Treatment of Distal Posterior Cerebral Artery Aneurysm Utilizing Flow Diverter Device: Technical Report
Andrew Dennison1, Sruthi Konduro2, Mahmoud Abbas1*, Anas S Al-Smadi3, Marisa Smitt4, and Ali Luqman4
1Department of Radiology, Wayne State University, School of Medicine, Detroit, MI, USA
2Department of Neurology, Wayne State University, School of Medicine, Detroit, MI, USA
3Department of Radiology, University of Chicago Medical Center, Chicago, IL, USA
4Department of Neurosurgery, Wayne State University, School of Medicine, Detroit, MI, USA
Submission: November 18, 2022; Published: November 28, 2022
*Corresponding author: Mahmoud Abbas, Department of Radiology, Wayne State University, School of Medicine, Detroit, MI, USA
How to cite this article: Andrew D, Sruthi K, Mahmoud A, Anas S A-S, Marisa S. Treatment of Distal Posterior Cerebral Artery Aneurysm Utilizing Flow Diverter Device: Technical Report. Open Access J Neurol Neurosurg 2022; 17(4): 555969.DOI: 10.19080/OAJNN.2022.17.555969.
Abstract
Although distal posterior cerebral artery (PCA) aneurysms are rare entities, they present a treatment challenge due to their deep anatomic location, complex surrounding neuroanatomic structures, higher incidence of fusiform and large saccular aneurysms, saccular aneurysms are more likely dissecting in origin which are unstable with higher rate of dilatation and hemorrhage, in addition to association with other vasculopathies like vasculitis, Arteriovenous malformations (AVMs) and Moyamoya. Of the available management options, endovascular treatment has become the mainstay of treatment. Recent advance in flow diverters has led to increasing utilization of these devices in the treatment of various aneurysms including PCA. In this study, we describe our technical notes in the off-label utilization of Pipeline embolization device (PED) in the treatment of distal PCA aneurysms.
Keywords: Cerebral Artery; Arteriovenous Malformations; Moyamoya; Neuroanatomic Structures; Cerebrovascular
Introduction
Aneurysm of the distal posterior cerebral artery is a rare and challenging entity to treat due to its characteristics, deep anatomical location and surrounding complex neuroanatomic structures. Treatment options of distal PCA aneurysms include surgical clipping, parent vessel occlusion (PVO) and endovascular treatment. Among these, endovascular management with flow diverter stents has been increasingly utilized recently with good outcomes. In this study, we describe our technical observations in the treatment of a P3 aneurysm utilizing PED.
Case Report
A 63-year-old male with a history of multiple cerebrovascular accidents (CVAs) resulting in residual left-sided weakness, seizure disorder, multiple cerebral aneurysms status post coiling and clipping, was brought in by family due to progressive decline in mentation over the course of few weeks. At baseline, patient is alert and oriented x 3, lives in a nursing home, non-ambulatory with left sided weakness and contractures.
The patient has a significant history of multiple aneurysms, for which he had right carotid terminus/M1 stent and right V4 vertebrobasilar stent assisted coils placed (Neuroform EZ and Target coils). Previous angiograms also denote numerous small aneurysms and blister like changes within the basilar artery with concerns for cerebral vasculitis.
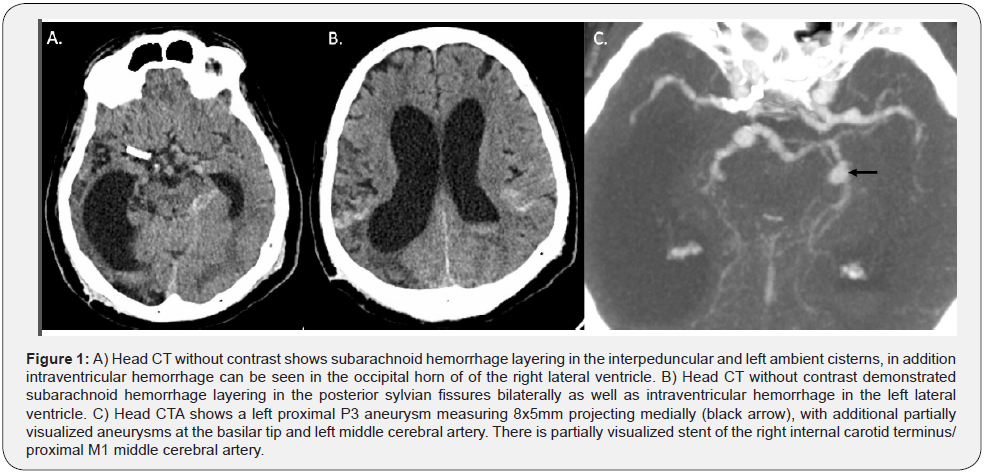
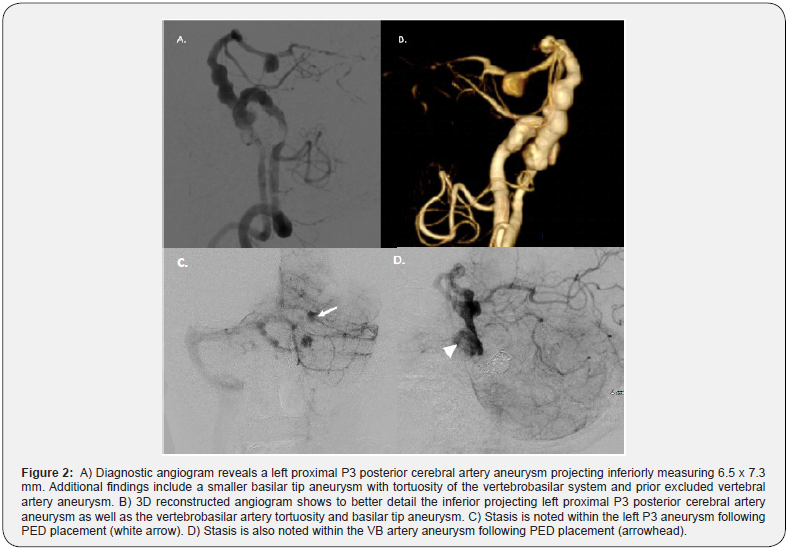
On presentation to the emergency department, he was found to have subarachnoid hemorrhage (SAH) layering in the interpeduncular and left ambient cisterns, sylvian fissures, as well as intraventricular hemorrhage and hydrocephalus (Figures 1 & 2). On CTA, there was evidence of prior stenting and coiling of multiple aneurysms, as well as an 8 x5 mm inferiorly projecting aneurysm of the left P3 posterior cerebral artery (Figure 1). Patient underwent an emergent ventriculoperitoneal (VP) shunt with improvement in mentation. Due to enlarging left P3 aneurysm and likely etiology for hemorrhage, potential benefits and risks were discussed with patient and family, it was decided to proceed with pipeline embolization due to prior stent coiling. Diagnostic angiogram revealed a large left proximal P3 6.5 x 7.3 mm sidewall aneurysm, a small 2 mm basilar tip aneurysm, and very irregular basilar artery below the anterior inferior cerebellar artery (AICA) vessels with several small blebs and severe tortuosity (Figure 2A & B).
Technique
The procedure was performed under general endotracheal anesthesia. Femoral vascular access was obtained using 6F sheath. Heparin was given intravenously to maintain therapeutic activated clotting time and checked hourly. Using fluoroscopic guidance, selective catheterization angiogram was done of the left common femoral artery and left vertebral artery. Guide catheter (neuron) was advanced to the V3 segment of left vertebral artery over a Bernstein catheter with 0.038” glide advantage wire due to type III arch and proximal tortuosity. The marksman was placed over the Synchro 2 ST wire into the distal P4 PCA past the large 6.5 x 7.3 mm P3 sidewall aneurysm. The PCA diameter was measured 1.9 mm proximal and distal to the aneurysm. Due to a great deal of tortuosity, required Synchro ST versus soft micro wire under working views. The Neuroform stent at the Vertebrobasilar (VB) junction from a previous aneurysm intervention at that site was difficult to pass given possible in-stent stenosis near this site or irregular wall apposition. After crossing, 2.5 x 10 mm PED was deployed under fluoroscopic guidance in the P3 segment of the left PCA just covering the aneurysm neck on both sides. The lead wire was then retrieved more proximal into the lower basilar artery past the Neuroform stent below the AICA vessels.
For the treatment of the enlarging VB aneurysm, a second PED was deployed using push and pull technique with 5 mm distal overlap of the Neuroform stent ending below the PICA takeoff. The first attempt with deploying 4.25 x 35 mm PED without intermediate catheter failed given proximal movement from the landing zone due to tortuosity. Therefore, a Sofia intermediate catheter was used for the VB junction 4.5x35 mm PED deployment. Post-procedure angiogram showed good intra-aneurysmal flow stasis at both left P3 sidewall aneurysm and VB junction aneurysm (Figure 2C & D). Small basilar tip aneurysm remains, as does diffuse vasculopathic changes with numerous vessel irregularities within the basilar and PCA arteries. Patient tolerated the procedure well, total procedure time was approximately 3 hours with return to baseline function. Follow up CTA revealed stability to the multiple stents, coiled aneurysms, and remaining aneurysms (Figure 3). Follow up angiogram showed significantly smaller PCA aneurysm and successful flow diversion at the VB junction (Figure 4).

Discussion
Aneurysms of the PCA represent a rare and a challenging entity to treat. They tend to have specific characteristics when compared to cerebral aneurysms elsewhere including predilection to involve proximal segments (P1 and P2), higher incidence of fusiform and large saccular aneurysms, saccular aneurysms are more likely dissecting in origin which are unstable with higher rate of dilatation and hemorrhage, in addition to association with other vasculopathies like vasculitis, AVMs and Moyamoya [1-4].
Due to the complexity of PCA aneurysm location, difficult to reach surgically especially in the distal segments, higher rate of large or unclippable aneurysms, and reinforced by recent advancements in endovascular techniques and devices [5-8], endovascular treatment has become the mainstay of management. Deconstructive (parent vessel occlusion) and reconstructive (selective coiling and flow diverting stents) techniques have both been utilized in the treatment of PCA aneurysms and proved to be effective with high occlusion (70-100%) and low complication rate (0-15%) [3,4,7,9,10]. Selection of whichever technique should consider aneurysm size, complexity, location and knowledge of anatomic variants. However, preservation of vessel anatomy should be the main goal to maintain the antegrade flow [3,4,9].

Flow diverters, including PED used in our case, have been increasingly utilized in off-label indications and operators have become more familiar and comfortable deploying FDs in unfavorable anatomy [11]. Given less perforators originating from the distal segments, endovascular treatments are expected to have lower complication rate [3]. The patient described in our case had, besides the hemorrhagic complication, seizure disorder which was reported in the literature to be associated with PCA aneurysms [4]. The aneurysm arises from P3 segment and saccular in morphology, which is likely dissecting in nature as previously discussed and more likely to expand, already presented with bleeding, in addition to associated vasculopathy. Therefore, decision was made to secure this aneurysm and an enlarging VB aneurysm among other ones the patient already have. The extremely tortuous and vasculopathic arteries which increase suspicion of underlying vasculitis disorder, in addition to the distal location, made intervention particularly challenging. Another challenge was the previously treated VB junction aneurysm with Neuroform stent complicated with in stent stenosis. This required exchanging Synchro soft to ST micro-wire, extreme care while advancing devices and maintain activated Partial Thromboplastin Time (aPTT) within therapeutic level to avoid micro-thrombi distally. Care also should be taken while advancing the microcatheter over the micro-wire into the distal smaller arterial segments to avoid dissection. The PCA diameter proximal and distal to the aneurysm was 1.9 mm, which was deemed sufficient to deploy PED [3]. We chose Marksman microcatheter (without intermediate catheter) for the delivery of PED and was advanced into P4 segment. However, we needed to use Sofia intermediate catheter to provide stability while deploying PED overlapping with the previously placed Neuroform to treat the enlarging VB junction aneurysm. Of the limitations and challenges of utilizing flow diverters in distal PCA segments are the extremely small and tortuous vessels, the risk of stenosis and thrombosis which require placing the patient on dual antiplanets that can increase the risk of hemorrhage especially in old patients with multiple comorbidities and risk of recurrent falls.
Conclusion
Distal PCA aneurysms are rare and challenging entities to treat. The use of FDs has been proven to be safe and effective in the treatment of distal PCA aneurysms especially in unfavorable anatomy.
References
- Goehre F, Jahromi BR, Hernesniemi J, Elsharkawy A, Kivisaari R, et al. (2014) Characteristics of posterior cerebral artery aneurysms: an angiographic analysis of 93 aneurysms in 81 patients. Neurosurgery 75(2): 134-144.
- Kobkitsuksakul C, Somboonnitiphol K, Apirakkan M, Lueangapapong P, Chanthanaphak E (2020) Dolichoectasia of the internal carotid artery terminus, posterior communicating artery, and posterior cerebral artery: The embryonic caudal ramus internal carotid segmental vulnerability legacy. Interv Neuroradiol J peritherapeutic Neuroradiol Surg Proced Relat Neurosci 26(2): 124-130.
- Hou K, Lv X, Yu J (2022) Endovascular Treatment of Posterior Cerebral Artery Trunk Aneurysm: The Status Quo and Dilemma. Front Neurol 12: 746525.
- Ciceri EF, Klucznik RP, Grossman RG, Rose JE, Mawad ME (2001) Aneurysms of the posterior cerebral artery: classification and endovascular treatment. AJNR Am J Neuroradiol 22(1): 27-34.
- Onekura MY, Agata IN (2004) Aneurysms of the Posterior Cerebral Artery: Retrospective Review of Surgical Treatment. Neurol Med Chir (Tokyo) 44(4): 164-169.
- Hallacq P, Piotin M, Moret J (2002) Endovascular occlusion of the posterior cerebral artery for the treatment of p2 segment aneurysms: retrospective review of a 10-year series. AJNR Am J Neuroradiol 23(7): 1128-1136.
- Dossani RH, Smolar D, Waqas M (2020) Role of parent artery sacrifice in the treatment of posterior cerebral artery aneurysms. Neurol India 68(2): 325-326.
- Liu L, He H, Jiang C, Lv X, Li Y (2011) Deliberate parent artery occlusion for non-saccular posterior cerebral artery aneurysms. Interv Neuroradiol J peritherapeutic Neuroradiol Surg Proced Relat Neurosci 17(2): 159-168.
- Awad AJ, Mascitelli JR, Haroun RR, De Leacy RA, Fifi JT, et al. (2017) Endovascular management of fusiform aneurysms in the posterior circulation: the era of flow diversion. Neurosurg Focus 42(6): E14.
- Wallace AN, Grossberg JA, Almandoz JED, Kamran M, Anil K, et al. (2018) Endovascular Treatment of Posterior Cerebral Artery Aneurysms With Flow Diversion: Case Series and Systematic Review. Neurosurgery 83(4): 790-799.
- Brouillard AM, Sun X, Siddiqui AH, Lin N (2016) The Use of Flow Diversion for the Treatment of Intracranial Aneurysms: Expansion of Indications. Cureus 8(1): 1-8.






























