Autonomy Outcomes Measured with Barthel Index in Patients with Ischaemic Stroke during SARS-CoV-2 Pandemic. A Descriptive Study
Emilio Rubén Pego Pérez1*, Lourdes Bermello López2, María del Rosario Marín Arnés2, Eva Gómez Fernández2, María Irene Núñez Hernández2 and Isidoro Rodríguez Pérez3
1Department of Psychiatry, Radiology, Public Health, Nursing and Medicine, University of Santiago de Compostela, Spain
Faculty of Nursing, Avenida Xoán XXIII s/n, 15704, Santiago de Compostela, Spain
Hospital Hestia La Robleda. Mental Health Department, O Pino, Spain
Research group GI Dependence, Gerontology and Geriatry, University of Santiago de Compostela, Santiago de Compostela, Spain
2Nursing staff of neurology area of Lucus Augusti Universitary Hospital, Spain
3Nursing School of Lugo, University of Santiago de Compostela, Spain
Submission: July 08, 2022; Published: July 26, 2022
*Corresponding author: Emilio Rubén Pego Pérez, Department of Psychiatry, Radiology, Public Health, Nursing and Medicine, University of Santiago de Compostela, Spain
How to cite this article: Pego Pérez ER, Bermello López L, Marín Arnés MR, Gómez Fernández E, Núñez Hernández MI, et al. Autonomy Outcomes Measured with Barthel Index in Patients with Ischaemic Stroke during SARS-CoV-2 Pandemic. A Descriptive Study. Open Access J Neurol Neurosurg 2022; 17(3): 555961.DOI: 10.19080/OAJNN.2022.17.555961.
Abstract
Background: Acute stroke is the 3rd cause of mortality, the 1st in disability in the adult population, studies focused on the subacute stroke phase are less frequent, and those that focus on longer-term evolution are rare.
Aim: To determine the functional repercussion in patients with ischemic stroke during the SARS-CoV-2 pandemic.
Methods: A qualitative and retrospective study with a sample of 674 patients with acute ischaemic stroke that were selected. The outcomes were measured with Barthel index.
Results: The distribution in the moderate and severe degrees has been higher for the year 2020, in the independent and mild degrees it has been higher in the years 2019 and 2021, for the degree of total dependence it has been higher in the years 2019 and 2021. No significant correlation was found between age and the result of the Barthel scale or between the year in which the stroke occurred and the result of the Barthel scale.
Conclusion: No relationship is seen between the SARS-CoV-2 pandemic and worsening of functionality. The structural changes during the pandemic and the reduction in personnel have not affected the diagnosis and involvement of ischemic stroke. The effort of the staff, to maintain adequate care, has been decisive in the functional results of the patients.
Keywords: Acute ischaemic stroke; ABVD; Autonomy; Barthel index; Nursing; Outcomes; Quality of Life; Rehabilitation; Quality Improvement; SARS-CoV-2
Background
Stroke is one of the main causes of disability and the second in mortality [1]. Acute stroke is the 3rd cause of mortality, the 1st in disability in the adult population in developed countries and the 2nd in dementia. Its incidence increases according to age, its increase being directly proportional to population aging, reaching 280 episodes/100,000 inhabitants/year in >20 years [2]. With ischemic stroke mortality declining in all age groups, the prevalence of stroke continues to increase [3]. The trend towards an increasing incidence of ischemic stroke in the younger population adds to the large number of survivors who will live many years with their stroke-related disabilities [4]. At 6 months of follow-up, 26.1% of patients die, 41.5% achieve an independent life and 32.4% are dependent. Of the independent approximately 44% suffer a functional dependency [5]. On the other hand, of the 1,113,626 dependent people over 65 years of age, 73% (that is, 811,746) are attributable to stroke, with a third of them developing mild dependence, in half of the situation’s moderate dependence and 16 % severe dependency. Among the most frequent deficits are paralysis, gait and language disturbances, visual disturbances, cognitive disturbances, among others [5]. In relation to sex, it seems to have a significant effect on hospital mortality after stroke, with men tending to have worse results. Although there are controversies, since some studies have found a higher risk of mortality from stroke among women, others Research has shown that this increased mortality risk exists only in patients with subarachnoid heamorrhage. Recurrent stroke is postulated to be an independent predictor of poor long-term outcomes [5].
In relation to direct costs, the treatment, prevention, and diagnosis of stroke consume between 3-4% of public health spending in our country, 76% of which is attributable specially to spending on the hospitalization process. This data becomes more relevant considering that annually around 1,288,010 hospital stays are calculated for stroke (more than those caused by ischemic heart disease) in our country. On the other hand, the cost of stroke during the first year is around 20,000-30,000 euros [5]. Finally, it is highlighted that stroke not only has costs attributable to the disease process itself, but that it is of special mention, the cost on informal caregivers, which is between 801.7-1,243.9 million euros and developed comorbidities amount to spending 1,125.3-1,746.0 million euros. With around 50% of stroke survivors going straight home from acute care, family caregivers play a central role in supporting them as they transition through rehabilitation and back to community life [6]. In relation to the second point, indirect costs, stroke in Europe is responsible for 6.8% of disability-adjusted life years (DALYs), occupying second place ahead of dementia and Alzheimer’s, the latter being in 5th place. In Spain, of every 100 DALYs due to stroke, 62.1% will mean death and 37.9% will be years lived with disability [7].
The functional evolution of the patient after a stroke is classically established in three periods. An acute period that goes from the onset of symptoms to hospital discharge, a subacute period in which there is a progressive functional improvement, which continues in most cases during the first 3-6 months and finally a chronic phase functional stabilization. Some authors postulate a progressive functional improvement beyond 12 months when accompanied by rehabilitation treatment, and on the contrary a progressive functional deterioration in the absence of specific rehabilitation therapy [5]. Most attention to stroke patients has commonly focused on the acute phase, where recent efforts and medical advances have managed to reduce morbidity and mortality. However, studies focused on the subacute phase are less frequent, and those that focus on longer-term evolution are rare [5]. A variety of ADL assessment scales had been used, these included the Barthel Index (BI), the modified BI (MBI), the Functional Independence Measure (FIM), the Stroke Impairment Assessment Set (SIAS), and the modified Rankin Scale (mRS) [8]. Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) was identified in December 2019 and caused a global pandemic of coronavirus disease 2019 (COVID-19) [9]. At the beginning of 2021, more than 110 million people have been infected, with more than 60 million recovered and nearly 2.5 million deaths [10,11]. Besides, risk factors for mental health professionals were identified in more than 90% of nurses, affecting their psychological state with feelings of exhaustion, emotional overload [12]. All nonurgent clinical activities, such as surgical interventions, followups, treatments, tests, were suspended. Operating theatres were converted to intensive care units and several health professionals moved to COVID wards to support their colleagues, retired staff returned to work to overcome staff shortages, several health professionals moved out of their homes, even so, many of them became infected or even died [11]. Thus, the aim of this study is to determine the functional repercussion in patients with ischemic stroke during the SARS-CoV-2 pandemic.
Methods
Study Design and patients
This is a retrospective study of consecutive patients with ischaemic stroke at our institution between January 2019 to May 2021.
Patient selection
Inclusion criteria were anterior or posterior circulation acute cerebral occlusion, age > 18 years, with NIHSS ≥ 6. All patients received intravenous thrombolysis before intervention and < 4.5 hours from symptom onset, following the guidelines of the Spanish Society of Neurology. Thus, time from symptom onset to hospital arrival was < 4.5 hours.
Exclusion criteria were as follows: (a) presence of intracranial haemorrhage, (b) Pregnant patients.
Variables and data collection
Demographics: age; gender; start date of the study (dd/mm/ yyyy) and Barthel index.
Imaging evaluation
At admission and after a clinical evaluation by a neurologist, the majority of patients underwent a baseline CT scan, supraaortic and cerebral CT angiography, and cerebral perfusion CT. The other patients underwent to MRI, the DWI sequence was used to determine ASPECTS score. The ASPECTS analysis is performed on two axial sections of the CT, the first at the level of the thalamus and ganglia base (plane A) and the second adjacent to the upper edge of the ganglia of the base, without visualizing it (plane B). In both planes, the territory of the middle cerebral artery is divided into 10 regions, each valuing 1 point (M1-M10). Each affected area subtracts 1 point and the value of “normality” is set to 10 points.
Study Outcomes
Clinical outcome was measured with Barthel Index considering: Unable to perform task (<20 points), attempts task but unsafe (20-35 points), moderate help required (40-55 points), minimal help required (60-95 points) and fully independent (100 points).
Statistical and Data Analysis
A descriptive analysis was carried out using measures of central tendency (mean (M)) and dispersion (standard deviation (SD) when it was considered appropriate for quantitative variables, and percentages for qualitative variables). To analyse the differences between groups, the Chi2 test was used for the qualitative variables. A significance level of 0.05 was chosen to select the variables finally included in the binary logistic regression model. All analyses and calculations were performed using the statistical package PASW (v. 24.0; SPSS Inc., Chicago, Illinois).
Results
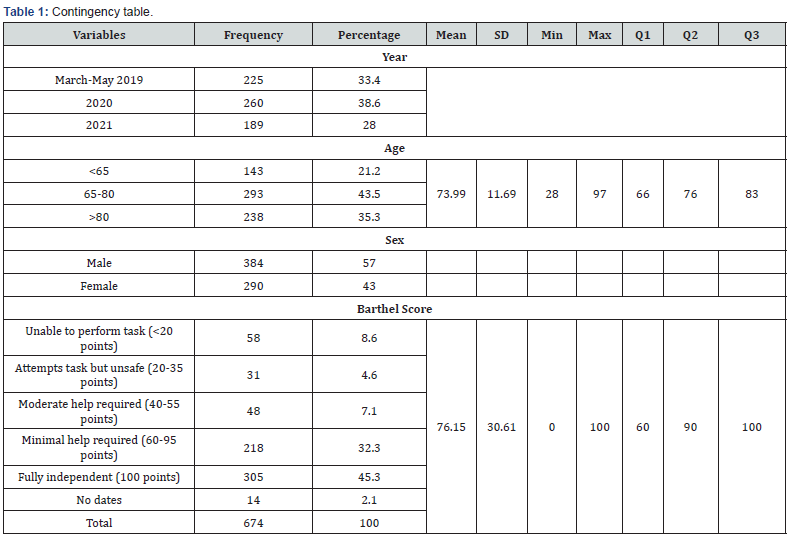
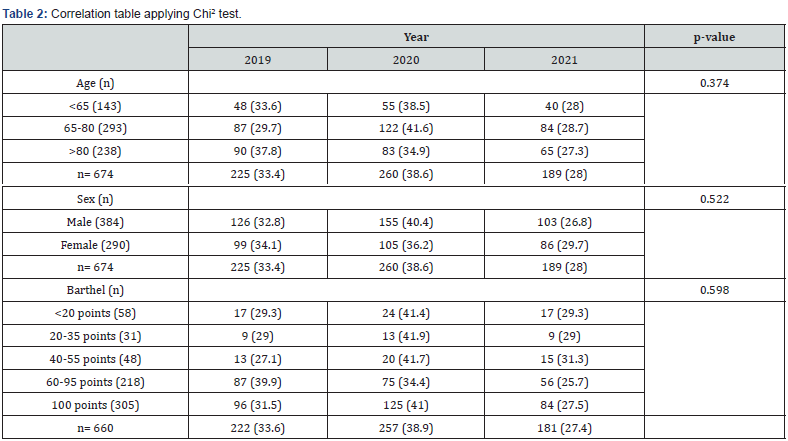
The total number of admissions for ischemic stroke in 2019 was 225 patients; in 2020 it was 261 and from January to May 31, 2021, it was 121 patients. During the months of March, April, and May 2019, 15, 18 and 18 patients were hospitalized, respectively; in 2020 it was 16, 14 and 15 patients, in 2021 it was 30, 15 and 24 patients. To observe the characteristics of the sample a contingency table was made (Table 1). The distribution in the moderate and severe degrees has been higher for the year 2020, in the independent and mild degrees it has been higher in the years 2019 and 2021, for the degree of total dependence it has been higher in the years 2019 and 2021. No significant correlation was found between age and the result of the Barthel scale or between the year in which the stroke occurred and the result of the Barthel scale (Table 2).
Discussion
In this study, the total number of admissions for ischemic stroke in 2019 was 225 patients; in 2020 it was 261 patients and from January to May 31, 2021, it was 121 patients. During 2021 there has been an increase in the number of hospitalized patients, probably related to the effects derived from the SARS-CoV-2 infection. Over the last two decades, the absolute number of people experiencing a first episode of stroke, the number of survivors after having a stroke, and the number of years of life lost have all increased. Consequently, survivors need and use numerous health resources, including intensive care, rehabilitation, social and community services [13,14]. With the progressive aging of the population, the magnitude of the problem and its consequences are increasing [15,16]. Implementation of regional and national stroke care and quality systems and improvement initiatives have a significant impact on reducing stroke-related morbidity and mortality and improving outcomes [5,17]. The mean age in this study was 73.99 years (SD: 11.69 years). The distribution by groups has been 140 patients for <65 years; of 286 patients for the group of 65-80 years and of 234 patients for the group of >80 years. The results in relation to age compared to other studies are very similar. Dura Mata et al. [18] determined a mean age of 72.44 years with a standard deviation of 10.1 years; Sajobi et al. [19] observed that the mean age was 68.1 years; Queralt-Tomas [16] of 71.9 years with a standard deviation of 12.3 years and Kaesmacher et al. [20] determined an age of 72.9 years with a standard deviation of 13.9 years [2, 16,19].
The mean age in the main RCTs ranges from 66-71 years, an interval in which our sample also falls [21-26]. Age was independently associated with outcome in the overall cohort, although this association could not always be identified after adjusting for other predictive variables, results consistent with current scientific evidence [2,27]. Patient functionality after stroke is significantly associated with the likelihood of hospital readmission and is an important outcome to consider in stroke, especially considering recent Medicare avoidable readmission policies. Patients with poor function, at the time of discharge, are also more likely to need long-term care and intensive rehabilitation plans, which implies a greater financial impact and more serious consequences for the family of the stroke survivor [28]. In relation to the subacute phase, the evaluation of the functional status of the ABVD is recorded in only 24.6% of the cases at discharge and for six months after the episode in the primary care database; functional status after stroke is a predictor of long-term mortality [23]. Autonomy has been found to be a fundamental precondition for effective participation. Previous research has described autonomy as the ability to make decisions, feel in control of the activities in which to participate and how these activities are carried out, it is important to consider this concept since the objective was to capture the quality of participation rather than of only the frequency in the activities [29].
The first six months after stroke are critical for rehabilitation with the ultimate goal of returning the individual to a satisfactory level of participation [5]. Functionality has become a broad term that includes the interaction of positive aspects between the 3 main components of the International Classification of Functioning (ICF): body functions and structures; activity and participation; and environmental and personal factors. With this model, the environment is viewed as either a facilitator or a barrier to functional recovery [30]. The authors found that 48% of the studies only evaluated body functions, 1% evaluated body structures, 45% only evaluated activity and/or participation, and 7% evaluated environmental factors. These findings demonstrate that post-stroke functionality has not yet been comprehensively assessed, as recommended by the ICF [30]. In a sample of 237 stroke survivors with a predominantly mild stroke at baseline, one study found that more than a quarter of survivors after seven years remained inactive on many items related to housework. About 91.5% lived independently without the help of community services, however, the participants depended on other reference persons for activities such as preparing meals, doing laundry or housework. Having to depend on others for activities of daily living affects not only stroke survivors but also the primary caregiver [4].
Both Teasdale and Walsh reported changes and restrictions in leisure activities in 60% of their samples [31]. Sveen, et al. [32] have suggested that a possible explanation for this is that these activities would require higher cognitive and social skills than activities carried out within the family environment. Compared to other studies, the functional results at discharge are similar, for example Törnbom, et al. [29] places in their sample 38% with mild or moderate disability and 41% with severe disability (value 3-5 of the mRS). In this study, the mean of the Barthel scale score was 76.15 points (SD: 30.62 points). The distribution has been 58 patients for total dependence (<20 points); of 31 patients for severe dependence (20-35 points); of 48 patients for moderate dependence (40-55 points); of 218 patients for mild dependence (50-95 points) and 305 patients for independence (100 points), results similar to the previously mentioned studies.
Regarding the functional result, the mean value of the Barthel scale at discharge was calculated, being 71.16 points for 2019, 77 points for 2020 and 73.71 points for 2021. The frequencies by degrees of affection were for the year 2019 independent 37.3%, mild dependency 38.09%, moderate dependency 7.93%, severe dependency 4.76% and total dependency 4.76%; for the year 2020 it was independent 47.82%, mild dependency 28.98%, moderate dependency 10.14%, severe dependency 10.14% and total dependency 8.69%; finally, for the year 2021 it was independent for 40.9%, mild dependency for 36.36%, moderate dependency for 7.27%, severe dependency for 2.73% and total dependency for 12.72%. The distribution in the moderate and severe degrees has been higher for the year 2020, in the independent and mild degrees it has been higher in the years 2019 and 2021, for the degree of total dependence it has been higher in the years 2019 and 2021. Compared to other studies, our results are similar. Jagini and Suresh [33] determined an asymptomatic-mild degree of disability in 75% of their sample and moderate-severe incapacity in 25% at three months. Another study determined that 25% of their sample improved their mRS values by one or more degrees between 3 months and 1 year [34].
In the DEFUSE 3 study, around 50% showed grade 0-1 on the mRS scale and around 80% grade 0-2. On the other hand, in the HERMES meta-analysis, it was shown in 25%-10% (intervention vs alteplase alone) grade 0-1 and 46%-25% (intervention vs control) grade 0-2. The results of our study are similar to those shown in the main RCTs, although there are significant differences if we compare them with the recent advances developed in the DEFUSE 3 study [26,35]. Sánchez Lozano, et al. [36] determined no functional impairment in a third of their sample, mild disability in half of the sample, and moderate-severe impairment in the remaining proportion at 6 months. Ganesh et al. [34] independently predicted dementia at 5 years and institutionalization by determining the value of the mRS between 3-5 as higher risk of dementia compared to the other grades, in addition, each step in the mRS scale was associated with a jump in the risk of dementia and subsequent institutionalization of the patient.
In Spain, results have been published after rehabilitation of patients with moderate to very severe initial loss and disability. Between 60 and 75% of these patients with moderate to very severe involvement recovers the ability to walk independently, and a percentage close to 50% recover levels of functional independence in activities of daily living, obtaining functional gains with multidisciplinary rehabilitation treatment in acute and subacute phase, greater than 50 points on the Barthel scale [36]. Articles suggested that a BI score ≧90 with mRS ≦2 to be the optimal cut-off score to define a favourable outcome, but recent articles have reported that BI ≧75 and mRS ≦2 could be used to define a favourable outcome in acute stroke patients [37]. The average scores of muscle strength of the affected upper limbs and lower limbs were 2.3±1.7 and 2.9±1.5, respectively [8]. After the first stroke, 44.9% of stroke survivors go directly home and the percentage of patients in each degree of dependency triples with a greater loss in the previous Barthel score among women (7.3) than in men (3.6) [16].
Mobility and independence assessments in ABVD continue to be the most frequently used measures in rehabilitation studies. With a trend towards an increase in the number of stroke survivors returning to independent living, these measures are probably insufficient to capture the demands of everyday life [5]. In describing ABVD as a measure of long-term stroke outcome, it is important to separate the ability to perform ABVD, such as feeding, dressing, and managing personal hygiene, from the ability to participate in more complex activities, such as housework, social activities, and paid work, called instrumental activities of daily living (IADL) [4]. IADL addresses a distinctly higher level of ABVD and consists of the more complex daily tasks that must be performed for the stroke survivor to continue living in the community. Exploring community integration and long-term needs up to five years after stroke [5]. Queralt-Tomas [16] proposes that nursing professionals carry out interventions according to general practice to provide continuity of care for stroke patients throughout the stroke recovery trajectory and also support for older caregivers. beyond the length of the patient’s hospital stay. Integrated care is desirable and constitutes a reference model for all situations considered.
Teaching and discharge planning can help families of stroke survivors make long-term arrangements specific to the expected functional outcome. Families may need modifications to the home environment, such as ramps, grab bars in the shower, and easy access beds. The earlier these plans are put into place, the sooner an impeded stroke patient can be discharged, reducing the length of a patient’s hospital stay [28]. Nurses must participate in research on the results in the functionality of patients, add services based on new technologies, lead support groups and educational resources, and administer telecare supervision in order to perform comprehensive care, while that the use of resources would be minimized, and accessibility would be improved [16]. Even so, knowledge of the long-term results of stroke, that is, beyond the first year, is scarce. With the global burden of stroke increasing, estimates of long-term outcomes and evaluation of prognostic factors are increasingly important for planning health service resources, providing evidence-based rehabilitation after care settings acute and also offer information for survivors and their families [4,7].
Conclusion
In this study, a progressive increase in admissions for stroke is observed over the 3 years, there is no evidence that this factor is due to the pandemic, it could be related to population aging and increased life expectancy. No relationship is seen between the SARS-CoV-2 pandemic and worsening of functionality. The structural changes during the pandemic and the reduction in personnel have not affected the diagnosis and involvement of ischemic stroke. The effort of the staff, to maintain adequate care, has been decisive in the functional results of the patients.
References
1. Vos T, Barber RM, Bell B, Bertozzi-Villa SA, Biryukov S, et al. (2015) Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. lancet 386(9995): 743-800.
- Pego Perez ER, Fernández I, Pumar JM (2021) Functional outcomes of patients with stroke treated with thrombectomy by aspiration. Brain Injury 35(4): 476-483.
- Vila Córcoles Á, Satué Gracia E, Ochoa Gondar O, Diego Cabanes CD, Vila Rovira Á, et al. (2014) Incidencia y letalidad del ictus isquémico en la población mayor de 60 años del área de Tarragona, España (2008-2011). Rev Neurol 59(11): 490-496.
- Blomgren C, Jood K, Jern C, Holmegaard L, Redfors P, et al. (2018) Long-term performance of instrumental activities of daily living (IADL) in young and middle-aged stroke survivors: Results from SAHLSIS outcome. Scand J Occup Ther 25(2): 119-126
- Pego-Pérez E R, Fernández-Rodríguez I, Pumar-Cebreiro JM (2019) National Institutes of Health Stroke Scale, modified Rankin Scale, and modified Thrombolysis in Cerebral Infarction as autonomy predictive tools for stroke patients. Rev Neurosci 30(7): 701-708.
- Magalhães R, Abreu P, Correia M, Whiteley W, Silva MC, et al. (2014) Functional status three months after the first ischemic stroke is associated with long-term outcome: data from a community-based cohort. Cerebrovasc Dis 38(1): 46-54.
- Pego Pérez ER, Fernández Rodríguez I, Pumar Cebreiro JM (2021) Autonomy results in post-mechanical thrombectomy applied to patients with stroke a retrospective study. Open access journal of Neurology and Neurosurgery 16(1): 1-8.
- Yang H, Chen Y, Wang J, Wei H, Chen Y, et al. (2021) Activities of daily living measurement after ischemic stroke: Rasch analysis of the modified Barthel Index. Medicine (Baltimore) 100(9): e24926.
- Bardenheier BH, Gravenstein S, Blackman C, Gutman R, Sarkar IN, et al. (2021) Adverse events following mRNA SARS-CoV-2 vaccination among US nursing home residents. Vaccine 39(29): 3844-3851.
- Chen M, Yuan Y, Zhou Y, Deng Z, Zhao, et al. (2021) Safety of SARS-CoV-2 vaccines: a systematic review and meta-analysis of randomized controlled trials. Infect Dis Poverty 10(1): 94.
- Della Monica A, Ferrara P, Dal Mas F, Cobianchi L, Scannapieco F, et al. (2022) The impact of Covid-19 healthcare emergency on the psychological well-being of health professionals: a review of literature. Ann Ig 34(1): 27-44.
- Del Pozo-Herce P, Garrido-García R, Santolalla-Arnedo I, Gea-Caballero V, García-Molina P, et al. (2021) Psychological impact on the nursing professionals of the rioja health service (Spain) due to the SARS-CoV-2 virus. Int J Environ Res Public Health 18(2): 580.
- Feigin VL, Forouzanfar MH, Krishnamurthi R, Mensah GA, Connor M, et al. (2014) Global and regional burden of stroke during 1990–2010: findings from the Global Burden of Disease Study 2010. Lancet 383(9913): 245-255.
- Ma VY, Chan L, Carruthers K J (2014) Incidence, prevalence, costs, and impact on disability of common conditions requiring rehabilitation in the United States: stroke, spinal cord injury, traumatic brain injury, multiple sclerosis, osteoarthritis, rheumatoid arthritis, limb loss, and back pain. Arch Phys Med Rehabil 95(5): 986-995.
- Serrano-Villar S, Fresco G, Ruiz-Artacho P, Bravo A, Valencia C, et al. (2012) Stroke in the very old: myths and realities. Medicina Clínica 140(2): 53-58.
- Queralt-Tomas L (2015) Coordination strategies of care across stroke recovery: Proposals for nursing interventions in primary care. Clinical Nursing Studies 3(2): 81-89.
- Rost NS, Bottle A, Lee JM, Randall M, Middleton S, et al. (2016) Stroke severity is a crucial predictor of outcome: an international prospective validation study. J Am Heart Assoc 5(1): e002433.
- Durà Mata MJ, Molleda Marzo M, García Almazán C, Mallol Badellino J, Calderón Padilla V (2011) Factores pronósticos en el ictus. De la fase aguda a los tres añ Rehabilitación 45(1): 18-23.
- Sajobi TT, Menon BK, Wang M, Lawal O, Shuaib A, et al. (2017) Early trajectory of stroke severity predicts long-term functional outcomes in ischemic stroke subjects: results from the ESCAPE Trial (Endovascular Treatment for Small Core and Anterior Circulation Proximal Occlusion With Emphasis on Minimizing CT to Recanalization Times). Stroke 48(1): 105-110.
- Kaesmacher J, Kleine JF (2018) Bridging Therapy with i.v. rtPA in MCA Occlusion Prior to Endovascular Thrombectomy: a Double-Edged Sword. Clin Neuroradiol 28(1): 81-89.
- Berkhemer OA, Fransen PS, Beumer D, Van Den Berg LA, Lingsma HF, et al. (2015) A randomized trial of intraarterial treatment for acute ischemic stroke. n Engl J Med 372 (1): 11-20.
- Campbell BC, Mitchell PJ, Kleinig TJ, Dewey HM, Churilov L, et al. (2015) Endovascular therapy for ischemic stroke with perfusion-imaging selection. N Engl J Med 372(11): 1009-1018.
- Goyal M, Demchuk AM, Menon BK, Eesa M, Rempel JL, et al. (2015). Randomized assessment of rapid endovascular treatment of ischemic stroke. N Engl J Med 372(11): 1019-1030.
- Jovin TG, Chamorro A, Cobo E, de Miquel MA, Molina CA, et al. (2015) Thrombectomy within 8 hours after symptom onset in ischemic stroke. N Engl J Med 372(24): 2296-2306.
- Saver JL, Goyal M, Bonafe A, Diener HC, Levy EI, et al. (2015) Stent-retriever thrombectomy after intravenous t-PA vs. t-PA alone in stroke. N Engl J Med 372(24): 2285-2295.
- Lansberg MG, Mlynash M, Hamilton S, Yeatts SD, Christensen S, et al. (2019) Association of thrombectomy with stroke outcomes among patient subgroups: secondary analyses of the DEFUSE 3 randomized clinical trial. JAMA Neurol 76(4): 447-453.
- Wouters A, Nysten C, Thijs V, Lemmens R (2018) Prediction of outcome in patients with acute ischemic stroke based on initial severity and improvement in the first 24 h. Front Neurol 9: 308.
- Nichols C, Carrozzella J, Yeatts S, Tomsick T, Broderick J, et al. (2018) Is periprocedural sedation during acute stroke therapy associated with poorer functional outcomes?. Journal of neuro interventional surgery 10(Suppl 1): i40-i43.
- Törnbom K, Hadartz K, Sunnerhagen KS (2018) Self-perceived participation and autonomy at 1-year post stroke: a part of the stroke arm longitudinal study at the University of Gothenburg (SALGOT Study). J Stroke Cerebrovasc Dis 27(4): 1115-1122.
- Silva SM, Corrêa FI, de Morais Faria CDC, Buchalla CM, da Costa Silva PF, et al. (2015) Evaluation of post-stroke functionality based on the International Classification of Functioning, Disability, and Health: a proposal for use of assessment tools. J Phys Ther Sci 27(6): 1665-1670.
- Walsh ME, Galvin R, Loughnane C, Macey C, Horgan NF (2015) Community re-integration and long-term need in the first five years after stroke: results from a national survey. Disabil Rehabil 37(20): 1834-1838.
- Sveen U, Thommessen B, Bautz-Holter E, Wyller TB, Laake K (2004) Well-being and instrumental activities of daily living after stroke. Clin Rehabil 18(3): 267-274.
- Jagini SP, Suresh I (2018) Clinical profile of patients with acute ischemic stroke receiving intravenous thrombolysis (rtPA-alteplase). International Journal of Advances in Medicine 5(1).
- Ganesh A, Luengo-FR, Wharton RM, Gutnikov SA, Silver LE, et al. (2017) Time-course of functional recovery after acute ischaemic stroke and its relationship to cause-specific mortality: implications for follow-up of stroke trials. Neurology 88(16): S19-004.
- Goyal M, Menon BK, van Zwam WH, Dippel DW, Mitchell PJ, et al. (2016) Endovascular thrombectomy after large-vessel ischaemic stroke: a meta-analysis of individual patient data from five randomised trials. Lancet 387(10029): 1723-1731.
- Sánchez Lozano A, PandoTorres R, de la Maza Martínez J, González Alba G, Bernal Valladares E, et al. (2018) Calidad de vida de pacientes a los 6 meses de un ictus isqué Rev. Finlay 8(1): 18-25.
- Zhou M, Liu X, Zha F, Liu F, Zhou J, et al. (2021) Stroke Outcome Assessment: Optimizing Cutoff Scores For The Longshi Scale, Modified Rankin Scale And Barthel Index. Plos One 16(5): E0251103.






























