Functional Outcomes in Patients with Hemorrhagic Stroke during SARS-CoV-2 Pandemic. A Descriptive Study
Emilio Rubén Pego Pérez1*, Lourdes Bermello López2, Isidoro Rodríguez Pérez3, María del Rosario Marín Arnés2 and Eva Gómez Fernández2
1Department of Psychiatry, Radiology, Public Health, Nursing and Medicine, University of Santiago de Compostela, Spain
2Nursing staff of neurology area of Lucus Augusti University Hospital, Spain
3Nursing School of Lugo, University of Santiago de Compostela, Spain
Submission: August 18, 2022; Published: August 26, 2022
*Corresponding author: Emilio Rubén Pego Pérez, Department of Psychiatry, Radiology, Public Health, Nursing and Medicine, University of Santiago de Compostela, Spain
How to cite this article: Pego Pérez ER, Bermello López L, Rodríguez Pérez I, Marín Arnés MR, Gómez Fernández E, et al. Functional Outcomes in Patients with Hemorrhagic Stroke during SARS-CoV-2 Pandemic. A Descriptive Study. Open Access J Neurol Neurosurg 2022; 17(3): 555963.DOI: 10.19080/OAJNN.2022.17.555963.
Abstract
Background: Stroke is the second leading cause of death worldwide and one of the leading causes of disability in adults. About 85% of them will be ischemic, and the other 15%, hemorrhagic stroke. Evidence suggested that COVID-19 patients may experience increased rates of thromboembolism and the risk of a hemorrhagic stroke.
Aim: to determine the functional outcomes in patients with hemorrhagic stroke during the SARS-CoV-2 pandemic.
Methods: a descriptive and retrospective study that included a sample of 92 patients with acute hemorrhagic stroke. The functional outcomes were measured with Barthel Index.
Results: The distribution in the moderate and severe degrees has been higher for the year 2019, in the independent and minimal help required degrees it has been higher in the year 2020. No significant correlation was found between age and the categorized Barthel Index, not between the year and the categorized Barthel Index.
Conclusion: No relationship is seen between the SARS-CoV-2 pandemic and worsening of functionality. The structural changes during the pandemic and the reduction in personnel have not affected the diagnosis and involvement of ischemic stroke. The effort of the staff, to maintain adequate care, has been decisive in the functional results of the patients.
Keywords: Acute hemorrhagic stroke; IADL; Autonomy; Barthel index; Outcomes; Quality of Life; SARS-CoV-2
Background
Stroke is the second leading cause of death worldwide and one of the leading causes of disability in adults. Despite currently available treatment options for stroke, patients often face the potential for significant post-stroke disability. About 85% of them will be ischemic, and the other 15%, hemorrhagic stroke [1,2]. Stroke represents the second cause of death in Spain. Hospital mortality from stroke ranges between 8% and 14% depending on age, severity of stroke, prior functionality, as well as associated disease. The prevalence in Spain is around 4-8% in people over 65 years of age. The risk of suffering a stroke is especially increased in the population > 65 years of age, with 75% suffering from strokes and more frequent in the group of women than in the group of men. Regarding age and groups, the risk of suffering a stroke in women is 74.6 ± 11.4 years and in men it is 68.8 ± 11.9 years [3,4].
Stroke incidence and prevalence rates have been reported to be high and approximately 90% of stroke survivors have some type of disability. If a person suffers a stroke, mortality rises to 73% and the probability of being dependent rises to 39% [2,5]. At 6 months of follow-up, 26.1% of patients die, 41.5% achieve an independent life and 32.4% are dependent. Of those who are independent, approximately 44% suffer from a functional dependency. The first six months after stroke are critical for rehabilitation with the goal of returning the individual to a satisfactory level of participation [6,7]. Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) was identified in December 2019 and caused a global pandemic of coronavirus disease 2019 (COVID-19). At the beginning of 2021, more than 110 million people have been infected, with more than 60 million recovered and nearly 2.5 million deaths [6,8,9].
All non-urgent clinical activities were suspended. Operating theaters were converted to intensive care units and several health professionals moved to COVID wards to support their colleagues, retired staff returned to work to overcome staff shortages, several health professionals moved out of their homes, even so, many of them became infected or even died [9]. During the acute phase of the pandemic, studies highlighted a reduction in stroke admissions, but there were accumulating reports of acute cerebrovascular diseases, including hemorrhagic stroke. Reviews showed an association between cerebrovascular diseases and increased severity and mortality of COVID-19, others reviewed the spectrum of neurological manifestation in COVID-19 [10]. Evidence suggested that COVID-19 patients may experience increased rates of thromboembolism and the risk of a hemorrhagic stroke. The possible mechanisms underlying hemorrhagic stroke in COVID-19 patients included the expression of angiotensin converting enzyme 2, immunity, inflammation, endothelial dysfunction at the blood-brain-barrier aging, stress, and anxiety [11].
Thus, the objective of this article is to determine the functional repercussion in patients with hemorrhagic stroke during the SARS-CoV-2 pandemic.
Methods
Study Design and patients
This is a retrospective study of consecutive patients with ischemic stroke at our institution between January 2019 to May 2021.
Patient selection
Inclusion criteria were hemorrhagic stroke, age > 18 years.
Exclusion criteria were as follows: Pregnant patients.
Variables and data collection
Demographics: age; gender; start date of the study (dd/mm/ yyyy) and Barthel index.
Imaging evaluation
At admission and after a clinical evaluation by a neurologist, most patients underwent a baseline CT scan, supra-aortic and cerebral CT angiography, and cerebral perfusion CT. The other patients underwent to MRI.
Study Outcomes
Clinical outcomes were measured with Barthel Index considering: Unable to perform task (<20 points), attempts task but unsafe (20-35 points), moderate help required (40-55 points), minimal help required (60-95 points) and fully independent (100 points).
Statistical and Data Analysis
A descriptive analysis was carried out using measures of central tendency (mean (M)) and dispersion (standard deviation (SD) when it was considered appropriate for quantitative variables), and percentages (for qualitative variables). The Chi2 test was used for the qualitative variables to analyze the differences between groups. A significance level of 0.05 was chosen. All analyses and calculations were performed using the statistical package PASW (v. 24.0; SPSS Inc., Chicago, Illinois).
Results
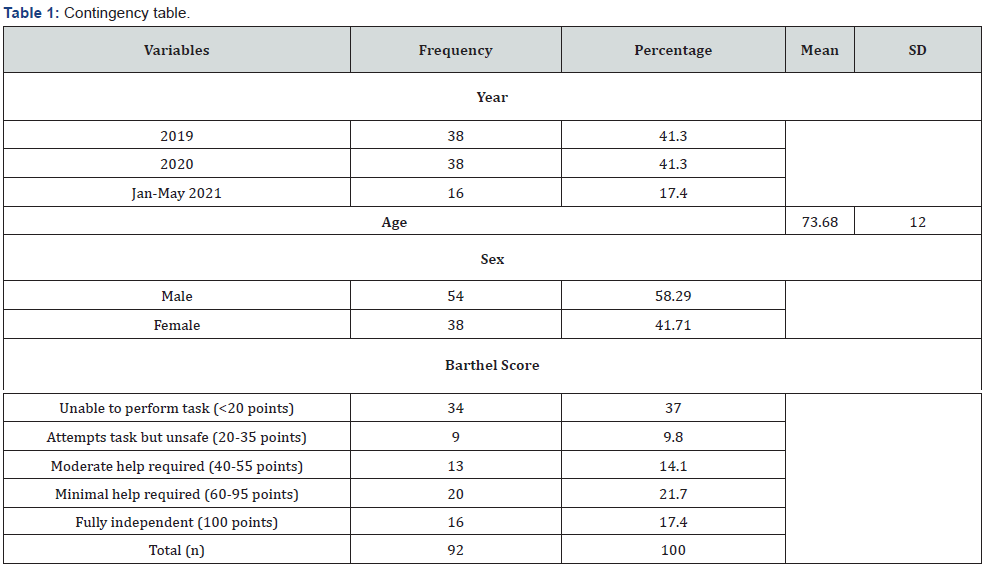
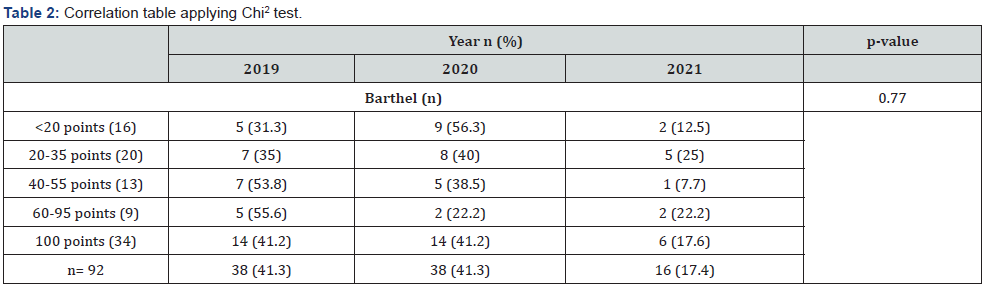
The number of patients with hemorrhagic stroke in 2019 was of 38 patients; in 2020 it was 38 and from January to May 31, 2021, it was 16 patients. The characteristics of the sample were included at a contingency table (Table 1). The distribution in the moderate and severe degrees has been higher for the year 2019, in the independent and minimal help required degrees it has been higher in the year 2020, for the degree of unable to perform task it has been similar in proportion beside the three years (Table 2). No significant correlation was found between sex or age and the result of the Barthel scale, and not between the year in which the hemorrhagic stroke occurred and the result of the Barthel scale (Table 2).
Discussion
The functional outcomes, of the patients after suffering a stroke, was classically established in three periods [2,4]. An acute period that included from the onset of symptoms to hospital discharge; a subacute period in which was a progressive functional improvement, which continues in most cases during the first 3-6 months and finally, a chronic period or functional stabilization [2,3]. Most attention to stroke patients has commonly focused on the acute phase, where recent efforts and medical advances have managed to reduce morbidity and mortality. However, studies focused on the subacute phase are less frequent, and few studies focus on longer-term evolution [6]. In relation to the subacute phase, the evaluation of the functional status of the Instrumental Activities of Daily Living (IADL) is recorded in only 24.6% of the cases at discharge and for six months after the episode in the primary care database; functional status after stroke is a predictor of long-term mortality [12]. In this study, the total number of admissions for ischemic stroke in 2019 was 38 patients; in 2020 it was 38 patients and from January to May 31, 2021, it was 16 patients. About 58% of the sample was male. The number of admitted patients couldn’t change between the years analyzed.
The mean age in this study was 73.68 years (SD: 12.43 years). The results in relation to age compared to other studies were higher. One article determined that the median age was 65.3 (CI: 61.4-67.6) years, and the majority was male (62.4%) [10]. Zhu & Jiang [13], determined a mean of age lower than the results of this article, 53 years (SD= 12 years old). An article revised twenty-four observational cohort studies that reported the incidence of acute cerebrovascular disease in COVID-19 patients ranging from 0.4 to 8.1%; there were a total of 108,571 COVID-19 patients, of which ischemic or hemorrhagic stroke was reported in 1106 patients, in Asia 3.1% (95% CI: 1.9-5.1), in Europe 1.2% (CI: 0.7-1.9) and in North America 1.1% (CI: 0.8-1.4). At the same article, they founded in 202 patients in China, a mean of BI in 54.4 points (SD: 29.5), a mean of age in 53.0 (SD: 12.0) years and 94 males with hemorrhagic stroke [13].
In different continents, a systematic review and metaanalysis determined in 1912 patients that the median age was 65.3 (CI: 61.4-67.6) years, and the majority was male (62.4%), that COVID-19 patients that developed acute cerebrovascular disease were older and that there was no sex difference. Stroke in COVID-19 patients was associated with more severe infectious disease [10]. In other review and meta-analysis founded that the pooled rates of hemorrhagic strokes among hospital admissions of patients infected by SARS-CoV-2 were 0.2% (95% CI). Among SARS-CoV-2–infected patients admitted to neurological wards, 5.4% were diagnosed with hemorrhagic stroke. Patients suffering from cerebrovascular events were found to have higher odds for in-hospital mortality when infected with SARS-CoV-2 compared to their contemporary noninfected or historical counterparts [14].
Another systematic review and meta-analysis showed that hemorrhagic stroke was reported in 18 studies including 67,155 patients infected by SARS-CoV-2, with a pooled estimate of prevalence of 0.46% (95% CI: 0.40–0.53). The incidence of hemorrhagic stroke, in an article included in the review with a sample of 760 patients with COVID-19, was 28.42%. Finally, the mortality rate of COVID-19 patients who experienced hemorrhagic stroke was 44.72% [11]. Patient functionality after stroke is significantly associated with the likelihood of hospital readmission and is an important outcome to consider in stroke, especially considering recent Medicare avoidable readmission policies. Patients with poor function, at the time of discharge, are also more likely to need long-term care and intensive rehabilitation plans, which implies a greater financial impact and more serious consequences for the family of the stroke survivor [6,15]. Previous research has described autonomy as the ability to make decisions, feel in control of the activities in which to participate and how these activities are carried out, it is important to consider this concept since the objective was to capture the quality of participation rather than of only the frequency in the activities [6,16].
Functionality has become a broad term that includes the interaction of positive aspects between the 3 main components of the International Classification of functioning (ICF): body functions and structures; activity and participation; and environmental and personal factors. With this model, the environment is viewed as either a facilitator or a barrier to functional recovery [5,6]. The distribution in the Barthel Index (BI) categorized was 34 patients for unable to perform task (<20 points); of 9 patients for attempts task but unsafe (20-35 points); of 13 patients for moderate help required (40-55 points); of 20 patients for minimal help required (60-95 points) and 16 patients for fully independent (100 points). Regarding the functional outcomes by years, the frequencies by degrees of affection were for the year 2019 about 36.84% for unable to perform task (<20 points), 13.15% for attempts task but unsafe (20-35 points), 18.42% for moderate help required (40-55 points), 18.42% for minimal help required (60-95 points) and 13.15% for fully independent (100 points). For the year 2020 about 36.84% for unable to perform task (<20 points), 5.26% for attempts task but unsafe (20-35 points), 13.15% for moderate help required (40-55 points), 11.05% for minimal help required (60-95 points) and 23.68% for fully independent (100 points). Finally, for the year 2021 it was about 37.5% for unable to perform task (<20 points), 12.5% for attempts task but unsafe (20-35 points), 6.25% for moderate help required (40-55 points), 31.25% for minimal help required (60-95 points) and 12.5% for fully independent (100 points).
One article determined that the incidence of hemorrhagic stroke among all stroke types in COVID-19 patients fluctuated, about 12.2% in May 2020, 9.7% in June 2020, 17.2% in July 2020, 11.6% in September 2020, and 28.42% in November 2020 [11]. Articles suggested that a BI score ≧90 was the optimal cutoff score to define a favorable outcome, but recent articles have reported that BI ≧75 could be used to define a favorable outcome in acute stroke patients [6,17]. The challenge for stroke research lies in increasing knowledge of long-term functional outcomes, these being increasingly important for planning health service resources, providing evidence-based rehabilitation after acute care settings, also provide information for survivors and their families [4,6,18].
Conclusion
The structural changes during the pandemic and the reduction in personnel have not affected the diagnosis and involvement of hemorrhagic stroke. The effort of the staff to maintain adequate care has been decisive in the functional outcomes of the patients.
References
- Feigin VL, Bennett DA, Barker CSL, Parag V (2009) Worldwide stroke incidence and early case fatality reported in 56 population-based studies: a systematic review. Lancet Neurol 8(4): 355-369.
- Pego PER, Fernández RI, Pumar CJM (2019) National Institutes of Health Stroke Scale, modified Rankin Scale, and modified Thrombolysis in Cerebral Infarction as autonomy predictive tools for stroke patients. Reviews in the neurosciences 30(7): 701-708.
- Durà MMJ, Molleda MM, García AC, Mallol BJ, Calderón PV (2011) Factores pronósticos en el ictus. De la fase aguda a los tres años. Rehabilitación (Madr) 45(1): 18-23.
- Pego PER, Fernández RI, Pumar CJM (2021) Autonomy results in post-mechanical thrombectomy applied to patients with stroke a retrospective study. Open access journal of Neurology and Neurosurgery, 16(1): 1-8.
- Silva SM, Corrêa FI, Coelho DC, Buchalla CM, da Costa PF, et al. (2015) Evaluation of post-stroke functionality based on the International Classification of Functioning, Disability, and Health: a proposal for use of assessment tools. J Phys Ther Sci 27(6): 1665-1670.
- Pego PER, Bermello LL, Marín AMR, Gómez FE, Núñez HMI, et al. (2022) Autonomy Outcomes Measured with Barthel Index in Patients with Ischaemic Stroke during SARS-CoV-2 Pandemic. A Descriptive Study. Open access journal of Neurology and Neurosurgery 17(3): 1-7.
- Saqqur, M, Tsivgoulis, G, Molina CA, Demchuk AM, Siddiqui M, et al. (2008) Symptomatic intracerebral hemorrhage, and recanalization after IV rt-PA A multicenter study. Neurology 71(17): 1304-1312.
- Bardenheier BH, Gravenstein S, Blackman C, Gutman R, Sarkar IN, et al. (2021) Adverse events following mRNA SARS-CoV-2 vaccination among US nursing home residents. Vaccine 39(29): 3844-3851.
- Chen M, Yuan Y, Zhou Y, Deng Z, Zhao, et al. (2021) Safety of SARS-CoV-2 vaccines: a systematic review and meta-analysis of randomized controlled trials. Infectious diseases of poverty 10(1): 1-12.
- Nannoni S, de Groot R, Bell S, Markus HS (2021) Stroke in COVID-19: a systematic review and meta-analysis. International Journal of Stroke 16(2): 137-149.
- Syahrul S, Maliga HA, Ilmawan M, Fahriani M, Mamada SS, et al. (2021) Hemorrhagic and ischemic stroke in patients with coronavirus disease 2019: incidence, risk factors, and pathogenesis - a systematic review and meta-analysis. F1000Research 10: 34.
- Goyal M, Fargen KM, Turk, AS, Mocco, J, Liebeskind, DS, et al. (2014) 2C or not 2C: defining an improved revascularization grading scale and the need for standardization of angiography outcomes in stroke trials. J Neurointer Surg 6(2): 83-86.
- Zhu W, Jiang Y (2019) Determinants of quality of life in patients with hemorrhagic stroke: A path analysis. Medicine 98(5): e13928.
- Katsanos AH, Palaiodimou L, Zand R, Yaghi S, Kamel H, et al. (2021) The impact of SARS‐CoV‐2 on stroke epidemiology and care: a meta‐ Annals of neurology 89(2): 380-388.
- Nichols C, Carrozzella J, Yeatts S, Tomsick T, Broderick J, et al. (2018) Is periprocedural sedation during acute stroke therapy associated with poorer functional outcomes? Journal of neurointerventional surgery 10(Suppl 1): i40-i43.
- Törnbom K, Hadartz K, Sunnerhagen KS (2018) Self-perceived participation and autonomy at 1-year post stroke: a part of the stroke arm longitudinal study at the University of Gothenburg (SALGOT Study). Journal of Stroke and Cerebrovascular Diseases 27(4): 1115-1122.
- Zhou M, Liu X, Zha F, Liu F, Zhou J, et al. (2021) Stroke outcome assessment: Optimizing cutoff scores for the Longshi Scale, modified Rankin Scale and Barthel Index. Plos one 16(5): e0251103.
- Blomgren C, Jood K, Jern C, Holmegaard L, Redfors P, et al. (2018) Long-term performance of instrumental activities of daily living (IADL) in young and middle-aged stroke survivors: Results from SAHLSIS outcome. Scandinavian journal of occupational therapy 25(2): 119-126.






























