Frequency of Beta Thalassemia and Iron Deficiency Anemia in Moderate Anaemic Pregnant Patients Visiting to Tertiary Care
Bushra Zulfiqar1*, Kausar Jillani1, Farhana Shaikh2 and Muhammad Faisal Fahim3
1Department of Gynecology & Obstetrics, Isra University, Pakistan
2Facu!ty of Gynecology & Obstetrics, AI-Tibri Medical College & Hospital, Pakistan
3Department of Quality Enhancement cell & Research, Isra University, Pakistan
Submission: May 16, 2017; Published: August 10, 2017
*Corresponding author: Bushra Zulfiqar, Department of Gynecology & Obstetrics, Al-Tibri Medical College & Hospital, Isra University, Pakistan; Tel: 0092-333-3549470; Email: drbztehami@gmail.com
How to cite this article: Bushra Z, Kausar J, Farhana S, Muhammad F F. Frequency of Beta Thalassemia and Iron Deficiency Anemia in Moderate Anaemic Pregnant Patients Visiting to Tertiary Care. Biostat Biometrics Open Acc J. 2017: 2(4): 555593. DOI: 10.19080/BBOAJ.2017.02.555593.
Abstract
Objective: To screen out the moderate anemic patients for iron deficiency anemia, β-thalassemia or combined iron deficiency anemia & β-thalassemia.
Study Design: Cross-sectional observational study.
Place and Duration: Obstetrics & Gynaecology OPD Isra University, Al-Tibri Medical College & Hospital Karachi Campus from 1st-June-2016 to 31st-August-2016.
Methodology: Sampling method was non-probability purposive. Pregnant patients of 18-45 years, with any gestational age who came in outpatient department for antenatal checkup having hemoglobin level 7-10 gm/dl were selected for the study. Females who are non-pregnant and pregnant females having mild anemia 10-11 gm/dl were excluded from the study. A written consent was taken. History and relevant clinical examination was performed. On the basis of CBC result if moderate anaemia present Hb% electrophoresis and serum ferrit in was done to screen out the presence of two diseases. SPSS version 20.0 was used for data analysis.
Result: A total of 140 women with moderate anemia in antenatal clinic recruited for testing serum ferritin to label as iron deficiency anemia and Hb% electrophoresis for Beta thalassemia trait. The age of the women included ranges from 18—45 years in which most of the patients 75 (53%) belongs to 18—30 years of age group. From 140 pregnant women with moderate anemia, 70 (50%) were multigravida, 40 (28.5%) were grand multigravida and 30 (21%) were primigravida. From total number of patients 140, 128 (91.4%) patients have only iron deficiency anemia, 4 (2.8%) have only Beta thalassemia and 8 (5.7%) having combined IDA & BTT.
Conclusion: Iron deficiency is the leading factor for anemia found in this study, but thalassemia trait also a significant contributing factor. The recommendation is to give proper treatment for only iron deficiency anemia, only β-thalassemia and co-existent cases.
Keywords: Iron deficiency anemia; β-thalassemia
Introduction
During pregnancy 30-50% of women become anaemic and mostly because of iron deficiency anaemia. The capacity of oxygen carrying of red blood cells decreased to fulfill the body requirements in anaemia which is a pathological condition. The hematological disease in developing countries is Iron Deficiency Anaemia (IDA) affecting 30% of world population [1]. People living in Indian subcontinent, middle east and central Asia are more affected by iron deficiency anemia [2]. 3.5%-10% quoted prevalence of Beta Thalassemia Trait (BTT) in India [3,4].
Iron deficiency anaemia commonly present in Pakistan especially in female and young children, 70-80% and 6% of pregnant population having iron deficiency anaemia and β-Thalassemia Trait (BTT) respectively [5]. There is huge English research data with few Indian reports available about presence of concomitant BTT and iron deficiency. Many studies have shown the occurrence of iron deficiency anemia in patients with beta thalassemia trait [6-8].
There is a large range of IDA in pregnancy from iron deficiency without anemia to apparent anemia [9]. In clinical practice the identification, treatment and possible prevention for iron deficiency anemia with iron supplementation is straight forward while BTT is usually diagnosed only after failure of treatment for IDA during pregnancy or after delivery [10]. Beta Thalassemia is the most common type of hemoglobin opathies transmitted by heredity found in people of Pakistan and so far more than 200 variables have been diagnosed [11]. Beta Thalassemia Trait (BTT) patients are usually asymptomatic and incognizant of their carrier state unless diagnosed by testing. The rationale of this study is that due to lack of awareness and hospital facilities pregnant patients of moderate anaemia are not screened properly, either they are only iron deficiency anemic or β-thalassemia or combined IDA & β-Thalassemia.
Methodology
The study design is cross sectional, observational study and was conducted at Isra University, Al-Tibri Medical College & Hospital Karachi Campus in Gynae & Obs (OPD) from 1st June to 31st Aug 2016. Approval of the study was taken from (IREC) Institute Research Ethical Committee of ATMC & H. The sample size calculated from the software G power version 3.0.10. The required sample size found to be 140 cases through one tailed t-test with alpha error 0.05 and power of test (1-p err prob) was used to be 0.7 and 95% confidence interval. Non-probability purposive sampling method was used for the selection of patients. All pregnant women age 18-45 years and at any gestational age having Hb% level 7-10gm/dl were included in the study. Non pregnant patient and pregnant women with hemoglobin 10-11gm/dl were excluded. All pregnant women who were visiting first time for antenatal visits their complete blood count was performed on hematology analyzer auto machine (Nihon Kohden Mek 6410k). On the basis of result of complete blood count if HB% level falls in between 7-10gm/ dl, the pregnant ladies were enrolled for the study. A written consent was taken and Hb% electrophoresis HPLC Method on ADAMS ARKRAY Analyzer and serum ferritin by Architect 8001 was done to screen out the presence of two diseases. Data was analyzed through the software SPSS-V.20. The entire continuous variable was presented as Mean+SD. The entire categorical variables were shown in frequency and percentages.
Results
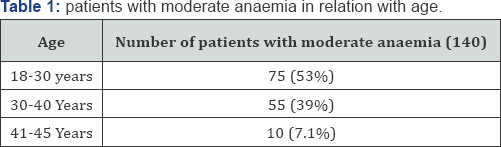
uring the period of 3 months 140 women with moderate anemia in antenatal clinic recruited for testing serum ferritin to label as iron deficiency anemia and Hb% electrophoresis for Beta thalassemia trait. The age of the women included ranges from 18-45 years Table 1 show the presence of moderate anemia in relation with the age of pregnant female in which most of the patients 75 (53%) belongs to 18-30 years of age group.
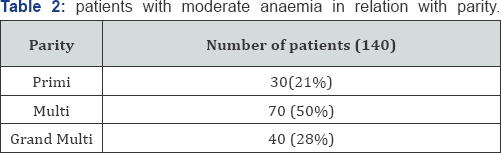
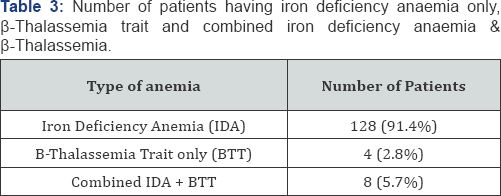
In Table 2 from 140 pregnant women with moderate anemia, 70 (50%) were multigravida, 40 (28.5%) were grand multigravida and 30 (21%) were primigravida. In Table 3 from total number of patients 140, 128 (91.4%) patients have only iron deficiency anemia, 4 (2.8%) have only Beta thalassemia and 8 (5.7%) having combined IDA & BTT.
Discussion
Iron Deficiency Anemia (IDA) and β-Thalassemia (BTT) are the two main types of hypochromic microcytic anemia [12,13]. The most common nutritional disorder worldwide is iron deficiency anemia which contributes approximately one half from all anemic cases. It is due to decreased red blood cell production because of diminished iron stores in the body [14,15]. The thalassemia syndrome is inherited disorder due to globin chain synthesis abnormality [16,17]. The conventional test for IDA is serum ferritin and for thalassemia trait is hemoglobin electrophoresis [18,13].
WHO 2008, Global epidemiology of hematology disorder and derived service indicators stated that β-thalassemia Trait varies from 1.7 to 9% worldwide and 1-7% are β-thalassemia carrier in Pakistan, the same result shows by Guler E et al in their study [19,20]. In present study β-thalassemia trait are 2.8% in our setup in Pakistan. Health Survey for England (HSE) data from 2004 proved that Indian women has highest prevalence of anemia 29% while 16% in Black Caribbean women and 6-7% in Chinese [21]. According to agency for health care research of screening of iron deficiency anemia in childhood and pregnancy, the prevalence data specific to iron deficiency anemia in pregnancy are limited [22]. A study conducted in 2005 by SchollTO reported high tendency of iron deficiency anemia as pregnancy advances in low income group 1.8% in the first trimester 8.2% in second trimester and 27.4% in the third trimester [23]. IDA has wide spread in under developed countries [24].
Hoofar H et al reported that iron level should be checked in β-thalassemia trait patients to avoid harmful effects of iron overload in early stages of the disorder [17]. Keramati MR et al stated that, out of 150 patients of thalassemia minor, only 29 (19.3%) were found to have IDA, while 121 (80.6%) had adequate iron store [25] and in comparison in present study majority of the patient had iron deficiency anemia 128 (91.4%), 4 (28%) patients had BTT while IDA and BTT coexist in 8 (5.7%).
Data related to accurate prevalence of hemoglobin disorder in Pakistan is very limited. Ansari SH et al conducted a study in Karachi, reported 62.2% siblings are β-thalassemia carrier in first family members of the patients [26]. In Bangladesh β-thalassemia minor were 21.3% [27] and in India 57 out of 60 inspected cases on peripheral smears were found to have same type of thalassemia trait [28]. The patients of BTT can also develop ID and they need iron therapy but differentiation in both diseases is necessary for their respective management to avoid serious consequences of iron overload on one side and to exclude severe hemoglobinopathy in developing fetus/newborn.
Conclusion
Iron deficiency is the leading factor for anemia found in this study, but thalassemia trait also a significant contributing factor. The recommendation is to give proper treatment for only IDA, only β-thalassemia and co-existent cases
References
- Rathod DA, Kaur A, Patel V, Patel K, Kabrawala R, et al. (2007) Usefulness of cell counter-based parameters and formulas in detection of beta-thalassemia trait in areas of high prevalence. Am J Clin Pathol 128(4): 585-589.
- D J Weatherall, J B Clegg (2001) The Thalassemia Syndromes. Oxford: Blackwell Scientific Publications.
- Sood SK, Madan N, Colah R, Sharma S, Apte S V, (1993) Collaborative Studies on Thalassemia: Report of ICMR Task Force Study, Indian Council of Medical Research, New Delhi, India.
- Modell B, Bulyzhenkov V (1988) Distribution and control of some genetic disorders. World Health Stat Q 41(3-4): 209-218.
- Ahmed S, Petrou M, Saleem M (1996) Molecular genetics of beta- thalassemia in Pakistan: a basis for prenatal diagnosis. Br J Haematol 94(3): 476-482.
- Saraya AK, Kumar R, Kailash S, Sehgal AK (1984) Iron deficiency in beta-heterozygous thalassaemia. Indian J Med Res 79: 68-75.
- Madan N, Sikka M, Sharma S, Rusia U (1998) Phenotypic expression of hemoglobin A2 in beta-thalassemia trait with iron deficiency. Ann Hematol 77(3): 93-96.
- Mehta BC, Iyer PD, Gandhi SG (1973) Diagnosis of Heterozygous Beta Thalassemia in a Population with High Prevalence of Iron Deficiency. Indian J Med Sci 27(11): 832-835.
- Milman N (2008) Prepartum anemia: prevention and treatment. Ann Hematol 87(12): 949-959.
- Decherney A H, Nathan L. Laufer N, Roman A S. Current Diagnosis & Treatment Obstetrics & Gynaecology. 11th Edition: Page 549.
- Usman M, Moinuddin M, Ghani R, Usman S (2009) Screening of Five Common Beta Thalassemia Mutations in the Pakistani Population: A basis for prenatal diagnosis. Sultan Qaboos Univ Med J 9(3): 305-310.
- Ghaneei M, Movahhedi M, Mirzadeh MJ, Adibi P (1997) Probability for differentiation of blood indices for determination of Iron deficiency in minor Thalassemia based on red cell. Journal of Medical Faculty Guilan University of Medical Sciences 22(6): 1-6.
- Chrobak L (2001) Microcytic and hypochromic anemias. Vnitr Lek 47(3): 166-174.
- World Health Organization (2001) Iron Deficiency Anaemia: Assessment, Prevention, and Control: A guide for programme managers. Geneva, Switzerland: World Health Organization.
- Johnson-Wimbley TD, Graham DY (2011) Diagnosis and management of iron deficiency anemia in the 21st century. Therap Adv Gastroenterol 4(3): 177-184.
- (1998) Recommendation to Prevent and Control Iron Deficiency in the United States, MMWR 47(3): 1-36.
- Hoorfar H, Sadrarhami S, Keshteli AH, Ardestani SK, Ataei M, et al. (2008) Evaluation of iron status by serum ferritin level in Iranian carriers of beta thalassemia minor. Int J Vitam Nutr Res 78(4-5): 204207.
- Joutovsky A, Hadzi-Nezic J, Nardi MA (2004) HPLC retention time as a diagnostic tool for hemoglobin variants and hemoglobinopathies: a study of 60000 samples in a clinical diagnostic laboratory. Clin Chem 50(10): 1736-1747.
- Modell B, Darlison M (2008) Global epidemiology of haemoglobin disorders and derived service indicators. Bull World Health Organ 86(6): 480-487.
- Guler E, Garipardic M, Dalkiran T, Davutoglu M (2010) Premarital screening test results for p thalassemia and sickle cell anemia trait in east Mediterranean region of Turkey. Pediatr Hematol Oncol 27(8): 608-613.
- HSE: Health Survey for England: Health of Minority Ethnic Groups Summary of Findings. In. Center HaSCI, 2006.
- Scholl TO (2005) Iron status during pregnancy: setting the stage for mother and infant. Am J Clin Nutr 81(5): 1218S-1222S.
- WHO (2001) Iron deficiency anaemia: assessment, prevention and control: a guide for programme managers. World Health Organization, Geneva.
- Beard JL (2000) Iron requirements in adolescent females. J Nutr 130(2 suppl): 440S-442S.
- M. Reza KERAMATI, N. Tayyebi MAYBODI (2007) The effect of Iron Deficiency Anemia (IDA) on HbA2 level and comparison of hematologic values between IDA and Thalassemia minor. International Journal of Hematology and oncology 17(3): 151-156.
- Ansari SH, Baig N, Shamsi TS, Saif-ur-Rehman, Ansari ZH, et al. (2012) Screening immediate family members for carrier identification and counseling: a cost-effective and practical approach. J Pak Med Assoc 62(12): 1314-1317.
- Uddin MM, Akteruzzaman S, Rahman T, Hasan AK, Shekhar HU (2012) Pattern of β-thalassemia and Other Haemoglobinopathies: A CrossSectional Study in Bangladesh. ISRN Hematol 2012: 659191.
- Alwar V, Kavadia R, Singh N, Rameshkumar K (2009) Hunt for hidden trait. J Lab Physicians 1(1): 15-18.






























