Transcranial Doppler: A Beginning of a New Era for Stroke Diagnosis
Bafna A1*, Bafna P2, Jobanputra Y2 and Kadam DB1
1BJ Medical College, Pune, India
2RCSM Government Medical College, Kolhapur, India
Submission: December 08, 2022 ; Published: February 06, 2023
*Corresponding author: Bafna A, RCSM Government Medical College, Kolhapur, India
How to cite this article: Bafna A, Bafna P, Jobanputra Y and Kadam DB. Transcranial Doppler: A Beginning of a New Era for Stroke Diagnosis. Open Access J Neurol Neurosurg 2023; 17(5): 555974. DOI: 10.19080/OAJNN.2023.17.555974.
Abstract
Transcranial Doppler (TCD) is an intracranial neurovascular exam that provides a real-time, rapid, non-invasive ultrasound technique to analyze cerebrovascular function. It uses high-frequency sound waves to assess the blood flow velocity, detect the deficit that causes focal vascular stenosis, and diagnose the embolic signals inside these arteries. Moreover, it can be used to analyze particular vascular territory of physiologic health by measuring cerebral vasoreactivity, cerebral autoregulation, and functional hyperemia. The information obtained from these examinations is increasingly becoming pertinent for therapeutic decision-making. In this study, we are going to focus on a comparative analysis of TCD findings using clinical and other modalities and assess the specificity, sensitivity, and positive and negative predictive value of TCD findings in Asymptomatic and Symptomatic high-risk elderly patients. Furthermore, we will study the clinical usefulness of TCD in evaluating patients with cerebrovascular accidents (CVA).
Keywords: :Stroke; Transcranial Doppler; Hypertension; Ischemic heart disease; Cerebral hemodynamics
Introduction
The blood flow in the brain helps transport the essential nutrients throughout the brain and simultaneously helps eliminate waste. During this process, the brain’s metabolic rate is maintained constantly. Restrictions of blood flow can occur due to the narrowing of blood vessels (stenosis) or due to several other reasons like blockage (embolism), clot formation (thrombosis), and blood vessel rupture (hemorrhage). This type of restriction leads to a lack of adequate blood flow in the brain (ischemia), which can result in a stroke [1].
The Transcranial Doppler (TCD) ultrasonography helps determine the blood flow through the arteries. This procedure passes a high-frequency sound wave through the patient’s tissues. These sound waves reflect off the blood cells present in the vessels, allowing the examiner to interpret their direction and speed. The sound waves are then recorded and displayed on the screen [2]. TCD’s specificity and sensitivity are lower than other imaging methods such as Magnetic Resonance Angiography (MRA) and Computed Tomography Angiography (CTA). It can detect most lesions requiring interventional therapy, such as angioplasty, stenting, and local thrombolysis [3]. It can assess the cerebral hemodynamic consequences of steno-occlusive lesions in the cervical parent artery and monitor Intracranial Pressure (ICP), Cerebral Perfusion Pressure (CPP), and Midline Deviation allowing us to assess the patient’s neurocritical pathological characteristics in a non-invasive manner [4].
Cerebral angiography has been able to show acute occlusion in which 76% of critical Middle Cerebral Artery (MCA) territory gets infracted within 6 hours from the onset of stroke [5]. TCD can easily detect this kind of angiographic occlusion with high specificity (90%) and sensitivity, giving a very high positive predictive value [6]. TCD also helps screen for Diabetes Mellitus (DM), as the risk of stroke increases by two folds compared to non-diabetic [7]. These are a few of the actual uses of TCD. In this research, we are going to study about
i. The comparative analysis of TCD findings with clinical & other imaging modalities.
ii. To assess the sensitivity, Specificity, Positive Predictive Value, and Negative Predictive Value of TCD Findings in the asymptomatic and symptomatic high-risk elderly population.
iii. To study the clinical usefulness of TCD study in evaluating patients with Cardiovascular Accidents (CVA).
Methods
The proposed study included 60 elderly patients ( 60 years of age). Out of these 60 patients, 32 patients showed effects of cerebellar ataxia, symptomatic hemiplegia, ocular symptoms, and aphasia. The remaining 28 patients were asymptomatic with high-risk factors of CVA (HTN, DM, IHD, and previous stroke/TIA). All of these patients were screened using a TCD machine. The four different examination windows studied were: transtemporal, submandibular, transorbital, and suboccipital. The lesions found in the examination were classified as stenosis or vessel occlusion, then the results were compared with Magnetic Resonance Angiography (MRA).
Diagnostic Criteria
For stenosis:
• Mean Velocity: - 100 cm/s
• Comparison of PSV with contralateral vessel PSV
• PSV> 30% - suspicious
• PSV> 50% - definite
For Occlusion: -
• Absence of arterial wave signal at expected death.
• Presence of signals in vessels that communicate with
the occluded artery.
• Altered flow in communicating vessels, indicating
collateralization.
Results
4 patients out of 32 symptomatic patients and 5 out of 28 asymptomatic patients had a poor examination window; therefore, they were not included in the statistical calculation.

The TCD findings demonstrated a specificity of 60.87% and a sensitivity of (75%) (P=0.0096). The Positive Predictive value (PPV) was 70%, and the Negative Predictive Value (NPV) was 66.7%. The TCD results of the patients were also compared with the MRA results of those similar patients. The findings are as follows:
Asymptomatic Patients:

The sensitivity was 78.57%and specificity was 66.67% (P= 0.030). The PPV was 78.57%, and the NPV was 66.67%.
Symptomatic Patients:

Sensitivity was 81.81% and specificity was 50% (P= 0.110). The PPV was 85.71%, and the NPV was 42,86%.
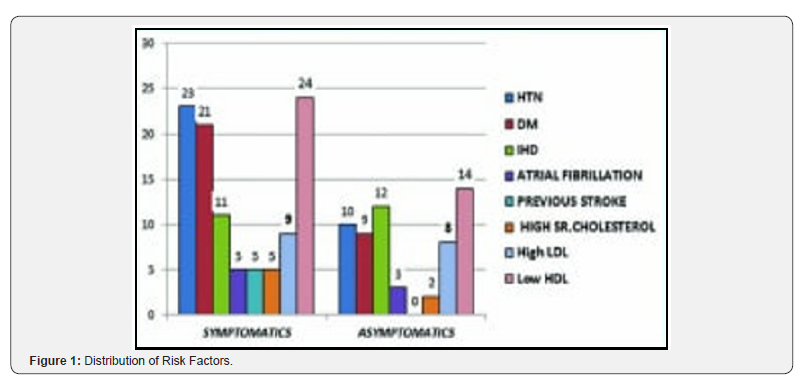
(Figure 1) In symptomatic patients, majority of them had 23 Hypertension (HTN), 21 (Diabetes Mellitus) DM, 24 Low HDL (High-Density Lipoprotein) followed by 11 Ischemic Heart Disease (IHD). 9 patients had High LDL (Low-Density Lipoprotein), 5 patient had Atrial Fibrillation, 5 patients with history of Stroke, and 5 had High Serum Cholesterol. In asymptomatic patients, 14 patients had high degree of Low HDL, followed by 12 had IHD. 10 patients had HTN, 9 had DM and 8 had High LDL (Low-Density Lipoprotein). Furthermore, 3 patients had Atrial Fibrillation, 2 patients were suffering from High Serum Cholesterol (Figure 2).
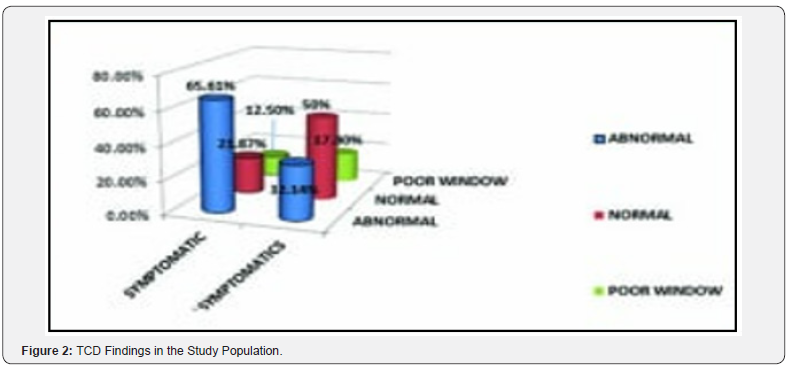
The TCD findings of the symptomatic patients show that 65.62% have abnormal TCD, and 21.88% have normal TCD, 12.50% have a poor window period, so they are not added to the study analysis. Whereas, in asymptomatic patients, 50% of them have normal TCD and 32.18% have abnormal TCD, 17.22% have a poor window period, so they were not included in the study (Figure 3).
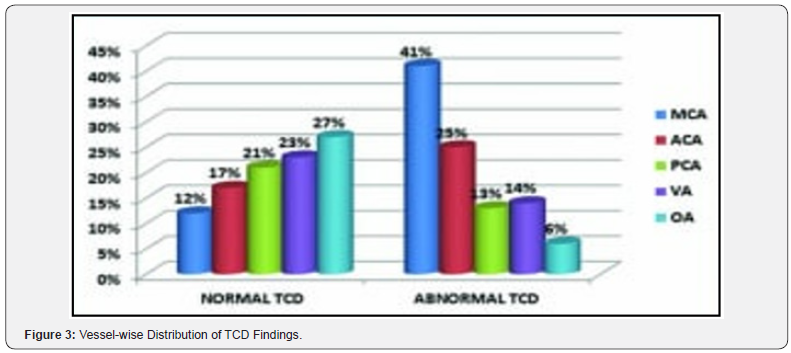
If we look at vessel-wise distribution, abnormal TCD group had 41% MCA, 25% ACA (Anticardiolipin), 13% PCA (Patient- Controlled Analgesia), 14% VA (Ventriculo-Atrial) and 6% OA (Osteoarthritis). Whereas normal TCD group had 27% OA, 23% VA, 21% PCA, 17% ACA and 12% MCA (Figure 4).
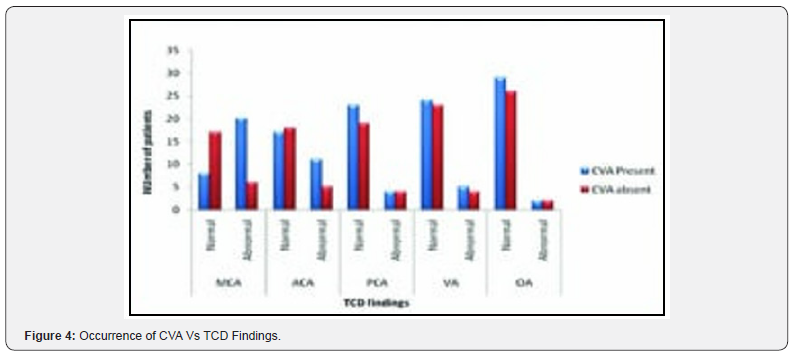
In the normal MCA group, the occurrence of CVA was present in 7 patients and absent in 17 patients. Whereas in the abnormal MCA group, the occurrence of CVA was present in 20 patients and absent in 5 patients. In the normal ACA group, the occurrence of CVA was present in 16 patients and absent in 17 patients. Whereas in the abnormal ACA group, the occurrence of CVA was present in 10 patients and absent in 5 patients. In the normal PCA group, the occurrence of CVA was present in 24 patients and absent in 19 patients. Whereas in the abnormal PCA group, the occurrence of CVA was present in 4 patients and absent in 4 patients In the normal VA group, the occurrence of CVA was present in 24 patients and absent in 23 patients. Whereas in the abnormal VA group, the occurrence of CVA was present in 5 patients and absent in 4 patients. In the normal OA group, the occurrence of CVA was present in 29 patients and absent in 26 patients. Whereas in the abnormal OA group, the occurrence of CVA was present in 2 patients and absent in 2 patients.
Discussion
TCD provides understanding regarding various intracranial and extracranial disorders and their detrimental effects on cerebral hemodynamic, which is impossible to find with other diagnostic and imagining techniques. It is very helpful for noninvasive examination of intracranial arteries for quantifying and detecting stenosis (8). It was found that the risk factors like low HDL, HTN and DM was higher in symptomatic patients as compared to asymptomatic patients. Hypertension is considered one of the major risk factors for CVA (9), which is similar to the findings of some other studies (9-11). It was found that symptomatic patients have a higher percentage of abnormal TCD compared to asymptomatic patients indicating either hyperemic status due to chronic anaemia or arterial stenosis (12). According to vessel-wise distribution of TCD findings, it was seen that MCA and ACA were higher in abnormal TCD compared to normal TCD, whereas, PCA, VA, and OA were higher in normal TCD compared to that of abnormal TCD. Furthermore, there is a high occurance of CVA in TCD findings of abnormal MCA, abnormal ACA, normal PCA, normal VA, and normal OA, compared to their contrary.
Conclusion
TCD is a very useful technique for the treatment of elderly patients with CVA. It can be used to determine the stroke conditions, mainly those mechanisms related to intracranial or extracranial arterial disease, which further helps in the exceptional treatment of those diseases. The capability of TCD to detect the blood flow over a long period helps accurately detect the stroke. Asymptomatic elderly patients with significant intracranial artery stenosis or occlusion can be rendered with early intervention in prevention of CVA. Due to its non-invasive nature routine testing and close follow-up are possible. Although MRA remains the golden standard for diagnosing CVA, the rapid technological advances in this procedure make this tool more reliable and help it increase its use.
References
- American Association of Neurological Suergons. Cardiovascular disease
- Cleveland Clinic. Transcranial Doppler Ultrasound (Ultrasonography Test)
- Yuanmei Pan, Wenbin Wan, Minjie Xiang (2022) Transcranial Doppler Ultrasonography as a Diagnostic Tool for Cerebrovascular Disorders
- Andres Fabricio Caballero-Lozada, Kapil Laxman Nanwani, Favio Pavon (2020) Clinical Applications of Ultrasonography in Neurocritically Ill Patient
- Cesare Fieschi, Corrado Argentino, Gian Luigi Lenzi, (1989) Clinical and instrumental evaluation of patients with ischemic stroke within the first six hours
- Wijman C A C, Babikian V L, Matjucha I C A.et alCerebral microembolism in patients with retinal ischaemia. Stroke 1998291139–1143
- M. Sprafka, B.A. Virnig, E. Shahar (1994) Trends in Diabetes Prevalence Among Stroke Patients and the Effect of Diabetes on Stroke Survival: the Minnesota Heart Survey
- Sanjukta Sarkar, Sujoy Ghosh, Sandip Kumar Ghosh (2007) Role of transcranial Doppler ultrasonography in stroke
- Saha MS, Sana NK, Shaha RK. Serum lipid profile of hypertensive patients in the northern region of Bangladesh. J Bio-Sci. 2006; 14: 93–98
- Anjum R, Zahra N, Rehman K, et al. Comparative Analysis of Serum Lipid Profile between Normotensive and Hypertensive Pakistani Pregnant Women. J Mol Genet Med. 2013;7:64
- Bambara R, Mittal Y, Mathur A. Evaluation of Lipid Profile of North Indian Hypertensive Subjects. Asian Journal of Biomedical and Pharmaceutical Sciences. 2013;3:38–41
- Walaa Ismail Musa Ismail, Mustafa Elnour, Alam Eldin Musa Mustafa Evaluation of transcranial Doppler abnormalities in children with sickle cell disease in El-Obeid Specialized Children's Hospital. 2019. 8(3): 1176–1181






























