Diagnostic Correlates of Psychiatric Presenting Symptoms of Idiopathic Basal Ganglian Calcification (Fahr’s Disease)
Shalan Joodah Rhemah Al Abbudi*
Department of Psychiatry, Consultant Psychiatrist, Imamain Kadhimain Medical City, Iraq
Submission: October 17, 2019; Published: January 8, 2020
*Corresponding author: Department of Psychiatry, Consultant Psychiatrist, Imamain Kadhimain Medical City, Baghdad, Iraq
How to cite this article: Shalan Joodah Rhemah Al Abbudi. Diagnostic Correlates of Psychiatric Presenting Symptoms of Idiopathic Basal Ganglian Calcification (Fahr’s Disease). Open Access J Neurol Neurosurg. 2020; 12(4): 555843. DOI: 10.19080/OAJNN.2020.12.555843.
Abstract
Background: Psychiatric disturbances were the major presenting symptoms of idiopathic basal ganglion calcification
Objectives: evaluation of psychological presenting symptoms, clinical and sociodemographic variables
Methods: Fahr’s disease patients were assessed by a consultant psychiatrist. Sociodemographic and clinical variables were assessed. Semi-structured clinical interview and mini-mental state examination was done. Data analysis and significance was done.
Results: total 40 patients with Idiopathic basal ganglia calcification were assessed. The age range 35-78 years mean 56.4±13 years, 64% married, 88% of higher education. Psychiatric presenting symptoms were; schizophrenia 32.1%, depression 18.9%, mania17.0%, bipolar disorder 17.0% and dementia 15.1%. Negative investigation was 3%, cognitive impairment 17%, seizures11.3%, movement disorders.5%, vertigo 26.4%, headache 9.4%, unsteadiness and difficulty of swallowing 56.6%. Psychiatric morbidity was significantly associated with; cognitive impairment (P<0.001), movement disorders (P=0.034), unsteadiness (P=0.019), difficulty of swallowing (P=0.019).
Conclusion: Fahr’s disease diagnosis could be challenging, due to discrepancy between clinical presentations and radio-imaging findings. Fahr’s disease should be kept in mind in any patients with late onset neuropsychiatric disorders
Keywords: Fahr’s disease Neuropsychiatric presentation Schizophrenia Depression
Introduction
Idiopathic basal ganglia calcification which known as Fahr’s disease [1] is chronic, slow, neurodegeneration with deposition of calcium in the basal ganglia [2], cerebellum subcortical white matter, cerebral cortex, thalamus, dentate nucleus, and hippocampus [3,4]. Globus pallidus is frequent site of the calcification. Calcification may involve other nuclei; putamen, caudate, internal capsule, dentate, thalamus, cerebellum, and cerebral white matter [5]. Histologically, the media layer of the small vessels contains proteins and polysaccharides in the perivascular space [6]. Pathogenesis may be due to blood brain barrier impairment or to a disorder of metabolism of neuronal calcium [2]. The clinical picture may accompanied by extra pyramidal and cerebellar symptoms, Parkinsonian features, convulsive seizures, speech disorders and dementia. Disease appears during age of 40-60 years [2,7,8] give a prevalence <1/1,000,000 [9]. the disease is usually of insidious onset and frequently misdiagnosed as a psychiatric illness or dementia [3]. Most cases initially presented with extra pyramidal symptoms, cerebellar dysfunction, speech difficulty, and dementia [9,10]. Fahr’s disease is most commonly transmitted as an Autosomal Dominant trait; but it may also be passed on as an autosomal recessive trait or it may occur sporadically [9,11]. The differential diagnoses of Fahr’s disease are infections, enchapalitis, calcified angiomas, and Addison’s disease[9]. Common clinical picture of the disease were headache, movement disorders such as Parkinsonism, dystonia, chorea and ataxia, syncope, seizures and psychiatric symptoms [12].
Patients and Methods
Data source
An analytic cross-sectional study conducted at Imamain Kadhimain Medical City, Psychiatry Unit, during the period from January 1st, 2014 to December 31st, 2018.
Patient selection
All patients with Fahr’s disease, both genders who have consulted during the period of study, agree to participate, wereincluded. Approval of psychiatric department was taken. A questionnaire was prepared and administered to each patient consulted during the study period.
Patients’ background characteristic
All patients attended psychiatric clinic with suspicion of Fahr’s disease were send for brain radio-imaging and blood investigations to confirm the diagnosis. A questionnaire filled out by a consultant psychiatrist, which included two parts. The first part consists of collection of clinical and sociodemographic data. The second part consists of the Mini-Mental State Examination (MMSE) to assess the cognitive impairment for each patient. Cutoff scores were 27-30 normal, 21-26 mild impairment, 11- 20 moderate impairment and ≤10 is severe impairment [13]. All patients were selected for administration of the semi-structured clinical interview for DSM-IV-TR (SCID) [14] by a consultant psychiatrist to assess the psychiatric morbidity. Other clinical symptoms were collected through the same interview.
Definition of Variables
The independent variables assumed to explain the psychiatric morbidity were socio- clinical and demographic variables. Sociodemographic includes; age, gender, marital status, education, occupation. Clinical variables include the associated features like; investigation, movement disorders, headache, vertigo, seizures unsteadiness, and difficulty of swallowing.
Statistical analysis
Data processing and analysis was conducted using a Statistical Package for Social Sciences (SPSS) version 24. Results are expressed as percentages for qualitative variables. Association between variables was assessed by Chi‑square test. P≤0.05 was considering for significant.
Ethical issues
After clarifying the objectives of the study informed consent was obtained from the patients. Names, information, interviews were kept with full privacy
Results
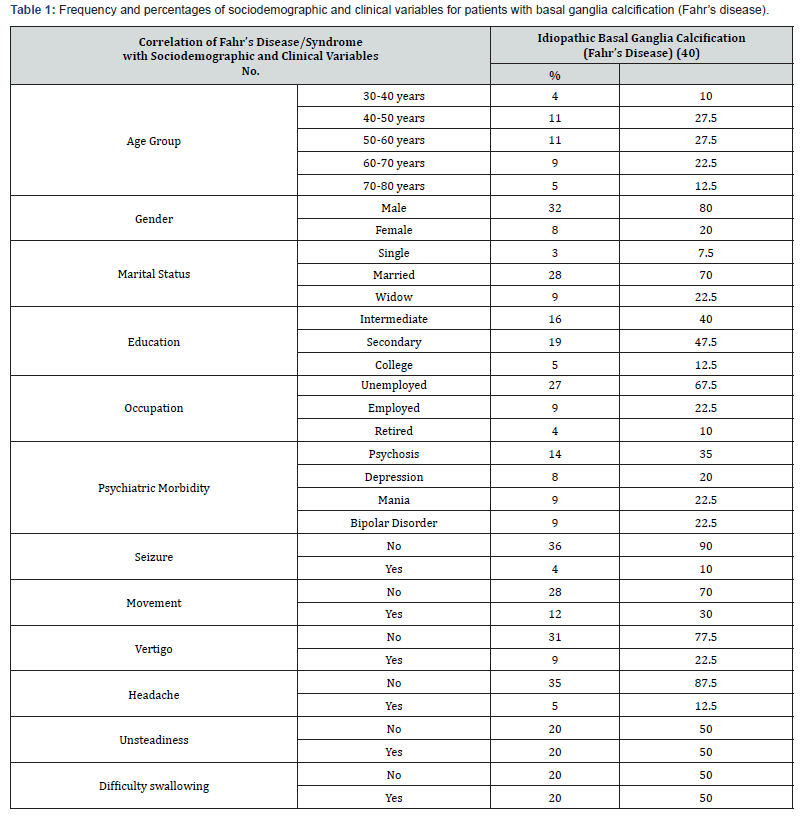
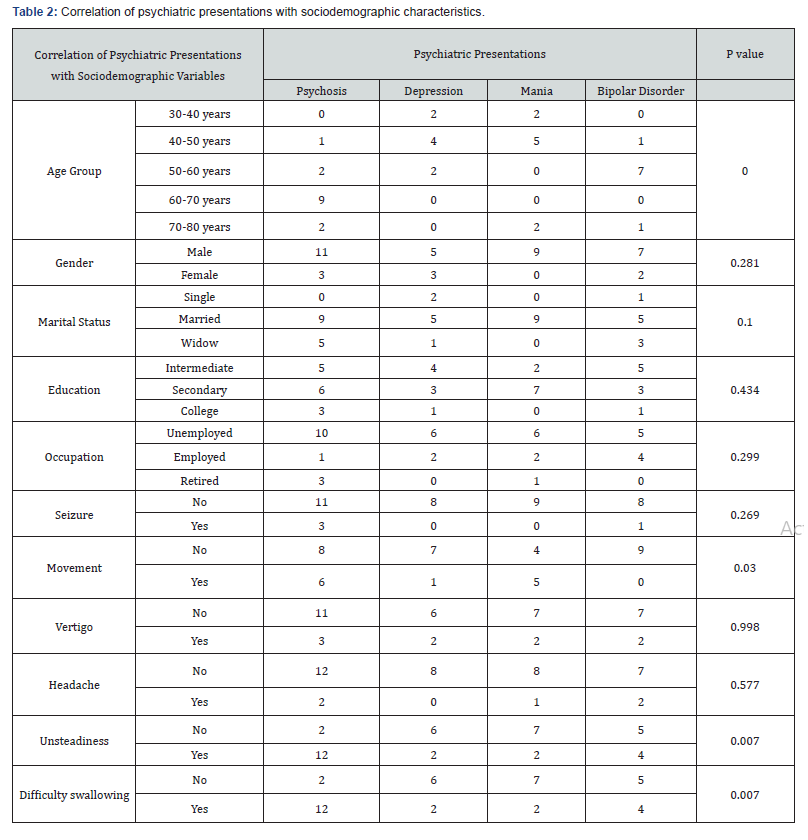
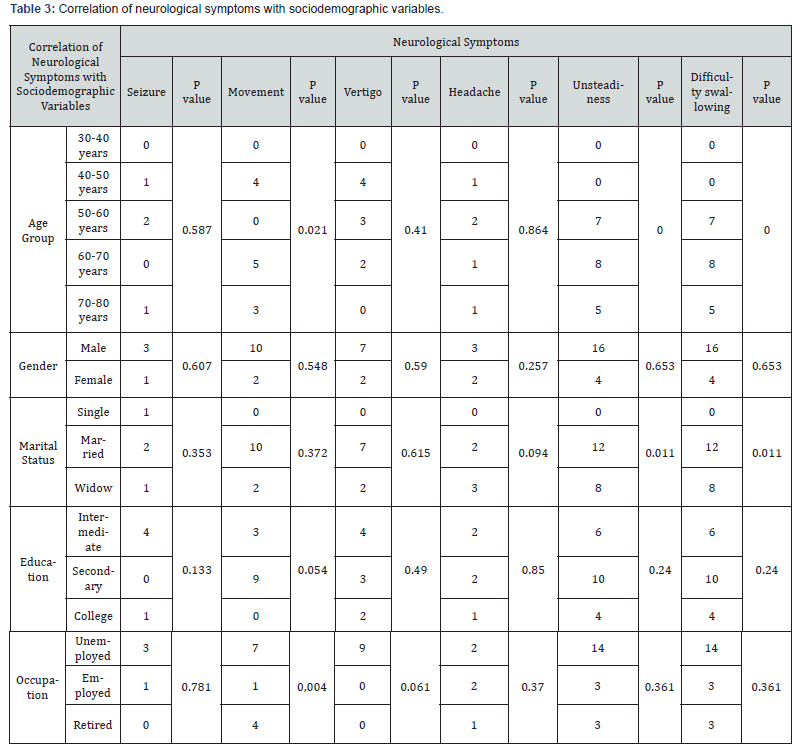
The study includes 40 patients with idiopathic calcification of basal ganglia. age range was 35-78 years, mean 56.4±13 years, half of cases fall into the age group 40 - 60 years, about 80% was male, 70% married, 87% of lower education, about three forth not working. MMSE reveals no cognitive dysfunction. Clinical interview for DSM-IV-TR (SCID) found that; psychosis and schizophrenia 14 (35%), depression 8 (20%), mania (9) 22.5%, and bipolar disorder (9) 22.5%. Investigation regarding parathyroid hormone, calcium and phosphate were negative. Abnormal movements Parkinson like symptoms; tremor, rigidity, was 30% of patients. Four percent have history of seizures. Vertigo present in 22.5% of patients. Headache present in 12.5% of patients. Unsteadiness and difficulty of swallowing found among 50% of patients (Table 1). Correlation of sociodemographic variables with psychiatric presentation was done. Psychiatric presentation of patients with basal ganglia calcification was significantly associated with age (P<0.001), movement disorders (P=0.034), unsteadiness (P=0.019), difficulty of swallowing (P=0.019) (Table 2). Correlation of sociodemographic and neurological symptoms of patients found significant association of age with movement disorders (P=0.021), unsteadiness (P<0.001), and difficulty of swallowing (P<0.001). Marital status was significantly associated with unsteadiness (P=0.011), difficulty of swallowing (P=0.011). Occupation was significantly associated with movement disorder (P=0.004) (Table 3).
Discussion
The psychiatric presentation of patients with Fahr’s disease was psychosis and schizophrenia 35%, mania 22.5%, bipolar disorder 22.5%, and depression 20%. The neurological symptoms were; abnormal movements; Parkinson like symptoms; tremor, rigidity, 30%, unsteadiness 50%, difficulty of swallowing 50%, vertigo 22.5%, headache 12.5%, and seizures 4%, Around 40% of patients with basal ganglia calcifications presented with psychiatric symptoms [15]. Studies suggest criteria for the diagnosis of Fahr’s disease include [16]; bilateral basal ganglia calcification; progressive neuropsychiatric symptoms; late onset in the fourth or fifth decade but earlier onset can also occur. Fahr’s disease symptoms are reported individual case reports because of the clinical rarity of the disease [17] thus no exact figures to compare this study results with it. Psychiatric symptomatology of Fahr’s disease might be the results of the interaction of basal ganglia and cerebellum. Fahr’s disease patients of this study showed negative results of investigations. MMSE results were no cognitive dysfunction in patients with Fahr’s disease. Movement disorders account for 55% of the total symptomatic Fahr’s disease patients [2]. The dentate nucleus of the cerebellum provides disynaptic inputs to the basal ganglia [15], and motor and non-motor domains of the substantia nigra provide disynaptic inputs to the cerebellar cortex. These interactions may have clinical implications for neuropsychiatric disorders such as schizophrenia [18]. The basal ganglia may be involved in generating neuropsychiatric symptoms in major psychiatric disorders such as schizophrenia and depression [19]. Several basal ganglia disorders can have psychiatric manifestations [15]. The common psychiatric features are cognitive deterioration, psychotic symptoms, and mood disorders [20]. Organic affective symptoms were found more common in chronic cases of basal calcification15. Calcifications sites, clinical features and relevant investigations are important particularly upon incidental cases presenting with disorganised behavior, as there may be no other significant clinical features. Calcifications should be evaluated with clinical pictures for proper diagnosis [3].
Conclusion
Fahr’s disease diagnosis could be challenging, due to discrepancy between clinical presentations and radioimaging findings. Clinical presentation includes psychiatric and neurological symptoms. Psychiatric symptoms include;schizophrenia, psychosis, bipolar disorder, mania and depression. Neurological symptoms include Parkinson’s like movement, seizures, vertigo, headache, unsteadiness, and difficulty of swallowing. Fahr’s disease should be kept in mind in any patients with neuropsychiatric disorders.
Acknowledgement
We greatly appreciate the patients, their families, and medical staff of psychiatry unit, Imamain Kadhimain medical city, for their participation
References
- Mohammed D, Ibrahim GH, Sadisu MM, Saidu A, Sule SA, et al. (Idiopathic Bilateral Strio-Pallido-Dentate Calcinosis (Fahr’s Disease) and Chronic Subdural Haematoma In A 40-Year-Old Woman with Depression: A Case Report. IOSR Journal of Nursing and Health Science 6(2): 31-34.
- Asokan AG, D souza S, Jeganathan J, Pai S (2013) Fahr's Syndrome- An Interesting Case Presentation. J Clin Diagn Res 7(3): 532-533.
- Marinković DM, Dragović T, Kiković S, Janković SK, Djuran Z, et al. (2017) Fahr’s syndrome and idiopathic hypoparathyroidism – A case report. Vojnosanit Pregl 74(2): 184-188.
- Kavirayani DK, Jammulapati S (2014) Fahr's syndrome with psychotic features: Review and Case report. NMJ 3(2): 71-74.
- Kotan D, Aygul R (2009) Familial Fahr’s disease in a Turkish family. South Med J 102(1): 85-86.
- Malik R, Pandya VK, Naik D (2004) Fahr’s disease: A rare neurodegenerative disorder. Indian J Radiol Imaging 14: 383-384.
- Gülsün M, Baykız AF, Kabata S, Belli H (2006) Fahr’s Syndrome - Three cases presenting with psychiatric signs. Eur J Gen Med 3(1): 35-40.
- Kotan D, Aygul R (2009) Familial Fahr’s disease in a Turkish family. South Med J102(1): 85-86.
- Saleem S, Aslam H M, Anwar M, Anwar S, Saleem M, et al. (2013) Fahr’s syndrome: literature review of current evidence. Orphanet J Rare Dis 8: 156.
- Chiu HF, Lam LC, Shum PP, Li KW (1993) Idiopathic calcification of the basal ganglia. Postgrad Med J 69(807): 68-70.
- Yamada N, Hayashi T (2000) Asymptomatic familial basal ganglia calcification with autosomal dominant inheritance: a family report. No to Hattatsu 32(6): 515-519.
- Utku U, Utku BA (2014) Fahr’s Syndrome Case Presented with Vertigo. Eur J Gen Med 11(2): 115-116.
- Albanna M, Yehya A, Khairi A, Dafeeah E, Elhadi A (2017) Validation and cultural adaptation of the Arabic versions of the Mini–Mental Status Examination – 2 and Mini-Cog test. Neuropsychiatric Disease and Treatment 13: 793-801.
- First MB, Gibbon M, Spitzer RL (2001) User’s Guide for the Structured Clinical Interview for DSM-IV-TR Axis I Disorders: SCID-I, Research Version. New York, New York State Psychiatric Institute, Biometric Research Department, USA.
- Mufaddel AA, Al-Hassani GA (2014) Familial idiopathic basal ganglia calcification (Fahr’s disease). Neurosciences 19 (3): 171-177.
- Lazar M, Ion DA, Streinu-Cercel A, Badarau AI (2009) Fahr’s syndrome: diagnosis issues in patients with unknown family history of disease. Rom J Morphol Embryol 50(3): 425-428.
- Abubakar SA, Saidu S (2012) Idiopathic bilateral strio-pallido-dentate calcinosis (Fahr’s disease): a case report and review of the literature. Ann Afr Med 11(4): 234-237.
- Bostan AC, Strick PL (2010) The cerebellum and basal ganglia are interconnected. Neuropsychol Rev 20(3): 261-270.
- Ring HA, Serra-Mestres JS (2002) Neuropsychiatry of the basal ganglia. J Neurol Neurosurg Psychiatry 72(1): 12-21.
- Konig P (1989) Psychopathological alterations in cases of symmetrical basal ganglia sclerosis. Biol Psychiatry 25(4): 459-468.






























