Surgical treatment of Comminuted Calcaneal Fractures using the Sinus Tarsi Approach with Tibio-Calcaneal Distraction: A Case Series
Johannes Pachinger, Florian Hess, Christoph Knoth, Benedikt Kislinger, Ralph Zettl and Nicolas Kesterke*
Department for Orthopedics and Traumatology, Kantonsspital Frauenfeld, Switzerland
Submission: December 12, 2019;Published: January 10, 2019
*Corresponding author: Nicolas Kesterke, Department for Orthopedics and Traumatology, Kantonsspital Frauenfeld, Pfaffenholzstrasse 3, 8500 Frauenfeld, Switzerland.
How to cite this article: Johannes P, Florian H, Christoph K, Benedikt K, Ralph Z, Nicolas K. Surgical treatment of Comminuted Calcaneal Fractures using the Sinus Tarsi Approach with Tibio-Calcaneal Distraction: A Case Series. Ortho & Rheum Open Access J 2019; 13(3): 555863. DOI: 10.19080/OROAJ.2019.13.555863
Abstract
Objectives: To describe the surgical technique and outcomes in patients with comminuted calcaneal fractures treated with the sinus tarsi approach using tibio-calcaneal distraction. Fractures were fixed with 1/3 tubular or anatomic plates.
Design: Case series
Setting: : Operating room and outpatient care center in hospital
Patients: From 2013-2016 fourteen cases of displaced calcaneal fractures (13 patients) were surgically treated using the sinus tarsi approach with tibio-calcaneal distraction. The fractures were Sanders Type 4 (9), Sanders Type 2B (2), Sanders Type 3BC (2), and Sanders 3AB (1).
Intervention: Surgical treatment using the sinus tarsi approach with tibio-calcaneal distraction. Either a 1/3 tubular (10) or calcaneal (4) plate was used for fixation.
Main Outcome Measures: Clinical and radiological follow-up visits (6, 12, and 36 weeks) in addition to annual postoperative assessments using the American Orthopedics Foot and Ankle Society (AOFAS) scale and the modified ROWE score.
Results: Anatomical reduction of the subtalar joint was achieved for all fracture types and the Bohler’s angle was restored in 71% (10/14) of cases. No skin necrosis or wound healing problems occurred. The mean operation time was 57 minutes (±13.8, range 25-95). At the annual follow-up visit, the mean AOFAS score was 85 (±10.5, range 68-100) and the modified Rowe score was 86 (±12, range 65-100).
Aim: The purpose of this study was to compare tightrope (Arthrex) technique in syndesmotic injury versus 3.5 mm tricortical trans-syndesmotic screw in terms of accuracy and syndesmosis reduction.
Conclusion: The sinus tarsi approach resulted in anatomical restoration in 71% of the cases. No notable differences in clinical and radiological parameters were found between the plate types. Operation time was short, complications were few, and clinical outcomes were favorable.
Level of Evidence:Therapeutic – Level IV
Keywords: Calcaneal fractures; extensive L-shaped approach; Sinus tarsi approach; Intraarticular fractures
Introduction
Calcaneal fractures are rare and account for approximately 2% of all skeletal fractures [1]. However, they are the most common type of tarsal fracture (60%) [2,3]. The injury mechanism is typically associated with an axial load from high energy trauma, such as falls from a height or motorcycle accidents.1 The prognosis for complete recovery is poor, with complication rates as high as 58% [4-6]. The most frequently reported complications are delayed wound healing, postoperative skin necrosis, and malunion due to insufficient intraoperative anatomical reduction [7-9]. Surgical outcomes are correlated with fracture severity and the quality of articular reduction [10].
The two main surgical approaches used to treat this condition are
i. an invasive technique using lateral L-shaped access, [11-16] and
ii. a minimally invasive technique using the sinus tarsi approach [17].
Despite a high rate of soft tissue complications associated with the extended lateral L-shaped approach, it continues to be the most widely used technique over the last decade [18-21]. The L-shaped soft tissue flap created when using this approach contains the lateral calcaneal branch of the peroneal artery. Consequently, surgeons must take care not to damage the sural nerve. Although this approach provides good visualization of the lateral wall and posterior facet, [22] it has the potential to cause considerable tissue damage, wound healing problems, and skin necrosis.
In recent years, a growing interest in the sinus tarsi approach has been reflected in the increased amount of publications describing its use. Two meta-analyses published in 2017 by Yoa et al. [8] and Zhang et al. [23] compared the sinus tarsi and the extensile lateral approaches. Most studies using the sinus tarsi approach included a calcaneal plate for fixation. The primary aim of this case series was to describe our experience with the sinus tarsi approach in combination with reduction using the AO distractor, and to assess the accompanying medical outcomes (e.g., wound healing and fracture reduction). In the majority of the cases, fixation was done with a 1/3 tube plate.
Methods
Patients
Between October 2013 and October 2016, 16 displaced calcaneal fractures (one bilateral) were treated at our institution. Fourteen of these cases (13 patients) were treated using the sinus tarsi approach with tibio-calcaneal distraction. According to our institution’s policy, indications for an “open reduction-internal fixation” procedure include the following: displaced tongue fractures, large extra-articular fractures (>1 cm) with detachment of Achilles tendon and/or > 2 mm displacement, Sanders Type II and III fractures, anterior process fractures with >25% involvement of calcaneocuboid joint, and displaced sustentaculum fractures [23]. Excluded from this case series were two patients with duckbill fractures without articular involvement who were treated with compression screws. Patient characteristics and fracture types are outlined in Table 1. The mean age of the patients was 48 years (±19.5; range 13-71) and mean body mass index was 23.8 (±4.1, range 17.6-32.8). Ten of the fourteen fractures resulted from high energy trauma.
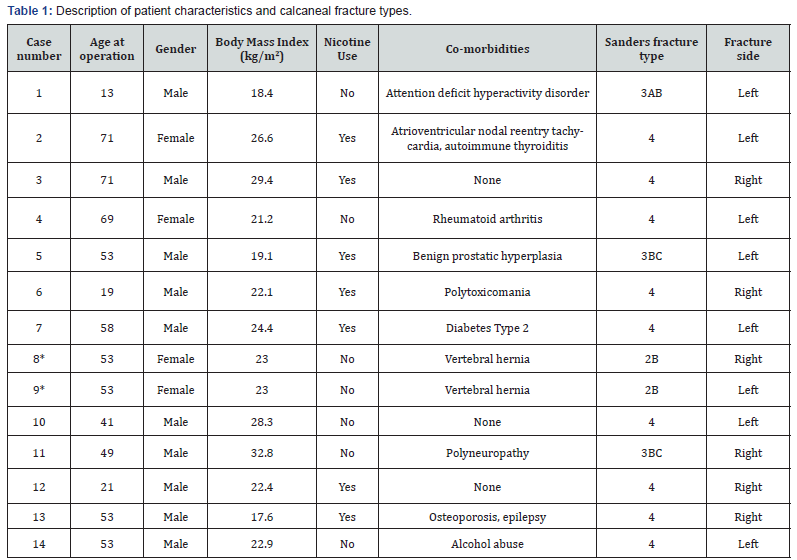
*Patient with bilateral calcaneal fractures.
Operative Technique
Ideal positioning for this type of operation is lateral with application of a high tourniquet. Perioperative use of an additional femoral catheter decreases the need for pain medication during the first few postoperative days. Surgical preparation included marking the anatomy on the skin, including the expected course of the sural nerve (Figure 1). A 5-cm incision started from the tip of the lateral malleolus to the center of the calcaneocuboid joint. The peroneal tendons were retained distally in order to enter the sinus area proximally. If the calcaneocuboid joint was involved, the fascia of the short extensor muscle was split at its origin and dissected to expose the joint and fracture margins. This previous step is not necessary for fractures that do not involve the anterior process. Therefore, the skin incision can be shorter. During soft tissue dissection, we used blunt skin retractors to reduce diminution of local blood supply. To reach the subtalar joint, dissection of the sinus fat pad was performed. At this point, full exposure to the calcaneocuboid and subtalar joint, as well as the posterior facet, was achieved.
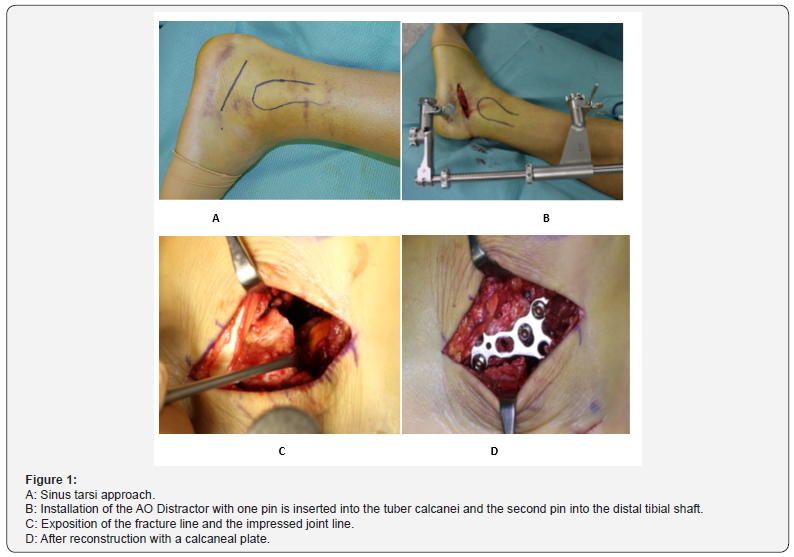

For plate insertion, distal dissection to the calcaneus body was often necessary and was done only fasciocutaneously. Caution was taken not to dissect too extensively since it has been associated with a higher risk of soft tissue complications. Although a variety of different plates are available for osteosynthesis of calcaneal fractures, we have found that the 1/3-tube plates (Synthes®, West Chester, PA, USA) reliably fix the reduced joint fragments to the calcaneal body. Anatomic calcaneal plates are larger and more difficult to insert through a small approach. Furthermore, the calcaneal plate covers more of the corpus, which requires a larger dissection for plate insertion. In patients with poor bone quality, we used the calcaneus plate 3.5mm (Synthes®, West Chester, PA, USA). Examples of each implant, including the postoperative radiological results, are illustrated in Figure 2.
After finishing the fasciocutaneous dissection for plate insertion, the AO-Distractor (Synthes®, West Chester, PA, USA) was applied to restore the Bohler’s angle and to assess anatomical reduction of the depressed joint fragments (Figure 1). A Schanz screw was inserted into the calcaneal tuberosity. The insertion point was carefully selected and evaluated under fluoroscopy to avoid inserting the screw into the fracture line. The second 5mm pin was inserted bi-cortically into the distal tibia shaft. The distractor was then fixed by connecting the two pins. When distraction has been performed, the subtalar joint might also needed to be reconstructed. To avoid overcorrection, the subtalar joint was fully exposed before restoring the Bohler’s angle. In our experience, distraction can be done under fluoroscopy. It not only restores angulation but also reduces fragments by ligamen to axis, especially of the tuberosity.
Postoperative Care
All patients underwent non-weightbearing postoperative care for 3 months. During this time, physiotherapy with ankle joint movement and drop-foot prophylaxis was performed. Further wound care and stitch removal following discharge from the hospital was conducted by the patient’s primary care physician.
Outcome Measurements
Clinical and radiological follow-up visits (6, 12, and 36 weeks) included assessments with the American Orthopedics Foot and Ankle Society (AOFAS) scale and the modified ROWE Score. Changes in the Bohler’s angle and intraarticular steps >2 mm were assessed by an independent radiologist. Additional longterm assessments (AOFAS and ROWE scores) were done at least one year postoperatively.
Results
Radiological Results
Most fractures were Sanders Type 4 (n=9). In addition, we treated two fractures (Sanders Type 2B), two Sanders Type 3BC and one Sanders 3AB fracture. In this case series, anatomical reduction of the subtalar joint and standard Bohler’s angle (normal range: 20-40 degrees) was possible in 10 (71%) cases. At the follow-up visits, a loss of Bohler’s angle of greater than 5 degrees was detected in one patient (Case 2). The mean postoperative Bohler’s angle was 27.5 degrees (±7.4, range 15- 40) and decreased to 25.7 degrees (±7.5, range 14- 37). The mean postoperative tibialcalcaneal angle was 39 degrees (±6.4, range 25- 50; normal range: 30-50). A displacement in the subtalar joint greater than 2 mm occurred in only one patient (Case 13). Fracture healing occurred in all cases. There were no notable differences between the 1/3-tube plate group and patients with calcaneal plate fixation techniques. Patient outcomes are presented in Table 2.
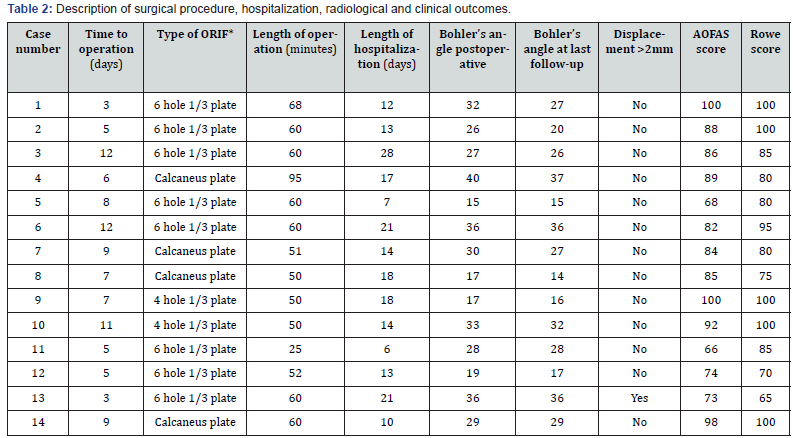
*Open reduction and internal fixation.
Clinical Results
The mean time to operation was 7 days (±2.8, range 3-12), and the mean operation time was 57 minutes (±13.8, range 25-95). Surgery was performed three days after trauma in the youngest patient in our cohort (case 1). The mean hospitalization time was 15 days (±5.5, range 7-28). At annual follow-up visits, the mean AOFAS score was 85 (±10.5, range 68-100) and modified Rowe Score was 86 (±12, range 65-100). Due to localized pain and swelling, implants were removed in two cases after complete fracture consolidation (7 and 13 months after initial surgery).
Complications
No wound healing disorders occurred. In two patients (cases 6 and 11), the tubular plate had to be removed due to localized residual pain and limitations in physical activities.
Discussion
Therapeutic options for displaced intra-articular calcaneal fractures continue to be debated in the literature [24,25] although most cases are eventually treated operatively. The functional outcome and patient satisfaction levels are reportedly better after surgery than non-operative therapy, particularly for younger patients [26]. Anatomic or near-anatomic reconstruction and restoration of the physiological calcaneal angulation play important roles in improved clinical results. When osteosynthesis is needed, the extended L-shaped lateral approach is often used [5,12-14]. This approach allows for good exposure of the corpus fragments. However, visualization of the subtalar and calcaneocuboid joint is often insufficient or associated with a large fasciocutaneous flap. Soft tissue necrosis, wound infections and bone necrosis due to lateral devascularization are common [13]. A variety of published reports describe minimally invasive techniques aimed at reducing damage to the blood supply, [10,27- 29] but these methods are also limited by insufficient exposition for anatomical reduction of the subtalar joint.
The sinus tarsi approach, which has been used in several studies, attempts to address the disadvantages of the L-shaped extended lateral approach [17,30-33]. Clinical results were comparable to those of the extended L-shaped approach but with less soft tissue complications [17,34,35]. Anatomic calcaneal plates are widely used, even with the less invasive sinus tarsi approach, and studies report good radiological and clinical outcomes. Due to the larger size of the anatomical plate, the approach must be enlarged and the periost dissected widely to ensure amble space for the plate. Based on our experience, smaller dissections are needed to insert tubular plates and blood supply damage can be minimized. With a minimally invasive approach, restoration of the Bohler angle may be easily performed using the AO distractor without access to the corpus of the calcaneus. Furthermore, findings from this case series indicate that the clinical and radiological outcomes do not differ from those following insertion of a calcaneal plate.
There are conflicting results in the medical literature about the effects of the length of time to surgery. In our case series, there was an average delay of 7 days, with a relatively wide range from 3 to 12 days. Kwon et al. [36] found increased wound complication rates in their cohort of patients who underwent sinus tarsi or percutaneous approach when the time span was greater than 7 days. The wound complication rate increased from 2% (0-7 days) to 8% (8-14 days). In the group with the extensile lateral approach, the rate did not change significantly in terms of the time to surgery (0-7 days 34%, 8-14 days 28%). However, the wound complication rate for the extensile lateral approach was significantly higher than the rate following the sinus tarsi approach. Nevertheless, a delay of surgery is associated with an increased amount of soft tissue swelling, which could have an influence on the development of complications.
A retrospective study of 65 calcaneal fractures conducted by Zhou et al. [37] showed a significantly lower wound necrosis rate in 28 fractures treated with a sinus tarsi approach and medial distraction. They used screws or micro plates for fixation. In the group undergoing a sinus tarsi approach, there was only one case of wound necrosis (4%) compared to two superficial infections (7%) and three cases of partial flap necrosis (11%) in the extended lateral approach group. In a prospective, randomized multicenter study, Basile et al. [38] compared the extended lateral approach with the sinus tarsi approach and distraction with a Schanz screw in the posterior tuberosity. Only one case of wound necrosis was found in the extended lateral approach group (7.9%), which was not statistically significant. They found no significant differences in the quality of reduction or the Bohler`s angle. Scott et al. [39] investigated radiological outcomes after reduction with a sinus tarsi approach in 39 displaced calcaneal fractures. The mean Bohler`s angle improved from 7.7 to 25.5 degrees, without relevant articular step-off. There was one deep wound infection and two cases of superficial wound dehiscence at the posterior apex wound. There were no complications at the incision site.
Park et al. [40] retrospectively reviewed 47 cases of calcaneal fractures treated with sinus tarsi approach and percutaneous screw fixation. They combined allogenous cancellous bone chips and a demineralized bone matrix to support the restored joint line. Sanders IV fractures were excluded from the study due to the difficulty of achieving the amount of visualization needed for the open reduction. They found 3 minor soft tissue complications, but no cases required revision. In their case series, the mean restoration of the Bohler’s angle was 71.6%.
Wang et al. [41] treated 18 patients with calcaneal fractures (14 Sanders Type II and 4 Sanders Type III) by using the sinus tarsi approach and a custom designed combined plate. The titanium plate has two mutually independent fixed arms and includes up to 6 locking screws. It was developed to create triangular support of the calcaneus using locking screws and to avoid extensive soft tissue damage. No wound healing problems occurred in their patient cohort.
We also believe that the standard calcaneal locking plates require extensive space and too often result in soft tissue damage for placement, even when using the minimally invasive sinus tarsi approach. It is our opinion that a locking screw system is not necessary. With the Bohler’s angle and the calcaneal joint line restored, a simple 1/3 tube plate and conventional screws provide sufficient stability. In our case series, the postoperative Bohler’s angle loss was small, which was comparable to findings from studies with calcaneal locking plates. Given that the number of patients in our case series was limited due to the low incidence of these fracture types, we recommend further investigations into the effectiveness of these approaches in combination with various implants.
Conclusion
In our case series, the sinus tarsi approach in combination with external distraction was a safe surgical procedure for the treatment of calcaneal fractures. It provided good visibility of the joint, and achieved restoration of the Bohler’s angle and the talonavicular joint surface. Moreover, there were no wound healing disorders. We believe the use of a calcaneal plate is not necessary in patients with normal bone quality and a short tubular plate is sufficient for joint restoration. Despite the limited number of cases in this series, we recommend further investigations and use of this procedure, particularly for those surgeons who prefer minimally invasive solutions.
References
- Bohl DD, Ondeck NT, Samuel AM, Diaz-Collado PJ, Nelson SJ, et al. (2016) Demographics, Mechanisms of Injury, and Concurrent Injuries Associated With Calcaneus Fractures: A Study of 14 516 Patients in the American College of Surgeons National Trauma Data Bank. Foot Ankle Spec 10(5): 402-410.
- Mitchell MJ, McKinley JC, Robinson CM (2009) The epidemiology of calcaneal fractures. Foot (Edinb) 19(4):197-200
- Griffin D, Parsons N, Shaw E 2014) Operative versus non-operative treatment for closed, displaced, intra-articular fractures of the calcaneus: randomised controlled trial. BMJ 349: g4483.
- Aldridge JM, Easley M, Nunley JA (2004) Open calcaneal fractures: results of operative treatment. J Orthop Trauma 18(1): 7-11.
- Benirschke SK, Kramer PA (2004) Wound healing complications in closed and open calcaneal fractures. J Orthop Trauma 18(1): 1-6.
- Wiersema B, Brokaw D, Weber T, Psaradellis T, Panero C, et al. (2011) Complications associated with open calcaneus fractures. Foot Ankle Int 32(11): 1052-1057.
- Silva LC, Heck JM, Guerra MT (2017) Surgical treatment of intraarticular fractures of the calcaneus: comparison between flat plate and calcaneal plate. Rev Bras Ortop 52(1): 29-34.
- Yao H, Liang T, Xu Y, Gang Hou, Lulu Lv, et al. (2017) Sinus tarsi approach versus extensile lateral approach for displaced intraarticular calcaneal fracture: a meta-analysis of current evidence base. J Orthop Surg Res 12(1): 43.
- Folk JW, Starr AJ, Early JS (1999) Early wound complications of operative treatment of calcaneus fractures: analysis of 190 fractures. J Orthop Trauma 13(5): 369-372.
- Omoto H, Nakamura K (2001) Method for manual reduction of displaced intra-articular fracture of the calcaneus: technique, indications and limitations. Foot Ankle Int 22(11): 874-879.
- Benirschke SK, Sangeorzan BJ (1993) Extensive intraarticular fractures of the foot. Surgical management of calcaneal fractures. Clin Orthop Relat Res 292: 128-134.
- Gould N (1984) Lateral approach to the os calcis. Foot Ankle 4(4): 218- 220.
- Letournel E (1993) Open treatment of acute calcaneal fractures. Clin Orthop Relat Res 290: 60-67.
- Zwipp H, Tscherne H, Thermann H, Weber T (1993) Osteosynthesis of displaced intraarticular fractures of the calcaneus. Results in 123 cases. Clin Orthop Relat Res 290: 76-86.
- Eastwood DM, Langkamer VG, Atkins RM (1993) Intra-articular fractures of the calcaneum. Part II: Open reduction and internal fixation by the extended lateral transcalcaneal approach. J Bone Joint Surg Br 75(2): 189-195.
- Freeman BJ, Duff S, Allen PE, Nicholson HD, Atkins RM, et al. (1998) The extended lateral approach to the hindfoot. Anatomical basis and surgical implications. J Bone Joint Surg Br 80(1): 139-142.
- Weber M, Lehmann O, Sagesser D, Krause F (2008) Limited open reduction and internal fixation of displaced intra-articular fractures of the calcaneum. J Bone Joint Surg Br 90(12): 1608-1616
- Bridgman SA, Dunn KM, McBride DJ, Richards PJ (2000) Interventions for treating calcaneal fractures. Cochrane Database Syst Rev 2: CD001161.
- Randle JA, Kreder HJ, Stephen D, Williams J, Jaglal S, et al. (2000) Should calcaneal fractures be treated surgically? A meta-analysis. Clin Orthop Relat Res 377: 217-227.
- Bajammal S, Tornetta P, Sanders D, Bhandari M (2005) Displaced intraarticular calcaneal fractures. J Orthop Trauma 19-5: 360-364.
- Gougoulias N, Khanna A, McBride DJ, Maffulli N (2009) Management of calcaneal fractures: systematic review of randomized trials. Br Med Bull 92:153-167.
- Kiewiet NJ, Sangeorzan BJ (2017) Calcaneal fracture management: extensile lateral approach versus small incision technique. Foot Ankle Clin 22(1): 77-91.
- Zhang F, Tian H, Li S, Liu B, Dong T, et al. (2017) Meta-analysis of two surgical approaches for calcaneal fractures: sinus tarsi versus extensile lateral approach. ANZ J Surg 87(3): 126-131.
- Jarvholm U, Korner L, Thoren O, Wiklund LM (1984) Fractures of the calcaneus. A comparison of open and closed treatment. Acta Orthop Scand 55(6): 652-656.
- Giachino AA, Uhthoff HK (1989) Intra-articular fractures of the calcaneus. J Bone Joint Surg Am 71(5): 784-787.
- Buckley R, Tough S, McCormack R, Pate G, Leighton R, et al. (2002) Operative compared with nonoperative treatment of displaced intraarticular calcaneal fractures: a prospective, randomized, controlled multicenter trial. J Bone Joint Surg Am 84-A(10): 1733-1744.
- Arastu M, Sheehan B, Buckley R (2014) Minimally invasive reduction and fixation of displaced calcaneal fractures: surgical technique and radiographic analysis. Int Orthop 38(3): 539-545.
- Magnan B, Bortolazzi R, Marangon A, Marino M, Dall’Oca C, et al. (2006) External fixation for displaced intra-articular fractures of the calcaneum. J Bone Joint Surg Br 88(11): 1474-1479.
- Stulik J, Stehlik J, Rysavy M, Wozniak A (2006) Minimally-invasive treatment of intra-articular fractures of the calcaneum. J Bone Joint Surg Br 88(12): 1634-1641.
- Ebraheim NA, Elgafy H, Sabry FF, Freih M, Abou-Chakra IS (2000) Sinus tarsi approach with trans-articular fixation for displaced intraarticular fractures of the calcaneus. Foot Ankle Int 21(2): 105-113.
- Femino JE, Vaseenon T, Levin DA, Yian EH (2010) Modification of the sinus tarsi approach for open reduction and plate fixation of intraarticular calcaneus fractures: the limits of proximal extension based upon the vascular anatomy of the lateral calcaneal artery. Iowa Orthop J 30: 161-167.
- Mostafa MF, El-Adl G, Hassanin EY, Abdellatif MS (2010) Surgical treatment of displaced intra-articular calcaneal fracture using a single small lateral approach. Strategies Trauma Limb Reconstr 5(2): 87-95.
- Shabat S, Early JS (2005) A minimal subtalar approach to fix a calcaneal fracture and a lateral process of talus fracture in a diabetic obese patient. Orthopedics 28(11): 1373-1374.
- Kikuchi C, Charlton TP, Thordarson DB (2013) Limited sinus tarsi approach for intra-articular calcaneus fractures. Foot Ankle Int 34(12): 1689-1694.
- Kline AJ, Anderson RB, Davis WH, Jones CP, Cohen BE (2013) Minimally invasive technique versus an extensile lateral approach for intraarticular calcaneal fractures. Foot Ankle Int 34(6): 773-780.
- Kwon JY, Guss D, Lin DE, Abousayed M, Jeng C, et al. (2015) Effect of delay to definitive surgical fixation on wound complications in the treatment of closed, intra-articular calcaneus fractures. Foot Ankle Int 36(5): 508-517.
- Zhou HC, Yu T, Ren HY, Li B, Chen K, et al. (2017) Clinical comparison of extensile lateral approach and sinus tarsi approach combined with medial distraction technique for intra-articular calcaneal fractures. Orthop Surg 9(1): 77-85.
- Basile A, Albo F, Via AG (2016) Comparison between sinus tarsi approach and extensile lateral approach for treatment of closed displaced intra-articular calcaneal fractures: a multicenter prospective study. J Foot Ankle Surg 55(3): 513-521.
- Scott AT, Pacholke DA, Hamid KS (2016) Radiographic and CT assessment of reduction of calcaneus fractures using a limited sinus tarsi incision. Foot Ankle Int 37(9): 950-957.
- Park J, Che JH (2017) The sinus tarsi approach in displaced intraarticular calcaneal fractures. Arch Orthop Trauma Surg 137(8): 1055- 1065.
- Wang Z, Wang XH, Li SL, Tang X, Fu BG, et al. (2016) Minimally invasive (sinus tarsi) approach for calcaneal fractures. J Orthop Surg Res 11(1): 164.






























