Physiotherapy Intervention in Delayed Motor Evolution in a Clinical Case of Neuromuscular Disease
Gustavo Desouzart1,2*
1RECI-Piaget Institute of Viseu, Portugal
2CIEQV-Quality of life research centre, Portugal
Submission: August 31, 2018; Published: September 20, 2018
*Corresponding author: Gustavo Desouzart, RECI-Piaget Institute of Viseu,CIEQV-Quality of life research centre, Portugal, Email: gustavodesouzart@gmail.com
How to cite this article: Gustavo Desouzart. Physiotherapy Intervention in Delayed Motor Evolution in a Clinical Case of Neuromuscular Disease. 002 Theranostics Brain Spine Neuro Disord. 2018; 4(1): 555626. DOI: 10.19080/TBSND.2018.04.555626
Abstract
Intracranial hemorrhage is a rare but significant complication of Herpes Simplex Encephalitis infection that should be thought of early. Although acyclovir is the definitive treatment of this encephalitis, there is no guarantee that it will prevent intracranial hemorrhage.
Introduction
Herpes Simplex Virus (HSV) encephalitis is a fatal sporadic encephalitis with mortality rate of 70% if untreated. Although petechial cortical hemorrhage is common in this entity, frank intracranial hemorrhage is extremely rare. As of 2011, only 11 cases were reported in the literature. Here we discuss a case of HSV encephalitis complicated with intracranial hemorrhage [1].
Case Report
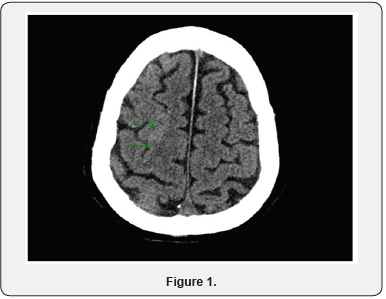
70 years old male who was recently in Philippines and came back 2 days prior to admission, was seen in the emergency department for fever and global headache. He had these symptoms for about 2-3 days. He denied vomiting, diarrhea and any sick contacts. His past medical history was significant for coronary artery disease with remote history of quadruple bypass and also diabetes mellitus type 2. He denied any history of smoking or alcohol abuse. On arrival he was febrile at 100.8 degree Fahrenheit. Physical exam was notable for mild neck tenderness and rigidity. He was oriented to person and place but not time. Computed tomography (CT) of brain showed no soft tissue mass, acute infarct or hemorrhage but it was noted that patient has asymmetry of right superior frontal sulcus that could be secondary to gyral swelling (Figure1). Magnetic resonance imaging could not be done since the patient had sternal wires. Lumbar puncture was done and cultures of cerebrospinal fluid (CSF) later came back positive for HSV1.
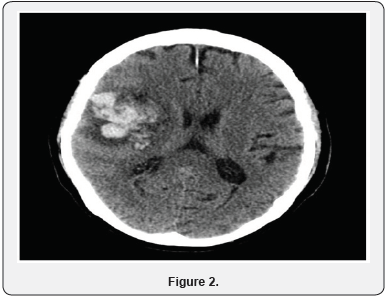
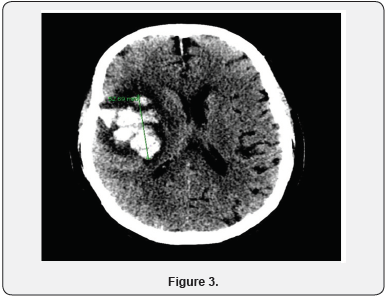
Initially patient was suspected to have meningitis and started on vancomycin, ampicillin, ceftriaxone and acyclovir. The antibiotics were stopped after HSV was confirmed and antiviral continued. On day 6 of hospitalization patient was noted to have decreased responsiveness. Patient had a Stat CT of the head which showed 5cm right temporal lobe hematoma with 3.5 mm midline shift to the Left (Figure 2). Neurosurgery was notified but it was determined that patient has a poor prognosis and is not a candidate for surgery. He was also transferred to intensive care due to respiratory distress and was intubated. The next day repeat CT of head showed increase in size of hematoma to 6 cm (Figure 3). Family decided to make the patient comfort care only and he was transferred to hospice.
Discussion
It is estimated that every year there are 20,000 cases of viral encephalitis which includes 10-20% of HSV encephalitis. As mentioned before, untreated cases of HSV encephalitis has a mortality rate of 70% [2], There are 3 possible pathogenesis for HSV invasion of central nervous system (CNS). First is invasion through trigeminal nerve and olfactory tract, second is after recurrent HSV- 1 infection and the third one is reactivation of HSV in situ within CNS [3]. Often temporal lobe necrosis with subsequent neurologic deficits occur as a complication of HSV infection. In animal studies, it was noted that HSV-1 produces focal lesions in the temporal lobe similar to what is seen in humans [4]. Studies have shown that host susceptibility seems to be affected by the Toll-like receptors (TRL) and defects in the signaling molecules of TLR pathway make the host susceptible to HSV infection [5]. Tissue injury seems to be immune mediated which might explain why HSV infection is more common in immunocompetent individuals. In fact, studies have shown that focal inflammatory lesions are the result of virus specific T cell response.
Correlation between production of nitric oxide and cytokines has also been noted in some animal models. Studies have shown that administration of IL-4 to mice infected with HSV-1 increases the severity of subsequent encephalitis [3,6]. HSV usually present with headache, confusion, fever and seizure. Failure to diagnose, might lead to permanent disability complications or demise. Petechial cortical hemorrhage are common but frank hematoma – as in this case- is extremely rare. There has been cases of HSV encephalitis with initial presentation of intracranial hemorrhage. In a comparison study done by Satoru Takeuchi between the reported cases of HSV encephalitis complicated by hemorrhage, hematoma location was noted to be in medial temporal lobe in 6 patients with exhibition of gyral pattern [1]. In 6 other patients it was noted that hemorrhagic conversion occurred in 5-15 days after initiation of symptoms which may suggest that initiation of treatment does not have any specific effect on the hemorrhagic complication. The mechanism of hemorrhage remains unknown. Fukushima et al. [7] proposed that increased intracranial pressure can lead to transient hypertension and vasculitis that in turn will lead to small vessel rupture and subsequent hematoma. Hematoma formation occurred at later stages in their study [7].
References
- Takeuchi S, Takasato Y (2011) Herpes simplex virus encephalitis complicated by intracerebral hematoma. Neurol India 59(4): 594-596.
- Baldwin KJ, Cummings CL (2018) Herpesvirus Infections of the Nervous System. Continuum (Minneap Minn) 24(5, Neuroinfectious Disease): 1349-1369.
- Mancini M, Vidal SM (2018) Insights into the pathogenesis of herpes simplex encephalitis from mouse models. Mamm Genome 29(7-8): 425-445.
- Mendez AA, Bosco A, Abdel Wahed L, Palmer K, Jones KA, et al. (2018) Fatal Case of Herpes Simplex Encephalitis with Two False-Negative Polymerase Chain Reactions. Case Rep Neurol 10(2): 217-222.
- Scheel M, Finke C (2018) MRI Findings Suggestive of Herpes Simplex Encephalitis in Patients with Anti-NMDA Receptor Encephalitis. AJNR Am J Neuroradiol.
- Fukushima Y, Tsuchimochi H, Hashimoto M, Yubi T, Nakajima Y, et al. (2010) A case of herpetic meningoencephalitis associated with massive intracerebral hemorrhage during acyclovir treatment: a rare complication. No Shinkei Geka 38(2): 171-176.
- Ramirez KA, Choudhri AF, Patel A, Lenny NT, Thompson RE, et al. (2018) Comparing molecular quantification of herpes simplex virus (HSV) in cerebrospinal fluid (CSF) with quantitative structural and functional disease severity in patients with HSV encephalitis (HSVE): Implications for improved therapeutic approaches. J Clin Virol p. 29-37.






























