Pectoralis Major and Delto-Pectoral Side by Side Flap for Large Skin Defect in Neck-Initial Experience with a Modified Method
Gupta Dinesh1, Gupta Shalini2, Shukla Deepak3, Sharma Richa4 and Sharma Vijay5*
1Department of Oncosurgery, India
2Department of Radiology, India
3Department of Medical Oncology, India
4Department of Community Medicine, India
5Department of Gastroenterology, India
Submission: May 04, 2018;Published: July 06, 2018
*Corresponding author: Dr. Richa Sharma, Department of Community Medicine, Regional Institute of Health, Medicine, Research, Indira colony, Bani Park, Jaipur, India, Email: drrichas@gmail.com
How to cite this article: Gupta D, Gupta S, Shukla D, Sharma R, Sharma V. Pectoralis Major and Delto-Pectoral Side by Side Flap for Large Skin Defect in Neck-Initial Experience with a Modified Method. Open Access J Surg. 2018; 9(4): 555766. DOI: 10.19080/OAJS.2018.09.555766.
Abstract
Free flaps are the first choice nowadays for reconstruction of large skin defect in the neck after Radical Neck Dissection. But few options are available after the failure of a free flap. Another free flap is an ideal option if possible but ruled out in our case because of non-availability of recipient’s vessels. Local rotation flaps are next best option after free flaps to cover large skin defects in the neck. Pectoralis Major Muscle flap and Delto-pectoral flap have been used for long in the reconstruction of head and neck malignancies. In our case, both these flaps were inadequate singly in width to cover the skin defect. So, we devised a unique strategy to cover the skin defect with these flaps in a way that both these flaps were used side by side to cover the half of skin defect. This technique has not been mentioned in literature before.
Keywords: Pectoralis Major and Delto-pectoral side by side flap; Pectoralis Major Muscle flap; Delto-pectoral flap; Reconstruction of skin defect in the neck
Introduction
We present here a case of large skin defect in the neck after extended RND. It was a case of the second neck with unknown primary, post Neoadjuvant Chemotherapy. The patient had a partial response to Chemotherapy. Surgery (Radical Neck Dissection (RND) with reconstruction) was planned. Extended RND was done followed by Antero-lateral Thigh (ALT) free flap reconstruction. Somehow ALT free flap could not survive. ALT free flap had to be removed with the need for a cover of large skin defect with another flap.
Options available for reconstruction
Best option available in this situation is another free flap (either ALT free flap from other leg or any other free flap) but could not be done because of non-availability of good recipient vessels in the neck because of previous surgery. So, the option of another free flap ruled out. Though a second free flap could still be done with anastomosis to vessels on the contralateral side of the neck.Next, the best option available is local rotation flap with large skin cover. Option available is Latisimmus Dorsi (LD) myocutaneous flap, Trapezius myocutaneous flap, Pectoralis Major Muscle (PMM) flap, Deltopectoral (DP) flap, etc.LD myocutaneous flap was not a good option because though it would provide a large muscle flap to cover the defect but has a limitation in the availability of size of skin paddle. A large skin paddle with bulky LD muscle flap will be difficult to deliver beneath the clavicle and would also require an SSG at back with difficulty in healing of SSG over back because of constant movement in that area. This surgery would have extended the field of surgery to back with associated difficulty in lying in prone position. Also, in our case, LD myocutaneous flap would fall short of the upper end of skin defect.
A Trapezius myocutaneous flap was also a good option but ruled out in our case because of non-availability of vessels to trapezius muscle because of previous surgery. Other local rotation flaps like a scapular flap, supraclavicular flap in the vicinity were also ruled out because of the same reason.A DP flap is an option but had a limitation of the size of skin (width) available. PMM Myocutaneous flap also had a limitation of the size of skin paddle available. PM Muscle only flap with SSG over raw surface could be applied but the width of Pectoralis Major Muscle was not sufficient to cover the defect in our case.
How we manage the case
We decided to cover the defect with PMM + DP flap but although both the flaps were good enough in length vertically to cover the defect, they were insufficient singly to cover the defect in width.So, we did a PMM+DP side by side flap wherein the PMM flap was used to cover the lateral half of skin defect and DP flap was used to cover the medial half of skin defect. The margins of both the flaps in the center were stitched to each other by interrupted sutures to maintain negative suction in the wound. SSG was applied over the raw surface of PMM flap. The wound healed well with no complications(Figure 1).
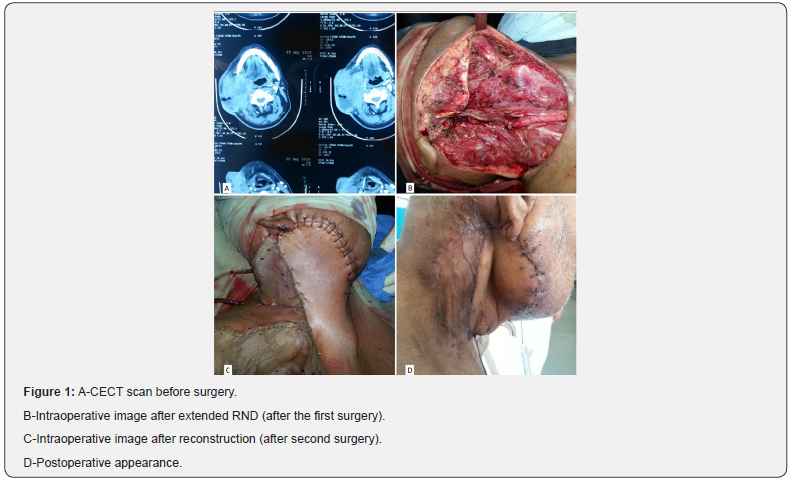
On searching the literature, we found that PMM and DP flap had been a workforce of H&N reconstructive surgeries for ages and have been used singly or in combination for long. The various combinations of PMM flap used for reconstruction in H&N are- PMM flap, PMM Myocutaneous flap, Pectoralis Major Osteomyocutaneous flap. The skin paddle of PMM has been used for either intraoral cover or for the cover of skin defect in the neck. The various combination of DP flap used for reconstruction in H&N is-DP skin flap alone for the cover of skin defect in the neck or in combination with PMM flap with PMM covering the intraoral defect and DP covering the neck skin defect.
But our reconstruction was unique in the sense that we have not found the use of PMM and DP flap side by side to cover a very large skin defect in the neck in search of the literature. The side by side PMM+DP flap is a good alternative for reconstruction of large neck skin defects because it avoids the surgeries and morbidities of the free flap on the thigh and of the back with LD myocutaneous flap.
Review of literature
Since its introduction by Ariyan in 1979, the pectoralis major myocutaneous flap (PMMF) has been a workhorse flap for the reconstruction of the head and neck defects for long. Advantages of this flap include its easy harvest, abundant soft tissue volume, large skin paddle, relative versatility, considerable reliability, and short operating time. However, its popularity in head and neck reconstruction decreased recently with the development of microvascular techniques and the wide use of free tissue transfers. Disadvantages of the PMMF include excessive bulk sometimes, thoracic wall deformity, partial necrosis of its skin paddle, functional impairment of the neck and shoulder and high incidence of complications. But it is still quite often used in developing countries with limited medical resources. Its role has shifted from a “workhorse flap” to a “salvage flap” in the era of free flaps. However, the role of the PMMF is irreplaceable, even though free flaps are more popular. It can safely be used not only as a “salvage flap” in cases with flap failure or complications (e.g. fistula and carotid rupture) but also as a primary procedure in patients who were predictably high-risk candidates for a free flap, in situations where bulky flaps are needed (e.g. total glossectomy reconstruction), and in cases where simultaneous protection of the major vessels of the neck is necessary.
Baliarsing et al.[1] in his review article has mentioned that for large skin defects, options available for reconstruction are free ALT flap, pedicled LD myocutaneous flap, and PMMC flap. Muyuan Liu et al. [2] in his study evaluated the role of PMMC flap for H&N defects in the era of free flaps. Akash G Anand et al. [3] in his article mentioned Reconstruction of Large Lateral Facial Defects Utilizing Variations of the Cervicopectoral Rotation Flap. Hanasono et al. [4] describe the impact of microsurgery in patients with advanced oral cavity cancers. They find that many patients have been reconstructed with local pedicled or regional flaps despite the availability of free tissue transfer.
Bibhuti B Nayak et al.[5]described a technique of reconstruction of the composite defect with the use of Single stage reconstructions in head and neck surgery using deltopectoral and pectoralis major myocutaneous flaps. RM Makkar et al. [6] in his study described the use of faciocervicopectoral flap for non-oncological cases of cheek reconstruction in gunshot and explosive injuries but defect in his study ranged from 3cm to 5cm and 3.5cm to 7cm in width and length respectively before debridement, with an increase in both dimensions by 0.5-1cm after debridement. The mean defect size was 3.93cm x 5.25cm.
KS Gopinath et al. [7] described the use of scapular fasciocutaneous flap for reconstruction of the posterior neck. Rampukar Chaudhary et al. [8] described the Use of pectoralis major myocutaneous flap for resurfacing the soft tissue defects of head and neck.It is concluded that PMMC is the highly versatile and reliable flap with an excellent vascularity, wide arc of rotation, large flap dimension, easy to harvest, economical and with minimal donor site morbidity and limited complications.
References
- Amresh S Baliarsing, Tushar S Thorat, Arunesh Gupta, Uday Bhat, Sanchit Garg, et al. (2013) Flap Selection in Head and Neck Cancer Reconstruction. Otorhinolaryngology Clinics: An International Journal May- 5(2): 63-76.
- Liu M, Liu W, Yang X, Guo H, Peng H (2017) Pectoralis Major Myocutaneous Flap for Head and Neck Defects in the Era of Free Flaps: Harvesting Technique and Indications. Sci Rep 7: 46256.
- Anand AG, Amedee RG, Butcher RB (2008) Reconstruction of Large lateral Facial Defects Utilizing Variations of the Cervicopectoral Rotation Flap. Ochsner J 8(4): 186-190.
- Hanasono MM (2014) Reconstructive Surgery for Head and Neck Cancer Patients. Adv Med 2014: 795483.
- Nayak BB, Nilamani M (2012) Single stage reconstructions in head and neck surgery using deltopectoral and pectoralis major myocutaneous flaps. Indian J Plast Surg 45(1): 151-153.
- Makkar RM (2013) The faciocervicopectoral flap for non-oncological cases of cheek reconstruction. Ann R Coll Surg Engl 95(6): 397-400.
- Gopinath KS, Chandrashekar M, Vijaya Kumar M, Bhargava A (1993) The scapular fasciocutaneous flap: a new flap for reconstruction of the posterior neck. British Journal of Plastic Surgery 46: 508-510.
- Chaudhary R, Akhtar MS, Bariar LM, Khurram MF (2014) Use of pectoralis major myocutaneous flap for resurfacing the soft tissue defects of head and neck. Journal of Orofacial Sciences 6(2): 88-93.






























