The Diagnostic and Treatment Challenges of Adult Rasmussen’s Encephalitis: A Case Report and Literature Review
Alawi A Al-Attas1*, Tahani A Jamaly1, Naif S Alnefaie2 and Abdullah A Kokandi2
1 Department of Neurology, King Faisal Specialist Hospital and Research Centre, Saudi Arabia
2 College of Medicine, Imam Mohammad Ibn Saud Islamic University (IMSIU), Saudi Arabia
Submission: March 14, 2022; Published: April 11, 2022
*Corresponding author: Alawi A Al-Attas, Department of Neurology, King Faisal Specialist Hospital and Research Centre, Postal Code: 11525 Riyadh P. O. Box: 59046, Riyadh, Saudi Arabia
How to cite this article: Alawi A Al-A, Tahani A J, Naif S A, Abdullah A K. The Diagnostic and Treatment Challenges of Adult Rasmussen’s Encephalitis: 002 A Case Report and Literature Review. Open Access J Neurol Neurosurg 2022; 17(1): 555953. DOI 10.19080/OAJNN.2022.17.555953.
Abstract
Background: Rasmussen's encephalitis (RE) is a chronic inflammation of the brain (encephalitis) with refractory seizures, loss of motor skills and speech, hemiparesis, and mental deterioration. It causes devastating consequences if not recognized earlier and treated promptly.
Case presentation: Herein, we reported an adult girl with Rasmussen's encephalitis who failed immunotherapy, however responded dramatically to surgical intervention.
Discussion: RE was exclusively linked to the pediatric group and rarely encountered in an adult; however, the revised Bien criteria recently no longer considered the age at onset as a diagnostic criterion; furthermore, there is an increasing number of reported adults RE cases in the literature. Neither anti-seizure medications (ASMs) nor immunotherapy control seizures. However, surgical options with hemispherectomy remain the mainstay of treatment
Conclusion: RE is a rare chronic progressive disorder that should be considered as a possible differential diagnosis in patients who present with intractable seizures.
Keywords: Rasmussen's encephalitis; Refractory seizures; ASMs; Immunotherapy; Hemispherectomy
Abbreviations:: RE: Rasmussen’s Encephalitis, ASMs: Anti-Seizure Medications, EPC: Epilepsia Partialis Continua, IVIG: Intravenous Immunoglobulin, CSF: Cerebrospinal Fluid, ECG: Electrocardiogram
Introduction
Rasmussen's encephalitis (RE) is a chronic progressive unilateral localized neurological deterioration characterized by intractable seizures, neurological and cognitive decline [1]. The first case of RE was diagnosed in 1950 by the neurosurgeon Theodore Rasmussen [2]. It is a rare disease; there are 2.4 per 10 million estimated cases in people aged 18 years and younger, with an average age at onset of 6 years. It consists of three stages: prodromal, acute, and residual stages [1]. Although studies suggest autoimmune origin based on the brain's immune reaction and immune-modulatory treatment's efficacy on slowing the disease's course, the disease mechanism is unknown [1,3]. The diagnosis of RE is challenging as it requires high suspicion early in the disease course. Based on the European consensus statement, there are two sets of criteria: either one could reach the RE diagnosis, depending on the clinical features, MRI results, EEG, and histopathology. However, the main aim of treatment is to alleviate both seizure activity and clinical deterioration [3,4]. There are two recommended treatment arms: Immunotherapy and surgical hemispherectomy. The choice between them depends on the disease's stage, current neurological deficit, and the dominant hemisphere's involvement. Immunotherapy is preferred in early diagnosed cases of RE [5]. On the other hand, in late-diagnosed cases with stable neurological deficits, surgical hemispherectomy is recommended and is the only permanent cure of seizure activity but may cause more deterioration if done early in the stage. The course of the disease and treatment methods are still not well understood [6]. Here we report a case of an adult woman presenting with epilepsia partialis continua (EPC) caused by Rasmussen’s encephalitis.
Case Presentation
We reported a case of a 19-year-old girl right-handed, first-year college student, who presented with continuous left upper limb movements and left facial twitches for eight months. She had continuous left upper limb jerky movements; she was taken to the local hospital and was admitted and started on ASMs.
One week later, she presented an aware focal to bilateral tonic-clonic seizure; for that reason, she sought medical advice and was admitted for two weeks. She received intravenous ASMs. but, unfortunately, without improvement. Brain magnetic resonance imaging showed apparent atrophy on the right hemisphere with high signal intensity on the right parieto-occipital areas and right cerebellum. The treating physician presumed the underlying autoimmune disease; hence, she was started empirically on intravenous immunoglobulin (IVIG) and three doses of one-gram intravenous Methylprednisolone. Then, she was referred to our hospital for further evaluation and management. There was no history of fever, joint pain, skin rash, chronic cough, raw milk ingestion, diabetes mellitus, jaundice, significant head injury, prior central nervous system infections, or family history of epilepsy.
On examination, her temperature 36 [7]. degrees centigrade, blood pressure 100 systolic and 61 diastolic, pulse rate was 75 beats per minute, respiratory rate 20 per minute, and oxygen saturation 100 percent on room air. Alert, awake and oriented has left facial flattening of upper motor neuron and left hemiparesis with a power of about 3/5 distally more than proximal. However, she maintained good power over right side. The examination was interrupted by frequent focal aware seizures characterized by sudden twitches of the left eye, left face, and then jerky movement of the left upper limb that lasted for about a minute without focal to bilateral tonic clonic seizures. The rest of the clinical examination was unremarkable.
Blood investigations revealed unremarkable blood cell count results, blood glucose level, renal function tests, liver function tests, and electrolytes. Cerebrospinal fluid (CSF) analysis was completely normal. Further testing for the following paraneoplastic and autoimmune encephalitis antibodies were negative. Electrocardiogram (ECG), CT scan of the chest, abdomen and pelvis were all normal. Brain MRI revealed focal grey matter gliotic changes involving the right frontal, temporal and parietal lobes associated with significant atrophy over the right hemisphere predominantly over the temporal and frontal lobes with minimal atrophy on the contralateral hemisphere Figure 1.

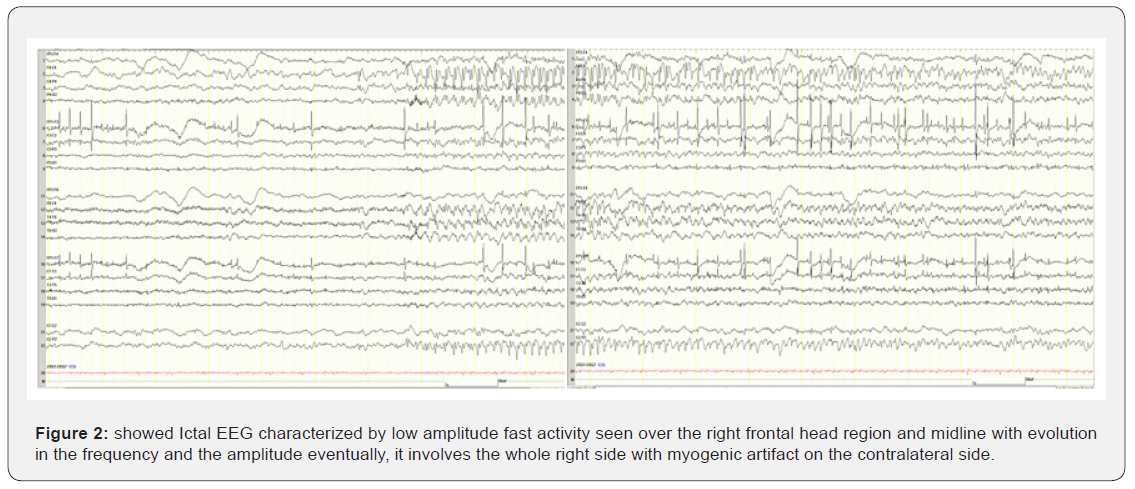
A positron emission tomography scan showed hypometabolism over the right frontal and temporal regions. The neuropsychology evaluation was challenging due to frequent seizures. Video EEG monitoring revealed a background of 8 Hz, symmetrical, and reactive to eye-opening. However, over the left side, myogenic artifacts obscured the background. There was continuous focal slow wave consisting of mixed delta and theta range activity of medium amplitude seen over the right frontocentral and, to a lesser extent, the right parietal head regions. Asymmetric sleep potentials were observed in which vertex and sleep spindles were seen more prominent over the left central head regions. There were spikes and wave complexes, and polyspikes observed over the right frontocentral-parietal and to a lesser extent over the right temporal head region Figure 2.
ECG showed normal sinus rhythm. We could capture frequent focal aware seizures, characterized by sudden left eye blink followed by head turned to the left side, and then left-hand clonic seizure, last for about 1-2 minutes with and without focal to bilateral tonic clonic. Biopsy from both right frontal and temporal lobes was consistent with the advanced stage of Rasmussen's encephalitis. She received five intravenous immunoglobulin doses (IVIG) and three doses of one-gram intravenous methylprednisolone, levetiracetam 1000 mg twice a day and valproate 750 mg twice a day; without improvement. The case was discussed in the epilepsy monitoring unit conference. Hence, hemispherectomy was performed after proper counselling. Fortunately, seizures were resolved, but she was ended with left-sided hemiplegia.
Discussion
We described a late onset of Rasmussen encephalitis at 19-years of age, with no response to immunotherapy, and excellent remission after hemispherectomy. The patient meets the criterion-A and B for the diagnosis of RE described by the European consensus statement in 2005 [3]. Although this is not the typical age of presentation, the case had a typical disease progression, as described in the Bien in 2002 study [1]. The symptoms started few months back with the prodromal stage, then shifted to the acute phase when the patient presented with continuous left upper limb movements and left facial twitches, followed by frequent focal aware seizures but did not reach the residual stage. and EEG findings consistent with the right hemispheric onset of seizure spreading and involving both hemispheres. The MRI showed significant atrophy over the right hemisphere, more predominant on the frontal and the temporal lobes. RE is usually resistant to ASMs, as in this case, unfortunately, focal seizures have continued despite concurrent administration of Levetiracetam 1000 mg twice a day and valproate 750 mg twice a day.
As shown in the immunomodulatory experience studies, there were patients who benefited temporarily by decreasing seizure activity and improved their neurologic status. However, this case received immunotherapy without obvious seizure control or improvement in the neurologic status. Granata et al, proposed immunomodulation to delay surgery in patients with late-onset RE with slower and milder course than the typical childhood-onset form [5]. Moreover, Dupont et al. had an extensive review of late-onset RE compared to classical RE, the late-onset RE patients found to have:
i) frequent focal complex partial seizures,
ii) less frequent epilepsia partialis continua
iii) a slower evolution with a delayed occurrence of cortical deficit,
iv) less cognitive deterioration and
v) the immunotherapy, even if performed in a late stage, improved late-onset RE. This review confirmed that late-onset RE has specific clinical and radiological features [7]. However, our reported case has some differences with their findings in terms of seizure type, evolution, and response to immunotherapy.
Similarly, McLachlan et al has described three adults with RE were clinical, electroencephalographic, and magnetic resonance imaging findings indicated patchy, multifocal involvement of primarily one hemisphere, but the adults had more evidence of disease in the opposite hemisphere than occurs in children [8]. The average length of the prodromal period in pediatric RE has been described in months; however, adult RE has an extended prodromal period makes early diagnosis very challenging. Furthermore, the variable clinical courses, work-up for paraneoplastic and autoimmune syndromes was proposed by the authors [4]. Wang et highlighted the safety, efficacy and of favorable prognosis after functional hemispherectomy in an adult patient with RE [6]. The patient underwent right hemispherectomy due to intractability, seizure recurrence, and disease progression with an excellent remission and left-sided hemiplegia. Over a 1-year follow-up, with extensive rehabilitation some motor functions improved. Repeated MRI brain revealed stable post-surgical changes.
Conclusion
Rasmussen's encephalitis is a cause of intractable epilepsy with progressive neurological deficits in adults and children. Treatment of Rasmussen's encephalitis represents a challenge in an adult population; however, hemispherectomy is the best surgical tool for properly selected adult patients with pre-existing hemiparesis and intractable epilepsy.
References
- Varadkar S, Bien CG, Kruse CA, Frances E Jensen, Jan Bauer, et al. (2014) Rasmussen's encephalitis: clinical features, pathobiology, and treatment advances. Lancet Neurol 13(2): 195-205.
- Rasmussen T, Olszewski J, Lloyd-Smith D (1958) Focal seizures due to chronic localized encephalitis. Neurology 8(6): 435-435.
- Bien CG, Granata T, Antozzi C, J H Cross, O Dulac, et al. (2005) Pathogenesis, diagnosis and treatment of Rasmussen encephalitis: a European consensus statement. Brain 128(pt3): 454-471.
- Castellano JF, Meyer JA, Lado FA (2017) A case series of adult-onset Rasmussen’s encephalitis: diagnostic and therapeutic challenges. Front neurol 8: 564.
- Granata T, Fusco L, Gobbi G, G Broggi, R Mantegazza, et al. (2003) Experience with immunomodulatory treatments in Rasmussen’s encephalitis. Neurology 61(12): 1807-1810.
- Wang Q, Zhu Z, Wang G, Lichao Sun, Jiqing Qiu (2019) Functional hemispherectomy for adult Rasmussen encephalitis: a case report and literature review. Turk Neurosurg 29(6): 945-949.
- Dupont S, Gales A, Sammey S, Marie Vidailhet, Virginie Lambrecq (2017) Late-onset Rasmussen encephalitis: A literature appraisal. Autoimmun Rev 16(8): 803-810.
- McLachlan RS, Girvin JP, Blume WT, H Reichman (1993) Rasmussen's chronic encephalitis in adults. Arch neurol 50(3): 269-274.






























