A Successful Separation of Total Vertical Craneopagus Conjoined Twins in Costa Rica
Juan Luis Segura Valverde1*, Justiniano Zamora Chaves2, Edgar Jimenez Masis3, Humberto Trejos Fonseca4, Juan Luis Segura Masis5 and Isabela Peña Pino2
1Department of Pediatric Neurosurgery, National Children’s Hospital Dr. Carlos Saenz Herrera, San José, Costa Rica
2Universidad de Ciencias Médicas Andres Vesalio Guzman, San José, Costa Rica
Submission: October 05, 2020; Published: October 20, 2020
*Corresponding author: Juan Luis Segura Valverde, Department of Pediatric Neurosurgery, National Children’s Hospital Dr. Carlos Saenz Herrera Calle 20 Avenida 0, Paseo Colon San Jose, 10103, Costa Rica
How to cite this article: Juan L S V, Justiniano Z C, Edgar J M, Humberto T F, Juan L S M, et al. A Successful Separation of Total Vertical Craneopagus Conjoined Twins in Costa Rica. Open Access J Neurol Neurosurg 2020; 14(3): 555887.DOI: 10.19080/OAJNN.2020.14.555887.
Abstract
Conjoined twins that are attached at the head are classified as craneopagus twins and they represent an extremely rare congenital malformation. The broad phenotypic variation within this group requires an extensive workup to determine the internal shared anatomy, since a separation surgery may require dividing not only skin and calvarium, but also dura mater, venous circulation and even brain cortex. We present such a case in a 2-year-old male pair of type I total vertical craneopagus twins who were surgically separated successfully at the National Children’s Hospital of Costa Rica. Given the highly complex shared venous morphology, this single surgery required the division of a circumferential dural sinus, a common torcula herophili and abundant secondary venous drainage. To achieve this, novel techniques were implemented to optimize surgical time and blood loss as well as attain an equitable distribution of structures. Despite the high morbidity and mortality associated with this type of surgery, both twins now live with their parents one year later.
Keywords:Craneopagus; conjoined twins; Circumferential dural sinus
Introduction
Conjoined twins who are attached by the calvarium are called craneopagus twins (CT) [1]. This congenital malformation has an extremely low incidence of 0.6 births per million people in the U.S. and represents a 2-6% of all types of conjoined twins [2-5]. Of all CT, approximately 73% of them are stillborn or die in the perinatal period [2]; therefore, only 25% live long enough to attempt a separation [3, 6]. In Costa Rica, a birth rate of 68,000 births/year [7] predicts that one of these operable cases will occur once every 98 years. Given the rarity of this malformation, our team took the planned separation of such twins as a serious and challenging task. To our knowledge, this is the second CT separation surgery performed in our institution and in Costa Rica, both by the same surgeon. Since every conjoined pair of twins will intrinsically present an altered anatomy, multiple descriptions have attempted to classify the heterogeneity amongst the craneopagus variations, despite the fact that no two pairs are exactly the same [8, 9]. The angle of cephalic junction and level of depth of shared structures present a wide spectrum of phenotypes that will determine the prognosis of a separation surgery [2,3]. Therefore, Stone and Goodrich propose a classification system that subdivides CT into partial and total based on the amount of shared structures and into vertical or angular based on the angle of attachment [3]. This system is important because total CT are predisposed to having a worse outcome from surgery since they can present fusion of deep structures such as blood vessels and cerebral cortex in addition to sharing meningeal layers and calvarium [2,10]. One common and critical morphological alteration in total CT is that of a shared superior sagittal sinus in the shape of a circumferential loop overlying the line of contact between opposing hemispheres; the division of this structure determines the technical difficulty of separation surgery [1-4,8]. In the face of such a rare condition and the variability amongst the subtypes, a standard surgical technique has not been established. However, a divergence in approach has surged with growing numbers: one single surgery versus multiple staged surgeries [2]. Regardless of which technique is chosen, the separation of CT is a daunting but necessary task that can offer a substantial improvement in quality of life and independence to these patients.
Case Presentation
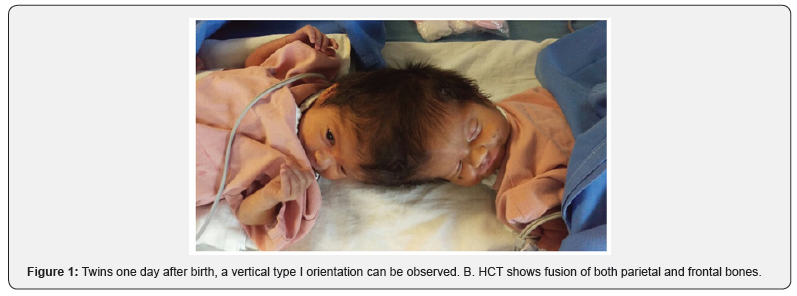
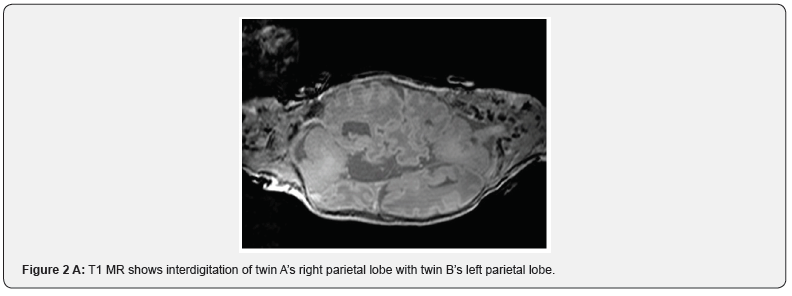
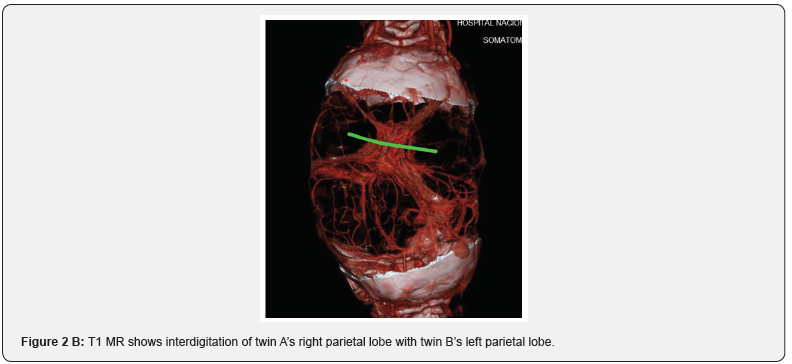
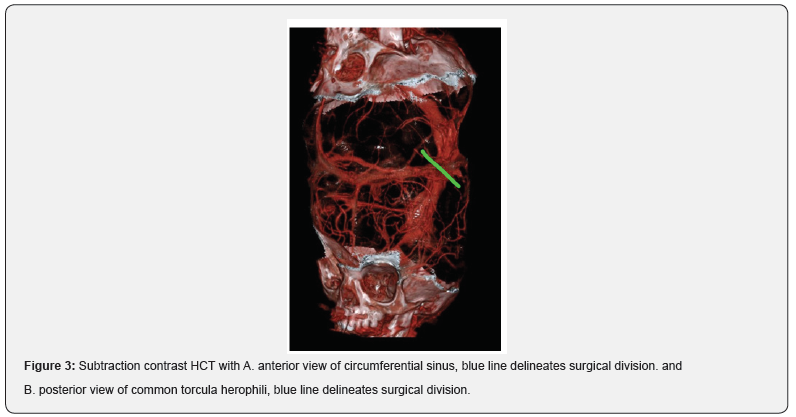
We present the case of a pair of male conjoined craneopagus twins treated at the National Children’s Hospital of Costa Rica. Having been diagnosed prenatally at 24 gestational weeks, they were born by planned cesarean section without complications and without any other congenital malformations other than presenting with a total vertical type I junction of the heads (Stone and Goodrich classification)[4] with minimal longitudinal angulation (<40˚)(Figure 1). Along with the Reconstructive Surgery team, the department of Neurosurgery began planning for surgical separation since birth, with the initial placing of tissue expanders at 1 year of age to ensure adequate skin closure. When they turned 2 years and 2 months, they were admitted to the surgical unit for the definitive separation. On the day of admission, they both presented neurodevelopmental delay in language, slight muscular atrophy of the lower extremities from lack of use and twin B was discretely smaller in size than twin A. Amongst the preoperative imaging studies, the HCT (Head Computerized Tomography) showed a cranial vault with continuous bilateral parietal and frontal bones (Figure 1). The MR (Magnetic Resonance) illustrated a clear separation between twin A’s left cerebral hemisphere from twin B’s right cerebral hemisphere and some interdigitation with possible fusion of the respective contralateral superior parietal lobes (Figure 2a). The angiography demonstrated a shared venous circulation with bidirectional filling (Figure 2b). Lastly, the subtraction contrast HCT showed a circumferential venous sinus with a common torcula herophili posteriorly (Figure 3). These patients’ anatomical characteristics place them as type D CT according to Winston’s classification [3].
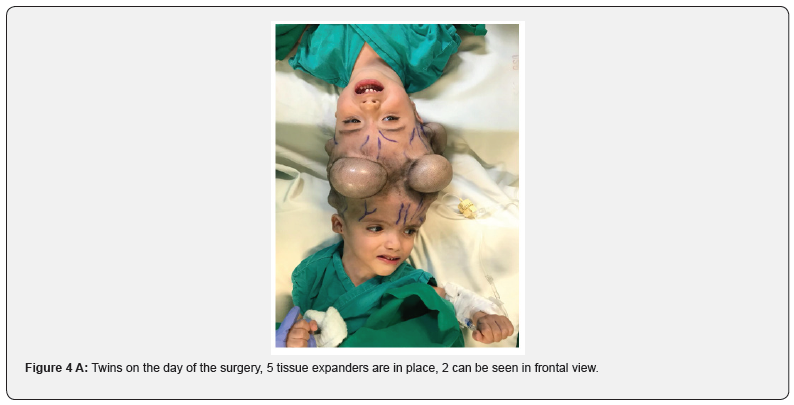
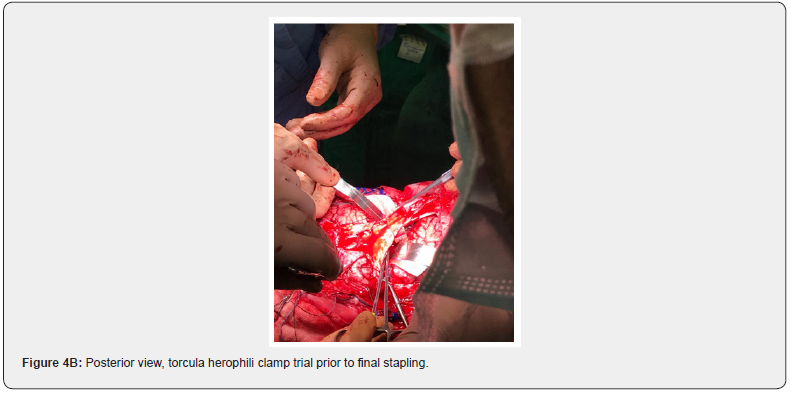
On the day of the surgery, a multidisciplinary team of neurosurgeons, reconstructive surgeons, anesthesiologists and operating room technicians was assigned to each twin. A semicircumferential frontal sinusoidal incision was made (Figure 4a), followed by a band craniotomy of the shared fronto-parietal bone. A synchronized flip was performed to place the patients face down and the circumferential skin incision and band craniotomy were completed posteriorly. The dura was incised up until the edges of the circumferential sinus and torcula herophili. A clamp trial along the diagonal cross-section of the torcula showed neither cortical edema nor erythema after a sufficient amount of time (Figure 4b). A gastrointestinal anastomosis stapler (GIA Coviden™) was used for the final separation of the torcula (Figure 3a-b) and there was no bleeding along the staple line. This technique significantly reduced the expected bleeding and surgical time for this type of procedure as well as the risk of air emboli. As the division of dura mater continued, including a reflection layer resembling a falx cerebri, several secondary bridging venous sinuses had to be divided in an effort to ensure a balanced separation. Once a deeper dissection was attained, the shared superior parietal lobe was divided with bipolar dissection. After dividing the frontal aspect of dura mater, the twins were finally separated, surgical tables moved apart and closure began. Despite the measures taken to ensure closure, a biological graft (DuRepair™) was used to close the Dural defect and a regeneration matrix (Integra™) covered the skin defect of about 30% in both twins. Because of the shared circulation, there was an intraoperative selective distribution of fluids that generated fluid overload with pulmonary edema in twin A and hemodynamic instability that required resuscitation with fluids and inotropic agents in twin B. These issues resolved immediately after vascular separation was attained. After 20 hours, both patients left the OR (operating room). After the surgery, twin A had a surgical wound infection with biofilm formation on the biological grafts for which he had to be taken to the OR for washouts on several occasions. This delayed skin closure until 30 days after the initial surgery. He also developed hydrocephalus and pseudomeningocele formation that required placement of an EVD (External Ventricular Drain); this complication resolved before the final skin closure. Twin a presented lesional epilepsy, chronic diarrhea of central origin, cerebral salt wasting syndrome and hypertension. He was discharged from the hospital 4 months after the initial surgery with significant neurological secuelae characterized by spastic tetraparesis with predominance of the lower extremities and limited spontaneous movement. His last HCT showed diffuse hypoxic injury of the cerebral upper cortex. Currently, twin A breathes through a tracheostomy on room air, feeds through a gastrostomy tube and takes medications for epilepsy and hypertension.
Postoperatively, twin B had refractory coagulopathy that promoted the formation of a left fronto-parietal intraparenchymal hematoma, which required emergent evacuation. He also developed hydrocephalus and a pseudomeningocele that resolved with the temporary placement of an EVD. Skin closure was delayed until 18 days after the initial surgery. While he was admitted, twin B developed lesional epilepsy, fever of central origin and corneal deepithelization. Three months after the initial surgery, he was discharged with significant neurological secuelae characterized by spastic tetraparesis mainly of the right side. His last HCT showed diffuse hypoxic injury of the cerebral upper cortex and associated ventriculomegaly. Currently, twin B breathes through a tracheostomy with nocturnal supplementary oxygen, feeds through a gastrostomy tube and takes medications for epilepsy. Both twins currently live at home with their parents and older brother (Figure 4). Cranioplasty has been indefinitely delayed until they reach the adequate level of maturity.
Discussion
As described in the literature, separation surgery of total vertical CT has a mortality rate of 48% with only a 25% of patients having normal to moderate neurological outcomes, while partial CT surgery has a mortality rate of 14% [4]. This difference in mortality is attributed to the risk that separating a complex venous drainage system entails [11, 12], so much, so that a statistically significant correlation has been identified between complexity of venous drainage and neurological outcome after surgery [2]. Since the first successful separation surgery in 1953 [8], it was only until 2004 that the first separation of total vertical CT type I with a normal neurological outcome was reported [4]. Despite the fact that cerebral cortex fusion has not been proven to affect separation surgery mortality, it will inherently increase neurological morbidity [2]. In the case of our patients, them being classified as type I vertical CT with a shared circumferential venous dural sinus and interdigitation/fusion of one parietal lobe were all factors that determined a greater preoperative risk of morbidity and mortality. The extensive preoperative imaging studies that were performed helped the assessment of this risk by the multidisciplinary team and as a result, aided in the parents’ informed decision to go forth with the surgery.
The reported complications for the separation surgery are venous blood loss, venous occlusion, cerebral edema, hemorrhage, ischemia and gaseous embolus [1,4], with blood loss having the most impact in mortality [11]. In our case, measures such as using autologous blood transfusions (Cellsaver™) and the novel use of a gastrointestinal anastomosis stapler (GIA Coviden™) for the splitting of a large vascular structure such as the shared torcula herophili were crucial in managing intraoperative blood loss. The latter technique significantly reduced the risk of massive blood loss and gaseous embolus as well as shortened the operative time. There is still some controversy regarding the single surgery approach versus a staged surgery method for the management of separating a set of complex shared venous anatomy [2]. One must take into consideration the benefit of achieving optimal venous circulation with the progressive induction of collateral circulation through pruning against the risks of submitting sets of twins to repetitious major intracranial surgeries, each with its own set of complications [2,12]. In a revision of 41 cases, a staged separation was associated with 23% mortality compared to a mortality of 63% in single separations [4]. Despite the growing evidence leaning towards a greater safety in a staged approach, the technique described in patients similar to this case report requires choosing a recipient and a donor of the circumferential sinus [13]. Hence, pruning becomes essential to induce collateral drainage in the donor twin who will be rendered devoid of a major vascular structure [2]. In our case, it was the team’s and the parents’ decision to give both patients an equal distribution of structures. Since they had such robust venous structures with bidirectional flow, it was feasible to attempt a single approach in which our technique allowed for an even separation of the shared venous torcula and its feeding structures. Because venous hypertension was a risk we had undertaken, cerebral edema and erythema were repeatedly ruled out throughout the case before making definitive vascular cuts and final closure. Regrettably, the postoperative CTH showed hypodensities consistent with venous infarcts and both patients’ neurological outcomes were suboptimal. Upon such a challenging condition for the surgical community, several novel techniques have been implemented to improve the separation surgery, such as the use of distraction osteogenesis and soft tissue molding [5], as well as the use of embolization of shared venous circulation as an alternative to the staged surgery pruning [12,14]. Given the low incidence of craneopagus twinning, each separation attempt can serve as an opportunity for improvement and innovation. By sharing our experience, we hope to contribute to the idiosyncrasy that envelops this surgical feat.
Established Facts and Novel Insights
Established Facts
a. The incidence of conjoined craneopagus twins is extremely low
b. Conjoined twin separation surgery presents a high morbidity and mortality rate, especially in total vertical craneopagus twins
c. A frequent anatomical presentation in total vertical craneopagus twins is a circumferential dural venous sinus
d. The amount of shared venous drainage is directly related to the morbidity/mortality rate of separation surgery Novel Insights
a. Presentation of clinical and surgical aspects of a separation surgery of total vertical craneopagus twins, a very rare procedure
b. Description of a highly complex and rare venous drainage anatomy
c. Description of an equal separation of venous sinuses with venoplasty in a single procedure
d. Novel use of an anastomosis stapler for the division of a common torcula herophili

Acknowledgement
We wish to acknowledge the patients’ parents for believing in our team to care for their children. We also wish to acknowledge all of the National Children’s Hospital ICU, anesthesiology, plastic surgery, infectious disease teams and ancillary staff who aided in the extensive care that the twins required with the utmost dedication and effort that allowed for their survival.
Statement of Ethics
The patients’ parents have both given written consent to publish their children’s case including publication of images.
Disclosure Statement
The authors have no conflicts of interest to declare.
Funding Sources
The authors received no financial support for the data acquisition or authorship of this manuscript.
Author Contribution
Concept and design: Segura Valverde, Zamora Chaves, Jimenez Masis, Trejos Fonseca, Segura Masis, Peña Pino. Acquisition of data: Peña Pino. Analysis and interpretation of data: Segura Valverde, Peña Pino. Drafting the article: Peña Pino. Critical revision of article: All authors. Reviewed final version of manuscript: All authors.
References
- Staffenberg DA, Goodrich JT (2005) Separation of craniopagus conjoined twins: an evolution in thought. Clin Plastic Surg 32(1):25-34.
- Walker M, Browd SR (2004) Craniopagus twins: embryology, classification, surgical anatomy, and separation. Child Nerv Syst. 20(8-9):554-556.
- Browd SR, Goodrich JT, Walker ML (2008) Craniopagus twins. J Neurosurg Pediatr 1:1-20.
- Stone JL, Goodrich JT (2006) The Craniopagus malformation: classification and implications for surgical separation. Brain 129(Pt 5): 1084-1095.
- Heuer GG, Madsen PJ, Flanders TM, Kennedy BC, Storm PB, et al. (2019) Separation of Craniopagus Twins by a Multidisciplinary Team. N Eng J Med 380(4):358-364.
- Kheir AEM, Dunaway D, Jeelani UN, Osman NM, Omer IM, et al. (2012) Successful separation of Craniopagus Conjoined Twins. Sudan J Pediatr 12(2):73-76.
- INEC [Internet]. Tasa Bruta de Natalidad 1950-2017.
- O Connell JEA (1976) Craniopagus twins: surgical anatomy and embryology and their implications. J Neurol Neurosurg Psychiatry 39(1): 1-22.
- Goh KYC(2004) Separation surgery of total vertical craniopagus twins. Childs Nerv Syst 20(8-9):567-575.
- Nejat F, Habibi Z, Goudarzi M, Azad MS, Moradi E, et al. (2017) Emergency separation of craniopagus twins: case report. J Neurosurg Pediatr 20(4):307-313.
- Pai KM, Naidu RC, Raja A, Rai YS, Kumar N, et al. (2018) Surgical nuances in the separation of craniopagus twins – Our experience and a follow up of 15 years. Neurol India66:426-433.
- Harvey DJ, Vaca EE, Totonchi A, Gosain AK (2018) Eleven-Year Follow-Up of Craniopagus Twins After Unsuccessful Attempt at Separation: Are They Better Off? The Clef Palate-Craniofacial Journal 56(6): 817-822.
- Harvey DJ, Totonchi A, Gosain AK (2016) Separation of Craniopagus Twins over the Past 20 years: A systemativ Review of the Variables That Lead to Successful Separation. Plastic and Reconstructive Surgery Journal 138(1): 190-200.
- Alokaili RN, Ahmed ME, Feryan AA, Goodrich JT, Aloraidi A (2015) Neurointerventional participation in craniopagus separation. Interv Neuroradiol 21(4):552-557.






























