level was elevated in obese patients compared with non-obese without a significant difference (P=0.5).
High BMI is involved in the transition from HBV carrier state to hepatocellular carcinoma (HCC) and liver-related mortality [25,26]. Similarly, in the present study the ultrasound findings showed that bright liver, liver cirrhosis, and splenomegaly were higher in obese patients than in non-obese.
In a study including 850 HBV patients, the prevalence of MS was found to be 5%. The extent of liver fibrosis was found more serious in patients accompanying metabolic syndrome. Body mass index (BMI) was one of the factors that showed association with advanced fibrosis (fibrosis stages 3 to 4). In multivariate analysis, metabolic syndrome was found to be independently associated with liver fibrosis [27].
In a recent prospective cohort study of 663 CHB patients, obesity was found to be associated with liver fibrosis progression [7]. Even the effect of such coincident, metabolic syndrome was most apparent in the immune tolerant phase. Its effect was independent of the change in viral load and ALT level [7]. This is supported by the observation from a survey in general population that CHB is associated with a lower prevalence of fatty liver, hypertriglyceridemia and metabolic syndrome [7].
These studies are consistent with the current study in which obese subjects with BMI ≥ 30 kg/m2 were not associated with advanced fibrosis as shown in histologic examination.
Conclusion
Subjects with body mass index ≥30 kg/m2 were at higher risk for elevated serum levels of ALT and for lower serum levels of HBV DNA and possible liver cirrhosis based on ultrasonographic findings. We did not find association between obesity and stage of fibrosis.
References
- ASF Lok, BJ McMahon (2007) Chronic hepatitis B. Hepatology 45(2): 507-539.
- (2007) Asian Pacific Association for the Study of the Liver (APASL) hepatitis C working party. Asian Pacific Association for the Study of the Liver consensus statements on the diagnosis, management and treatment of hepatitis C virus infection. J Gastroenterol Hepatol 22: 615-633.
- JD Browning, LS Szczepaniak, R Dobbins, P Nuremberg, JD Horton, et al. (2004) Prevalence of hepatic steatosis in an urban population in the United States: impact of ethnicity. Hepatology 40(6): 1387-1395.
- S Petta, C Cammà, V Di Marco, FS Macaluso, M Maida, et al. (2011) Hepatic steatosis and insulin resistance are associated with severe fibrosis in patients with chronic hepatitis caused by HBV or HCV. Liver Int 31(4): 507-515.
- LF Hourigan, GA Macdonald, D Purdie, VH Whitehall, C Shorthouse, et al. (1999) Fibrosis in chronic hepatitis C correlates significantly with body mass index and steatosis. Hepatology 29(4): 1215-1219.
- Á Mena, JD Pedreira, Á Castro, S López, P Vázquez, et al. (2014) Metabolic syndrome association with fibrosis development in chronic hepatitis B virus inactive carriers. J Gastroenterol Hepatol 29(1): 173- 178.
- GL Wong, HL Chan, Z Yu, AW Chan, PC Choi, et al. (2014) Coincidental metabolic syndrome increases the risk of liver fibrosis progression in patients with chronic hepatitis B–a prospective cohort study with paired transient elastography examinations. Aliment Pharmacol Ther 39(8): 883-893.
- A Regev, M Berho, LJ Jeffers, C Milikowaski, EG Molina, et al. (2002) Sampling error and inter-observer variation in liver biopsy in patients with chronic HCV infection. Am J Gastroenterol 97(10): 2614-2618.
- Bedossa P, Poynard T (1996) An algorithm for the grading of activity in chronic hepatitis C. Hepatology 24(2): 289-293.
- Ganem D, Prince AM (2004) Hepatitis B virus infection-natural history and clinical consequences. N Engl J Med 350(11): 1118-1129.
- Friedman SL (2010) Evolving challenges in hepatic fibrosis. Nat Rev Gastroenterol Hepatol 7(8): 425-436.
- Hernandez-Gea V, Friedman SL (2011) Pathogenesis of liver fibrosis. Annu Rev Pathol 6: 425-456.
- Chan HL, Sung JJ (2006) Hepatocellular carcinoma and hepatitis B virus. Semin Liver Dis 26(2): 153-161.
- Wong GL, Chan HL, Chan HY, Tse PC, Tse YK, et al. (2013) Accuracy of risk scores for patients with chronic hepatitis B receiving entecavir treatment. Gastroenterology 144(5): 933-944.
- Gristina V, Cupri MG, Torchio M, Mezzogori C, Cacciabue L, et al. (2015) Diabetes and cancer: A critical appraisal of the pathogenetic and therapeutic links. Biomed Rep 3(2): 131-136.
- (2001) Summary of The Third Report of The National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, And Treatment of High Blood Cholesterol In Adults (Adult Treatment Panel III) JAMA 285: 2486-2497.
- Jaroszewicz J, Flisiak R (2013) Metabolic syndrome and hepatitis C infection-brothers in arms. Liver Int 33(8): 1135-1137.
- Wang CS, Wang ST, Yao WJ, Chang TT, Chou P (2007) Hepatitis C virus infection and the development of type 2 diabetes in a communitybased longitudinal study. Am J Epidemiol 166(2): 196-203.
- Chiang CH, Huang KC (2014) Association between metabolic factors and chronic hepatitis B virus infection. World J Gastroenterol 20(23): 7213-7216.
- Chiang CH, Yang HI, Jen CL, Lu SN, Wang LY, et al. (2013) Association between obesity, hypertriglyceridemia and low hepatitis B viral load. Int J Obes 37(3): 410-415.
- Liu J, Yang HI, Lee MH, Lu SN, Jen CL, et al. (2010) Incidence and determinants of spontaneous hepatitis B surface antigen seroclearance: a community-based follow-up study. Gastroenterology 139(2): 474-482.
- Jinjuvadia R, Liangpunsakul S (2014) Association between metabolic syndrome and its individual components with viral hepatitis B. Am J Med Sci 347(1): 23-27.
- Liu Z, Que S, Ning H, Wang L, Peng T (2013) Elevated alanine aminotransferase is strongly associated with incident metabolic syndrome: a meta-analysis of prospective studies. PloS One 8(12): e80596.
- Kunutsor SK, Seddoh D (2014) Alanine aminotransferase and risk of the metabolic syndrome: a linear dose–response relationship. PloS One 9(4): e96068.
- Lee IC, Huang YH, Chan CC, Huo TI, Chu CJ, et al. (2011) Impact of body mass index and viral load on liver histology in hepatitis B e antigennegative chronic hepatitis B. Clin Nutr 30(5): 647-652.
- Wong GL, Wong VW, Choi PC, Chan AW, Chim AM, et al. (2009) Metabolic syndrome increases the risk of liver cirrhosis in chronic hepatitis B. Gut 58(1): 111-117.
- Zhao J, Zhao Y, Wang H, Gu X, Ji J, et al. (2011) Association between metabolic abnormalities and HBV related hepatocelluar carcinoma in Chinese: a cross-sectional study. Nutr J 10: 49.






























