How Misconception of Insulin Therapy Affects Type 2 Diabetes Mellitus Patients' Acceptance on Daily Injection
FU Sau-Nga1* and CHENUG Siu-Keung #2
1Department of Family Medicine & Primary Health Care, Kowloon West Cluster, Hong Kong
2Department of Sociology, Hong Kong Shue Yan University, Hong Kong
These authors contributed equally to this work.
Submission: June 2, 2017; Published: June 15, 2017
*Corresponding author: FU Sau-Nga, Department of Family Medicine & Primary Health Care, Kowloon West Cluster, Hong Kong S.A.R, Email: fsn299@ha.org.hk
How to cite this article: FU Sau-Nga , Siu-Keung C.How Misconception of Insulin Therapy Affects Type 2 Diabetes Mellitus Patients' Acceptance on Daily Injection Curre Res Diabetes & Obes J. 2017; 2(4): 555591. DOI:10.19080/CRDOJ.2017.02.555591
Abstract
Objectives: To find out the development of misconception that leads to Psychological Insulin Resistance in type 2 diabetes mellitus patients.
Methods: 24 focus group interviewsof124insulin naive Chinese patients in 11 primary care clinics. Thematic analysis of the interview transcript was based on patient's expectation of insulin injection in their physical, psychological and social view, to identify the origin of negative attitudes.
Results: Three main sources of misconception are: 1) lacking adequate knowledge, 2) conflicting medical advice, and 3) hearsay from community. Most participants never saw the insulin pen. Patients deferred insulin commencement because they could choose among different clinicians' medical advice. Patients commonly keep peace of mind rather than trying daily injection. They took daily injection as a stigma and ignored the possible DM complications.
Conclusion: Different parties contributed to the development of misconception on insulin therapy. Clinicians should identify and control patients' possible misconceptions.
Keywords: Qualitative research; Treatment refusal; Insulin; Diabetes mellitus type 2; Therapeutic misconception; Hyperglycemia
Introduction
Type 2 diabetes mellitus (T2DM) is increasingly prevalent worldwide. In order to reduce complications, insulin replacement therapy is frequently required because of the progressive nature of T2DM [1]. However, patient refusal of insulin is often found [2] as a result of psychological insulin resistance (PIR), which means a strong negative attitude against insulin therapy [3]. When comparing to the western countries (28% [4]), the prevalence of PIR has been particularly high in Asia (70.6% [5]). PIR involves such a wide range of adverse emotions and practical concerns as questioning the necessity to intensifying medication by insulin, pain, phobia, failure, fear of side effects, operation of insulin pen, economic cost for insulin therapy, language barrier, inadequate knowledge, poor social support, perceived damages on personal image, social life and perceived clinicians' negative attitude towards insulin [4]. In line with the higher PIR in some ethnic groups, it was well-documented that female [5], people with lower income, lower educational level [6], older age group [7], lower glycoslated haemoglobin (HbA1c) level [8], being insulin naive [9] were more unwilling to commence insulin.
Clinicians have tackled PIR as a complex and multifactorial phenomenon by patient-centered approach and through the recommended clinical practices. Most countries including Hong Kong have at the same time adopted newer insulin delivery devices, commonly insulin pen, with shorter and thinner needle that enables injection ease and reduces pain. It is therefore pressing to examine why PIR still commonly circulates among T2DM patients, especially those relatively older, with lower income and lower educational level. This study adopts a qualitative research approach to take a close scrutiny of how patients acquired different knowledge about insulin therapy, and why negative perceptions and emotions are resulted from this knowledge [10]. The findings from this study advance insights for formulating proactive strategies that may possibly enhance the acceptance rate of insulin injection.
Methods
Setting
The study sites were eleven government-funded primary care clinics, where provide health care for more than 25,000 people with T2DM in urban Hong Kong annually. The majority of the visiting patients are older Chinese, relatively less educated, and from the lower social economic class [11]. The consultation fee for each visit is USD6. All prescriptions and investigations are free of charge. Some patients not only consult the clinicians in public setting, but also pay out of their own pockets to attend
Since 2009, some ofthe public primary care clinics have provided insulin commencement for indicated T2DM patients. Free-of-charge injection pen and vials of insulin are provided. Patients only need to pay for the needles of injection pen and the consumables for self-glucose monitoring. However, the successful cases of commencing insulin remain a few. From 2010 to 2012, only less than 4% of patients with T2DM had successfully started on insulin therapy [11].
Participants
This study included insulin naive T2DM patients on maximum tolerated dose of oral antidiabetic agents (OAAs). Their latest haemoglobin A1c level was ≥7.5% (58.5 mmol/mol). Subjects under 18-year-oldor being pregnant were excluded.
Study design
The moderators conducted focus group interview by asking broad views from participants about insulin therapy, before asking focal questions on the development of misconceptions identified. Focus groups were used in order to collect group interaction that encourages participants to explore and clarify attitudes, priorities, group norm and cultural value [10]. All participants offered their written informed consent.
The interviews were conducted in clinic meeting rooms from June 2013 to May 2014. Each focus group interview ran with 3 to 8 participants and lasted for 60 to 90 minutes. One moderator (one of the authors) and one observer (research assistants) were arranged to conduct the focus group interview in Cantonese (one of the Chinese language)according to thestandard interview protocol. (Supplementary Data S1)Investigators avoided interviewing our own patients. The focus groups interviews were terminated when data saturation was reached after 24 focus groups,where adding participants to the existing sampleis unlikely to generate any new ideas [10].
Data analysis
All focus group interviews were recorded as digital audio files and transcribed verbatim into Chinese. The transcript was entered into NVIVO 10® (QSR international) in Chinese for data analysis. A coding tree with definition and operational guidelines for each code was formulated. The authors employed thematic analysisto identify important themes, patterns, features, meanings as well as issues and stories. Finally, SF translated the selected data into English. SC then translated the transcript back into Chinese to assess translational equivalence. Discrepancies between the original Chinese items and back-translated items were reviewed and modified by allauthors.
Results
Characteristics of participants (Table 1)
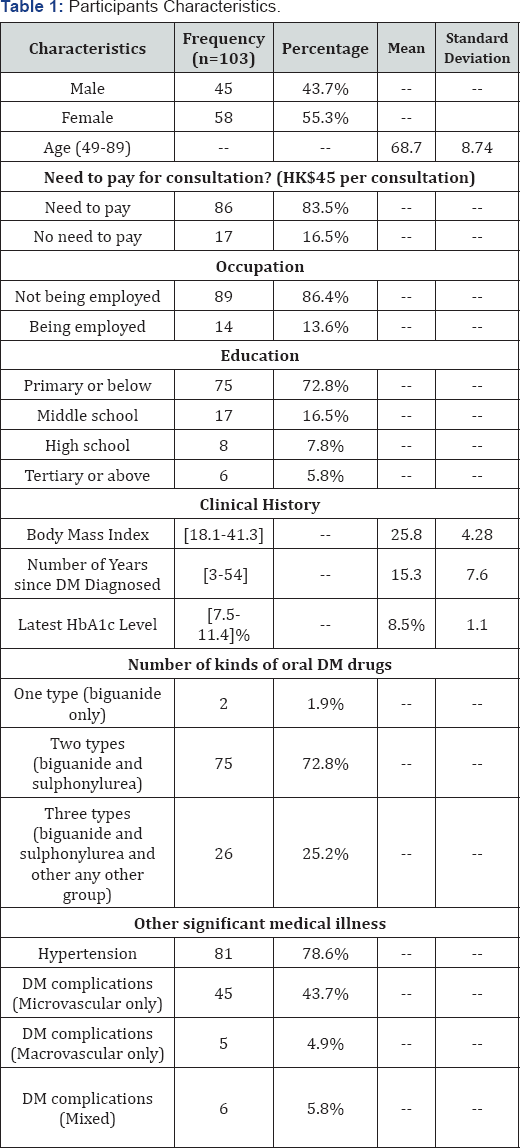
Note: DM: Diabetes Mellitus
* Reasons of �no need to pay�includes being staffs or dependents of government or hospital authority, on social security scheme.
**Not being employed includes being housewife, retired, or unemployed.
***DM complications includes any microvascular or macrovascular complications related to DM
124 participants (mean age= 68.1, M:F ratio = 1.03) were interviewed in 24 focus groups. Most participants (86.3%) were not in full time employment (i.e. housewife, unemployed or retired). Their educational level was relatively low: 67% attained primary school education or below, while only 5% received tertiary education. Their mean latest HbA1c amounted 8.5% (69.4 mmol/mol) and that indicated poor glycaemic control. The majority (98.4%) were prescribed with two or more types of OAAs.
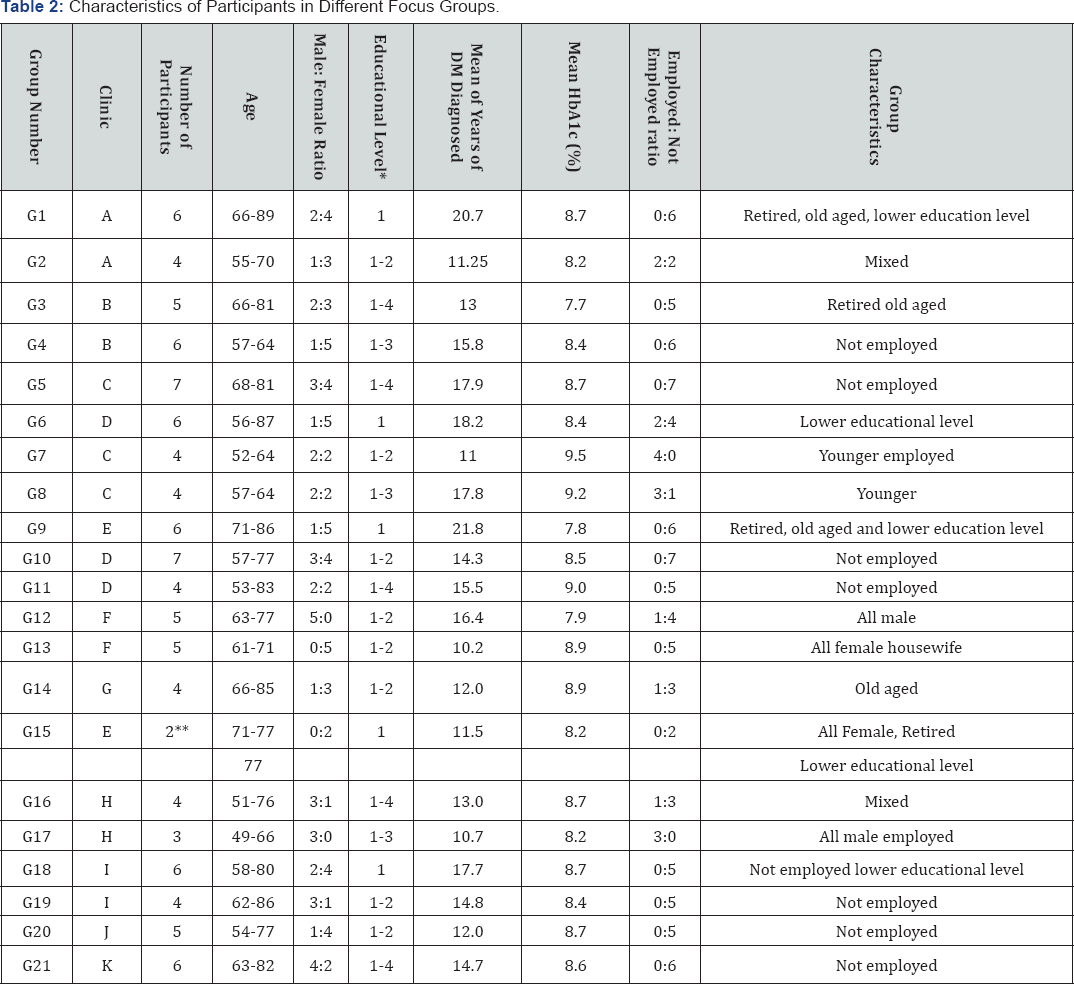
* 1 = primary or below; 2= middle school; 3 = high school; 4 = university or above
Major findings
The characteristic of different groups were shown in Table 2. Misconception in this study refers to any inaccurate idea, belief, myth, presumption and conjecture that deviate from the proven medical knowledge. The three main sources of misconception among the participants are: 1) lacking adequate knowledge 2) conflicting medical advice, and 3) hearsay from community. All participants' names were replaced by assigned number P1, P2, P3, etc. Group names were assigned as G1 (Group 1), G2,etc.
Misconceptions from lacking adequate knowledge (Table 3)
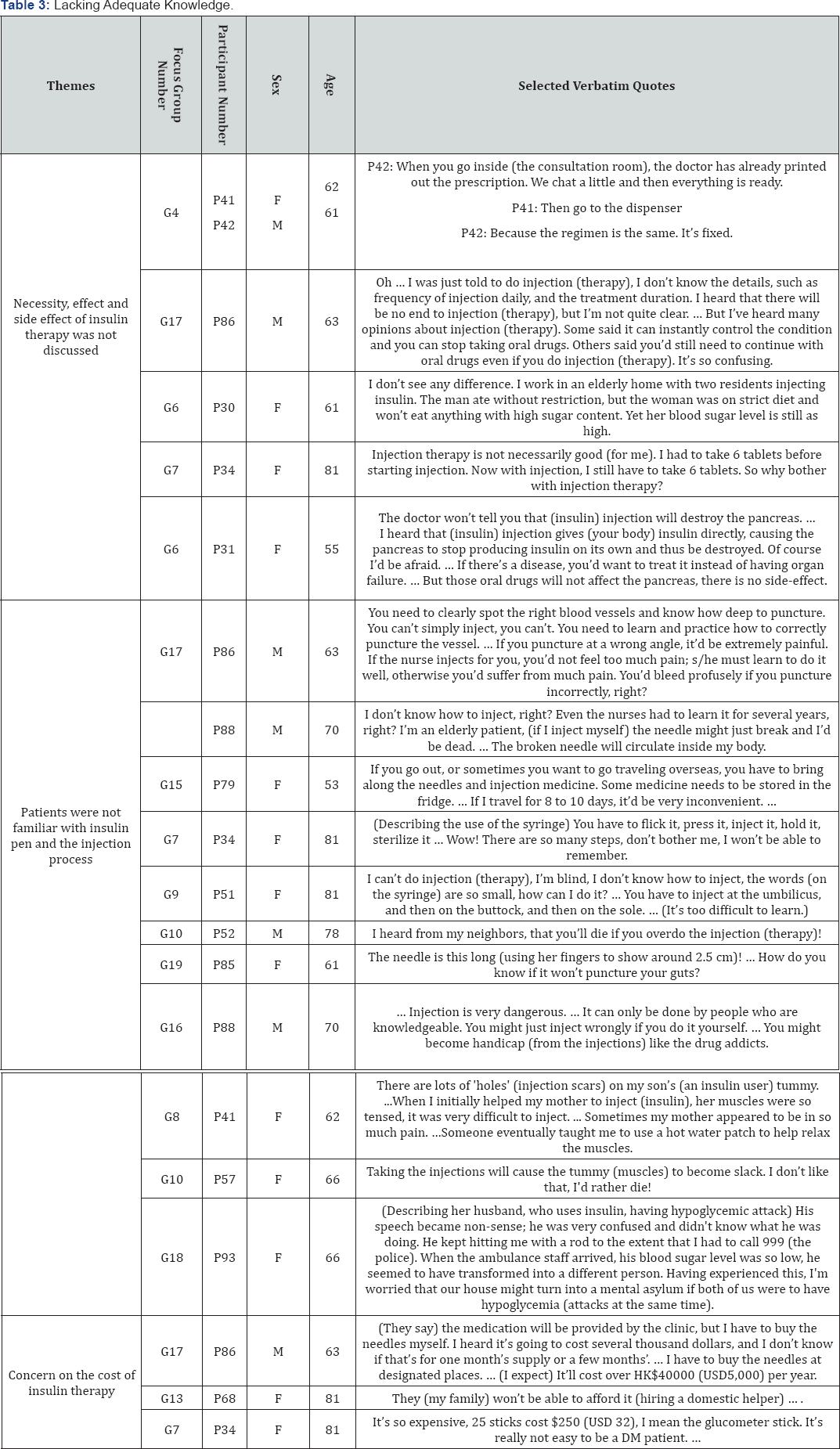
Most participants confirmed heavy psychological burden such as fear, anxious, shock, depressed if they had to commence insulin as most of literature description [4]. Almost all participants did not know or could not give accurate information about insulin pen or injection process.
Necessity, effect and side effect of insulin therapy was not discussed: The discussion between P41 (female, 62-year- old) and P42 (male, 61-year-old) in G4 described an extreme situation of the communication with doctors. Doctors would print out prescription sheet few minutes after consultation started. The patients therefore felt that there was no need to understand insulin therapy. Others participants reported that they would strongly challenge their doctors about the necessity of using insulin therapy. While they recognized that the effect the effectiveness of insulin therapy, particularly what was its of oral drug would be diminishing, they had no idea about difference fromoral drugs in controlling blood sugar.
Likewise, discussion of the side effects of insulin was insufficient. Three participants P31 (female, 55-year-old), P75 (male, 70-year-old) and P88 (male, 73-year-old), from 3 focus groups expressed a shared worry that exogenous insulin would take over remaining pancreatic function and thereby result in organ (pancreas) failure. They suspected direct injection of insulin was overly potent. It would therefore stop pancreatic cells from producing insulin. Other commonly exaggerated insulin side effects include chronic neuralgic pain, profuse bleeding, broken needle, punctured internal organ and consequential scars over body with many holes, and subsequent changes of skin texture and colour. Air bubbles might be injected into body that could result in death. Few participants described their observation of hypoglycemic attack of their relatives. The victim became uncontrollable, insane and unable to handle. Collectively, insulin injection should be avoided at all cost for self-preservation.
Patients were not familiar with insulin pen and the injection process: On the contrary to the existing research finding that most insulin naive DM patients were familiar with insulin pen [12], most participants in this study never sawan insulin pen, much less the injecting process. Consequently,some participants associated injection of insulin with what they saw and felt in their existing experience from their visits to clinics or hospitals. The needle is a much longer and bigger, 20 or 25 -gauges and 25 to 30 mm long. This explained why some participants were prompted into anxiety, fear of pain, phobia of blood, and other physiological responses (e.g., chills, rigor, sweating and palpitation).
Participants generally perceived that the injection of insulin was a complicated process requiring intensive professional knowledge and training. The storage of insulin, the sterilization of instruments, and the steps for injecting were all highly demanding and rigorous. Some participants illustrated the difficulty of injection by their clinicians' multiple attempts before successful venepuncture even though they were professionally trained. Injection of insulin was definitely beyond their literacy, knowledge and ability to handle. Various sites for insulin injection were also aired amongst the participants such as buttock, cubital fossa, umbilicus, anus and even the sole. It bothered much more the older age group because of their illiteracy in English, some also in Chinese, and their decline in eyesight and hand functioning.
Concern on the cost of insulin therapy: Given that most participants came from the lower socio-economic class, they worried much about the cost of insulin therapy. Some participants thought that they had to buy the pen and injection medicine from their pocket. In fact, people on insulin therapy only need to buy the needles of insulin pen that costs HK$200 (USD25) per month. The cost would be reimbursable if they were on the social security scheme. However, nearly none of the participants were clear about the policy. P86 (male, 63-year- old) even estimated the regular expenses for insulin therapy to be up to HK$40,000 (USD 5,000) per year. In line with the drug cost, P68 (female, 81-year-old, lives alone) worried about the additional financial cost for employing a helper to perform injection for her.
Misconceptions from conflicting medical advice (Table 4)
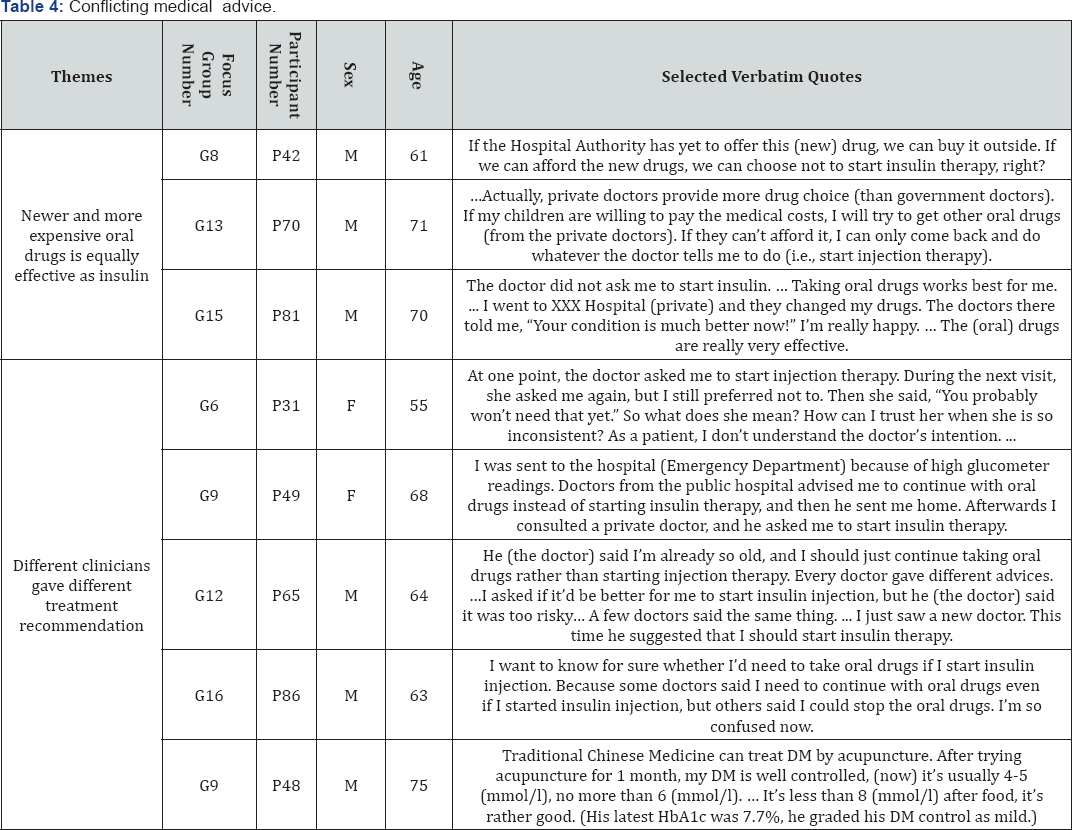
Most participants reported that the continuity of care from public and private doctors for their chronic illnesses was generally poor and the consultation time was short and erratic. If different clinicians gave different opinions, it confused patients of which DM treatment was the best in their condition. As a result, most participants simply chose the advice that supported their intention to delay or avoid insulin therapy.
Newer and more expensive oral drugs is equally effective as insulin: Many participants believed newer generation of OAAs that was ever effective and potent in controlling their blood sugar. The switch to insulin therapy was therefore deferrable if one could afford the expensive newer generation of OAAs. P58 (female, 55-year-old) claimed that she regularly attended both public clinics and a private doctor. While her latest HbA1c had been already up to 10.7% (93.4mmol/mol), she appreciated her private doctor who reassured and prescribed her with "drugs not available in public clinics". She adhered to oral therapy and had no intention to start insulin therapy. Such form of personal presumption gives rise to a myth in real life: the deferability of insulin therapy depended on money.
Different clinicians gave different treatment recommendation: The most common advices from clinicians were "you should be more careful about what you eat", "you should get out and move about" when the participants' blood sugar was high. They have an impression that one's success or failure in maintaining the optimal blood sugar level was solely a matter of diet and lifestyle control. P65 (64-year-old) knew that his blood sugar was always high, which was harmful to his health. He was hesitated whether he should start insulin therapy or not. Some doctors encouraged him, but one of them told him that he was too old, and therefore too risky to start insulin therapy. Overall, our participants commonly perceived clinician's negative attitude towards insulin.
Misconception from Hearsay from Community (Table 5)
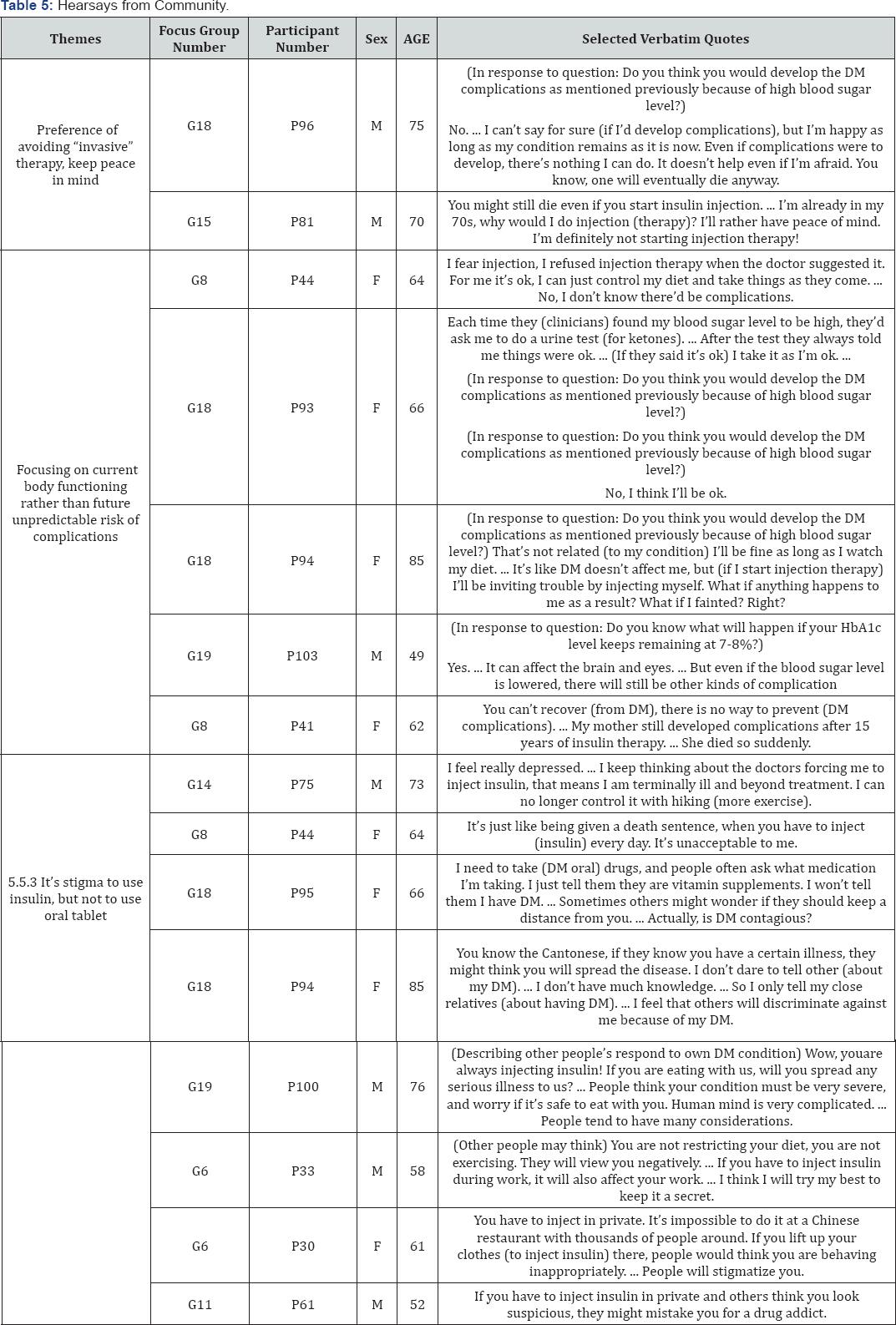
Discussions from focus groups showed that most participants were haunted by the rumours and myths from one's social circle and from the media such as newspaper and online discussions.
Preference of avoiding “invasive” therapy, keep peace in mind: The older participants often expressed their will of keeping peace in their remaining life because their age is approaching the end. Any procedure or treatment that would increase physical suffering should be avoided. They preferred minimal use of drugs in any form. They believe that self-injection could not improve their health but only add suffering. Some of the participants even regarded daily injection as"torturing their remaining life.
Focusing on Current Body Functioningrather than Future Unpredictable Risk of complications: In order to justify their resistance to insulin injection, many older participants cited the hearsay from community that the rise of DM complications was independent of the blood sugar control. Most of them at the same time denied their risk of having complications because they had been well-disciplined in diet control and regular exercising. They did not experience any disabilities or ill-health sensation at the moment. They would emphasize current situation and would not bother "future risks".
It's a stigma to use insulin, but not to use oral tablet: Most participants favoured the oral therapy largely due to their concern on self-dignity and social status. Some of them would like to cover up their condition of having DM. Others did not mind being known the need of regular oral drug-taking always because it was generally acceptable in the community. Even when others saw them taking oral tablets, P95 (female, 66-year- old) said that she could simply liethat she was taking vitamin supplement when she was questioned.
Similar to other research finding, the use of insulin in the Chinese peoples' view represented a person to be really sick [13], P44 (female, 64-year-old)expressed that she would feel like "being given a death sentence" if she had to inject insulin every day. P75 (male, 73-year-old) from G14 claimed that he would be depressed if he had to commence insulin. He used to reduce his blood sugar by increasing the amount of physical activities. Failure to reduce blood sugar by his own effort meant that he lost control of his own body. Other participants also associated insulin users with some negative images such as the drug addict. The association was not only their personal imagination but also a common sense in the community. They thus found it egregiously stigmatizing if others knew that their body functions relied on daily injections. The comment from P100 (male, 76-year-old)was illustrative: "people would look down on you if they know you are using needles. ... They probably think that you have a contagious disease!" This was particularly troubling to participants who were employed, such as P62 (male, 58-year- old). Their main concern was that if their colleagues saw their daily insulin injection, they might be viewed as a "weak," a "handicapped," or a "criminal." Consequently, they might lose their job.
Discussion and Conclusion
Discussion
This is the first study in Hong Kong that adopts a qualitative approach to investigate insulin naiveT2DM patients' misconception on insulin therapy. The participants' socioeconomic background were characterised mostly by not being employed,with lower educational level and lower income. They were comparable with patients generally found in government funded primary care clinics in Hong Kong [14]. The analysis confirms with the existing research insights to the prevalence of PIR, particularly the lack of adequate knowledge on necessity [15], expected effect an dungrounded side effect of insulin therapy as profuse bleeding, severe skin reactions, injection process, patients' concern on treatment cost, stigmatization associated, patients' attitude of preference to oral tablet [16], and the concerning quality of health at the moment, but not future risk of complications [17] from most of the participants.
This study advances several new insights into patients' lived experience of how and why they became poorly informed about the treatment options. There were multiple sources from daily knowledge to social network. First of all, the DM patients in this study were not familiar with the insulin pen as the DM patients from other countries [12]. Many patients in Hong Kong primary care setting have never seen the insulin pen, much less understanding of the injection process. Under consultation time constraint, there were few opportunities for discussion about insulin therapy in either causal or structural manner.The result of poor patient-clinician communication was that many patients would favour and accept hear says. Some would even believe that exogenous insulin was toxic to pancreatic cells, and speeded up organ failure.
This study also found that the presence of conflicting medical advice opened the rooms for patients to run upon their preference for treatment. Without a consistent medical advice for the switch to insulin therapy, patients occurred to distort what the clinicians suggested them to do for their health in various manners. For instance, when doctors suggested newer generations of OAAs and insulin as options of managing hyperglycemia, patients might interpret the newer drugs as replacement of insulin therapy. While clinicians advised patients to maintain a proper diet and lifestyle, patients might believe that the blood sugar can be largely controlled by that alone. Clinicians should be alert to such over-interpretations and the like by clarifying the details and giving the sufficient information for patients. Another important finding from this study appears to be the presence of a remarkable difference between the Western and the Chinese DM patients. Namely, the Chinese patients concerns less on fear of weight gain and hypoglycaemia as the Western patients did [18]. In line with their negative evaluation of insulin therapy, the Chinese patients instead concern more on keeping peace in mind. They avoid being stigmatized as a sick person while they consider insulin commencement [19]. They also appealed to hear says from community to justify their indifference to DM complications and resistance to insulin therapy. Clinicians should aware of patients' attitude on stepping up drugs, especially in relatively older patient in order to arrive share understanding of disease management [20].
Conclusion
This qualitative study demonstrates how the prevalence of PIR involves misconceptions on insulin therapy among people with T2DM and in the general public. The three major sources of misconception include the lack of adequate knowledge, conflicting medical advice, and hearsay from community. When T2DM patients failed to rectify them is conceptions, their selfefficacy in starting insulin therapy will be undermined as what the research subjects in this study indicated. The possible improvement of the acceptance rate of insulin therapy from the improvement of insulin delivery devices will be equally upset due to the continuation of a large gap of the T2DM patients from what are the proper medical understanding and doings. Clinicians should be therefore sensitive to the rise of such misconceptionsin part of their actions to ensure the offering of proper insulin therapy forT2DM patients.
Acknowledgement
The study was funded by the Health and Medical Research Fund, Research Fund Secretariat, The Food and Health Bureau, the government of Hong Kong Special Administrative Region (grant number: 11122751, URL: https://rfs2.fhb.gov.hk/app/ fundedsearch/projectdetail.xhtml?id=1386 ).
References
- Inzucchi SE, Bergenstal RM, Buse JB, Diamant M, Ferrannini E, et al. (2015) Management of hyperglycemia in type 2 diabetes, 2015: a patient-centered approach: update to a position statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care 38(1): 140-149.
- Holman RR, Paul SK, Bethel MA, Matthews DR, Neil HA (2008) 10-year follow-up of intensive glucose control in type 2 diabetes. N Engl J Med 359(15): 1577-1589.
- Peyrot M, Rubin RR, Lauritzen T, Skovlund SE, Snoek FJ, et al. (2005) Resistance to insulin therapy among patients and providers: results of the cross-national Diabetes Attitudes, Wishes, and Needs (DAWN) study. Diabetes Care 28(11): 2673-2679.
- Polonsky WH, Fisher L, Guzman S, Villa-Caballero L, Edelman SV (2005) Psychological insulin resistance in patients with type 2 diabetes: the scope of the problem. Diabetes care 28(10): 2543-2545.
- Wong S, Lee J, Ko Y, Chong MF, Lam CK, et al. (2011) Perceptions of insulin therapy amongst Asian patients with diabetes in Singapore. Diabet Med 28(2): 206-211.
- Machinani S, Bazargan-Hejazi S, Hsia SH (2013) Psychological insulin resistance among low-income, U.S. racial minority patients with type 2 diabetes. Prim Care Diabetes 7(1): 51-55.
- Lakkis NA, Maalouf GJ, Mahmassani DM, Hamadeh GN (2013) Insulin therapy attitudes and beliefs of physicians in Middle Eastern Arab countries. Fam Pract 30(5): 560-567.
- Fu SN, Wong CK, Chin WY, Luk W (2016) Association of more negative attitude towards commencing insulin with lower glycosylated hemoglobin (HbA1c) level: a survey on insulin-naive type 2 diabetes mellitus Chinese patients. J Diabetes Metab Disord 15: 3.
- Bahrmann A, Abel A, Zeyfang A, Petrak F, Kubiak T, et al. (2014) Psychological insulin resistance in geriatric patients with diabetes mellitus. Patient Educ Couns 94(3): 417-422.
- Pope C, Ziebland S, Mays N (2000) Qualitative research in health care. Analysing qualitative data. BMJ 320(7227): 114-116.
- Wong CK, Wong WC, Wan YF, Chan AK, Chung KL, et al. (2015) Patient Empowerment Programme in primary care reduced all-cause mortality and cardiovascular diseases in patients with type 2 diabetes mellitus: a population-based propensity-matched cohort study. Diabetes Obes Metab17(2): 128-135.
- Krall J, Gabbay R, Zickmund S, Hamm ME, Williams KR, et al. (2015) Current perspectives on psychological insulin resistance: primary care provider and patient views. Diabetes Technol Ther 17(4): 268-274.
- Ho EY, James J (2006) Cultural barriers to initiating insulin therapy in Chinese people with type 2 diabetes living in Canada. Canadian Journal of Diabetes 30(4): 390-396.
- Hung SL, Fu SN, Lau PS, Wong SY (2015) A qualitative study on why did the poorly-educated Chinese elderly fail to attend nurse-led case manager clinic and how to facilitate their attendance. Int J Equity Health 14:10.
- Phillips A (2007) Experiences of patients with type 2 diabetes starting insulin therapy. Nurs Stand 21(23): 35-41.
- Polonsky WH, Hajos TR, Dain MP, Snoek FJ (2011) Are patients with type 2 diabetes reluctant to start insulin therapy? An examination of the scope and underpinnings of psychological insulin resistance in a large, international population. Curr Med Res Opin 27(6): 1169-1174.
- Grant RW, Pabon-Nau L, Ross KM, Youatt EJ, Pandiscio JC, et al. (2011) Diabetes oral medication initiation and intensification: patient views compared with current treatment guidelines. Diabetes Educ 37(1): 7884.
- Holmes-Truscott E, Blackberry I, O'Neal DN, Furler JS, Speight J (2016) Willingness to initiate insulin among adults with type 2 diabetes in Australian primary care: Results from the Stepping Up Study. Diabetes Res Clin Pract 114: 126-135.
- Rubino A, McQuay LJ, Gough SC, Kvasz M, Tennis P (2007) Delayed initiation of subcutaneous insulin therapy after failure of oral glucose- lowering agents in patients with Type 2 diabetes: a population-based analysis in the UK. Diabet Med 24(12): 1412-1418.
- Wong MC, Sin CKL, Lee JP (2012) The reference framework for diabetes care in primary care settings. Hong Kong Med J 18(3): 238-246.






























