What is the Effective Technique for Syndesmotic Stabilization Tight Rope or Screw?
Elsayed Shaheen*
Orthopedic Department, Al-Azhar university, Egypt
Submission: December 01, 2018;Published: December 17, 2018
*Corresponding author: Elsayed Shaheen, Orthopedic Department, Al-Azhar university, Egypt .
How to cite this article: Elsayed Shaheen. What is the Effective Technique for Syndesmotic Stabilization Tight Rope or Screw?. Ortho & Rheum Open Access J 2018; 13(3): 555862. DOI: 10.19080/OROAJ.2018.13.555862.
Abstract
Background: Complex syndesmotic ankle injuries (SAI) require restoration of normal biomechanics aiming to minimize expected complications.
Aim: The purpose of this study was to compare tightrope (Arthrex) technique in syndesmotic injury versus 3.5 mm tricortical trans-syndesmotic screw in terms of accuracy and syndesmosis reduction.
Methods: prospective clinical for twenty-two patients presented by SAI randomly allocated into two groups. Group A was fixed using tightrope technique, while group B fixed using 3.5 mm trans-syndesmotic cortical screw. All patients underwent clinical examination, radiological investigations, functional evaluation using American Orthopedic Foot and Ankle Society (AOFAS); preoperative, 6th, 12th and 17th months as follow up. SPSS was used for statistical analysis.
Results: The mean participants’ age was (39.4±3.7) years and mean follow up was (15.7±3.4) months. The study showed that AOFAS scores were better in Tightrope group (P value < 0.018); with faster weight bearing (4.9 weeks), which required 6 weeks in tricortical trans-syndesmotic screw group. Along follow up period, tightrope group was shown higher range of motion (ROM) than group B (P value < 0.042). Moreover, tightrope group not required secondary implant removal. Conclusion: Tightrope technique provides alternate safe, efficient SAI fixation and advantageous early weight bearing, plus long-term stability that radiologically confirmed as well shown higher AOFAS scores.
Keywords: Tightrope; Screw fixation; Syndesmosis; AOFAS scores; Ankle stability
Abbrevations: SAI: Syndesmotic Ankle Injuries; AOFAS: American Orthopedic Foot and Ankle Society; ROM: Range of Motion
Introduction
SAI may occur in 10 up to 15% in patients presented with ankle fractures commonly associated with pronated, external rotated ankle injuries, [1] or Weber C fractures, and around 20% of ankle fractures require surgical stabilization [2]. Most misdiagnosed SAI complicated by chronic ankle pain, rapid degeneration, functional disabilities, instability and latent diastasis [3,4]. Evidence gap still prove a specific and standard care for SAI; fixation technique, screws size and numbers of cortices and weight bearing progression. On the other hand, drawbacks of SAI fixation presented some complications including limited ankle mobility, delayed weight bearing, risk of screw breakage and necessity of its removal [5,6], which may complicate by wound infection, screw breakage or syndesmotic diastasis [7].
Numerous studied confirmed that tightrope SAI fixation is a minimal invasive technique, which allows micro syndesmosis motion throughout reduction with least pain, and longer stability that permits early patients mobility, weight bearing and faster return to work. Furthermore, it was advised for osteoporosis (snowshoe, hold on cortical bone), while screw fixation may lead to cut out due to low screw breakage risk or need for its removal [8,9]. Otherwise, loose tightrope may lead to later syndesmosis diastasis [10]. Recently, tightrope technique was highly recommended for SAI, as well for isolated syndesmosis separations. The purpose of the current study was to compare tightrope procedure (Arthrex, Naples, FL, USA) versus 3.5 mm tricortical trans-syndesmotic screw in terms of accuracy and adequate syndesmosis reduction.
Patients and Methods
Twenty-two patients were management in this prospective study from February 2016 to July 2017. The eligible patients mean ages was (39.4±3.7), were included if have SAI that are sustained distal tibiofibular (tibiofibular clear space “TFCS” >6 mm on A/P or mortise radiographs or tibiofibular overlap “TFOL” <6 mm on A/P radiographs or <1mm on mortise radiographs, or medial clear space “MCS” >5mm on A/P radiographs) [11], syndesmotic diastasis with or without ankle fractures less than 4 weeks. Patients were excluded if they had polytrauma or open fracture, open growth plates, uncontrolled diabetes mellitus and neuropathic arthropathy.
Each patient had signed a written informed consent then all patients were randomized allocated into two groups. Every patient underwent complete clinical examination and preoperative, 6th, 12th and 17th months follow up specific radiological investigations; functional evaluation using American Orthopedic Foot and Ankle Society (AOFAS), total 100 points divided into nine items grouped into three categories; (pain: 40 points, functional abilities: 50 points, alignment) [12].
Tightrope Structure
Tightrope implant (Arthrex, Naples, FL, USA) consists of two-button construct (titanium or stainless steel), and two No.5 braided fibre suturing wire, when tensioned provide ankle mortise stability, where previous clinical trials reported its equivalent strength that improve clinical outcomes [13].
Surgical Procedures
Both tightrope and screw SAI fixation techniques were almost similar procedures, where tightrope used one device, but may augment by another one in highly unstable distal tibiofibular joint or screw technique used one tricortical screw. Open reduction and internal fixation of ankle fractures, almost syndesmotic diastasis reduced spontaneously. While, remaining diastasis were reduced primary by reduction clamp placed across ankle and compressed SAI then reduction maintained by the tightrope or screw which were inserted directly, through fibula or fibular plate`s hole, in case of fibular fracture.
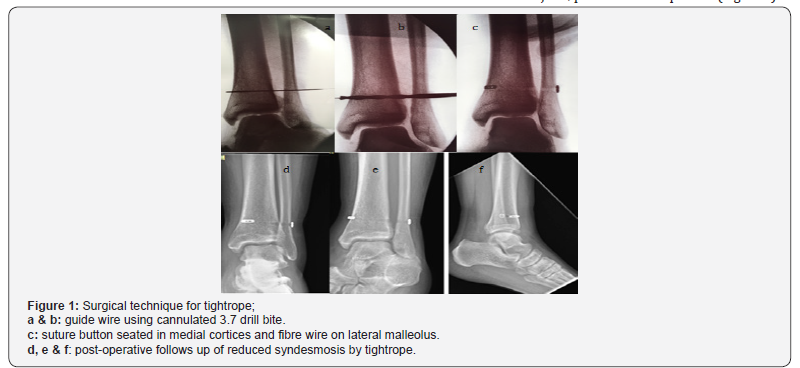
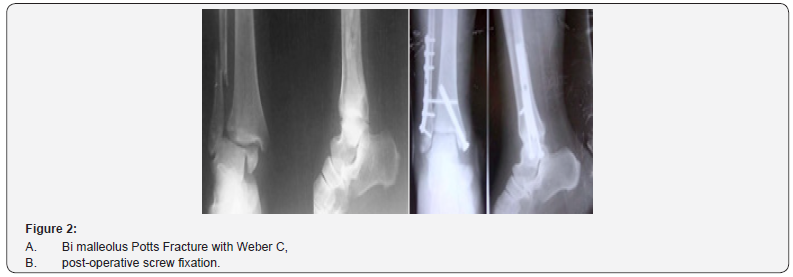
In tightrope fixation all fractures were stabilized prior to tightrope insertion. Once a plate fixed to distal fibula, one or more cortices screw holes (2-5 cm above tibial plat fond using 3.7 mm drill bit) used for tightrope. A guide wire using cannulated drill bite was recommended to confirm accurate drill positioning prior by fluoroscopy, guided suturing along drill holes to intact medial skin, where button seated direct on medial cortex that confirmed by C-arm. Flipping was done by transmitting medial pressure from the needle to fibre wire suture laterally then toggling the two pairs, which ensured endobutton flat seating preventing later losing. With reduction clamp in place, both ends of fibre wire tensioned on lateral side providing compression on buttons aiming to maintain syndesmosis reduction (Figure 1). In screw fixation; with ankle in neutral position used a 3.5 mm cortise screw was inserted into previously drilled 2.5 fibular hole 30° from posterior to anterior up to lateral tibial cortex, just inferior to inferior tibiofibular joint, parallel to tibial plafond (Figure 2).
Results
Twenty-two patients with syndesmotic disruption were management with tightrope or screw, the mean age was (39.4±3.7) years. There were 17 patients sustained ankle fractures; 9 patients presented Weber C fracture and 8 patients Weber B fracture, plus 5 patients have been diagnosed isolated syndesmosis diastasis (Table 1).
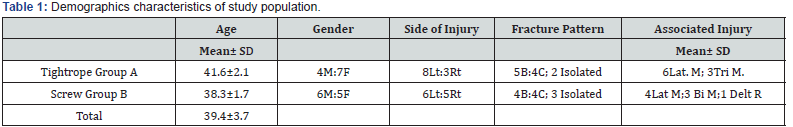
SD: Standard deviation; Lat M: Lateral Malleolus; Tri M: Trimalleolus; Bi M: Bimalleolus; Delt R: Deltoid Repair
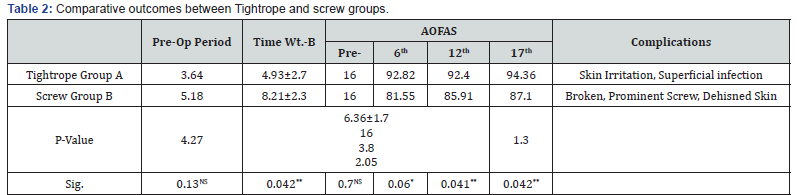
*: (P-value≤0.05). **: (P-value≤0.01).
Per-Op: Pre-Operative; TWt-B: Time to Weight Bearing; AOFAS: American Orthopedic Foot and Ankle Society; NS: Non-significant
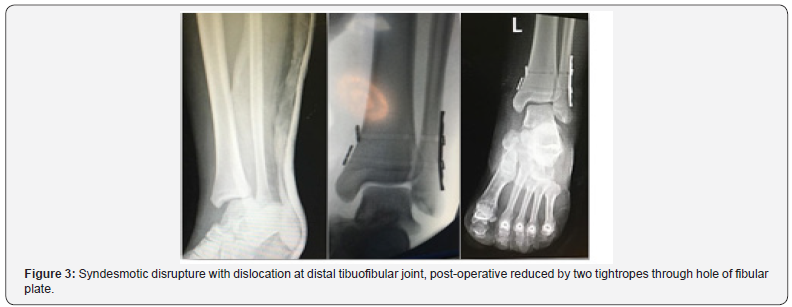
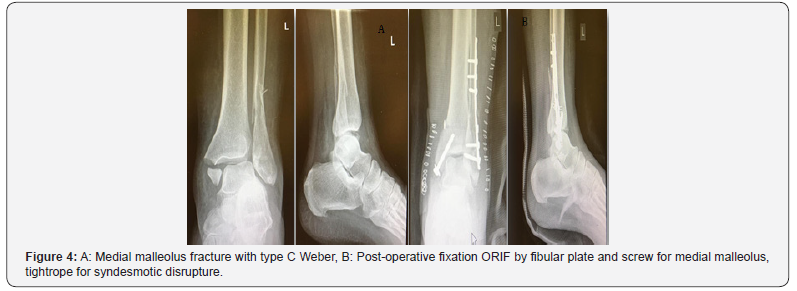
In tightrope group A, 6 patients presented by fracture lateral malleolus associated with syndesmosis diastases were spontaneously reduced post fracture fixation then tightrope inserted through fibular plate hole. Other 2 patients presented isolated syndesmosis disruption, and single tightrope was done. One case presented with complete torn syndesmotic diastasis with dislocation at distal tibiofibular joint so added another tight rope to restore ankle stability and augmented by small lateral plate without screws (Figure 3), two patients presented trimalleolar fracture and underwent medial malleolar screws and one tightrope done. Uneventful complications reported, unless one case had lateral side superficial infection and another one had a small stitch irritation on medial side (Table 2). There are two cases had been evaluated at 6th and 12th months follow up period but lost after that (Figure 4).
In screw group B, 3 patients presented isolated syndesmosis diastases managed by one screw tricortical insertion. Another 4 patients underwent standard fibula plate plus syndesmosis screw fixation. As well, 3 patients presented bimalleolar Potts fractures and medial malleolar fixation plus tricortical syndesmosis screw were done. Only one patient underwent deltoid repair (MCS > 5mm). Furthermore, complicated cases at follow up period were reported as, one patient underwent a large fragment removal due to prominent screw head, another one broken screw accidentally discovered throughout routine implant removal and that patient presented by intermittent lateral ankle pain (Table 2). Other patient was presented with dehisned wound and superficial infection after removed of screw.
The mean follow up average was (15.7±3.4) months, and AOFAS were significantly higher in tightrope group versus screw group (91:80; 93:83 and 94:86) by 6th, 12th and 17th months follow up, respectively (P value < 0.018). Average time delayed nonweight bearing 4.9 weeks (range .3.5-6W) versus 6Weeks (range4- 12W) in screw group (P value < 0.042), and routine screw removal after 8-12 weeks (Table 2). Finally, the study results shown that tightrope group had significantly better ROM (P value < 0.054) than screw group (P value < 0.018), (Table 3).
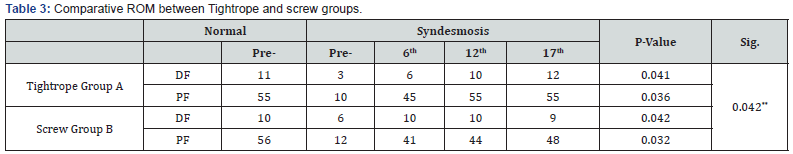
NS: Non-significant. **: (P-value≤0.01). DF: Dorsi flexion. PL: Planter flexion. Per: Pre-Operative.
Discussion
Tightrope stabilization of a syndesmotic injury has been shown as an alternative that has significant outcomes and is more physiological than standard screw techniques [14]. The dynamic flexible fixation of tight rope permits micro-movement of the distal tibiofibular joint, which provides better outcomes in terms of mobility, accelerated ligament healing, earlier return to full weight-bearing and returns of physical abilities, as well unnecessary implant removal [15].
The present study has been shown that tightrope technique provides long standing and accurate syndesmosis reduction, better mobility, plus faster functional abilities, with significantly higher in AOFAS scores, range of motion and full-time weight bearing when compared the screw group along the latest follow up period. Furthermore, the study reported minor complications about (18%) one case skin irritation at medial ankle side, and another case had superficial infection at lateral malleolus when compared with screw technique about (27%), broken screw, prominent head of screw and diastasis after removal of screw, especially within second intervention, while routine implant removal.
The present result coincide with, Thomes et al. [16] reported that tightrope technique permitted earlier weight bearing, and stated its safe, efficient and simple nature versus screw technique, which required second removal surgery. In terms of functional abilities, it was reported higher AOFAS in patients underwent tightrope fixation than screw technique [17,18]. Plus, tightrope fixation patients were permitted earlier weight bearing (4.1 weeks) with no need for further surgical interventions as reported by Naqvi et al. [19] in advance no loading failure or residual diastasis were reported even with accelerated full weight bearing [20-22].
Cottom et al. [23] also reported that it was accelerated early weight bearing in the tightrope group with no complication such as implant failure or removal was noted. Degroot et al. [18] demonstrated that shorter average time to full weight-bearing of 5.7 weeks using tightrope, with no complication of implant failure or residual displacement at a follow-up of 2years. On the other hand, in this study usage of second tight rope was occurring in highly unstable distal tibiofibular joint with improper fixation by single device. This agree with Naqvi et al. [19] usage of extra tightrope implant to gain accurate syndesmosis reduction was advised in 26% of population study and 75% as confirmed by DeGroot et al. [18] to prevent later enlarged tibial hole or implant subsidence or in case of oseolysis. This study was undertaken routine removal of syndesmotic screws range from 8-12 Weeks, however, did not occur routinely at tight rope group. Moreover, Schepers et al. [24] recommended no significant differences when elective screw removal or not, additionally routine screw removal procedure as second intervention, commonly associated with complication more than 20% with both recurrent diastases or wound infection risks [25], In contrary, tightrope implant removal was not required, even in case that will be minor invasive with no definite evidence reported, yet [26].
In same context with previous studies, screws placement level determines the protection period prior allowing patient to weight bearing that directly affects mobility in term of ROM [27]. Cottom et al. [23] demonstrated that tightrope technique has a valid, safe and least cost with low irritation, infection risks. They also recommended; performing of two suture buttons could also be more useful for in Weber C or comminuted fibular fractures. Furthermore, Klitzman et al. [28] confirmed tightrope permits more flexibility than screw technique through using suture button fixation, which was accelerated the physiological healing of syndesmosis. Moreover, Rigby and Cottom ensured that less invasive nature of tightrope technique provides advantageous ankle stability for rediastasis [29] than screw fixation, where the later had routine second intervention for implant removal by 8-12 weeks.
Storey et al. [30] determined potential the disadvantages of tightrope such as skin irritation by fibre wire, rediastasis loosening due to osteolytic reaction, are the most common complications. They has been recommended to remove the implant just in case of osteolysis [30]. The current study had some limitation those should be addressed in future clinical trials, which are small sample size with absence of control group, plus potential bias concerning clinical picture and radiological evaluation. Although satisfactory outcome were reported in all nine-patient treated by Tightrope stabilization of the distal tibiofibular joint does not appear to be a major problem this study has shown that. Finally, Tightrope and screw fixation of the injured syndesmosis provided effective reduction of the syndesmosis, each with its advantages and disadvantages [31].
Conclusion
The dynamic stabilization or flexible fixation was done by tightrope provides an alternate to static fixation done by syndesmotic screw features a lot of advantages besides its complications. It permits remarkable earlier return to work with longer efficient syndesmosis reduction and better stability, as well preventable risks and correctable complications. In screw fixation group achieve rigid fixation with lack of mobility at syndesmosis to achieve ligament healing, however hardware removed had done routinely at a later date with minor complications attributable such as broken, prominent screw and superficial infection.
Acknowledgment
I cordially appreciate the helps that provided by Dr. Taha Elsaman consultant of orthopedic and sport injuries at Saudi- German Hospital, Jeddah, Saudi Arabia. I would like to express MY gratitude for her help in reviewing and verifying this paper.
Conflict of Interest
No conflict of interest.
References
- Jensen SL, Andresen BK, Mencke S, Nielsen PT (1998) Epidemiology of ankle fractures: A prospective population-based study of 212 cases in Aalborg, Denmark. Acta Orthop Scand 69(1): 48-50.
- Dattani R, Patnaik S, Kantak A, Srikanth B, Selvan TP (2008) Injuries to the tibiofibular syndesmosis. J Bone Joint Surg Br 90(4): 405-410.
- Kim JH, Gwak HC, Lee CR, Choo HJ, Kim JG, et al. (2016) A comparison of screw fixation and suture-button fixation in a Syndesmosis injury in an ankle fracture. J Foot Ankle Surg 55(5): 985-990.
- Schepers T (2012) Acute distal tibiofibular syndesmosis injury: a systematic review of suture-button versus syndesmotic screw repair. Int Orthop 36(6): 1199-1206.
- Hodgson P and Thomas R (2011) Avoiding suture knot prominence with suture button along distal fibula: technical tip. Foot Ankle Int 32(9): 908-909.
- Soin SP, Knight TA, Dinah AF, Mears SC, Swierstra BA (2009) Suturebutton versus screw fixation in a syndesmosis rupture model: a biomechanical comparison. Foot Ankle Int 30(4): 346-352.
- Andersen MR, Frihagen F, Madsen JE, Figved W (2015) High complication rate after syndesmotic screw removal. Injury 46(11): 2283-2287.
- Laflamme M, Belzile EL, Bédard L, Van Den Bekerom MPJ, Glazebrook M, et al. (2015) A prospective randomized multicenter trial comparing clinical outcomes of patients treated surgically with a static or dynamic implant for acute ankle syndesmosis rupture. J Orthop Trauma 29(5): 216-223.
- Xu G, Chen W, Zhang Q, Wang J, Su Y, et al. (2013) Flexible fixation of syndesmotic diastasis using the assembled bolt-tightrope system. Scand J Trauma Resusc Emerg Med 21(1): 71.
- Treon K, Beastall J, Kumar K, Hope M (2011) Complications of ankle syndesmosis stabilisation using a tightrope. J Bone Joint Surg Br 93: 62-72.
- Amendola A, Williams G, Foster D (2006) Evidence-based approach to treatment of acute traumatic syndesmosis (high ankle) sprains. Sports Med Arthrosc 14(4): 232-236.
- Kitaoka HB, Alexander IJ, Adelaar RS, Nunley JA, Myerson MS, et al. (1994) Clinical rating systems for the ankle-hindfoot, mid-foot, hallux and lesser toes. Foot Ankle Int 15(7): 135-149.
- Arthrex Inc. TightRope.
- Cottom JM, Hyer CF, Philbin TM, Berlet GC (2008) Treatment of syndesmotic disruptions with the Arthrex Tightrope: a report of 25 cases. Foot Ankle Int 29(8): 773-780.
- Willmott HJ, Singh B, David LA (2009) Outcome and complications of treatment of ankle diastasis with tightrope fixation. Injury J 40(11): 1204-1206.
- Thornes B, Walsh A, Hislop M, Murray P, O’Brien M (2003) Sutureendobutton fixation of ankle tibio-fibular diastasis: a cadaver study. Foot Ankle Int 24(2): 142-146.
- Coetzee J, Ebeling P (2009) Treatment of syndesmoses disruptions: a prospective, randomized study comparing conventional screw fixation vs TightRope® fiber wire fixation-medium term results. S Afr Orthop J 8: 32-37.
- Degroot H, Al-Omari AA, El Ghazaly SA (2011) Outcomes of suture button repair of the distal tibiofibular syndesmosis. Foot Ankle Int 32(3): 250-256.
- Naqvi GA, Shafqat A, Awan N (2012) Tightrope fixation of ankle syndesmosis injuries: Clinical outcome, complications and technique modification. Injury 43(6): 838-842.
- Guohui X, Chen W, Zhang Q, Wang J, Su Y, et al. (2013) Flexible fixation of syndesmotic diastasis using the assembled bolt-tightrope system. Scandinavian J Tra, Res Emer Med 21: 71.
- http://www.sjtrem.com/content/21/1/7.
- Thornes B, Shannon F, Guiney AM, Hession P, Masterson E (2005) Suture-button syndesmosis fixation: accelerated rehabilitation and improved outcomes. Clin Orthop Relat Res 431: 207-212.
- Hohman DW, Affonso J, Marzo JM, Ritter CA (2011) Pathologic tibia/ fibula fracture through a suture button screw tract: case report. Am J Sports Med 39(3): 645-648.
- Cottom JM, Hyer CF, Philbin TM, Berlet GC (2009) Transosseous fixation of the distal tibiofibular Syndesmosis: comparison of an Interosseous suture and Endobutton to traditional screw fixation in 50 cases. J Foot Ankle Surg 48(6): 620-630.
- Schepers T (2011) To retain or remove the syndesmotic screw: a review of literature. Arch Orthop Trauma Surg 131(7): 879-883.
- Hsu YT, Wu CC, Lee WC, Fan KF, Tseng IC, et al. (2011) Surgical treatment of syndesmotic diastasis: emphasis on effect of syndesmotic screw on ankle function. Int Orthop 35(3): 359-364.
- Walley KC, Hofmann KJ, Velasco BT, Kwon JY (2017) Removal of hardware after syndesmotic screw fixation: a systematic literature review. Foot Ankle Spec 10(3): 252-257.
- Dingemans SA, Rammelt S, White TO, Goslings JC, Schepers T (2016) Should syndesmotic screws be removed after surgical fixation of unstable ankle fractures? A systematic review. Bone Joint J 98(B): 1497-1504.
- Klitzman R, Zhao H, Zhang LQ, Strohmeyer G, Vora A (2010) Suture button versus screw fixation of the syndesmosis: a biomechanical analysis. Foot Ankle Int 31(1): 69-75.
- Rigby RB, Cottom JM (2013) Does the Arthrex Tight Rope® provide maintenance of the distal tibiofibular syndesmosis? A 2-year follow-up of 64 TightRopes® in 37 patients. J Foot Ankle Surg 52: 563-567.
- Storey P, Gadd RJ, Blundell C, Davies MB (2012) Complications of suture button ankle syndesmosis stabilization with modifications of surgical technique. Foot Ankle Int 33(9): 717-721.






























