Load Management in Sports Must Include Biomechanical Analytics℠
Tim Maggs1, Steven Brownstein2* and Alexandros Siozos3
1DC, Director, Maggs Sports Chiropractic Biomechanics and Wellness Center Director, Sports Injuries and Biomechanics, USA
2MD, Radiologist, Medical Director of Dynamic Medical Imaging, Medical Director of Spinal Kinetics, LLC Union, USA
3MD, Consultant in Orthopaedic Surgery, Private Practice, Kozani, Greece
Submission: December 04, 2023; Published: December 14, 2023
*Corresponding author: Steven Brownstein, MD, Radiologist, Medical Director of Dynamic Medical Imaging, Medical Director of Spinal Kinetics,LLC Union, USA
How to cite this article: Tim Maggs1, Steven Brownstein2* and Alexandros Siozos3. Load Management in Sports Must Include Biomechanical Analytics℠. Ortho & Rheum Open Access J. 2023; 22(4): 556094. DOI: 10.19080/OROAJ.2023.22.556094
Abstract
As sports have become much more analytical over the past 2 decades, so has the science of loading and overloading joints, tendons, ligaments, bones, and muscles of athletes. The goal has always been twofold; first, to provide information that will help athletes stay under the “overloaded” point which leads to injury and second, to help keep athletes active, healthy, and participating. Our goal is to introduce the concept of biomechanical analytics and tests needed to identify more productive and relevant findings when trying to keep athletes uninjured. There are well established biomechanical “norms” for an athlete, however, to date, no one has systematized the testing required to determine normal and abnormal biomechanics of the athlete. This paper will introduce the very basic tests that must be performed to achieve ultimate load management. These tests are ideally performed prior to the season while an athlete is not injured.
Keywords: Structural Management®; Structural Fingerprint® Exam; Load Management; Normal and Abnormal Biomechanics; Biomechanical Analytics℠; Dr Maggs℠ Leg Length Test
Background of Traditional Load Management
Load management is defined as the deliberate temporary reduction of external physiological stressors intended to facilitate global improvements in athlete wellness and performance while preserving musculoskeletal and metabolic health. Basically, you reduce the amount of training and/or competition an athlete takes on to help them recover better and perform better over the long term [1]. Significant progress has been made in the field of injury prevention over the last few years. However, there is still a gap between research and the implementation of injury prevention programs in the real world and the burden of sports-related injuries remains high (Lee Herrington).
Introduction
The 3 major sports leagues in the U.S. are all paying special attention to the concept of load management. How much can a body take before it begins to break down? What steps can be taken to minimize the risk of injury to these athletes? The question of load management should be considered even for our youngest athletes playing sports today. At every age level and physiological maturation level, there is a point where the straw will break the camel’s back. Everyone’s goal is to stop before that point. Or learn how to raise the ceiling of potential. In every league, all load management guidelines have to do with external or activity factors. Minutes played. Pitches thrown. Innings played. Pitch velocity. To date, no one has looked internally at the athlete to understand the biomechanics, or more importantly, the abnormal biomechanics of an athlete that causes excessive loading to specific joints, tendons, muscles, ligaments, and bones. Along with excessive loading of any of these tissues, there is an accumulation of stresses prior to injury which increases the vulnerability of each athlete in unique ways. When an athlete weight trains, there is a point of tissue fatigue. This is due to the accumulation of stress in the short term. On a more macro level, tissues of the body that are under uncontrolled elevated stress due to abnormal biomechanics will accumulate stresses and will also reach a point of tissue fatigue, and that’s when injuries occur. This applies especially to injuries like ACL tears, Achilles tendon ruptures and torn hamstrings.
Dr. Maggs℠ Law of Tissue Tolerance
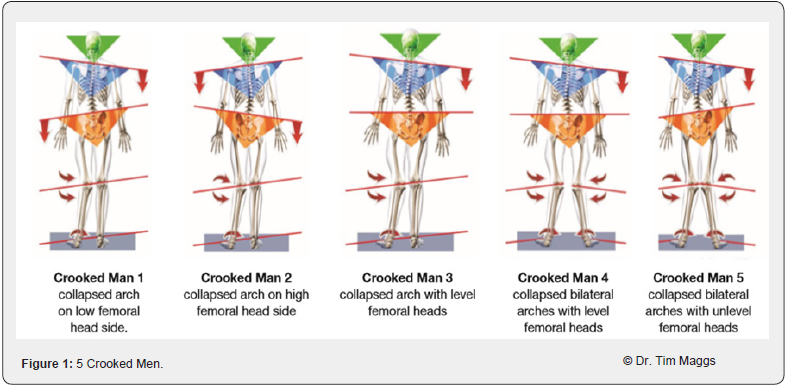
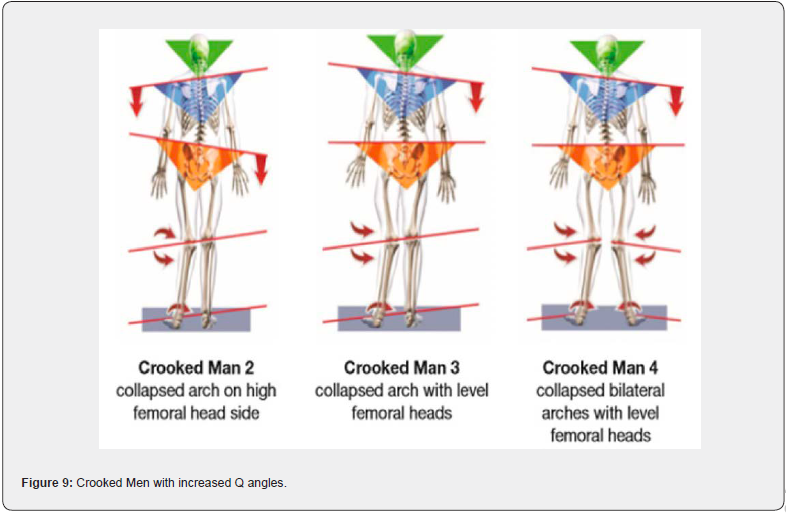
When the loading of a tissue exceeds the capacity of that tissue, compensatory physiological changes occur. Research has shown there are 5 unique biomechanical patterns (Crooked Man 1-5) [2], however, within each of these unique patterns, there are additional biomechanical faults that need to be detected when attempting to reduce the risk of injury in athletes (Figure 1).
Materials and Methods
This study has no control group. We are not looking to prove treatment efficacy, we are looking to prove that all people have biomechanical, or musculoskeletal, imbalances that can be detected using today’s technology. These imbalances are the breeding ground for the increased incidence in sports injuries, workplace injuries, and degenerative changes. This study highlights the evaluation of 4 critically important areas of the body when looking to reduce musculoskeletal injuries; the feet, the knees, the lumbo-pelvic spine, and the cervical spine. The lumbar spine (low back) and cervical spine (neck) both have lordotic curves and have proven over the years to be more pre-disposed to degenerative changes and injury, particularly strain/sprains and disc injuries. We will look at both normal and abnormal biomechanics as well as the tests that can be performed to detect these findings.
The Feet
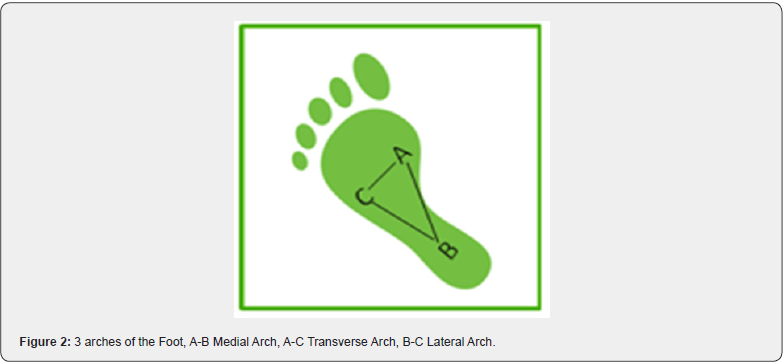
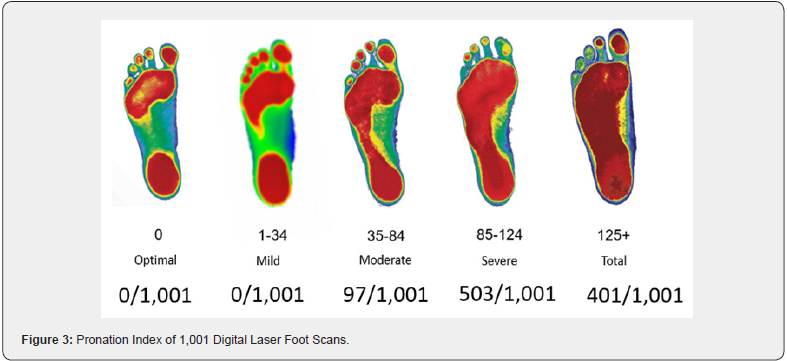
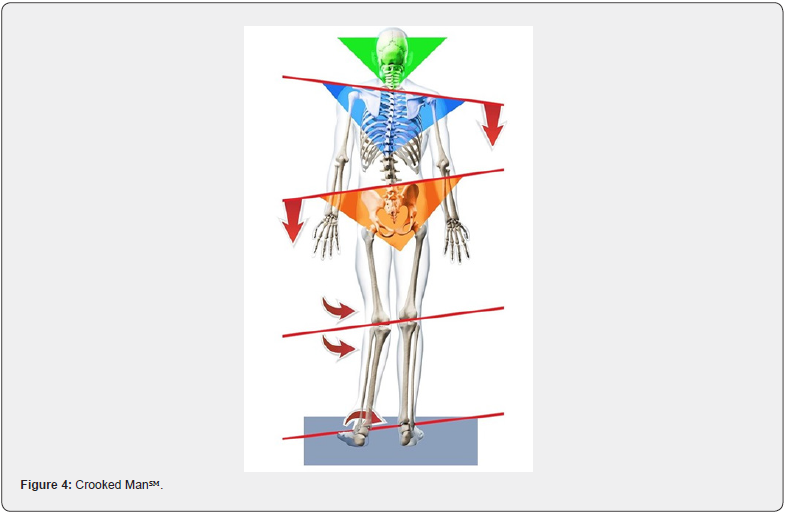
The feet are thoroughly overlooked by today’s sports medicine community. The feet are the foundation of the human body, and when the body is looked at architecturally, the importance of the function and symmetry of the feet cannot be overstated. There are 3 arches of the feet, the medial arch, the transverse arch, and the lateral arch (Figure 2). The feet are categorized as either pronated, neutral, or supinated. Some feet are defined as neutral and supinated by some experts. The lateral arch is the first arch of the foot to collapse and virtually all people have a collapsed lateral arch in their feet. Therefore, the entire foot cannot be defined by one category. Studies have shown there is a significant amount of arch collapse in all people [3,4]. This study used digital laser scanning to evaluate 1,001 patients. In each case, there is a unique collapse of one or more arches of the feet, and very often an asymmetrical collapse. An asymmetrical collapse is due to the imbalanced weight distribution of the body due to biomechanical imbalances of the entire structure. With the unique collapse of the feet, there is a domino-like effect going up the structure. Due to the fact the human body is compensatory when in a weight bearing state, the entire kinetic chain is affected by the collapse of the feet. Abnormal biomechanical findings found on the cervical (neck) x-rays, lumbo-pelvic (low back) x-rays, and knees can oftentimes be traced back to the collapse of the feet (Figure 3). Leg length plays an important role in the asymmetry of the feet. When one leg is detected to be longer than the other, there typically will be greater collapse of one foot compared to the other. The Dr. Maggs℠ Leg Length Test [2] was designed to determine an individual’s leg length difference. When the unique abnormal biomechanics of an individual are combined with repetitive and continual activity the most vulnerable area of that structure will predictably become injured first (Figure 4).
The Knees
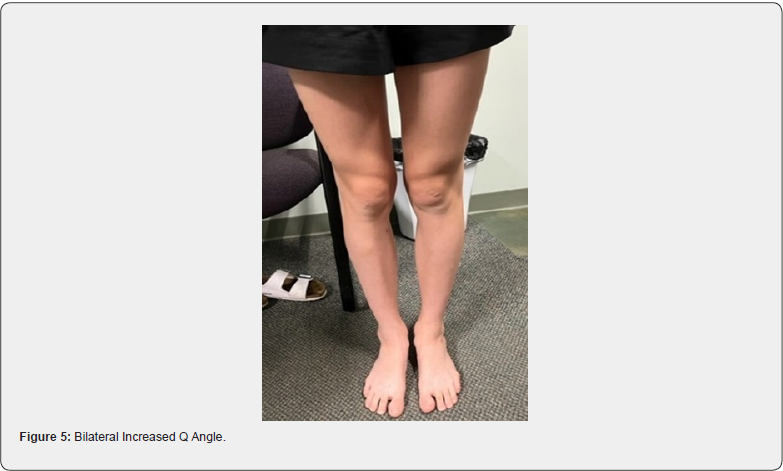
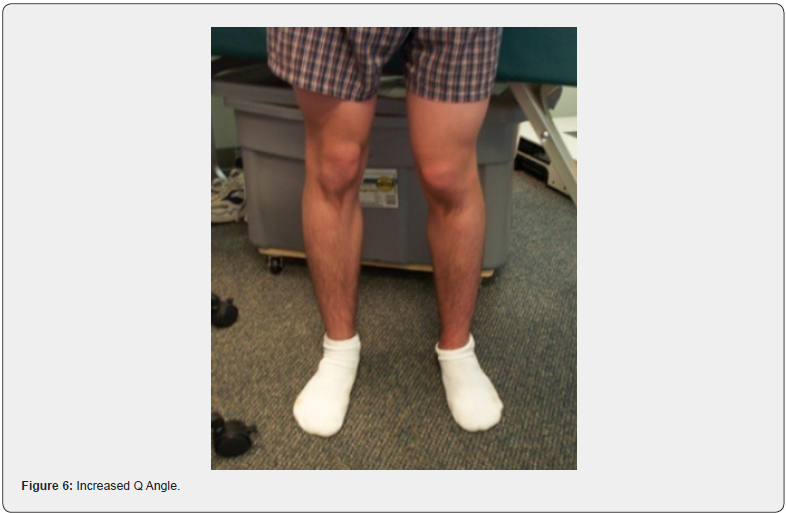
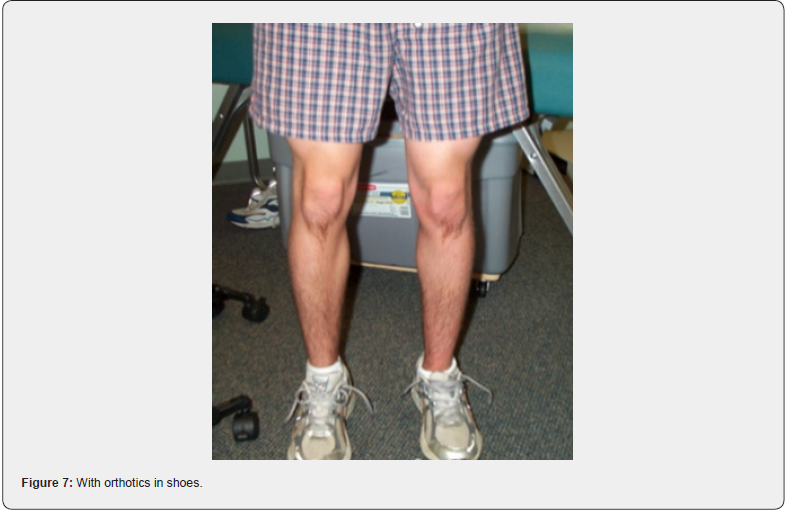
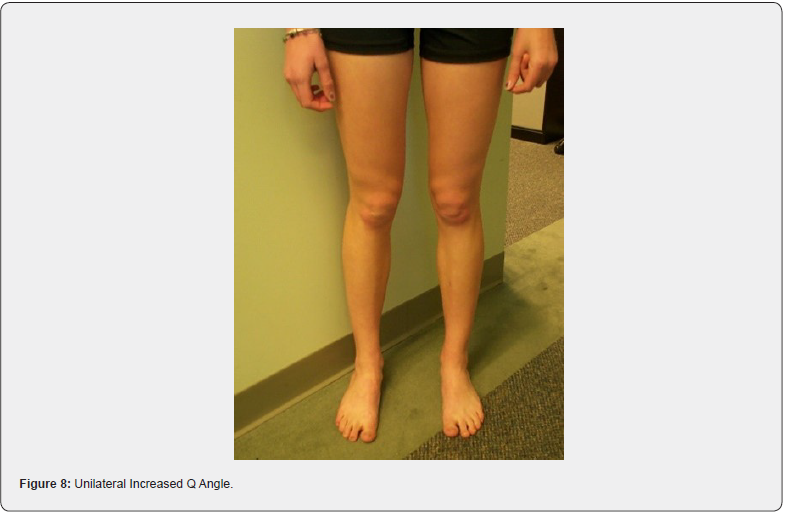
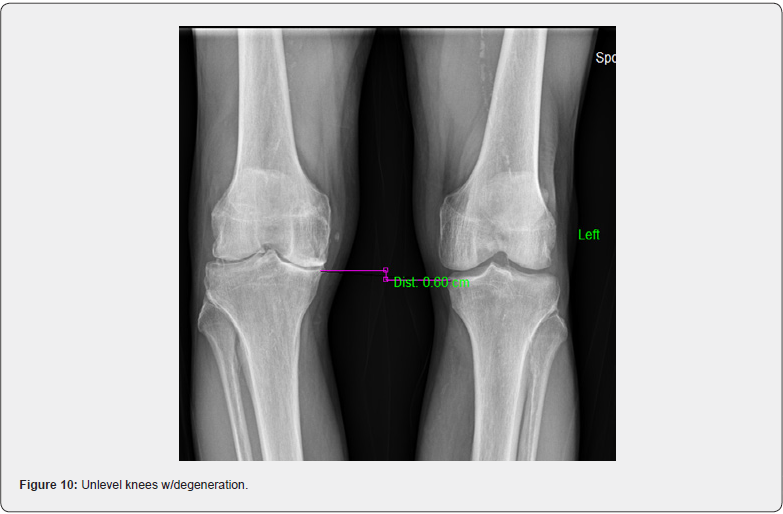
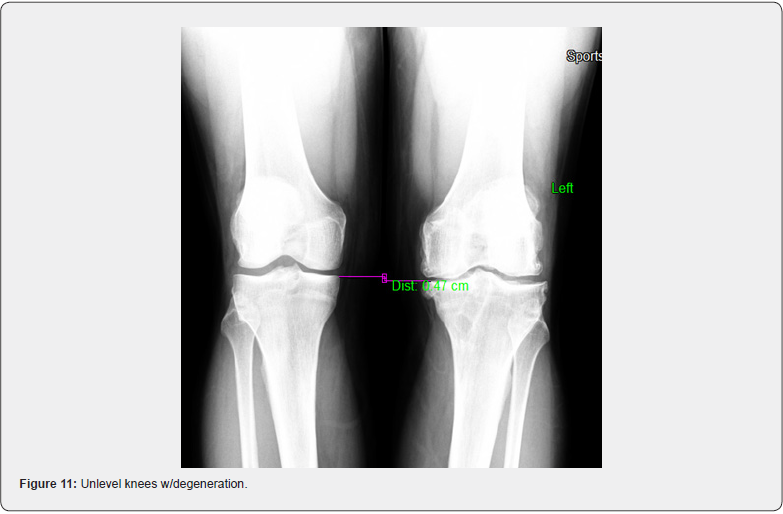
The knees are a hinge joint and with perfect alignment the weight distribution is more evenly distributed and best tolerated. In the standing position, the center of the patella (kneecap) should be midline. In many cases, there is a medial rotation of the patella, better known as an increased Q angle. This now creates an imbalanced hinge joint. This increased Q angle is more prevalent in younger athletes and seen more in younger female than male athletes. Active women are at least twice as likely to suffer serious knee injuries as men, but it’s not just athletes who are at risk. Since a woman has a wider pelvis, her femur (thigh bone) descends into the knee at an inward angle (Figure 5). When a woman becomes fatigued, as during an athletic event, the angle on landing becomes more pronounced, further increasing the chance of injury [4,5]. Biomechanical imbalances, which includes the knees, in both male and female athletes, contribute greatly to knee injuries and premature knee degeneration. An increased Q angle is always secondary to some degree of pronation of the feet. However, in some cases, correction of the feet with orthotics will provide full improvement of the Q angle if leg lengths and femoral head height are equal and level (Figures 6 & 7). In most of the population, however, femoral head height is still unlevel even after orthotics are put in the shoes [6]. This is always true with Crooked Man 2, Crooked Man 3, and Crooked Man 5. This most likely is due to the body’s tendency to attempt to level femoral heads during activity. The knee will “buckle” medially to accommodate this biomechanical pattern. This further promotes the need for an A-P L-S x-ray of the femoral heads with orthotics in the shoes to determine how much of a FHHD there is after the feet are corrected (Figures 8 & 9). An A-P bilateral knee x-ray in the standing position can also show a difference in the height of the knees, which when different enough, is a contributor to knee injuries and an accelerator of degeneration (Figures 10 & 11).
Lumbo-Pelvic Spine
The lumbo-pelvic spine (low back) is made up of the lumbar spine and the pelvis. The first and most informative biomechanical test to be done is with digital x-ray. It is important to have all x-rays taken with the patient standing to have the influence of gravity play a role in the evaluation of the patient. X-rays taken in the recumbent position eliminate the effects of gravity and will not allow the examiner to detect the needed biomechanical information.
A-P Lumbo-Pelvic Spine
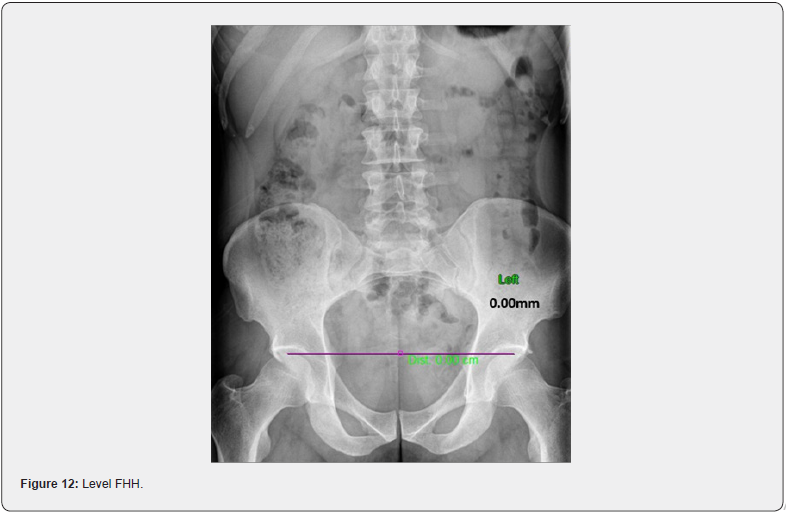
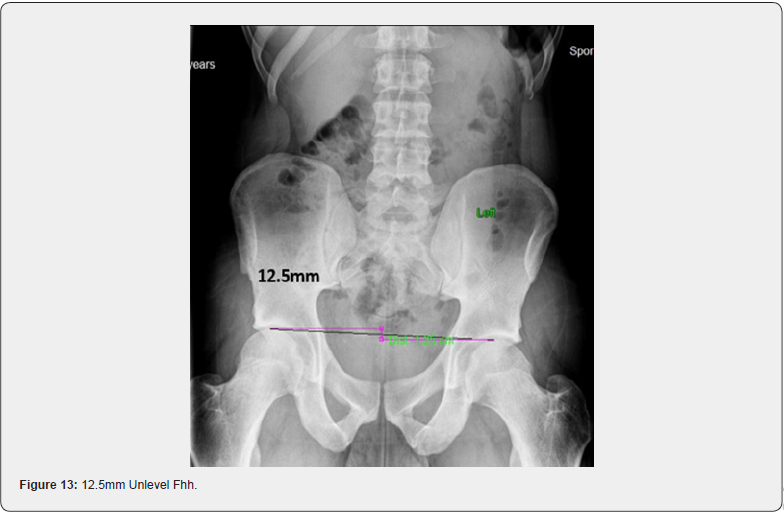
To detect leg length in the weight-bearing position, you must first correct the collapse of the arches of the feet. This is done with orthotics. The goal of orthotics is to provide arch support and to create symmetry in the feet. Once the feet are supported and symmetrical, there is an inherent reduction of stress in the knees, hips and low back. Once orthotics are in the shoes, an A-P L-S x-ray must be taken to determine femoral head height (hip height) difference (FHHD). The central ray of the x-ray should be 1” below the umbilicus to reduce abnormal magnification. Normal FHHD is < or = to 3mm [6]. If FHHD is greater than 3mm, then a lift must be placed underneath the heel of the orthotic on the low femoral head side. In cases where FHHD is extreme, i.e. 15mm or more, the examiner cannot use a lift that will produce level hips. Improved FHHD is the goal here. FHHD is the only measurement that is needed on this x-ray, and only needs to be addressed with a lift under the appropriate orthotic if the difference is > than 3mm (Figures 12 &13).
Normal Lateral Lumbo-Pelvic Spine
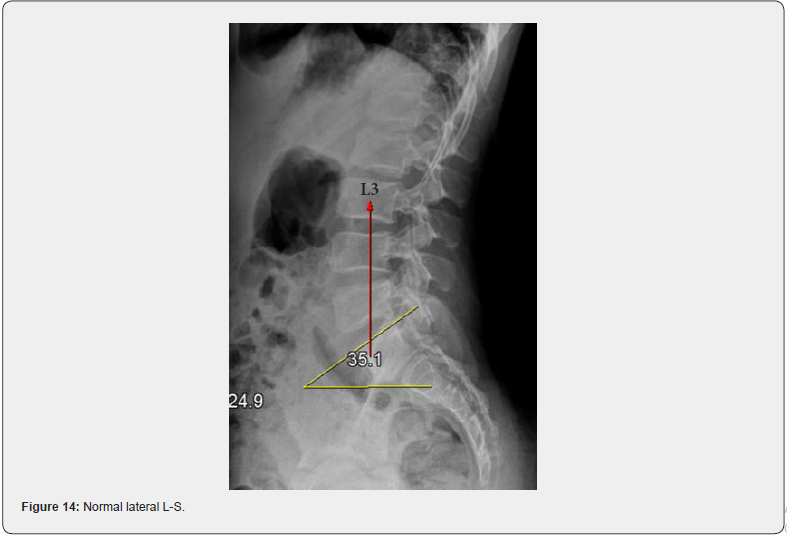
The lateral or side view x-ray provides significant and predictable information. From a biomechanical perspective, there are 2 key measurements, the sacral base angle and Ferguson’s center of gravity line [7]. The optimal sacral base angle is 35°-42°. The optimal center of gravity line (vertical line) originates in the center of the body of L3 and vertically bisects the anterior 1/3 of the sacral base. When these measurements are normal, the biomechanical weight bearing is being evenly distributed through the supportive tissues that are designed to handle this weight (Figure 14).
Abnormal Lumbo-Pelvic Spine
When the weight bearing in the low back engages tissues that are not designed to tolerate this weight, physiological changes occur. Initially, these changes consist of muscle tightening, inflammation, and pain.
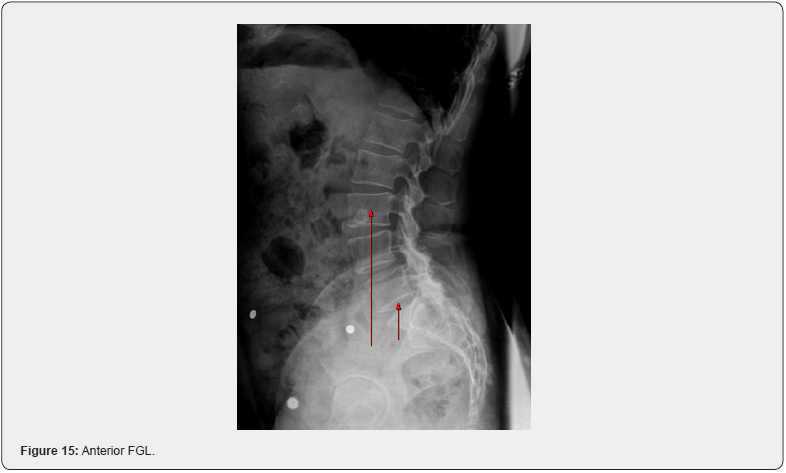
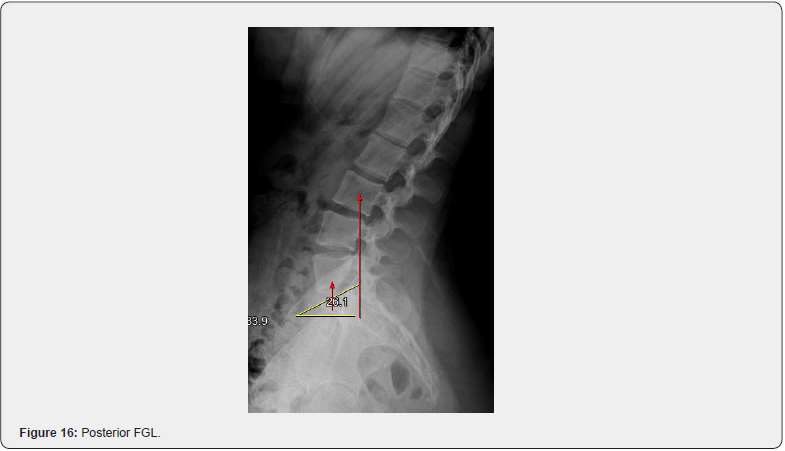
Over time, there are desiccation (dehydration) and bulging/herniation changes to the discs, arthritic changes to the facet joints, impingement of the nerve roots and an acceleration of degenerative changes and pain. When Ferguson’s center of gravity line falls anterior to normal, there is increased loading posterior at the facet joints (non-weight bearing joints). Over time, MRI findings would present facet arthrosis due to the long-term abnormal loading. When Ferguson’s center of gravity line falls posterior, the loading of the posterior discs is increased which increases the potential for disc injuries to occur. Discs begin to break down with disc bulges, but these bulges progress into herniations (protrusions and extrusions) [8]. Because our current sports medicine system never looks at the biomechanics of an athlete, disc health is only considered once injured and traditional treatment is usually a shot of cortisone, a series of physical therapy treatments or ultimately, surgery (Figures 15 & 16).
Cervical Spine
When discussing human biomechanics, the neck has often been called the 5th floor of the building. The variance here is that buildings are not compensatory while the human body is. The cervical spine’s position will be governed by the abnormal biomechanics of the feet, knees, femoral head height, and lumbar spine. The neck will be forced into whatever position the body needs to find balance. Unfortunately, since every human has biomechanical faults and all humans have some degree of collapse of the feet [5], it is very rare to find someone with normal cervical biomechanics.
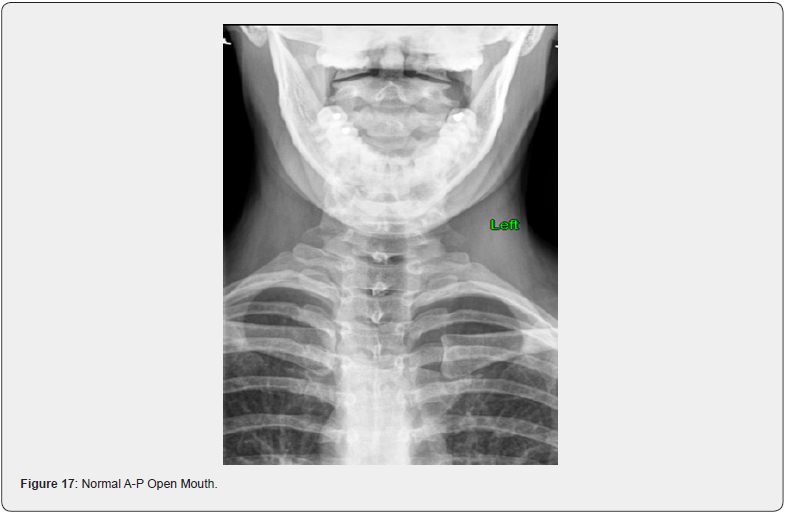
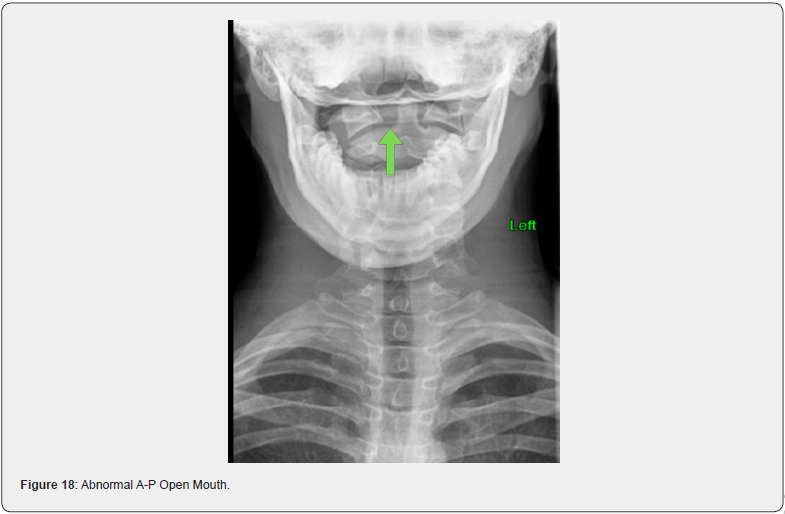
A-P Open Mouth View
This study has the patient open their mouth for the x-ray to remove the teeth from blocking the viewing of the top 2 vertebrae, Atlas and Axis. The importance of this view is to look at the alignment of these vertebrae, as the spinal cord must pass through these 2 vertebrae to bring nerve function and energy to the entire body. When there is misalignment, there is a predictable irritation to the nervous system producing a reduction or abnormal nerve flow to other areas of the body, including organs and glands. Symptoms that can arise from a misalignment of Atlas and Axis are headaches, stomach problems, asthma, allergies, and dizziness. In many cases, the imbalance at this level in the spine can be traced back to the feet or leg length difference (Figures 17 & 18).
Lateral Cervical
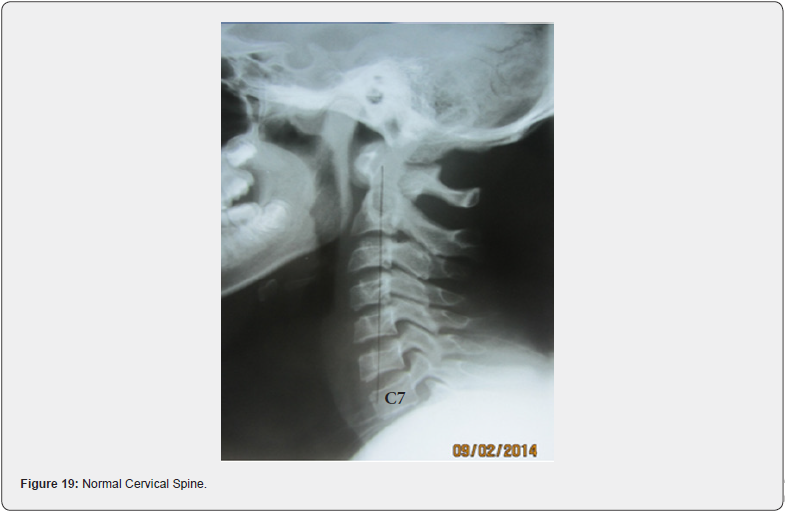
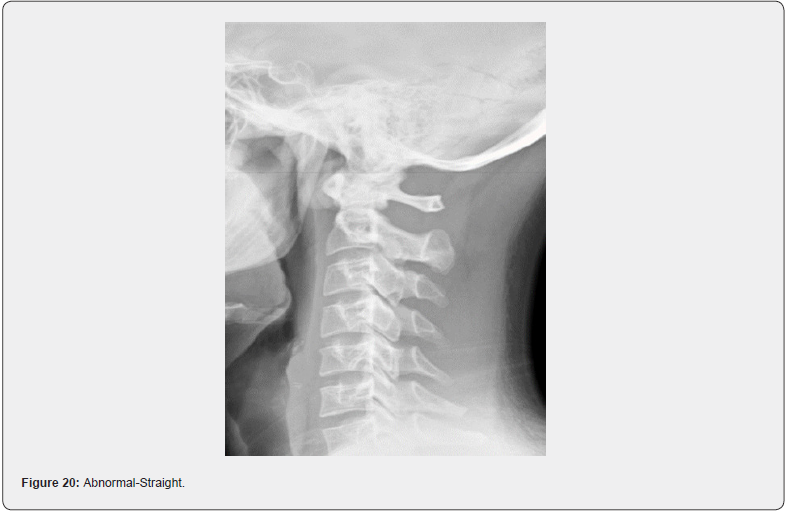
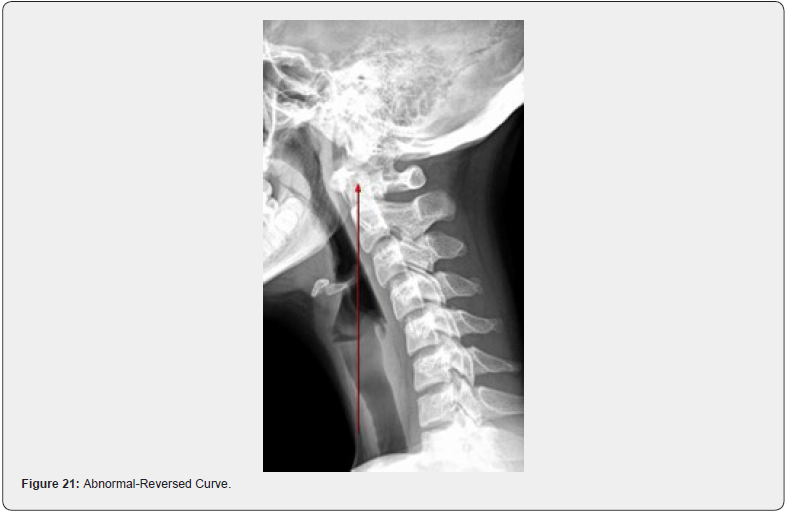
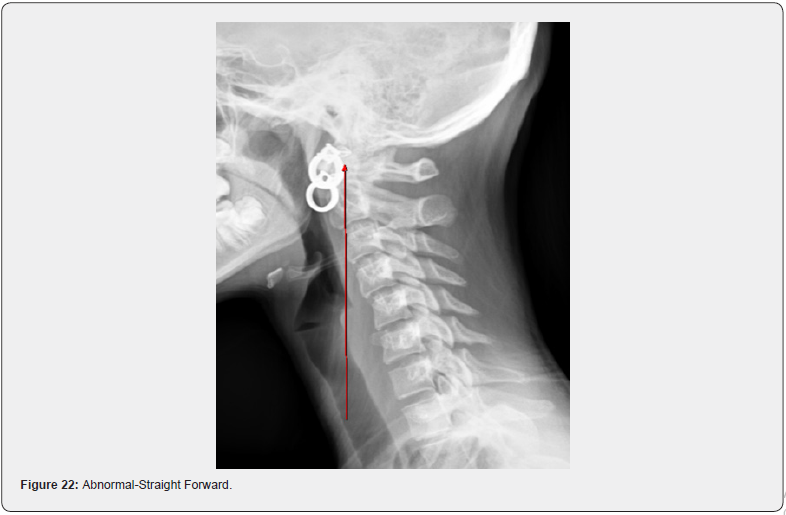
The lateral or side view of the neck looks at the curvature of the neck. The normal lordotic curve provides healthy shock absorption as the weight of the head, estimated to be approximately 10% of the body weight, produces tremendous stress on the joints and discs of the neck. The normal neck should have a forward, or lordotic, curve, with the gravity line running from the apex of the odontoid process through all segments of the spine and ultimately the body of C7. In other words, there should be a curve with every bone sharing in the distribution of weight of the head (Figures 19 & 20). An abnormal curvature can present in multiple ways. The neck can have a straight, or military curve. A neck with an abnormal curvature will produce a constant and increased stress throughout the neck as there is a reduced shock absorption that a normal curvature would provide. There is the reverse curve which will cause an increase in demand of the muscles of the back of the neck and shoulders to have to work overtime just to hold the head up. With this type of neck there is an increase of lower cervical degenerative changes, as the loading in the lower cervical spine is increased, producing fixations of the lower cervical joints and ultimately an increased vulnerability to injury and an acceleration of degeneration. Finally, there is the straight, forward leaning neck. This suffers the same consequences as the reverse curved neck (Figures 21 & 22).
Discussion
Injury prevention does not exist in sports today. Those in charge of locker rooms specialize in reactive care, not proactive care. For prevention to become a part of the future landscape of sports medicine, there must be a major paradigm shift. There must be 2 departments per team rather than one department. Drs. and therapists must be specially trained in the testing, diagnoses, and treatment of athletes from an injury prevention point of view. All human beings can be looked at as architectural structures, as they too are victims of gravity, aging, and stress. It is not clearly understood how the field of human biomechanics can be so advanced, with tests like The Structural Fingerprint® Exam and Dr. Maggs℠ Leg Length Test yet ignored by so many. The cost of injuries in the 3 major leagues in this country has now exceeded $1 billion per year. In 2023 the Albany Patroons, a storied professional minor league basketball team in upstate New York, played 32 games and one player missed 2 games with a strained knee. This is the first team to function under the Structural Management® Program, a proactive injury prevention program [5]. Not only do these recommendations apply to professional sports teams, but college, high school, middle school, and younger is where this approach should begin. The Concerned Parents of Young Athletes℠ Program was developed in 2004, and the single goal is to raise the awareness of sports biomechanics in the middle and high school population and encourage biomechanical exams in combination with the current medical exams that are now performed. Evaluating the eyes, ears, noses, and throats of our young athletes is hardly sufficient if the goal is injury free physiological growth. Much work must be done, but the protocols, guidelines, tests, and recommendations are waiting for the sports world to catch up. The decision to add an injury prevention department to a team should not be made by the experts in the reactive department. An injury prevention department is complementary, not a substitute or a replacement for existing sports med departments.
Conclusion
The information that can be provided from biomechanics has not been implemented in sports today. Reactive care is violently costly and must come to an end as the only form of care for athletes. Biomechanics research has been done, proactive injury prevention has shown massive success, and the protocols and programs are waiting to be implemented. We now need those responsible to step up and make bold decisions based on evidencebased science, not on politics and biases. There will always be a need for reactive care, however, it cannot and should not be the controlling department in the sports team’s locker rooms. That is analogous to only providing financial help to people once they are on the verge of bankruptcy. It’s already very late for today’s athletes. But, tomorrow’s athletes, team executives, and most importantly fans can experience a whole new world of sports once these decisions and changes are made.
References
- Giandonato J (2019) What is "Load Management" and Why Does it Matter to Athletes. Stack, p. 1-6.
- Maggs T, Steven B, Alexandros S (2020) When Correcting the Collapse of Arches of the Feet with Custom Orthotics, are Other Areas of the Body Effected? A Revolutionary Approach towards Reduced Injuries and Better Outcomes. Ortho & Rheum Open Access J 17(1): 555953.
- Maggs T, Steven B (2023) Each Person's Collapse of the Arches of the Foot May Be Unique, but its Correction is Standard. A Large Study Explains Why. Orthop & Rheum Open Access J p. 1-6.
- (2023) Knees are Casualties of Women's Sports.
- Maggs T, Steven B, Alexandros S (2023) From Disaster to Triumph: How a Professional Basketball Team Becomes Injury-Free Implementing a Revolutionary Proactive Approach to Injuries. Ortho & Rheum Open Access J 22(1): 556080.
- Maggs T, Steven B, Alexandros S (2021) Is Prescribing Custom Orthotics Enough to Prevent and Treat Musculoskeletal Injuries and Degeneration? What if we Integrated Biomechanical X-ray Measurements with the Laser Foot Scan Procedure? Could this Reduce Injuries Even More? Ortho & Rheum Open Access J 17(4): 555970.
- Rowe YA (2005) Essentials of Skeletal Radiology. Lippincott, Williams, and Wilkins.
- Lee Herrington P (nd.) Musculoskeletal Injury Prevention.






























