Selective Neuropsychological and Functional Improvement in Chronic Severe Traumatic Brain Injury Using Streptolysin O: A Case Report
Jeffrey Ewert P1*, Marshall McMillan P2, Stephen Mamber W3 and John McMichael3,4
1Carolina Neuroservices, Charlotte, NC
2Novant Health Crown Point Family Physicians, Charlotte, NC
3The Institute for Therapeutic Discovery, Delanson, NY
4Beech Tree Labs, Providence, RI
Submission: May 17, 2024; Published: May 31, 2024
*Corresponding author: Jeffrey Ewert, Carolina Neuroservices, Charlotte, NC, USA
How to cite this article: Jeffrey Ewert P, Marshall McMillan P, Stephen Mamber W, John M. Selective Neuropsychological and Functional Improvement in Chronic Severe Traumatic Brain Injury Using Streptolysin O: A Case Report. Open Access J Neurol Neurosurg 2024; 19(1): 556002. DOI: 10.19080/OAJNN.2024.19.556002.
Abstract
Background: A non-hemolytic form of streptolysin O (ML-05) can promote wound healing, decrease inflammation and alleviate fibrosis. It was hypothesized that ML-05 could promote neuronal cell survival and recovery in patients with traumatic brain injury (TBI).
Methods: A 58-year-old female was treated with ML-05 beginning eleven years after incurring severe automobile accident-related TBI. The patient self-administered sublingual ML-05 (32 ng/ml, 50 ul/dose, 4X/day for 36 months). Relative Change Index (RCI), IQ, neuropsychological, Minnesota Multiphasic Personality Inventory (MMPI-2-RF), Rey Complex Figure Test (RCFT) and self-assessments were made pre-ML-05 and again five and 31 months after initiation of dosing.
Results: At five months, the RCI showed improvement in eight of nine cognitive domains, though statistical significance (p<0.05) was only achieved for visual memory. Neuropsychological testing showed modest improvement and stability by 36 months. IQ improved from 88 to 98 in 36 months. There were statistically significant improvements in multiple MMPI-2-RF categories at 36 months. RCFT drawings markedly improved. Adaptive functioning improved. No side effects were reported.
Conclusion: Sublingual administration of ML-05 appeared to be safe and potentially useful in a patient with neurological impairment after TBI. Further clinical studies are needed for better understanding the value of ML-05 in treating other TBI patients.
Keywords: Streptolysin O; Traumatic brain injury; Sublingual administration; Visual memory; Self-confidence
Abbreviations: IQ: Intelligence Quotient; SLO: Streptolysin O; MMPI-2-RF: Minnesota Multiphasic Personality Inventory-2-Restructured Form; MMP9: Matrix metalloproteinase 9 gene; MMP-9: Matrix metalloproteinase 9 enzyme; MNB: Meyers Neuropsychological Battery; NSI: Neurobehavioral Symptom Inventory; PCRS: Patient Competency Rating Scales; RCI: Relative Change Index; RCFT: Rey Complex Figure Test; RCI: Relative Change Index; TBI: Traumatic Brain Injury; WAIS-IV-IQ Test: Wechsler Adult Intelligence Scale - Fourth Edition; CDC: Centers for Disease Control; IL-1beta: Interleukin-1beta; TNF-alpha: Tumor Necrosis Factor alpha; ECM: Extracellular Matrix ; ADHD: Attention-Deficit/Hyperactivity Disorder; CT: Computerized Tomography
Introduction
Traumatic brain injury (TBI) is a serious medical condition that results from such external physical traumas as sports injuries, motor vehicle accidents or falls. Some of the characteristic effects of TBI are headaches, confusion, behavioral changes and memory loss. The various neurological, cognitive and emotional impairments resulting from TBI can lead to long-term disability as well as being a cause of mortality. In fact, TBI has become a significant cause of morbidity and mortality, both in the United States and worldwide. The Centers for Disease Control and Prevention (CDC) estimated that by 2021, TBI accounted for over 220,000 hospitalizations and almost 70,000 TBI-related deaths in the United States alone [1-4]. The CDC categorizes TBI as mild (e.g., concussions), moderate and severe [3]. Recovery from TBI usually occurs in the first 18 months post injury, with minimal improvement in neuropsychological functioning after that. After five years, 22% of the inpatient individuals who received rehabilitation for TBI died, 30% got worse, 26% improved, and the remaining 22% showed no improvement in their condition [3]. On a biochemical and molecular basis, various mechanisms have been postulated to explain the neuronal damage caused by TBI. These mechanisms include the release of pro-inflammatory cytokines, e.g., interleukin-1beta (IL-1beta) and tumor necrosis factor alpha (TNF-alpha), which can contribute to neuronal cell damage [5,6]; oxidative stress [7,8]; disruption of the blood-brain barrier (9,10), and neuronal death through excitotoxicity [11,12] and apoptosis [13].
Another mechanism of interest is neuronal damage via the activation of matrix metalloproteinases (MMPs); [14,15]. MMPs are enzymes capable of remodeling or degrading the brain’s extracellular matrix (ECM), a network of proteins and related molecules, such as collagens, laminins and elastin, which provide structural support within the brain [16-18]. The ECM plays an important role in such processes as cell migration, cell proliferation and tissue repair [17,18]. Degradation of the ECM can lead to inflammation, neuronal cell death, and other actions that can further contribute to the damage caused by TBI [19]. One of the most important MMPs is MMP-9, which may have an essential role in TBI. The MMP9 gene and the MMP-9 enzyme are known to be up-regulated or overexpressed in the brains of animals and humans with TBI [20-22].
Although MMP-9 can help promote neuronal cell migration and proliferation to help repair brain damage, excessive MMP-9 activity can cause abnormal tissue remodeling and interfere with neuronal cell migration and proliferation, resulting in edema, inflammation, the formation of fibrosis or scar tissue in the brain, breakdown of the blood-brain barrier and cell death [14,20]. All of these actions can contribute to lasting brain damage. Accordingly, various studies have suggested that MMPs, notably MMP-9, may be a potential target for therapeutic intervention. Research has shown that inhibition of MMP-9 can reduce fibrosis and improve functional outcomes in TBI animal models. One such study found that inhibition of MMP-9 activity with a specific inhibitor in a rodent model of TBI reduced brain edema, blood-brain barrier disruption, and neuronal cell death [23]. Another in vivo animal study found that inhibition of MMP-9 reduced brain injury and improved cognitive function [24]. Thus, a therapeutic agent that can target MMP-9 and other components of an abnormal ECM could help reduce brain injury severity and improve TBI outcomes.
Streptolysin O (SLO) is a membrane-damaging extracellular toxin (cytolysin) produced by Group A beta-hemolytic streptococci [25,26]. However, low concentrations of an oxidized, non-hemolytic form of SLO (also known as ML-05), has shown beneficial effects on extracellular matrix (ECM) structure and function. In particular, ML-05 promoted keratinocyte migration and proliferation in wound-healing scratch assays and wound healing in a human skin organ culture wound model in vitro [27]. ML-05 also up- or down-regulated specific genes associated with cell migration, cell proliferation and inflammation [28]. Of particular interest was the down-regulation of the MMP9 gene, as the protein MMP-9 is associated with the pathogenesis of TBI. In vivo, ML-05 beneficially affected collagen levels in two separate mouse fibrosis models [29]. Based on these and other observations, it was hypothesized that ML-05 could help alleviate TBI by inhibiting MMP-9 or otherwise alleviating fibrosis, inflammation or ECM dysfunction, thus promoting neuronal cell survival, migration and proliferation. Accordingly, the purpose of this case study was to investigate the effects of sublingually administered ML-05 on various neuropsychological functions in a female adult with otherwise untreatable TBI.
Case Report
Patient Characteristics Pre-injury (pre-TBI)
The patient was a 58-year-old right-handed woman, with no previous history of head injury or any other neurological disorder prior to her acquiring a head injury in an accident. She had a bachelor’s degree in math with a 3.4 GPA. The patient’s level of premorbid functioning was known to be in the average range. However, she reported that she had a reading and written language disability. She further reported that she had Attention-deficit/hyperactivity disorder (ADHD) and failed the first grade. She was working as a software company database administrator for 25 years prior to her injury. She had two grown children and was living independently with her husband in a moderately sized city.
Nature of the Injury and Post-injury Recovery
The woman suffered a severe traumatic brain injury at age 47 in May 2007 in a motor vehicle accident. The patient’s vehicle was T-boned on the driver’s side, and the car rolled three times. She was unconscious for six weeks; the length of post-traumatic amnesia is uncertain. Her initial Glascow coma scale was a three. Cranial computerized tomography (CT) scan revealed bilateral subdural hematomas, and a right front temporal contusion. She initially exhibited left hemiparesis. Initial surgeries included a laparotomy, splenectomy and tracheostomy. A peg tube was placed in her stomach, and a Greenfield filter (for prevention of pulmonary emboli) was placed in the inferior vena cava. The patient was initially hospitalized at one hospital, and then was transferred to a rehabilitation institute. She was later transferred to a second rehabilitation facility where she was treated for nine months. She was finally treated at a third rehabilitation facility for an additional nine months. The patient did not receive any further rehabilitation. After her injury, the patient was unable to return to any type of employment. She lived at home with her husband and daughter. She spent her time gardening and doing some cleaning. She was unable to engage in food preparation or cooking activities due to her visual perceptual and organizational problems. She was also unable to handle financial affairs or drive a vehicle. She socialized on rare occasions with some friends and attended social meetings of community service organizations (e.g., Masons, Shriners). In short, she appeared unimproved but stable for nearly 11 years.
Neuropsychological Assessment Methods
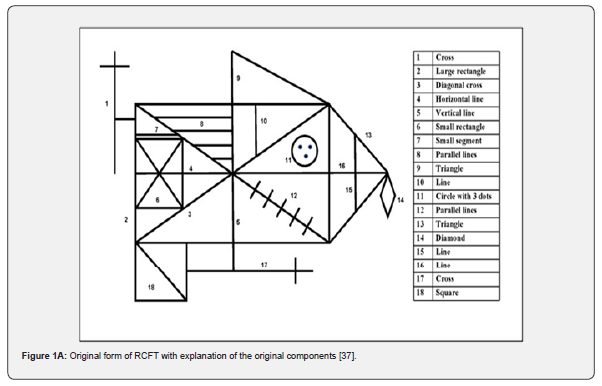
An initial extended Meyers Neuropsychological Battery (MNB); [30] was performed prior to administration of ML-05. The following neuropsychological battery of tests was administered across all three test periods, pre-ML-05 (March 2018), post-ML-05 (November 2018) and during a second post-ML-05 assessment (June 2021): a) The Neurobehavioral Cognitive Status Exam (NCSE; [31]), which measures nine domains of cognitive functioning, including attention/concentration, working memory; processing speed and mental flexibility; verbal and visual memory functioning, verbal and visual reasoning skills, bilateral motor skills and executive functioning; b) The Wechsler Adult Intelligence Scale - Fourth Edition (WAIS-IV-IQ test; [32,33]); c) The Meyers Neuropsychological Battery (MNB; [34]); d) The Rey Complex Figure Test Copy Phase (RCFT; [35-37]) and e) The Minnesota Multiphasic Personality Inventory-2-Restructured Form (MMPI–2–RF; [38]). Note: The actual RCFT with explanations of its components is shown in Figure 1A [37]. There also were subjective Patient Competency Rating Scales (PCRS) administered to both patient and spouse.
Data Analysis
Data were analyzed by comparing pre- and post-ML-05 scores from the various neuropsychological assessments. Standard statistical methods were used to obtain Z-scores or T-scores (two measures of statistical hypothesis testing) and determine statistical significance (at alpha = 0.05) The Relative Change Index was utilized with the MNB and WAIS –IV.
Patient Characteristics from Post-injury Neuropsychological Assessment (pre-ML-05)
The patient came to the clinic for a neuropsychological assessment in March 2018. She reported intermittent but ongoing, diplopia, ongoing left sided numbness and weakness, balance problems and headaches, dysarthria, and problems with concentration. She reported interpersonal problems resulting from defensiveness and social avoidance. She reported intermittent depression and frustration. She had significant anxiety when in crowds. She further reported functional memory problems for numbers, tasks, object locations, conversations, written information, routes and biographical information. In addition, she reported difficulty with simple mathematics.
Sublingual ML-05 administration
Treatment with sublingual ML-05 was considered under compassionate use and informed consent of the patient and her husband; both had exhausted all other treatment options. Although ML-05 is not an approved drug, the physician who prescribed it was familiar with its safety profile and chose to use it as part of his practice of medicine to the benefit of patients under his care. Valuable observations were expected from patients treated anecdotally under compassionate use without violating commonly accepted medical standards. The preparation of ML-05 has been described previously [29]. The low dose of ML-05 used (32 ng/ml, 50 ul per dose) has been established as neither hemolytic nor cytotoxic. The patient started taking ML-05 sublingually, four times a day through an eyedropper. Her first administration of ML-05 began on May 29, 2018. The patient continued with daily ML-05 for 36 months, through two neuropsychological examinations, and continues taking this agent to this day.
Results
Neuropsychological Assessment Performance in March 2018 (Pre-ML-05)
Neuropsychological testing was performed in March 2018, nearly 11 years after the patient's accident. At the time of her initial neuropsychological assessment, the patient was only taking the following two medications on a routine basis: The antidepressant citalopram, 20 mg/day, and the anticonvulsant lamotrigine, 25 mg/day. In the initial NSI, compared to a normative sample in which an average individual would be expected to show a score of 50 [39], her score was 71 (higher scores denote more symptoms reported). On the NSI Affective Scale and NSI Cognitive Scale, she showed scores of 64 and 59. respectively, which fell into the normal expected range. However, she had a score of 76 in the NSI Somatosensory Scale, indicating that she was reporting increased physical difficulties or complaints. On the NSI Vestibular Scale, she showed a score of 71, suggesting increased balance type difficulties or complaints. She reported symptoms as “Severe” or “Very Severe” in response to a variety of NSI questions.
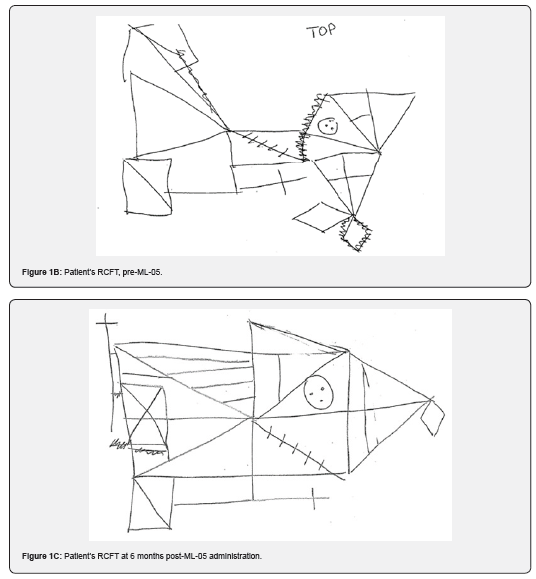
The results of the pre-ML-05 NCSE are shown in Table 1. The data from this assessment indicated impairment in most categories, with an Overall Test Battery Mean (OTBM) of 38. (The estimated premorbid level was a value of 50). In particular, executive functioning was substantially impaired. Analysis of performance on the Rey complex figure copy phase (Figure 1B) indicated profound impairment in visuo constructive abilities. Her impaired visual perceptual skills resulted in severe inability to copy the figure. These results were consistent with a severe TBI accompanied by focal damage to the anterior right cerebral hemisphere. With respect to composite scores on the WAIS-IV-IQ test (Table 2), the patient had an estimated full-scale premorbid IQ of 100, which was 88 at the time of this testing (pre-ML-05). Verbal conceptual IQ was 93; perceptual reasoning IQ was 90; working memory was 92; and processing speed IQ was 86. There was no evidence of malingering or poor effort, based on both embedded measures of effort and the results of a Test of Memory Malingering (TOMM; [40]; data not shown).
Clinical Results - First Neuropsychological Assessment, Five Months Post-ML-05
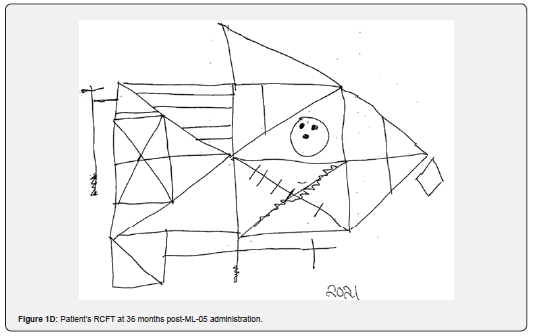
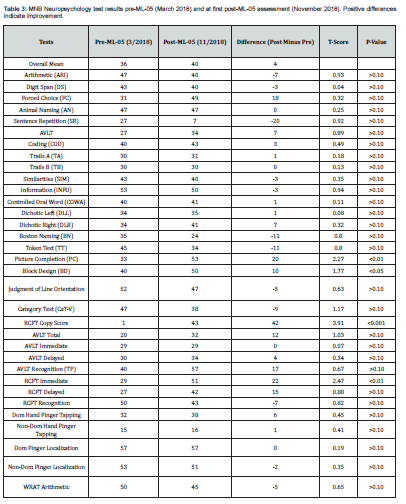
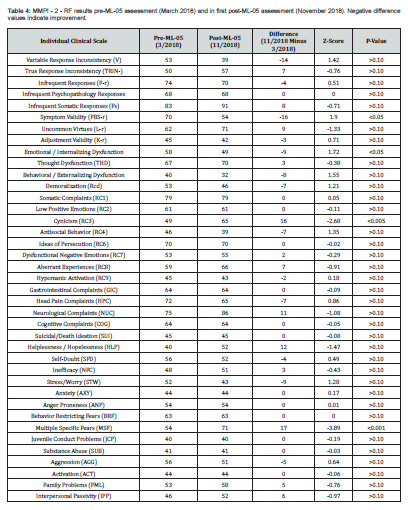
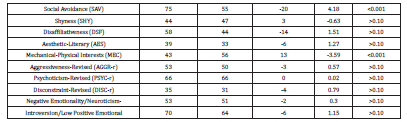
After ML-05 treatment for five months, a neuropsychological re-assessment was performed on November 1, 2018. There were no significant medical changes since the patient’s initial assessment. She was compliant with taking the ML-05 drops, based on reports from her husband. She did not engage in any type of rehabilitation during that time. The NCSE relative change index (RCI) (differences and Z-scores) between pre-ML-05 and five months of treatment are shown in Table 1. The patient continued to have impairment in various cognitive domains, with an OTBM of 41 (versus 38 pre-ML-05). Mild improvements (not statistically significant at alpha = 0.05) were found in eight of the 10 categories: Attention/concentration working memory, processing speed and mental flexibility, visual reasoning, verbal memory, and dominant motor functioning. Mild improvement was also found in executive functioning. Mild decline was seen in the domain of verbal reasoning ability. The only statistically significant improvement (p < 0.05) was found on a measure of visual memory, which improved to the average range of functioning. Overall WAIS-IV-IQ (Table 2) remained stable at 89 in comparison to previous testing (88). Verbal comprehension remained identical at 93. There was mild improvement in perceptual reasoning, from 90 to 94, while processing speed increased from 86 to 92. Working memory declined from 92 to 83. The improvement in the patient's drawing of the Rey complex figure (RCFT) was remarkable (Figure 1C). The patient had no recollection of her pre-ML-05 figure, so it was unlikely that there had been any practice effects resulting in this improved performance. MNB results between March and November 2018 (Table 3) did show statistically significant improvements in picture completion (33 to 53; p<0.01), block design (40 to 50; p<0.05), RCFT immediate (29 to 51; p<0.01) and the RCFT copy phase (which surprisingly scored at a value of 1 pre-ML-05; p<0.001). Although not statistically significant, values for delayed recall of the complex figure improved from 27 to 42. Assessment on the MMPI-2-RF between March and November 2018 (Table 4) yielded statistically significant improvements (based on decreases in the difference between results pre- and post-ML-05 over time) in symptom validity (70 to 54; p<0.05), internalizing dysfunction (58 to 49; p<0.05), and particularly in social avoidance (75 to 55; p<0.001). There also was a decrease in inconsistent, random responses, though this was not statistically significant at alpha = 0.05. On the other hand, the MMPI–2-RF showed statistically significant increases (i.e., adverse changes) in in cynicism (49 to 65; p<0.005), multiple specific fears (54 to 71; p<0.001), and in mechanical and physical interests (43 to 56; p<0.001).
Second Neuropsychological Assessment, 31 Months Post-ML-05
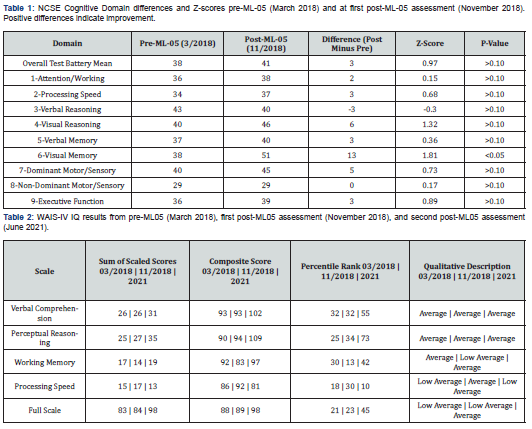
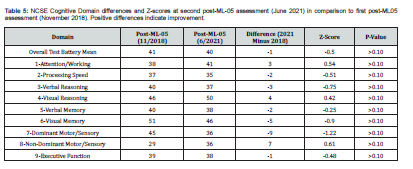
Neuropsychological reevaluation was performed for the second time on June 18, 2021, about 31 months after her last assessment. She reported that she continued to be compliant taking ML-05, and this was verified by her husband. Results of MNB RCI testing in June 2021, relative to the testing performed five months post-ML-05, demonstrated no significant improvement relative to the previous assessment, with the OTBM declining from 41 to 40 (Table 5). Mild improvement was noted in the domain of attention/concentration, working memory and visual reasoning. Executive functions, processing speed, verbal reasoning, verbal memory functioning and visual memory functioning all declined slightly. Dominant motor functioning also declined, though improvement was found with the non-dominant hand. Executive functions declined slightly. However, none of these increases or decreases were statistically significant, indicating some stability in the functions gained after starting and continuing with ML-05. Her second post-ML-05 RCFT showed notable further improvement (Figure 1D).
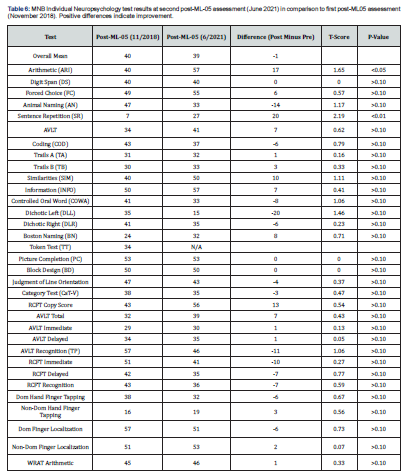
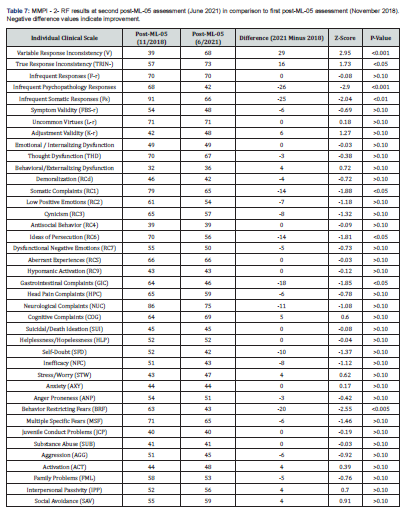
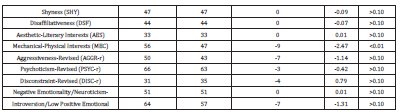
Results of WAIS-IV-IQ testing showed an improvement in full-scale IQ from 89 to 98 (Table 2). Verbal comprehension improved from 93 to 102; perceptual reasoning improved from 94 to 109; and working memory improved from 83 to 97. A mild decline was found in processing speed from 92 to 81. MNB testing showed statistically significant improvements in both arithmetic (p<0.05) and sentence repetition (p<0.01) (Table 6). Results of the second post-ML-05 MMPI-2-RF personality testing also indicated psychological improvement which appeared to be greater than neuropsychological improvement (Table 7).
Although there were statistically significant declines in variable response inconsistency and true response inconsistency, most of the other variables in this second MMPI-2-RF test were favorable, and six categories showed statistically significant improvement at alpha = 0.05. Results of the June 2021 PCRS indicated that the patient perceives herself as having a normal level of overall independent functioning, as demonstrated by a PCRS score of 46 versus 32 in November 2018; this difference was statistically significant (p < 0.01). All domains were now in the average range of functioning. However, the reports completed by her husband indicated that she still demonstrated a mildly impaired level of overall functioning, with mild impairment in activities of daily living, independent activities and functional cognitive abilities.
However, her emotional performance improved the score to 44, and her behavior score was in the low average range of 40. Overall, the patient’s spouse reported less problems in independent living during this assessment. The 2021 interview with the patient’s husband indicated that the patient continued to have problems with her short-term and recent memory. She still had functional memory problems for numbers, object locations, tasks, routes and names. She was better able to remember faces than previously. Interestingly, she could now remember details of the nightly news (as well as the news from the day before) which she could not do before taking ML-05. With respect to social interactions, the patient’s husband believes that her communication skills were an area of significant improvement. Her speech was greatly improved and has been much more understandable to others along with a better emotional connection. She now goes out to social events (e.g., to the Masonic Lodge) with her husband. She goes to a ladies’ group once a week. Her confidence has improved around others. She has also been more connected with her siblings subsequent to taking ML-05. The patient’s overall score of 31 on the second PCRS self-report (post-ML-05 between March 2018 and June 2021; data not shown) was in the borderline range, suggesting an impaired level of overall independent functioning. Results from this PCRS did not indicate significant improvement according to the patient's own report.
However, her overall emotional functioning appeared to improve with respect to feelings of demoralization and low positive emotions. Cognitive complaints declined as well. Overall feelings of helplessness/hopelessness, ineffectiveness, stress, worry and anxiety markedly declined. The ability to control anger also improved. Socially, the patient tended to affiliate with others, as evidenced by a decline in a measure of disaffiliativeness. Aberrant physical experiences also decreased: Gastrointestinal and head pain complaints declined substantially. A separate June 2021 PCRS was completed by the patient’s husband. He rated her as having severe impairment in her activities of daily living, independent activities and functional cognitive abilities. He felt her overall capacity for emotional control was a strength. However, her ability to keep friends and maintain herself as socially presentable was in the impaired range. Relative to the pre- and first post-ML-05 assessments (five months after dosing was initiated), the patient reported improvement in her overall level of daily functioning after being on ML-05 for 36 months. She reported significant improvement in her memory being on ML-05 relative to an over-the-counter supplement that she was taking prior to her using ML-05. Also prior to using ML-05, she had to use a tool for support (a hoe, rake or cane) to walk out to her garden. After five months of ML-05 and beyond, the patient was able to walk independently, and felt that her balance was better.
Furthermore, previous to ML-05, she was not able to bend over without assistance while gardening, while post-ML-05 she reported that she can bend over independently. In terms of social interaction with other individuals, she reported being better able to follow conversations, and was now able to transition from one conversation to another with an individual. She noted an improvement in her dysarthria as well.
Discussion
Results of pre- and post-ML-05 neuropsychological testing yielded mixed results, but overall indicated that ML-05 has potential for improving quality of life in patients with severe TBI. The initial improvements in visual memory and visual reasoning at the first (7-month) post-ML-05 assessment were remarkable. The patient’s initial (pre-ML-05) RCFT drawing during the copy phase was typical of a patient with severe TBI resulting in diffuse axonal injury and specific impairment to the anterior right hemisphere of the brain. The overall gestalt of the figure was lost in this drawing, and indicated severe problems with executive and visual perceptual abilities. However, both at five and especially at 36 months post-ML-05, the patient drew essentially a normal Rey complex figure for the copy phase. Correlating with this improvement in visual construction, improvement in clock drawing and block design performance were also found. Functional correlates in everyday life included improved ability to garden and locate her tools. Her ability to remember details of news reports on TV was probably a function of her improvement in visual memory.
Although improvement in visual memory/executive functioning on the RCFT copy phase have been documented in severe TBI at six- and 12-months post injury, [41], there have been no studies that evaluated improvement in these abilities this long post injury. Most clinicians would assume that this type of improvement would not be possible given the severity of the patient’s injury and the length of time postinjury. Additionally, the improvement in everyday functioning suggests that SLO improves both visual perceptual abilities, visual memory and executive functions. A further encouraging change in the patient after being on ML-05 was the improvement in her ability to communicate and willingness to affiliate with others. This is partially due to improvement in her dysarthria which made her much more intelligible. This improvement, in addition to changes in her cognitive functioning, resulted in increased self-confidence. As a result of this psychological improvement, she was able to take the risk of increased social interactions with others. The improvement in psychological functioning from the November 2018 test date to the June 2021 test date indicated an overall decline in somatic symptoms, and in neurological complaints in particular. There were decreased complaints related to depression, notably in feelings of demoralization and dysfunctional negative emotions. Anxiety decreased dramatically. The ability to control anger improved. These results were found despite results of neuroimaging performed on the patient which found worsening atrophy over time, in addition to initial acceleration/deceleration damage causing axonal shearing, right frontal lobe contusion and bilateral subdural hematomas. These findings were reviewed by a prominent neuropsychologist (E. D. Bigler, personal communication), who was surprised that such improvement, particularly in the RCFT, could be found in the patient with worsening brain anatomy over time.
The results found with this patient are suggestive that ML-05 may provide some hope for improvement in patients with chronic severe TBI. Although there are certainly limitations of this single case report. Improvement on the RCFT could have partially been due to practice effects, although we believe this is unlikely because of the five month and 31-month testing intervals, and the lack of practice effects that have been found with the Rey. We had no comparable control patient(s) in this study. Placebo effects could also account for some of the improvement in psychological functioning; however, it is believed that improvement in psychological functioning is due to the patient’s improvement in cognitive functioning and her ability to improve her level of interaction with others and overall adaptive functioning. Accordingly, studies with a larger sample size are needed to further evaluate the effects of ML-05 under more controlled conditions. Additional case studies and initial clinical trials of the effects of ML-05 on TBI are expected in the future. Based on ML-05’s mechanism(s) of action, it is hypothesized that dosing with ML-05 should begin as soon as possible after TBI occurs.
References
- TBI Data and Statistics (2019) Centers for Disease Control and Prevention.
- Centers for Disease Control and Prevention (2023) TBI: Get the Facts. CDC.
- Moderate and Severe TBI (2023) Concussion | Traumatic Brain Injury | CDC Injury Center.
- National Institute of Neurological Disorders and Stroke (2023) Traumatic Brain Injury Information Page | National Institute of Neurological Disorders and Stroke.
- Sordillo PP, Sordillo LA, Helson L (2016) Bifunctional role of pro-inflammatory cytokines after traumatic brain injury. Brain Injury 30(9): 1043-1053.
- Doğanyiğit Z, Erbakan K, Akyuz E, Polat AK, Arulsamy A, et al. (2022) The Role of Neuroinflammatory Mediators in the Pathogenesis of Traumatic Brain Injury: A Narrative Review. ACS Chemical Neurosci 13(13): 1835-1848.
- Khatri N, Thakur M, Pareek V, Kumar S, Sharma S, et al. (2018) Oxidative Stress: Major Threat in Traumatic Brain Injury. CNS & Neurological Disorders - Drug Targets 17(9): 689-695.
- Fesharaki-Zadeh A (2022) Oxidative Stress in Traumatic Brain Injury. Int J Mol Sci 23(21): 13000.
- Cash A, Theus MH (2020) Mechanisms of Blood-Brain Barrier Dysfunction in Traumatic Brain Injury. Int J Mol Sci 21(9): 3344.
- Sulhan S, Lyon KA, Shapiro LA, Huang JH (2018) Neuroinflammation and blood-brain barrier disruption following traumatic brain injury: Pathophysiology and potential therapeutic targets. J Neurosci Res 98(1): 19-28.
- Tehse J, Taghibiglou C (2019) The overlooked aspect of excitotoxicity: Glutamate-independent excitotoxicity in traumatic brain injuries. Eur J Neurosci 49(9): 1157-1170.
- Liao R, Wood TR, Nance E (2020) Nanotherapeutic modulation of excitotoxicity and oxidative stress in acute brain injury. Nanobiomed 7: 184954352097081.
- Akamatsu Y, Hanafy KA (2020) Cell Death and Recovery in Traumatic Brain Injury. Neurotherapeutics 17(2): 446-456.
- Abdul-Muneer PM, Pfister BJ, Haorah J, Chandra N (2015) Role of Matrix Metalloproteinases in the Pathogenesis of Traumatic Brain Injury. Mol Neurobiol 53(9): 6106-6123.
- Trivedi A, Noble-Haeusslein LJ, Levine JM, Santucci AD, Reeves TM, et al. (2019) Matrix metalloproteinase signals following neurotrauma are right on cue. Cell Mol Life Sci 76(16): 3141-3156.
- Cabral-Pacheco GA, Garza-Veloz I, Castruita-De la Rosa C, et al. (2020) The Roles of Matrix Metalloproteinases and Their Inhibitors in Human Diseases. Int J Mol Sci 21(24): 9739.
- Karamanos NK, Theocharis AD, Piperigkou Z, et al. (2021) A guide to the composition and functions of the extracellular matrix. FEBS J 288(24): 6850-6912.
- Bonnans C, Chou J, Werb Z (2014) Remodelling the extracellular matrix in development and disease. Nature Rev Mol Cell Biol 15(12): 786-801.
- George N, Geller HM (2018) Extracellular matrix and traumatic brain injury. J Neurosci Res 96(4): 573-588.
- Grossetete M, Phelps J, Arko L, Yonas H, Rosenberg GA (2009) Elevation of matrix metalloproteinases 3 and 9 in cerebrospinal fluid and blood in patients with severe traumatic brain injury. Neurosurgery 65(4): 702-708.
- Pijet B, Stefaniuk M, Kostrzewska-KA, Tsilibary PE, Tzinia A, et al. (2018) Elevation of MMP-9 Levels Promotes Epileptogenesis After Traumatic Brain Injury. Mol Neurobiol 55(12): 9294-9306.
- Hayashi T, Kaneko Y, Yu S, Bae E, Stahl CE, et al. (2009) Quantitative analyses of matrix metalloproteinase activity after traumatic brain injury in adult rats. Brain Res 1280: 172-177.
- Shi H, Wang HL, Pu HJ, Shi YJ, Zhang J, et al. (2015) Ethyl pyruvate protects against blood-brain barrier damage and improves long-term neurological outcomes in a rat model of traumatic brain injury. CNS Neurosci Ther 21(4): 374-384.
- Tao XG, Shi JH, Hao SY, Chen XT, Liu BY (2017) Protective Effects of Calpain Inhibition on Neurovascular Unit Injury through Downregulating Nuclear Factor-κB-related Inflammation during Traumatic Brain Injury in Mice. Chin Med J (Engl) 130(2): 187-198.
- Alouf JE (1980) Streptococcal toxins (streptolysin O, streptolysin S, erythrogenic toxin). Pharmacol Ther 11(3): 661-717.
- Wannamaker LW (1983) Streptococcal toxins. Rev Infect Dis 5(Suppl 4): S723-S732.
- Tomic-Canic M, Mamber SW, Stojadinovic O, Lee B, Radoja N, et al. (2007) Streptolysin O enhances keratinocyte migration and proliferation and promotes skin organ culture wound healing in vitro. Wound Repair Regen 15(1): 71-79.
- Mamber SW, Gurel V, Rhodes RG, McMichael J (2011) Effects of streptolysin o on extracellular matrix gene expression in normal human epidermal keratinocytes. Dose Response 9(4): 554-578.
- Mamber SW, Long V, Rhodes RG, Pond-Tor S, Wheeler LR, et al. (2004) The use of streptolysin o for the treatment of scars, adhesions and fibrosis: initial investigations using murine models of scleroderma. Nonlinearity Biol Toxicol Med 2(2): 67-87.
- Hoover PJ, Nix CA, Llop JZ, Lu LH, Bowles AO, et al. (2022) Correlations Between the Neurobehavioral Symptom Inventory and Other Commonly Used Questionnaires for Traumatic Brain Injury. Mil Med usab559.
- Wiederman MW, Morgan CD (1995) The Neurobehavioral Cognitive Status Exam (NCSE) with Geriatric Inpatients, Clinical Gerontologist 15(4): 35-47.
- Wechsler D (2008) NCS Pearson; Bloomington, MN: 2008. Wechsler Adult Intelligence Scale, Fourth Edition (WAIS-IV). APA PsycTests.
- Erdodi LA, Abeare CA (2020) Stronger Together: The Wechsler Adult Intelligence Scale-Fourth Edition as a Multivariate Performance Validity Test in Patients with Traumatic Brain Injury. Arch Clin Neuropsychol 35(2): 188-204.
- Meyers JE, Miller RM (2023) Objective methods for matching neuropsychological patterns: Formulas and comparisons. Appl Neuropsychol Adult 30(2): 249-258.
- Rey A (1941) L'examen psychologique dans les cas d'encéphalopathie traumatique. The psychological examination in cases of traumatic encepholopathy. Problems Arch Psychol 28: 215-285.
- Meyers JE, Meyers KR (1995) Rey Complex Figure Test and Recognition Trial: Professional Manual. Florida: Psychological Assessment Resources, Odessa.
- Zhang X, Lv L, Min G, Wang Q, Zhao Y, et al. (2021) Overview of the Complex Figure Test and Its Clinical Application in Neuropsychiatric Disorders, Including Copying and Recall. Front Neurol 12: 680474.
- Ben-Porath Y, Tellegen A (2008) Minnesota Multiphasic Personality Inventory-2-Restructured Form (MMPI-2-RF) [Database record]. APA PsycTests.
- Meyers JE, English J, Miller RM, Lee AJ (2015) Normative Data for the Neurobehavioral Symptom Inventory. Appl Neuropsychol Adult 22(6): 427-434.
- Lynch WJ (2004) Determination of effort level, exaggeration, and malingering in neurocognitive assessment. J Head Trauma Rehabil 19(3): 277-283.
- Zaninotto AL, Vicentini JE, Solla DJ, Silva TT, Guirado VM, et al. (2017) Visuospatial memory improvement in patients with diffuse axonal injury (DAI): a 1-year follow-up study. Acta Neuropsychiatr 29(1): 35-42.






























