Surgical Implication of a Cavernous Hemangioma of the Optic Chiasm Showing Recurrent Hemorrhage After Long-Term Clinical Stability: A Case Report
Takeru Umemura1*, Shigeru Nishizawa2, Junkoh Yamamoto2
1Department of Neurosurgery, Kyushu Rosai Hospital, Moji Medical Center, Japan
2Department of Neurosurgery, University of Occupational and Environmental Health, Japan
Submission: December 01, 2018; Published: February 07, 2019
*Corresponding author: Takeru Umemura, Department of Neurosurgery, Kyushu Rosai Hospital, Moji Medical Center, 3-1 Higashiminatomachi, Moji-ku, Kitakyushu City, Fukuoka 801-8502, Japan
How to cite this article: Takeru U, Shigeru N, Junkoh Y. Surgical Implication of a Cavernous Hemangioma of the Optic Chiasm ShowingRecurrent Hemorrhage After Long-Term Clinical Stability: A Case Report. Open Access J Neurol Neurosurg. 2019; 9(4): 555769. DOI: 10.19080/OAJNN.2019.09.555769.
Abstract
Cavernous hemangiomas of the optic chiasm are rare, and hemorrhage from cavernous hemangiomas causes acute visual loss. Although some cases have been reported, the appropriate treatment has not been determined yet because of the scarcity of these reports. Here, we describe a patient with recurrent hemorrhage from a cavernous hemangioma of the optic chiasm after a long clinically stable period, and we discuss the surgical implication of this lesion. A 45-year-old man sustained right visual loss due to hemorrhage from a cavernous hemangioma of the optic chiasm 20 years ago and was conservatively observed. He suffered from acute visual loss in the left eye following sudden onset of headache, and he was hospitalized in our hospital. The patient complained of severe visual disturbance in the left eye in addition to long-term right visual loss. Magnetic Resonance Imaging showed recurrent hemorrhage from the lesion, and the whole chiasm was affected. We performed total excision of the lesion, and his vision improved, enabling him to return to work. This is the first report of recurrent hemorrhage from a cavernous hemangioma of the optic chiasm. We recommend surgical resection, even in clinically stable patients, to prevent recurrence.
Keywords: Optic chiasm; Cavernous hemangioma; Recurrent hemorrhage; Surgical indication
Abbrevations: MRI: Magnetic Resonance Imaging; CISS: Constructive Interference in Steady State
Introduction
Cavernous hemangiomas, also known as cavernous malformations or cavernomas, are vascular malformations characterized by the presence of sinusoid-like capillary vessels [1,2]. They can develop in several locations in the central nervous system, such as in the cerebrum, cerebellum, brainstem, and spinal cord) [3]. However, cases of cavernous hemangiomas involving the cranial nerves are rarely reported. In particular, cavernous hemangiomas involving the optic pathway are extremely rare [4,5]. Therefore, treatment is controversial. Total excision is recommended for most symptomatic patients [6-8]. On the other hand, symptomatic patients may experience improvement after shrinkage of the cavernous hemangioma even without any surgical treatment, and only conservative follow-up is recommended in these cases [9]. Moreover, the surgical indication is obscure in patients with a long-term stable condition after the first episode of hemorrhage, as postoperative visual deficits are associated with decreased activities of daily living.
Here, we describe a patient with recurrent hemorrhage from a cavernous hemangioma of the optic chiasm whose symptoms had remained stable since the initial hemorrhage occurred 20 years ago, and we discuss the surgical indication of the lesion.
Case report
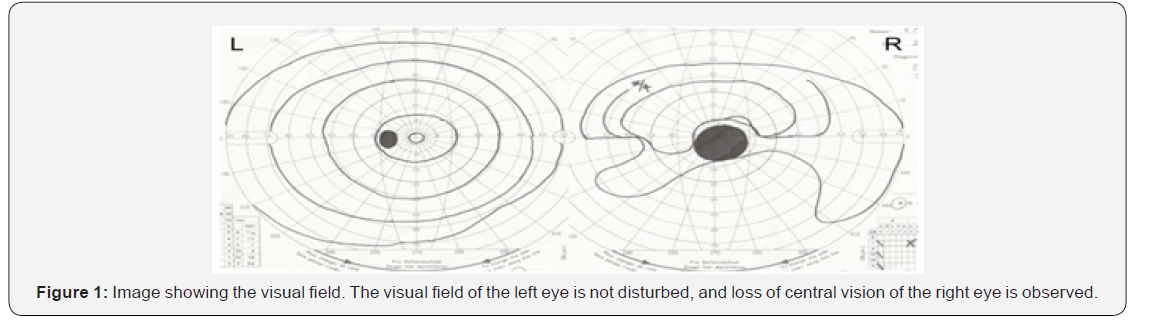
A 45-year-old man with acute visual loss in the left eye was admitted. He had a history of hemorrhage from a cavernous hemangioma of the optic chiasm. Since then, he lost central vision loss in the right eye 20 years ago, although left visual acuity was kept intact. Upon admission, he complained of a headache and left visual disturbance in addition to long-term right visual loss. The neuro-ophthalmological evaluation revealed severe left visual disturbance with the preservation of normal pupillary reaction to light in both eyes. The serological examination showed no pituitary dysfunction. Visual disturbance results were as follows: right 0.02 (nc) and left 0.4 (nc). Figure 1 shows the visual field. Visual loss in his right eye was due to previous hemorrhage from the cavernous hemangioma of the optic chiasm, whereas visual loss in his left eye was due to recurrence of the hemorrhage. A computed tomogram showed the hemorrhage in the optic chiasm (Figure 2A). Magnetic Resonance Imaging (MRI) was performed, and an axial Constructive Interference in Steady State (CISS) image showed that the lesion was a 10-mm mass with partial hyperintensity (Figure 2B). On the coronal MRI CISS image, the patient had multilocular lesions of different intensities that were found on the right side of the optic chiasm (Figure 2C). Cerebral angiography did not reveal any vascular malformations. We considered that the left eye worsened because the hemorrhage extended over the midline. The preoperative diagnosis was hemorrhage from the cavernous hemangioma of the optic chiasm, and we decided to perform surgical decompression of the optic chiasm.

Surgery was performed via a right pterional approach. The Sylvian fissure was widely opened, and the optic chiasm was exposed (Figure 3A). The lesion was brown, and bipolar coagulation was performed. The cavernous hemangioma shrunk and was dissected from the optic chiasm (Figure 3B), which was surrounded by gliosis at the interface. The lesion was totally removed. The histopathological analysis of the resected lesion showed vascular spaces containing blood elements, lined by a single layer of endothelial cells, and the lesion was diagnosed as a cavernous hemangioma.

The postoperative ophthalmological examination revealed improvement of visual disturbance in the left eye up to 0.9 (nc) without changes in the visual field and vision in the right eye.
Discussion
A cavernous hemangioma of the optic chiasm is rare [4,5]. Some cases have been reported, and the authors recommended total excision of the cavernous hemangioma of the optic chiasm [6-8], because early diagnosis is associated with good results and the prevention of recurrent hemorrhage [9,10]. However, clinical improvement can occur without operation; thus, close follow-up was recommended by other authors.
In our case, the patient sustained acute visual loss in the right eye due to hemorrhage from a cavernous hemangioma in the optic chiasm 20 years ago, and no clinical change occurred until the present admission. Recurrent hemorrhage from the cavernous hemangioma of the optic chiasm occurred again, and visual function worsened because of the expanding hemorrhage. If hemorrhage from the optic chiasm occurs again, visual loss will worsen even if the hemorrhage is small. Therefore, we consider that surgical treatment is the first choice for cavernous hemangiomas of the optic chiasm. Even in clinically stable patients, like ours, the potential for hemorrhage still exists. According to the literature, vascular malformations of cavernous hemangiomas of the optic chiasm occur more frequently than hemorrhages in the brain [10,11]. Therefore, previous studies support our opinion. We also considered that excising the hemangioma of the optic nerve could be conducted without causing neurological deficits; additionally, it may improve visual disturbance because the gliotic interspace between the hemangioma and normal neural tissue provides a plane for dissection, and decompression of the optic nerve may lead to good results [10]. In our case, we confirmed the gliotic interspace, and it made excision safe and accurate.
According to the literature, conservative treatment is also recommended because visual loss may improve after shrinking the cavernous hemangioma [9]. However, this treatment is not curative because the hemangioma remains intact and can bleed again. Visual loss may be severe if hemorrhage recurs. on the basis of MRI findings, we confirmed that the mass included lesions of different intensities. Based on the appearance of the lesions and pathological findings [12], the different intensities shown on the MRI CISS image suggested different stages of hemorrhage. This finding supports the diagnosis of cavernous hemangioma.
Conclusion
In conclusion, cavernous hemangiomas of the optic chiasm, even in clinically stable patients, need to be totally excised to prevent recurrent hemorrhage. In addition, MRI CISS imaging is useful for evaluating the hemorrhage.
References
- Murai Y, Adachi K, Koketsu K, Teramoto A (2011) Indocyanine green videoangiography of optic cavernous angioma - case report. Neurol Med Chir (Tokyo) 51(4): 296-298.
- Alafaci C, Grasso G, Granata F, Cutugno M, Marino D, et al. (2015) Cavernous malformation of the optic chiasm: an uncommon location. Surg Neurol Int 6: 60.
- Scholz M, Harders A, Lücke S, Pechlivanis I, Engelhardt M, et.al. (2008) Successful resection of the recurrence of a cavernous malformation of the optic chiasm. Clin Ophthalmol 2(4): 945-949.
- Iwai Y, Yamanaka K, Nakajima H, Miyaura T (1999) Cavernous angioma of the optic chiasm--case report. Neurol Med Chir (Tokyo) 39(8): 617–620.
- Rotondo M, Natale M, D Avanzo R, Pascale M, Scuotto A (2014) Cavernous malformations isolated from cranial nerves: unexpected diagnosis? Clin Neurol Neurosurg 126: 162-168.
- Panczykowski D, Piedra MP, Cetas JS, Delashaw JB Jr (2010) Optochiasmatic cavernous hemangioma. Br J Neurosurg 24(3): 301-302.
- Hempelmann RG, Mater E, Schröder F, Schön R (2007) Complete resection of a cavernous haemangioma of the optic nerve, the chiasm, and the optic tract. Acta Neurochir (Wien) 149(7): 699-703.
- Meng C, Bi Z, Jiang H, Jing Y, Wang J (2015) [Eight cases of cavernous hemangioma of the optic chiasm]. Zhonghua Yan Ke Za Zhi 51(12): 907-911.
- Marnat G, Gimbert E, Berge J, Rougier MB, Molinier S, et al. (2015) Chiasmatic cavernoma haemorrhage: to treat or not to treat? Concerning a clinical case. Neurochirurgie 61(5): 343-346.
- Shibuya M, Baskaya MK, Saito K, Suzuki Y, Ooka K, et al. (1995) Cavernous malformations of the optic chiasma. Acta Neurochir (Wien) 136(1-2): 29-36.
- Trentadue M, Pozzi Mucelli R, Piovan E, Pizzini FB (2016) Incidental optochiasmatic cavernoma: case report of an unusual finding on 3 Tesla MRI. Neuroradiol J 29(4): 289-294.
- Venkataramana NK, Rao SA, Arun LN, Krishna C (2016) Cavernous malformation of the optic chiasm: neuro-endoscopic removal. Asian J Neurosurg 11(1): 68-69.






























