Modifications to the Mipo Surgical Technique in Diaphysary Fractures of the Tibia
Leonardo Martínez Aparicio1, Lázaro Martin Martínez Estupiñán2, Roberto Morales Piñeiro3, Gerardo Castillo Oliva3, Claribel Plain Pazos4 and Tony Angel Abreu Yera5
1Specialist in Orthopaedics and Traumatology, Instructor Professor, University General Hospital Mártires del 9 de Abril, Cuba
2Doctor in Medical Sciences, II Degree Specialist in Orthopedics and Traumatology, Full Professor, University General Hospital Mártires del 9 de Abril, Cuba
3Specialist in Orthopaedics and Traumatology, Assistant Professor, University General Hospital Milián Castro. Villa Clara, Cuba
4I and II Degree Specialist in Comprehensive General Medicine, Faculty of Medical Sciences of Sagua la Grande, Cuba
5Specialist in Orthopaedics and Traumatology, Assistant Professor, University General Hospital Milián Castro. Villa Clara, Cuba
Submission: March 27, 2024; Published: May 08, 2024
*Corresponding author: Claribel Plain Pazos, Faculty of Medical Sciences of Sagua la Grande, Villa Clara, Cuba
How to cite this article: Leonardo M A, Lázaro Martin M E, Roberto M P, Gerardo Castillo O, Claribel P P, et al. Modifications to the Mipo Surgical Technique in Diaphysary Fractures of the Tibia. Ortho & Rheum Open Access J. 2024; 23(2): 556107. DOI: 10.19080/OROAJ.2024.23.556107
Summary
There are multiple techniques for the treatment of tibia fractures; sometimes these techniques require a group of special accessories and instruments that allow the surgeon to perform the procedure quickly and easily. Generally, these accessories are expensive, and the services do not have them. After calling a group of experts and meeting to make proposals for modifications to the MIPO technique, the ideas are prioritized and six proposals for modifications to the technique are presented. They are presented to the institutional Scientific Council and the Research Ethics Committee and approved to begin implementing it in our patients.
Keywords: Tibial fractures; Minimally invasive osteosynthesis; MIPO; Dynamic compression plates (DCP); Mobilization
Introduction
There are multiple techniques for the treatment of tibia fractures; sometimes these techniques require a group of special accessories and instruments that allow the surgeon to perform the procedure quickly and easily. Generally, these accessories are expensive, and the services do not have them. Fractures of the tibia have an incidence of 16.9/100,000 per year and between four and 23% are open injuries. Depending on the fracture pattern and soft tissue involvement, they can be treated conservatively or surgically; However, there is no consensus for determining the optimal surgical technique. Since the introduction of dynamic compression plates (DCP) for osteosynthesis, their popularity in the invasive treatment of these fractures has increased. In the latest research, study dynamics have been created regarding concepts such as biological osteosynthesis, minimally invasive osteosynthesis, relative stability and absolute stability [1]. It was Christian Krettec and Harald Tscherne who in 1997 introduced the concept of minimally invasive osteosynthesis [2]. The concept of biological osteosynthesis refers to the preservation of bone vascularity during surgical intervention to ensure the vitality of the individual fragments and achieve fracture healing with a minimum of damage to the soft tissues and a relative stability that favours the materials [3]. Conventional osteosynthesis techniques applied for multi fragmentary fractures can lead to a variety of complications: delayed union, infections, implant failure and non-union. This happens because to achieve anatomical reduction, extensive surgical exposure is necessary and, sometimes, the fracture fragments are stripped of the soft tissues that provide vascularity [4,5].
The first attempts in the use of biological osteosynthesis They appear in the 80s of the last century; The development of indirect reduction techniques and the use of new osteosynthesis materials caused a basic change in the treatment of fractures. Every fracture evolves towards consolidation, with pain, inflammation and immobility and reflects what is known as fracture disease, which, if not adequately treated, produces muscle atrophy and generates adhesions that, taken to an extreme, cannot be reversed. and determine sequelae that limit functionality [6]. An adequate quality of life is guaranteed by free and painless movement, this is the philosophy that motivates selecting a fracture fixation technique that allows achieving total mobilization and favours rapid recovery. revascularization of bone and soft tissues. Minimally invasive osteosynthesis is a method in which the percutaneous use of laminae to remotely fixate the fracture site through minimal exposure is an alternative procedure for the treatment of tibia fractures [7]. We intend to present a series of modifications to the MIPO surgical technique.
Method
A prospective longitudinal study was carried out where the mixed research paradigm was assumed, while quantitative and qualitative data were analysed in the same study to respond to the research problem.
Theoretical and empirical scientific research techniques were used. With a multistage study.
a. Stage 1 Explore. Identify and describe the current situation, selection of investigative techniques and the sample for the study.
b. Stage 2 Elaborate, where creation, preparation, design of modifications to the MIPO technique are carried out
c. Stage 3 Validate the results. Where the evaluation by the group of the modifications is defined.
A semi-structured interview is carried out with specialist doctors linked to trauma care
After agreement with each professional, a semi-structured interview was carried out in which the level of information and mastery of theoretical and practical aspects associated with traumatology and osteosynthesis was explored. Semi-structured interview with physicians involved in the care of patients with limb trauma.
General objective: Obtain information about the opinions and assessments of specialist doctors who participate in the process of medical care for patients with trauma of the limbs and spine.
Interviewer-interviewee relationship: Achieve social interaction, through a process of mutual understanding and trust.
Interview situation: Carry out in a climate that respects the natural interaction of people characterized by naturalness and free expression.
Guide or guidelines for the development of the interview:
a. Exploration of the knowledge that specialist doctors have about the process of medical care for patients with trauma of the limbs and spine.
b. Possibilities of proposals for the modification to MIPO osteosynthesis in our context.
c. Search for needs and contributions.
Evaluation of the judgment of specialists on the possibility of modifications to the MIPO technique: With the purpose of knowing the opinion of specialists with experience in the subject, regarding osteosynthesis and modifications to the MIPO technique, a questionnaire was applied to evaluate the judgment of specialists.
Description of the sample: The sample was made up of __23__ specialist medical professionals, selected from intentional non-probabilistic sampling. For its selection, the following inclusion criteria were established:
a. Willingness and interest to collaborate with the research, expressed through informed consent.
b. Theoretical and/or practical knowledge of the topics.
c. Possess more than ten years of professional experience.
Focus group: This technique allowed the generation of ideas through the identification of critical variables of medical care for adult patients with a diagnosis of tibia fracture and the establishment of priorities. An environment was fostered that stimulated interventions to identify the issues. of group consensus. A guide to the topics to be discussed was previously prepared.
Topic guide for Focus Groups
General objective: Explore the criteria of medical specialists, through individual and group reflection, on the variations in the concepts of osteosynthesis in the new century, the insufficiencies that osteosynthesis with the standard open technique of the fracture focus may present, and the proposals for modifications to the surgical technique.
Selection of participants: ______________________
Selection of the moderator and rapporteur: Moderator: ______________.
Rapporteur: ___________________________.
Description of the place where it takes place: ___________________.
Date: ____________. Hour: _____________.
Steps of the focus group technique
i. Explanation of the objectives of the technique and the rules of its development.
ii. Presentation of the questions.
iii. Reflection and individual recording of ideas.
iv. Presentation and debate of all ideas.
v. Assessment of common ideas.
Results
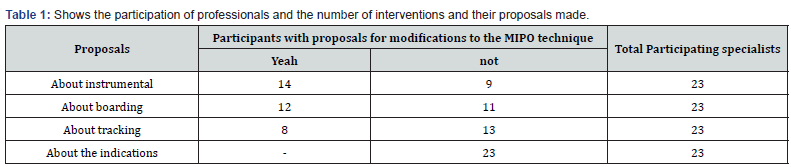
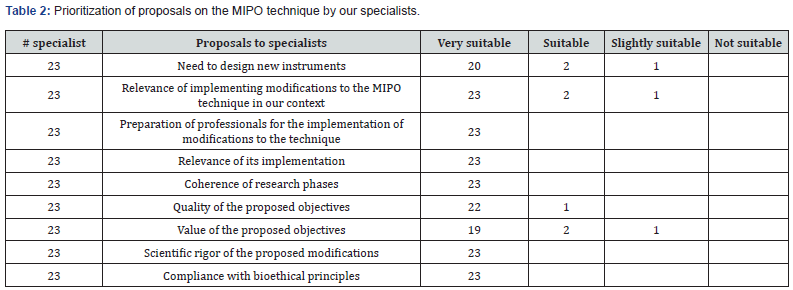
At the end of the systematic review on osteosynthesis and surgical treatment with MIPO for tibial diaphyseal fractures, a group technique was carried out with a group of high-category orthopaedic professionals, whether scientific, teaching and research, all members of the Cuban Society of Orthopaedics and Traumatology, who provided opinions on what modifications to the technique can be made in our current context, with our limitations to offer the population a surgical treatment option that is in accordance with modern principles of osteosynthesis, provides satisfaction and minimizes risks of the conventional open technique (Table 1). Each of the proposals made was addressed individually and prioritized by the group, who evaluated them to ultimately decide which ones could be proposed for implementation in our service Table 2. It can be seen that everyone agrees on the relevance of implementing modifications to the MIPO technique in our context, preparation of professionals for the implementation of the modifications to the technique, the relevance of its implementation, the coherence of the research phases, the rigor scientific of the proposed modifications and compliance with bioethical principles.
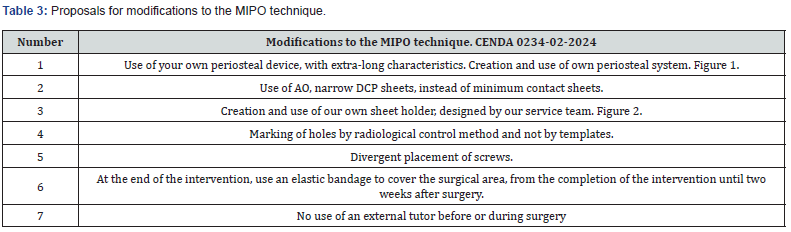

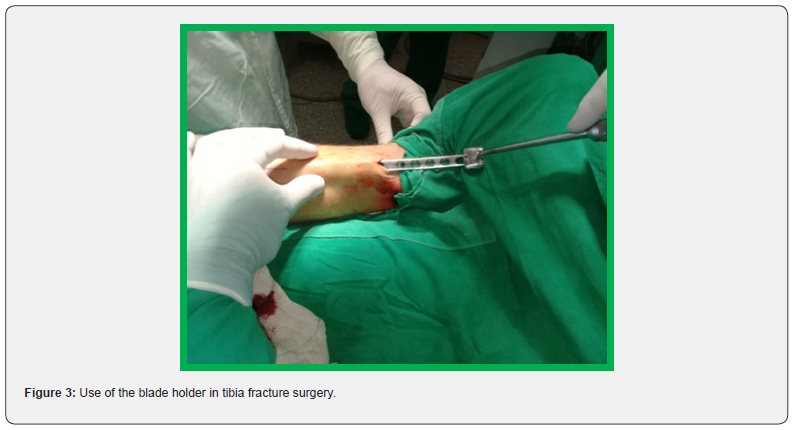
Thanks to the study of a focus group of professionals, a series of proposals are provided to make modifications to the MIPO technique in tibial diaphyseal fractures. These were prioritized by a nominal group of specialists, with experience in traumatology for more than 20 years and provided positive opinion, to present them to a group of experts. Based on the impossibility of having a minimally invasive surgery set, to perform osteosynthesis in tibia fractures, the same happens with the impossibility of acquiring minimal contact sheets, and with all these providing patients with a treatment option in accordance with the principles modern 2004 osteosynthesis association and combine them with less surgical aggression and the possibility of minimizing risks and avoiding complications. These professionals led by the project manager presented a series of modifications that, after being prioritized in the group, were as follows, table 3. Minimally invasive osteosynthesis is a suitable treatment method for tibial fractures and provides a high union rate and a good functional result. It can be an alternative treatment if its indications are taken into account; This technique can be reproducible with AO plates, without the need for special instrumentation (Figure 3) and, as it is a biological osteosynthesis that preserves vascularization and fracture hematoma, it has less risk of complications (Figures 1-3).


Discussion
The modification to the MIPO technique in our context is a necessity since we do not have the specific instruments to perform the technique as described by its authors, however, it complies with the general guidelines of the Arbeitsgemeinschaftfür Osteosynthesefragen (AO). This Swiss foundation, created in 1958, defines the principles of osteosynthesis worldwide. The development of AO surgical techniques for the treatment of fractures constituted a great advance in medicine [8]. The principles of fracture treatment enunciated by the AO are currently re-evaluated and redefined. The reformulation of these principles can be interpreted as follows:
Adequate functional reduction
One should always try to achieve the best possible anatomical restoration and the conservation of the longitudinal axis of the bone, a very important factor to allow correct mobilization of the joints neighbouring the fracture site. It is considered a primary or direct bone union in which osteosynthesis is carried out by opposition of the ends, anatomical reduction and interfragmentary compression; Minimally invasive osteosynthesis does not emphasize absolute stability, but rather the preservation of vascularity and soft tissues, [9] this term was developed by the AO/ASIF within the framework of a new conception of bone consolidation in the fractures of the diaphysis and contributes to achieving minimal disturbance of the biology in the fractured area [10]. The different forms of stability are explained from the histo-morphological point of view - the principle of compression is understood, which gave absolute stability, evidenced from the clinical point of view in early, painless movement without the formation of bone callus. to X-rays (per primamo consolidation without callus).
The biomechanical principle in osteosynthesis is the way in which the implants and the bone in which they are applied function or interact for the surgical treatment of fractures. At this point, some concepts have changed in recent times: [11] Indirect bone union is in which a non-anatomical reduction is achieved, preserving the axis and structural conformation of the bone through a tutor-like system in which a secondary consolidation, with the presence of bone callus and the preservation of the biological environment is prioritized; When a closed or minimally invasive bone reduction is added to this, it is known as biological osteosynthesis. Until very recently this procedure was not considered, the aim was always to faithfully reduce the fragments and place firm materials, by exposing the fracture focus; In light of the updated principles of osteosynthesis, the changes are evaluated.
Stable fixation: it is the most important factor if a satisfactory bone repair is to be achieved because excessive instability of the fragments induces osteolysis, delays the repair and induces a hypertrophic bone callus, even if the repair process fails. The function of an osteosynthesis material is to achieve relative stability while the fracture site, with its blood supply from the periosteum, is left virtually untouched [12]. As a consequence, movement between the fragments causes the fracture to heal secondarily. with callus formation; Indirect fracture reduction to achieve axial and rotational alignment is a challenging process. The amount of interfragmentary movement is influenced by the stability achieved, which is resolved by the rigidity of the material used, the width of the opening depends on the reduction achieved.
Appropriate surgical technique: the surgical technique must be as atraumatic as possible and avoid exaggerated manipulation of the tissues and it is necessary to be very careful with the irrigation of the fragments and the affected bone, all under the best possible conditions [13]. Biology is essential in the preservation of vascularization, with minimal access and minimally invasive osteosynthesis with plates, always guided by images, a precept with which our modifications to the technique comply. Significant soft tissue injuries contribute to delayed healing, in part due to loss of vascular supply to the bone; The intramedullary vascular supply is normally provided by nutrient vessels that irrigate the medullary contents and part of the cortex. Only the outer third of the cortical bone receives its blood supply from the tissues that cover it (periosteum). The most important factor in the management of a fracture is the care of the soft tissues and maintaining the blood supply to the bone fragments, without damage to the fracture hematoma [14]. In many displaced fractures of long bones, the spinal vascularization is altered and the vascular supply will depend only on the soft tissues adhered to the periosteum. The involvement of the remaining vascularization by surgical intervention in a displaced fracture has been clearly related to the lack of consolidation, due to the effects of periosteal detachment and soft tissue dissection. As consolidation occurs, the spinal system resumes and a normal vascularization pattern may be re-established.
Early mobilization: whenever osteosynthesis allows it, early mobilization of the affected limb should be initiated because it is an important stimulus for osteogenesis; The rapid return to activity significantly reduces the negative effects caused by fracture disease and minimizes muscle atrophy, adhesions and ankylosis. The author considers that although they are not frequently indicated, these techniques provide the specialist with an alternative method for bone stabilization in complex fractures of the tibia. The final objective, in any case, is to minimize the surgical aggression without reducing the effectiveness of the technique performed because it includes the preservation of the fracture hematoma, less surgical trauma to the soft tissues, the reduction of surgical time and, consequently, the reduction in the risk of infection and, finally, the indirect healing process with abundant callus. The performance of these techniques must be carried out by specialists experienced in traditional osteosynthesis. We must not forget that, during the learning curve, a mini-invasive procedure may require an open reduction of the focus, so in-depth knowledge of the anatomy of the musculoskeletal system and traditional surgical approaches is essential.
Babst and Khong [15] summarized the indications for minimally invasive osteosynthesis:
a. Epi-/metaphyseal fracture.
b. Inappropriate soft tissue condition.
c. Intramedullary nailing is not feasible, there is no image intensifier or they are not available.
In fractures of the tibia, these types of implants are indicated in injuries that occur in any area of the bone that ranges from the proximal end, diaphysis and distal end. The indications are the same as for traditional osteosynthesis with open reduction and wide approaches; However, one of the important differences is that minimally invasive plate osteosynthesis does not have as its primary objective anatomical reduction or exact, but only the correct alignment of the fragments in the longitudinal axis [16]. Care should be taken to avoid medial or lateral rotational defects and, finally, in multi-fragmented fractures it is important to avoid shortening. Osteosynthesis planning is essential to determine the length of the implant. It is important to mention that there is no publication, clinical research or textbook that mentions how long the implant should be. Some suggest that the ends of the fracture, proximal and distal, be located and from there measure at least two centimetres to place the screws most proximal to the fracture; It should be taken into account that there must be at least three screws at each end of the implant [17].
Various reduction methods can be used, from manual to the use of pointed forceps for percutaneous reduction. If the anatomical conditions of the bone and the fracture allow it, it is very important to perform a balanced osteosynthesis; That is, from the centre of the fracture towards the ends the same implant distance must be measured. After sliding the plate, radiological control should be performed to ensure that the bone drilling and screw placement are adequate. Finally, the wounds are sutured with conventional technique, without leaving drainage, and the leg is covered with gauze to protect the wounds. Postoperative management is the same as that used in traditional osteosynthesis. In the case of stable fractures with possibilities of bone support, weight unloading can begin from the beginning with partial weight bearing, which gradually increases until reaching full unloading in a period of six weeks. If there is no bone support (multi-fragmentation), you should wait until you see radiological signs of consolidation before starting weight bearing. Osteosynthesis evolves theoretically and practically throughout its use, trends in the use of large dissections for more rigid methods of fixation are moving towards minimally invasive osteosynthesis, but universal clinical adoption will depend on the clinical results observed, therefore that the evaluation of works on the subject is necessary to prove its effectiveness [18,19]. These minimally invasive treatments provide adequate union rates, with few complications, as well as quite good functional results [20].
Indirect reduction techniques were developed to avoid further soft tissue injury at the fracture site and thus improve fracture healing rates. In relation to the weeks of consolidation, Bingol et al. [21] published a study with 30 patients treated using a minimally invasive technique in which a consolidation of 19.2 weeks was obtained; in the study carried out by Zhang [22] the consolidation occurred around of 16.7 weeks and developed by Andalib and collaborators, similar results were obtained and analyses of the effectiveness of the method were carried out [23]. Despite the size of the sample in the consulted works and its retrospective design, the results of this research support that the treatment of tibia fracture using the minimally invasive technique has a group of advantages: surgical time is less, with less damage to the soft tissues, the surgical incisions are smaller, less painful and more aesthetic, the hospital stay, blood loss and infection rate are reduced, in general recovery is faster and postoperative pain is reduced.
Conclusion
The largest number of proposals on modifications to the MIPO technique for tibial diaphyseal fractures were made on the instruments, although the proposals are multiple; after prioritizing in the group, seven modifications to the technique remained as proposals. Modifications to the MIPO technique may be another alternative in the therapeutic arsenal, mainly in fracture injuries of the tibia with multiple fragments, although its limitations must be considered if the principles of osteosynthesis are not taken into account. Case studies with a larger number of samples and longer periods of evolution are necessary.
References
- Wenger R, Oehme F, Winkler J, Perren SM, Babst R, et al. (2017) Absolute or relative stability in minimal invasive plate osteosynthesis of simple distal meta or diaphyseal tibia fractures? Injury 48(6): 1217-1223.
- Aguyo GLM (2022) The transcendence of history in the development of modern orthopedics and traumatology. Orthotips 18(2): 170-175.
- Afzal T, Sharma N, Gupta A (2018) Treatment of Comminuted Long Bone Fractures by Biological Plating. JK Sci 20(1): 44-48.
- Hernández Vaquero D, Fernández Fairen M, Torres Pérez A, Santamaría A (2012) Minimally invasive surgery versus conventional surgery. An approach from scientific evidence. Rev Esp Cir Ortop Traumatol 56(6): 444-458.
- Schell H, Duda GN, Peters A, Tsitsilonis S, Johnson KA, et al. (2017) The haematoma and its role in bone healing. J Exp Orthop 4: 5.
- Sreejith Thampy J, Nagakumar JS, Manohar PV, Pammi Karthik R (2018) Minimally invasive percutaneous plate osteosynthesis (MIPPO) in distal tibia fractures-retrospective functional and radiological outcome analysis among rural population. Int J Orthop Sci 4(2): 596-600.
- Chandrakant Supe A, Vinayak Kinge K, Martand Badole C, Wandile KN, Patond KR (2016) Minimally invasive percutaneous plate osteosynthesis in distal tibial fracture: A series of 32 cases. Int J Orthop Sci 2(1): 6-9.
- Bemelman M, van Baal M, Yuan JZ, Leenen L (2016) The Role of Minimally Invasive Plate Osteosynthesis in Rib Fixation: A Review. Korean J Thorac Cardiovasc Surg 49(1): 1-8.
- Bhat R, Wani MM, Rashid S, Akhter N (2015) Minimally invasive percutaneous plate osteosynthesis for closed distal tibial fractures: a consecutive study based on 25 patients. Eur J Orthop Surg Traumatol 25(3): 563-568.
- Asimuddin M, Kulkarni M (2017) A clinical study of minimally invasive percutaneous plate osteosynthesis of proximal tibial fractures using locking compression plate. Int J Orthop Sci 3(1): 740-746.
- Wajnsztejn A, Santos Pires RE, Godoy Dos Santos AL, Labronici PJ, Alvachian Fernandes HJ, et al. (2017) Minimally invasive posteromedial percutaneous plate osteosynthesis for diaphysealtibial fractures: technique description. Injury 48(Suppl 4): S6-S9.
- Schwarz O, Majerníček M, Chomiak J (2020) Treatment of Fractures of the Distal Third of Tibia Diaphysis by MIPO Technique. Acta Chir Orthop Traumatol Cech 87(2): 114-119.
- Li A, Wei Z, Ding H, Tang H, Liu Y, et al. (2017) Minimally invasive percutaneous plates versus conventional fixation techniques for distal tibial fractures: A meta-analysis. Int J Surg 38: 52-60.
- Pawar KA, Panjwani TR, Panase JB, Sancheti PK (2015) Management of Comminuted Fractures of Lower Extremity with Minimally Invasive Plate Osteosynthesis. J Evol Med Dent Sci 4(61):10687-10696.
- Babst R, Khong KS (2007) Minimally invasive surgery. In: Rüedi TP, Buckley RE, Moran CG, eds. AO Principles of Fracture Management. Stuttgart: Georg ThiemeVerlag p. 199-212.
- Gülabi D, Bekler Hİ, Sağlam F, Taşdemir Z, Çeçen GS, et al. (2016) Surgical treatment of distal tibia fractures: open versus MIPO. Ulus Travma Acil Cerrahi Derg 22(1): 52-57.
- Vidović D, Matejčić A, Ivica M, Jurišić D, Elabjer E, Bakota B (2015) Minimally-invasive plate osteosynthesis in distal tibial fractures: Results and complications. Injury 46(Suppl 6): S96-S99.
- Yang KH, Won Y, Kang DH, Oh JC, Kim SJ (2015) Role of appositional screw fixation in minimally invasive plate osteosynthesis for distal tibial fracture. J Orthop Trauma 29(9): e331-335.
- Toogood P, Huang A, Siebuhr K, Miclau T (2018) Minimally invasive plate osteosynthesis versus conventional open insertion techniques for osteosynthesis. Injury 49(Suppl 1): S19-S23.
- Gupta P, Tiwari A, Thora A, Gandhi JK, Jog VP (2016) Minimally Invasive Plate Osteosynthesis (MIPO) for Proximal and Distal Fractures of The Tibia: A Biological Approach. Malays Orthop J 10(1): 29-37.
- Bingol I, Yalcin N, Bicici V, Tulunay T, Yuksel K, et al. (2015) Minimally invasive percutaneous plate osteosynthesis does not increase complication rates in extra-articular distal tibial fractures. Open Orthop J 9: 73-77.
- Zhang J, Ebraheim NA, Li M, He X, Liu J, et al. (2015) External Fixation Using a Locking Plate: A Reliable Way in Treating Distal Tibial Fractures. J Orthop Trauma 29(11): e454-458.
- Andalib A, Sheikhbahaei E, Andalib Z, Tahririan MA (2017) Effectiveness of Minimally Invasive Plate Osteosynthesis (MIPO) on Comminuted Tibial or Femoral Fractures. Arch Bone JtSurg 5(5): 290-295.






























