Papillary Hidradenoma of Vulva: A Rare Case Presentation
Kafil Akhtar1, Mohd Rafey2, Rana K Sherwani 1 and Zehra Mohsin1*
1Professor, Department of Pathology and Obstetrics & Gynaecology, Jawaharla! Nehru Medical College, AMU, India
2Resident, Department of Pathology and Obstetrics & Gynaecology, Jawaharla! Nehru Medical College, AMU, India
Submission: October 20, 2017; Published: November 10, 2017
*Corresponding author: Kafil Akhtar, Professor, Department of Pathology, Jawaharlal Nehru Medical College, Aligarh Muslim University, Aligarh (UP)-India, Email: drkafilakhtar@gmail.com
How to cite this article: Kafil Akhtar, Mohd Rafey, Rana K Sherwani, Zehra Mohsin. Papillary Hidradenoma of Vulva: A Rare Case Presentation. Open Access J Surg. 2017; 6(5): 555696. DOI: 10.19080/OAJS.2017.06.555696
Abstract
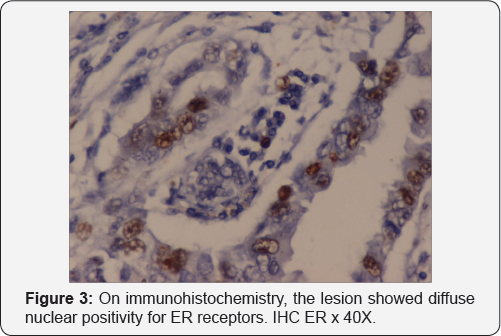
Papillary hidradenomas in the vulva arises from specialized anogenital mammary-like glands in and around the intralabial sulcus. These are benign lesions, which present as slow growing, circumscribed cystic masses. Histologically, papillary hidradenomas are characterized by glandular structures and complex branching papillae with fibrovascular stalks. The glands are lined by myoepithelial cells and epithelial secretory cells with a surrounding fibrous stroma. Oestrogen and progesterone receptors are potential markers to differentiate between anogenital sweat glands and conventional sweat glands. We intend to present a case of excoriating papillary hidradenoma of vulva in a 23-year old female with review of literature.
Keywords: Papillary hidradenoma, Vulva, Benign Tumor.
Introduction
Papillary hidradenoma is a rare, slow growing benign cystic papillary tumor which occurs in the anogenital region [1]. It is seen in middle-aged females, commonly between the ages of 30-49 years. Rarely, it can be seen over the head and neck, and over modified apocrine gland areas such as breast, external ear canal, and eyelid. It is then referred to as ectopic hidradenoma papilliferum [2]. Although the origin of papillary hidradenoma was previously thought to be an apocrine sweat gland, recent studies have suggested that it may derive from the anogenital mammary-like gland [2].
It usually presents as an asymptomatic flesh-colored nodule in the anogenital area of women [3]. It simulates Bartholin’s cyst, vulval abscess, lipoma and chronic vulval lesions. Clinically it may mimic a carcinoma, so the correct cytologic interpretation of the tumor cells with subsequent careful histologic confirmation is essential for good management. The tumor has got a good prognosis and malignant transformation is extremely rare [4]. We present a case of excoriating papillary hidradenoma of vulva in a 23-year old female with review of literature.
Case Summary
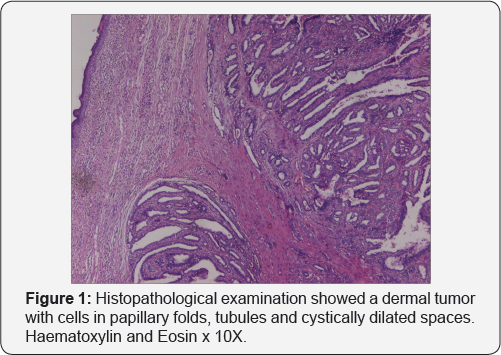
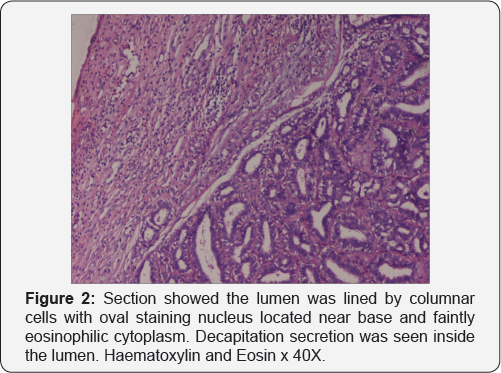
A 23 year old female presented to the Gynaecology outpatients department with complaints of painless swelling on the external genitalia since 3 months. On examination, the labial mass was 8x5x3 cm in size, sessile, non-tender, soft to firm in consistency. Speculum and bimanual examinations led to a provisional diagnosis of vulval lipoma. The mass was completely excised and histopathology revealed well circumscribed dermal nodules in complex papillary glandular pattern with nuclear stratification and foci of mild nuclear pleomorphism, lined by apocrine cells and myoepithelial cell layer (Figures 1 & 2). On immunohistochemistry, the lesion showed diffuse nuclear positivity for ER and PR receptors (Figure 3). Our patient is well after 12 months of follow-up period.
Discussion
Papillary hidradenoma is a rare, benign, cystic, papillary vulval tumor that occurs commonly in Caucasians, aged 3070 years [5]. It usually arises from the anogenital glands, with apocrine differentiation [2]. It usually presents as a solitary, slow growing, painless nodular mass on the labial fold or in the perianal area. Majority of the lesion occurs in the labia majora as an elevated reddish brown papillary ulcerated mass [3]. A painful lesion located on the lower aspects of labia may be misdiagnosed as Bartholin cyst/ abscess. Papillary hidradenoma originating from labia minora may be a predisposition for the development of Bartholin's abscess.2 Blockade to drainage of the Bartholin's duct by a tumor in the vicinity may also result in development of Bartholin’s cyst/ abscess [3].
The clinical differential diagnoses of papillary hidradenoma are epidermal inclusion cysts, seborrhoeic dermatitis, fibroepithelial polyp, fibroma, fibromyoma, dermatofibroma, lipoma, syringoma, hemangioma, angiokeratoma, pyogenic granuloma and malignancy [6,7]. Papillary hidradenoma, though benign, may be associated with concomitant vulvar invasive squamous cell carcinoma, Paget's disease and melanoma [8,9]. Nishie et al have reported a case of vulvar papillary hidradenoma with mixed histopathologic features of syringocystadenoma papilliferum and anogenital mammary glands [3].
Histologically, papillary hidradenoma is a dermal tumor, which represents an adenoma with apocrine differentiation, with a well-circumscribed pseudocapsule due to stromal compression [10,11]. Tubular and cystic structures are seen within the tumor mass, with papillary folds projecting into the cystic spaces. The lumina are usually surrounded by a dual cell layer of inner secretory cells and an outer cuboidal cell layer with myoepithelial cells. Occasionally, the cystic spaces are lined by a single layer of columnar cells with oval, hypochromatic nuclei and eosinophilic cytoplasm. Vazmitel et al have reported a case of ductal carcinoma in-situ arising in papillary hidradenoma, with suggestive viral etiology [5]. Kazakov et al. have reported human papilloma viral particles in 4 out of 15 cases of papillary hidradenomas [6].
Surgical excision has been regarded as adequate treatment of this benign lesion. In cases with associated Bartholin’s cysts and abscesses or suggested transformation into malignancy, wide surgical excision and careful follow-up is the appropriate approach of management [9,12]. Simple drainage of recurrent Bartholin's abscess may not be sufficient, especially in elderly women [12]. Our case presentation of vulval papillary hidradenoma in a young asian woman, with a large sized tumor at presentation and a short history suggestive of rapid course of progression makes it unique.
Conclusion
Papillary hidradenoma is a rare benign slow growing anogenital lesion of adult females with a malignant potential. When an adult female presents with a nodular lesion in the anogenital area, papillary hidradenoma should be kept in mind along with other conditons such as sexually transmitted diseases and other benign and malignant tumors and should be treated by a multidisciplinary approach, with wide surgical excision and a close follow-up and screening for human papilloma virus infection.
References
- Simpson WA, Burke M, Frappell J, Cook MG (2010) Paget's disease, melanocytic neoplasia and hidradenoma papilliferum of the vulva. Histopathol 12(6): 675-679.
- Wilkinson EJ, Xie D (2010) Benign disorders of the Vulva. In: Kurman RJ (ed) Blaustein's pathology of the female genital tract, 5th edn. Springer, New Delhi, pp. 37-98.
- Nishie W, Sawamura D, Mayuzumi M, Takahashi S, Shimizu H (2014) Hidradenoma papilliferum with mixed histopathologic features of syringocystadenoma papilliferum and anogenital mammary like glands. J Cutan Pathol 31(8): 561-564.
- Nirmala D, Rajnish K, Sunita S, Nidhi R (2011) Hidradenoma papilliferum of the vulva: case report and review of literature. Arch Gynecol Obstet 284: 1015-1017.
- Vazmitel M, Spagnolo DV, Nemcova J, Michal M, Kazakov DV (2011) Hidradenoma papilliferum with a ductal carcinoma in situ component: case report and review of literature. Am J Dermatopathol 30(4): 392394.
- Kazakov DV, Mikyskona I, Kutzner H, Simpson RH, Hes O, et al. (2010) Hidradenoma papilliferum with oxyphilic metaplasia: a clinicopathological study of 18 cases, including detection of human papilloma virus. Am J Dermatopathol 27(2): 102-110.
- Uke MS, Kulkarni MB, Ajit D, Gujral S (2010) Diagnosis of hidradenoma papilliferum of the vulva on cytologic smears: a case report. Acta Cytol 54(5): 907-910.
- Plantier F (2015) Hidradenoma papilliferum or anogenital mammary-like gland adenoma. Ann Dermatol Venereol 142(10): 609-612.
- Yuta K, Kosuke K, Kumiko K, Tokuya M, Tetsuo N (2014) Hidradenoma papilliferum of the vulva in association with an anogenital mammarylike gland. J of Dermatology 41(5): 411-413.
- Parks A, Branch KD, Metcalf J, Underwood P, Young J (2012) Hidradenoma papilliferum with mixed histopathologic features of syringocystadenoma papilliferum and anogenital mammarylike glands: report of a case and review of the literature. Am J Dermatopathol 34(1): 104-109.
- Ramli I, Hassam B (2014) Single nodule of the vulva: think of papillary hidradenoma. Pan Afr Med J 19: 301-302.
- Srinath M Kambil L, Ramesh MB, Deepti A, Celestine DS (2014) Hidradenoma papilliferum of the vulva. Indian Dermatol Online J 5(4): 523-524.






























