Historical Overview in Surgical Endodontics
Mohammed Mustafa*
Department of Conservative Dental Sciences, College of Dentistry, Prince Sattam bin Abdul Aziz University, Saudi Arabia
Submission: November 17, 2016; Published: December 05, 2016
*Corresponding author: Mohammed Mustafa, Assistant Professor and Head of Endodontic Division, Department of Conservative Dental Sciences, College of Dentistry, Prince Sattam bin Abdul Aziz University, PO BOX: 153, AlKharj-11942, Kingdom of Saudi Arabia, Tel: +00966-115886240; Email: ma,mustafa@pasu.edu.sa
How to cite this article: Mohammed M. Historical Overview in Surgical Endodontics. Adv Dent & Oral Health. 2016; 3(5): 555603. DOI: 10.19080/ADOH.2016.03.555603
Abstract
The historic pathway to present-day surgical endodontic procedures and their applications has been twisty and unrestrained. These surgical procedures have encountered many tests and trials over the decades. Luckily for present practitioners, prominent members of the oral surgery community, and a few reliable believers in retaining devitalized teeth, continued in their investigation and search for improved procedures that had expected outcomes. Many so-called “innovative” or newer techniques practiced today are nothing but a comeback of surgical concepts that were lost in the annals of time. With the advent of microsurgical endodontics, these procedures are now supported extensively by science of endodontics and by its integration into materials usage, microsurgical instruments, technique applications and outcomes research. However, in many respects, this story is just beginning, as the “origins” of surgical endodontics are discovered. The present article highlights a chronological sequence in the history of surgical endodontics. This historical perspective begins with the ancient civilizations and spotlight predominant dentists, especially endodontists and their contributions in the field of development of surgical endodontics through time.
Keywords: History of Surgical Endodontics, Microsurgery, Microsurgical Instruments, Materials, Techniques
Introduction
According to strictest sense and definition of the word “surgery”, most endodontic treatments fall into the category of a surgical procedure, since it involves removal of tissues, such as vital pulp, necrotic debris or dentin. The term surgery is derived from the Greek word ‘Cheir’ (Hand) ‘Ergon’ (to work), and from the latin word ‘Chirurgia’ “treatment of disease, injury or deformity by manual or instrumental operations, as the removal of diseased parts of tissue by cutting” [1].
The term “Endodontic Surgery” encompasses surgical procedures performed to remove the causative agents of radicular and periradicular disease and to restore these tissues to functional health [2,3].
Currently, endodontic surgery falls into more than one domain and is a predictable and integral part of comprehensive endodontic services [4,5]. The expanded scope of endodontic surgery includes apical curettage [6-8], apicoectomy [9,10], root-end resection [11-12]. Root-end filling [13-17], hemi sections, replantations [18], transplantations, and guided tissue regeneration [19], with more advances on the horizon.
Presently, there are four major areas of surgical endodontics, namely; surgical drainage, radicular surgery, replacement surgery and implant surgery. These areas of endodontic surgery have certain basic similarities but have considerable differences as well in terms of indications and techniques, which should be well known to the endodontists, as it has been correctly said by Late Dr. Irwing J Naidorf, that “A good surgeon knows how to cut, a better surgeon knows when to cut and the best surgeon knows when not to cut. [20]
Although, over the past few decades, the list of indications for surgery has diminished, there are definite cases in which the tooth cannot be saved without surgery and these constitute the ‘core’ of indications. But, the surgical approach is indicated only when non-surgical retreatment is not possible or will not correct the problem, as, endodontic surgery has often been perceived with skepticism because of high precision requirement, low success rate and management of conscious, nervous patients [2,3].
Hence, the modern day dental surgeon, who performs this surgery must have in-depth knowledge of surgical principles, selection, indications and contraindications of the procedure and recent advances [4,5,21,22].
Historical Perspective
The science of surgical endodontics dates its origin back to 1500 yrs ago, when the first recorded surgical endodontic procedure of incision and drainage of an acute abscess was performed by Aetius, a Greek physician dentist. Since then surgical endodontics has been developed and refined as a result of valuable contributions of many pioneers in dentistry including Abulcasis, Fauchard, Hullihan, Martin, Partisch and Black.
Dr. Louis I. Grossman, dean of endodontics in America, has contributed significantly to the science of endodontics and has divided the 200 yrs between 1776 and 1976 into four periods, and each period consist of fifty years duration. This bicentennial history of surgical endodontics against the background of general dentistry is presented here.
First period: 1776-1826
First book of oral surgery was published in 1776, by Jourdain.
Cauterization of the pulp:Principles of cauterization and use of cautery were proposed and practiced by Robert Woffendale in 1783.
Diagnosis and treatment of abscess:Josiah Flagg of Boston, the first native American to practice dentistry exclusively as a profession, relieved pain of an abscessed tooth by creating an opening in the tooth, leading to pulp cavity.
- John Baker’s handbills of 1776 indicate an early recognition of abscessed teeth.
- In 1801, Richard Cortland described an abscessed tooth as: “Pus being a fluid, and pent up in socket of the lower jaw, must and will make its way out. It cannot ascend to the surface or edge of the gum; it must therefore take another direction; and without early professionally assistance, penetrates the alveoli, gum and integuments of the face, from whence flows a watery ichor that continues until the cause is removed”.
The treatment of an abscessed tooth during this period was done by application of heat in the mouth to bring the abscess to a head so that the pus gets discharged, pressure is relieved and pain stopped.
Transplantation and Replantation of teeth:Joseph Fox, strongly recommended transplantation of single rooted teeth in his book
“The Natural History of the Human Teeth”, published in 1778.
- James Gardelte in 1850, proposed intentional replantation of teeth, for the first time in the history of dentistry.
Second period: 1826-1876
Introduction of Rubber Dam:Rubber dam was introduced by Sanford C. Barnum of New York, in 1864.
Anaesthetics
- - In 1800, Sir Humphry Davy used Nitrous oxide to abolish pain during surgery.
- - In 1846, William T.G. Morton, used sulfuric ether as an anaesthetic.
- - In 1847, James Y. Simpson, a Scott physician announced the discovery of chloroform.
- - First hypodermic injection using a syringe was performed by Dr. Francis Rynd. A syringe without suitable anaesthetic for injection however was useless, hence, in 1844, Carl Koller of Vienna, discovered the anesthetic effect of cocaine.
Management of alveolar abscess
- - Harris in 1839, proposed the use of a ‘lancet or sharp pointed knife to evacuate pus from a tumor of gums.
- - In 1874, Adolph Witzel, described an operation for mummification of pulp.
- - Simon P. Hullihan described an operation of entering the pulp chamber, through the neck of the tooth, for draining a periapical abscess. This procedure was called as “Hullihan’s operation”.
- - In 1850, W.H. Atkinson, suggested the use of sulphuric acid to burnout the fistula.
Third period: 1876-1926
Diagnostic Radiography
- - X-rays were discovered by W.K. Roentgen in 1895 and their use in endodontics was first propounded by Otto Walkhoff, who took radiographs of his own teeth.
- - In 1896, Otto Walkhoff and Fritz Giesel established the first dental roentgenological laboratory in the world.
Focal infection theory
- This theory was promulgated by William Hunter in 1910. It came as ‘black eye blow’ to the science of endodontic surgery as it led to wholesale extraction of pulpally involved teeth, which was encouraged by medical profession as a treatment of variety of illness, but was a setback to endodontics.
Advent of asepsis
- - In 1876, Robert Koch proposed his postulates. Nine years later, Lister, introduced antiseptic surgery by using a weak solution of phenol over wounds.
- - The concepts of asepsis were introduced in 1890s.
Local Anesthetics
- - William S. Halsted of New York gave the first mandibular block injection with a cocaine solution.
- - Use of procaine as a local anesthetic was first described in 1906.
- - By the mid 1920s, intra-pulpal anesthesia was being commonly used to induce anesthesia of the exposed pulp, using a cook syringe.
Root-end resection
- - Claude Martin was the father and the inventor of root end resection in 1881. He described the use of this technique to manage teeth with draining sinus tracts.
- - Root end resection was recommended in 1884, when Farrar managed the alveolar abscesses by passing a drill through gums and bone and reaching the root ends, which were then resected accordingly.
- - G.V. Black recommended the amputation of the apex of the root of any teeth in the case of long neglected abscesses in 1886.
- - Actual root end resection is often identified with pre Columbian dentistry practiced in Ecuador by Saville, who discovered a skull with a tooth which was implanted and gave every indication of resection of the apical portion of the root.
- - In the middle of 18th century the root end fillings placed after resection were usually wax, lead or gold.
- - A report on root end resection with immediate root canal fill and management of the apical filling was provided by Brophy in 1880.
- - Later in 1892, Ottolengui presented a succinct technique for immediate filling of root canal followed by resection of root apex.
- - Between 1893 to 1900 in Germany, Carl Partisch proposed “Wurzelspitzenresection” i.e. root end resection under “Chloroformnarkose” i.e. chloroform. He used a vertical incision with iodoform packing technique for the procedure.
Root resection
- - Complete root removal or root resection was first performed by Magitot in 1867, in 1867.
- - Later in 1893 White and Younger recognized the need to remove roots in their entirety that were plagued with “pyorrhea alveolaris”.
- - In 1908, Beal contributed towards development of endodontic surgery in France by publishing several articles and techniques on “root apex resection”.
- - In 1915, Neumann focused on lower molar surgery.
- - Otto Hofer, in 1935 provided a thorough review of surgical flap designs for purpose of endodontic surgery and Partisch I proposed soft tissue management and techniques for cyst management.
- - First indication for the use of amalgam as root-end filling material was provided by Ross in this era, when he described the Castenfeldt technique for management of exposed dentin.
- - This period was marked by the renaissance of endodontic treatment due to developments and improvement in radiographs, anesthetics, new agents, armamentarium, procedures and research.
- - During this era, attention on surgical armamentarium was at its peak, with introduction of Killian headband, which was used for root end resection, coupled with surgical shield, suggested by Witzel in conjunction with the head band.
- - Berger, Ruggier, Moorhead, Kay and Posner advocated semilunar flaps as modus operandi, with triangular flaps beginning to appear.
- - Also the use of mallet and chisel for root end resection was replaced by the use of burs.
- - In 1924, Blayney and Wach published an article on a study that they conducted to prove that new cementum deposition and periodontal healing were possible on the surface of resected dentin.
- - In 1935, Dr. Fernando Garcia, for the first time proposed the use of zinc oxide eugenol as root end filling material.
- - Between 1941 and 1950, Cyrus Jones from New York recommended one visit root canal fill followed by surgical curettage. He also used chloroform at the apex to soften and dissolve the excess gutta-percha making a perfect joint.
- - Also, during this period more attention was focused on surgical curettage and total eradication of the soft tissue surrounding the root.
- - In 1959, Omnell published case report identifying the presence of an electrolytic precipitate of zinc carbonate adjacent to an amalgam root fill. It was considered inflammatory due to resorption of adjacent bone.
- - Sommer and Eklof advocated the use of reverse silver cone placement if access to the root canal could not be obtained through the canal.
- - Later, in 1958 Messing introduced Messing-gun, which is routinely used for placement of amalgam at the root end.
- - In 1943, American Association of Endodontists was formed. The year 1950 saw the development of microsurgery and Digital Optical Microscopes were invented in 1960s.
- - A more conservative attitude with regard to apical surgery developed in the late 1960s when Bhaskar called attention to the fact that periapical cysts are present in more than 40% of cases, a much higher incidence, than previously reported.
- - During the 1970s evolution of surgical endodontics must be credited to the European professionals, who detailed surgical flap designs and management of the resected root ends.
- - In the latter half of the twentieth century, reason and rationale were brought to surgical endodontics with the extensive treatise on surgical endodontics by Jorgen Rud, Jens Andreasen and JE Moller-Jensen. Their studies fostered the use of alternative root end filling materials that favored tissue regeneration.
- - Later mineral trioxide aggregate (MTA) was discovered and brought into use by Mahmoud Torabinejad in 1993 in California.
- Incision and drainage.
- Cortical trephination (fistulative surgery).
- Curettage.
- Biopsy.
- Root end resection.
- Root end preparation and filling.
- Corrective surgery
- Perforation repair. Mechanical (iatrogenic). Resorptive (external and internal).
- Root resection.
- Hemisection.
- Endodontic implants.
- Root form osseous - integrated implants.
- Class A - It represents the absence of a peri-apical lesion but unresolved symptoms after non surgical approaches have
- been exhausted. The symptoms are the only reason for the surgery.
- Class B - Represents the presence of a small peri-apical lesion but no periodontal pockets.
- Class C - Represents the presence of a large peri-apical lesion progressing coronally, but without periodontal pockets.
- Class D - Represents a clinical picture similar to Class C, but with a periodontal pocket.
- Class E - Classifies a peri-apical lesion with an endodontic and periodontal communication, but no root fracture.
- Class F - Represents a tooth with an apical lesion and complete denudement of the buccal plate (Figure 1).
- Curettage, apicoectomy and retrograde filling.
- Surgery for root fractures.
- Incision for drainage.
- Apical surgery.
- Corrective surgery.
- Root amputation, hemisection and bi-cuspidization.
- Apicoectomy and retrograde filling.
- Correction of procedural errors.
- Management of root fractures.
- Intentional extrusion.
- Replantation.
- Transplantation.
- Hemisection.
- Root amputation.
- Elimination of toxins
- Alleviation of pain
- Obviously inadequate filling
- Apparently adequate filling
- Instrument fragmentation
- Non-negotiable ledging
- Over-instrumentation and apical fracture
- Symptomatic overfilling
- Instrument fragmentation
- Non-negotiable ledging
- Over-instrumentation and apical fracture
- Symptomatic overfilling
- Inaccessible branching canals with multiple portals of exit
- Severely curved roots
- Supernumerary roots
- Dens in dente
- Intentional
- Post -traumatic
- Endodontic
- Endosseous
- Poor systemic health
- Emotional distress
- Limitations in surgical skills and experience of the operator.
- Localized acute inflammation: emergency procedures such as incision and drainage or trephination may be indicated whereas elective peri - apical surgery should be avoided.
- Anatomic considerations: Procedures that penetrate the mandibular canal, maxillary sinus, mental foramen, floor of the nares or that sever the greater palatine blood vessels should be avoided where ever possible.
- Inaccessible surgical sites, especially in posterior teeth with dense layers of bone and teeth with poor prognosis such as short rooted teeth, teeth with advanced periodontitis and vertically fractured teeth should not be considered for surgery.
- Indiscriminate surgery - Endodontic surgery should not be a compensatory treatment approach.
- Michael Soutis (2006) Ancient Greek terminology in pediatric surgery: about the word meaning. J Pediatr Surg 41(7): 1302-1308.
- Johnson BR, Witherspoon DE (2006) Pathways of the pulp (9th edn), Mosby Publications, Periradicular surgery, USA, pp. 724-785.
- Kvist T, Reit C (2000) Postoperative discomfort associated with surgical and non-surgical endodontic retreatment. Endod Dent Traumatol 16(2): 71-74.
- Velvart P (2002) Papilla base incision: a new approach to recessionfree healing of the interdental papilla after endodontic surgery. Int Endod J 35(5): 453-460.
- Velvart P, Ebner-Zimmermann U, Ebner JP (2003) “Comparison of papilla healing following sulcular full-thickness flap and papilla base flap in endodontic surgery”. Int Endod J 36(10): 653-659.
- Sauveur GF, Roth M, Sobel, Boucher Y (1999) The control of haemorrhage at the operative site during periradicular surgery. Int Endod J 32(3): 225-228.
- Zuolo ML, Ferreira MOF, Gutmann JL (2000) Prognosis in periradicular surgery: a clinical prospective study. Int Endod J 33(2): 91-98.
- Rubinstein R, Kim S (2002) Long-term follow-up of cases considered healed one year after apical microsurgery, J Endod 28(5): 378-383.
- Arx, Montagne, Zwinggi, Lussi A (2003) Diagnostic accuracy of endoscopy in periradicular surgery -a comparative study with SEM. Int Endod J 36(10): 691-699.
- AErol S Apaydin, Mahmoud Torabinejad (2003) The effect of calcium sulfate on hard-tissue healing after periradicular surgery. J Endodontics 30(1): 17-20.
- Gutmann JL, Pitt Ford TR (1993) Management of the resected root-end: a clinical review. Int Endod J 26(5): 273-283.
- Mohamed I Fayad, Robert Hawkinson, Jon Daniel, Jianjun Hao (2004) The effect of CO2 laser irradiation on PDL cell attachment to resected root surfaces. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 97(4): 518-523.
- Mahmoud Torabinejad, Hong CU, McDonald F, Pitt Ford TR (1995) Physical and chemical properties of a new root-end filling material. J Endod 21(7): 349-353.
- Ernest S Rech, Edward C Combe (1997) “A new single step technique for apical retrofilling that significantly reduces microleakage”. J Endod 23(3): 149-151.
- Mahmoud Torabinejad, Noah Chivian (1999) Clinical applications of mineral trioxide aggregate. J Endod 25(3): 197-205.
- Hanan Balto, Saad Al-Nazhan (2003) Attachment of human periodontal ligament fibroblasts to 3 different root-end filling materials: Scanning electron microscopic observation. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 95: 222-227.
- Erol S Apaydin, Shahrokh Snabahang, Mahmoud Torabinejad (2004) Hard-tissue healing after application of fresh or set MTA as root-endfilling material. J Endod 30(1): 21-24.
- Mikako Hayashi, Yoshifumi Kinomoto, Fumio Takeshige, Shigeyuki Ebisum (2004) Prognosis of intentional replantation of vertically fractured roots reconstructed with dentin-bonded resin. J Endod 30(3): 145-148.
- Thomas V Arx, David L Cochran (2001)Rationale for the application of the GTR principle using a barrier member in Endodontic Surgery: A proposal of classification and literature review. Int J Perio Resto Dent 21(2): 127-139.
- Serge Dibart (2007) Practical Advanced Periodontal Surgery. Blackwell publishing company, USA, pp. 3-95.
- Louis I Grossman, Seymour Oliet, Carlos E Delrio (1988) Endodontic Practice. (11th edn), Lea & Febiger, Philadelphia, USA, pp. 150.
- Bellizzi R, Loushine R (2008) A Clinical Atlas of Endodontic Surgery, Quintessence Publishing Co, London.
- In Ingle JI & Bakland LK (2008) Endodontics (6th edn).
- Stephen Cohen, Richard C Burns (2015), Pathways of pulp (11th edn).
- Franklin S Weine (1996) Endodontic therapy (5th edn).
- Torabinejad M, Walton RE, Fouad AF (2014) Principles and practice of endodontics (5th edn).
- Kim S Color Atlas of Microsurgery in Endodontics. WB Saunders Company, USA.
- Luebke RG, Glick DH, Ingle JI (1964) Indications and contraindications for endodontic surgery. Oral Surg Oral Med Oral Pathol 18: 97-113.
- Pecora Gabriele, Andrean S (1993) Use of dental operating microscope in endodontic surgery. Oral Surg Oral Med Oral Pathol 75(6): 751-758
- Carr GB (1992) Microscope in endodontics. Journal of Calif Dent Assoc 11: 55-61.
- Samuel Seltzer (1988) Endodontology Biological considerations in Endodontic procedures, (2nd edn), Lea & Febiger, Philadelphia, USA, p. 17.
- Stephen Cohen, Richard C Burns (1994) Pathways of the pulp, (6th edn), CV Mosby co, St Louis, USA, pp. 539-543.
- Stock, Christopher JR, Gulabivala, Kishor, Walker, Richard T, Goodman Jane R (1995) Color Atlas and Text of Endodontics, (2nd edn), Mosby- Wolfe, London.
- Gutmann JL, Harrison JW Surgical Endodontics. All India Publication.
- Mu Mu Min, Cecil E Brown, Joseph J Legan, Kafrawy AH (1997) In vitro evaluation of effects of ultrasonic root-end preparation on resected root surfaces. J Endod 23(10): 624-628.
- Massimo Gagliani, Silvio Taschieri, Raffaella Molinari (1998) Ultrasonic root-end preparation: Influence of cutting angle on the apical seal. J Endod 24(11): 726-730.
- Leslie A Morgan, J Gordon Marshall (1999) A scanning electron microscopic study of in vivo ultrasonic root-end preparations. J Endod 25(8): 567-570.
- Chong (2016) Harty’s Endodontics in Clinical Practice, (7th edn), Churchill Livingstone, London, pp. 352.
- D ental Clinics of North America Microscopes in Endodontics (1997) Saunders Publication, USA, 41: 3.
- Kim S, Kratchman S (2006) Modern endodontic surgery concepts and practice: a review. J Endod 32(7): 601-623.
Sophistication of surgical endodontics
Fourth Period: 1926-1976
Classification of Endodontic Surgery
various classification has been given by many distinguished contributors in the field of endodontics which includes;
A.According to Ingle and Bakland [23]
1.Surgical drainage
2.Periradicular surgery
3.Replacement surgery (extraction/replantation)
4.Implant surgery(extraction/replantation)
B.According to Cohen and Burns [24]
Cohen and Burns classified surgical endodontics according to various radiographic and clinical presentations.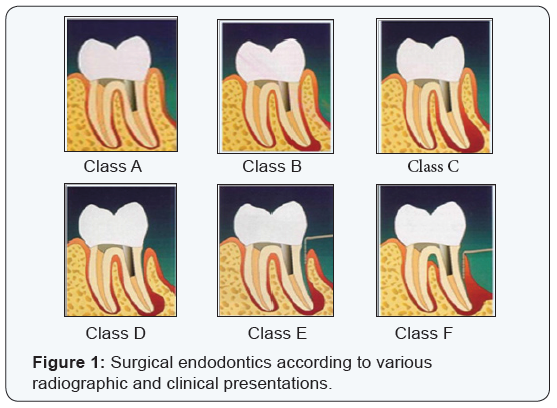
C. According to Franklin S. Weine [25]
1.Peri-apical surgery
2.Amputational surgery
D.According to Richard E. Walton and Torabinejad [26]
E.According to Kim [27]
1.Apical surgery
2.Peri-radicular surgery
A classic categorization of specific indications and contraindications was developed by Luebke, Glick and Ingle [28] these indications and contraindications should be applied as judgment and circumstances dictate.
I.Indications of Endodontic Surgery
1.Surgical drainage
A.Necessity for drainage
2.Apical surgery
A.Irretrievable root canal fillings
B.Calcified canals
C.Procedural errors
D.Presence of Dowels
E.Anatomic variations
D.Presence of Dowels
E.Anatomic variations
F.Apical cysts interfering with normal healing
G.Biopsy
3.Corrective surgery
A.Root anomalies
B.Perforating carious and resorptive defects
C.Periodontal - endodontic defects
4.Replacement surgery
A.Replant surgery
B.Implant surgery
II.Contra - Indications of Endodontic Surgery
A.General considerations
B. Local considerations
Now, coupled with the use of microscope that has provided the dental professionals with a new visionary pathway for successful treatment in the new millennium, all phases of endodontic microsurgery can be managed with greater predictability.
Prof. Gabriele Pecora stated that “Light and magnification have given a better standard of quality in dentistry with the invent of Surgical Operating Microscope” [29] (Figure 2).

With the advent of Surgical Operating Microscope which not only provides magnification, illumination, but also helps in documentation coupled with microsurgical instruments along with ultrasonic root-end preparations and sealing with new retrograde materials, the success of surgical endodontic treatment will provide the answer to solving myriad problems that were once considered hopeless [30-35] (Figure 3).
Other important factors that have enhanced the success and increased the application of surgery are research and education. Advanced endodontic programs have increasingly emphasized surgical training in response to the need for this treatment approach [36-38].
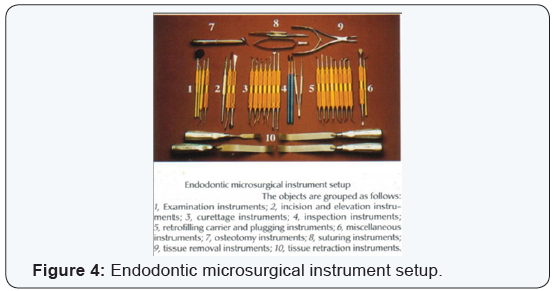
There has been a sea of changes in approach towards microsurgical endodontics in the past decade or two, due to an avalanche of new techniques and materials which have given clinician a wide range of choices in this conservative approach and allow us to go ahead with confidence, in treatment, management and conservation of each tooth that could not be otherwise saved [39,40] (Figure 4).
An exhaustive effort towards conservation of maximum possible tooth and supporting structures has been justified by the fact that “a mouth without teeth is like a mill without its stone, and you must value a tooth more than a diamond”.






























