Skin Closure: Our Experience with Glue in Spinal Surgical Cases. A Ten Years Experience
Leonello Tacconi* and Roberto Spinelli
Department of Neurosurgery, Azienda Universitaria Integrata, Italy
Submission: February 19, 2018; Published: March 14, 2018
*Correspondence author: Leonello Tacconi, Department of Neurosurgery, University Hospital of Trieste, Strada di Fiume, 447, Trieste, 34149, Italy, Tel: +39-040-3994041; Email: leonello.tacconi@asuits.sanita.fvg.it
How to cite this article: Leonello T, Paolo B. L5-S1 Disk Prolapse: Pure Endoscopic Approach: Our Experience. Open Access J Neurol Neurosurg. 2018; 7(2): 555709. DOI: 10.19080/OAJNN.2018.07.555709
Abstract
Background: There are two main different techniques for skin closure: sutures and metal clips. Besides these, cyanoacrylate has been correlated with good results in a wide variety of surgical fields. In this study, we describe our experience in the use of cyanoacrylate for the closure of spinal surgical wounds.
Methods: We prospectively selected 475 patients (30.3%) among a surgical series of 1567 patients who had undergone spinal surgery (lumbar disk surgery; lumbar decompression or foraminotomy; cervical anterior decompression or posterior foraminotomy) in a four years period. All the wounds, with a length shorter of 10 cm were closed with glue. Among all cases 126 (26.5%) operations had been performed in the elderly (71-83 years) and 35 (7.3%) were reoperation. We evaluated three parameters: the cosmetic results; the rate of wound complication and the patients satisfaction at 4 weeks, 6 and 12 months.
Results: In the entire series we had only 4 (0.8%) wound complication. From a cosmetic point of view almost all the wounds had a nice looking appearances at 6 months (98.9%). The patients satisfaction reached almost 100%. This study confirm that cyanoacrylate glue can be a valid and useful alternative also for spinal wound closure.
Keywords: Cyanoacrylate; Polymer; Wound; Infection; Cosmetic; Spine; Wound closure
Introduction
Besides the two classic skin closure techniques (sutures and metal clips) there is a third less used alternative especially in spine and neurosurgical wounds: the N-butyl cyanoacrylate (CNA). This polymer, which derives from a mix between cyanoacetate and formaldehyde, has already been correlated with positive effects in the wound healing process thanks to its properties such as neo vascularization, re-epithelialization and even antimicrobial activity [1-3]. Historically CNA polymers have been used in a wide variety of medical and surgical situations but its use in the neurosurgical field is still limited. This is mainly due to the surgeons' fear of wound closure breakage. However, along the years more and more articles have been published on its use in neurosurgery. In a previous paper from our Unit we have discussed the efficacy and usefulness of using glue for closing neurosurgical cranial wounds and we concluded that CNA was related to the same cosmetic results with concurrently a higher patient satisfaction and a reduced time closure when compared to traditional sutures [4].
In this article we would like to report our experience along a four years period with the use of CNA for the closure of spinal surgical wounds. We focused our attention, particularly, to the rate of postoperative wound complications, the cosmetic results as well as the patients satisfaction after a year follow up.
Materials and Methods
From January 2012 to January 2016 we prospectively selected 475 cases (30.3%) from a consecutive surgical series of 1567 patients, who underwent an elective spinal surgical procedure requiring a length skin incision shorter than 10cm. Emergent procedures, post traumatic skin lacerations and surgical sites suspicious for infection were excluded from the study. Our cohort was composed by 217cases (45.6%) operated on for a lumbar disk herniation either by microsurgical or endoscopic technique; 95 (21%) were lumbar microsurgical foraminotomy; 60 (13.2%) were single or double levels lumbar laminectomy; 9 were lumbar endoscopic decompressionand 71 (18 cases) were anterior cervical microdiscectomy. Twenty-six cases (5.7%) were reoperation and 69% of these were located in the lumbar region. If we consider, instead, the number of elderly people (older than 70 years old) from the entire group they were 126 (26.5%). Their median age was 76 years with a range between 71 and 83 year old. Of all 475 patients we registered the length of the wounds. The median was 4.5cm with a range from 0.8 cm to 10 cm. In the elderly group the median wound length was 7cm (4-10cm).We checked for wound complications; cosmetic results and patient satisfaction at 4 weeks, 6 and 12 months post operatively. The cosmetic results were divided in three categories: good, satisfactory and bad.
Results
The median follow up time was 14 months (range 12-18 months). At the first follow up interval (4 weeks) there was only one wound complication: a wound dehiscence secondary to cerebral spinal fluids (CSF) leakage which settled with a lumbar spinal drain. At two months we experienced two more wounds dehiscence secondary to superficial wounds infection by Staphylococcus aureus. Both improved, one with antibiotics and the second after wound debridement. The last complication was a reddish and hypertrophic wound neck scar which was present at 10 weeks and remained the same at 6 months. It however, improved at 12 months. From a cosmetic point of view at 4 weeks only 63.3% of the patients had a nice appearances care (20.6% in the elderly). This value increased respectively to 99.3% and 55.5% at 6 months to reach almost 100% in both group at 12 months. The patients satisfaction results were, instead, very high in both groups, reaching 100% in the elderly one (Table 1 & 2).


Discussion
At the end of an operation the surgeon can be tired or keen to leave the operating room to do something else and very often we consider the action of skin closure a trivial step. Instead it is an important phase of the operation not only for a cosmetic purpose, but also because a deficient skin closure increases the possibility of wound infection and many medical legal actions are carried out exactly for this reasons. The two classic closure' s methods , used worldwide, are the skin sutures (SS) and metal skin clips (SC). They are both effective but if we want to achieve a better cosmetic result, in a young patient or in a visible area, we have to use an intradermic running suture which gives a nicer result but it is very time consuming compared to SC. In the recent years, a new attractive technique has become a useful and valid alternative: the N-butyl cyanoacrylate (CNA) [4,5]. CNA monomers are made by condensation of cyanoacetate and formaldehyde. This polymers induce healing by neovascularization, re-epithelialization as well as they seem to be correlated to a strong antimicrobial activity, especially versus Gram Positive Strains [1-3]. Skin glue and sutures have a comparable strength closure [6].
CNA polymers has already been widely used in a various and heterogeneous medical fields: esophageal varices, general, ophthalmic, plastic, breast and cardiac surgery, cerebral arteriovenous malformation and even in cranial fixation after traumas [1,7-18]. Howard reported a large series of patients who underwent posterior spinal surgery with fusion at cervical, thoracic and lumbar levels. According to the Author, CNA is not related to greater rates of cerebrospinal fluid leak or wound infection if compared to traditional techniques [19]. Wachter et al. [20] reported similar results. Usefulness of CNA has also been verified in pediatric neurosurgery, where the need to remove sutures can causes an important discomfort in young patients. Wang and his colleagues reported a series of 102 cases with 142 incisions (mainly scalp and abdominal, but also spinal) with only 1 case with poor cosmetic result and no cases of infections [21]. Ando et al. [22] described less wound infection rate with the use of CNA than with staples for spinal surgery [22] and Eymann reported similar results for pediatric shunt procedures [23].
Further advantages of using CNA are that the method is faster than traditional skin closure, the patients cantake a shower also the same day of the surgical procedure, there is no need to apply a skin bandage and no necessity to remove the stitches [4,19]. Therefore the number of postsurgical outpatient visits is decreased with a consistent save for the National Health System and an easier logistic situation for the patient especially if old. Also the possibility to have a shower the day after surgery, without any precautions, has been very much appreciated by our patients as well as the idea to wear some clean clothes and go home very soon. In our previous study we assessed the efficacy and time consuming of this method on a smaller series and furthermore, all of them were cranial cases. In this report we wanted, instead, to determine the complication rate, the cosmetic results as well as the patients satisfaction on a much larger group of patients operate on in a different anatomical location: the spine. We also wanted to evaluate the cosmetic result at a longer follow up (one year) and because of the larger number of cases we were also able to assess the same end points for an elderly population group. Arbitrarily, we have decided to include in the study all patients with a wound which did not exceed 10 cm. This was due to our fear that long wounds and the bed prone position after surgery could increase the chances of wound breaking down. For this reason we started this study, to assess the glue's efficacy in this anatomical region, with a prudential protocol. We consider our study results very positive. We would like to point out the fact that the cosmetic wounds appearance becomes very nice only after several months while it did not look satisfactory in the short terms: only 63% and even less, 20% in the elderly population at 4 weeks follow-up. At six months the percentage of nice looking appearance wounds rose up, respectively, to 99.3% and 55.5% to reach almost 100% at 12 months in both group. Probably this is due to the fact that it takes at least 3-4 weeks for the glue to completely disappear and only after this phase the superficial skin healing process might start and this process takes longer in the elderly. In order to classify a wound appearance in nice, satisfactory or bad we took into consideration mainly the color of the zone; the presence of edge’s elevation and a well established nice, flat, color skin scar. Very interesting instead, the patients satisfaction was very high with a 99.3% in the entire group and not surprisingly a 100% in the elderly. This signifies the usefulness of this method, especially for old people, in reducing the number of hospital visits just for a simple medication or stiches removal; helping them mainly from a logistic transport point of view.
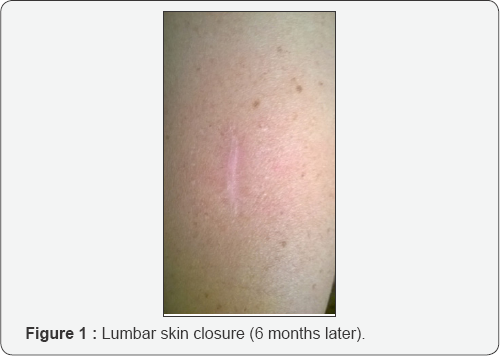
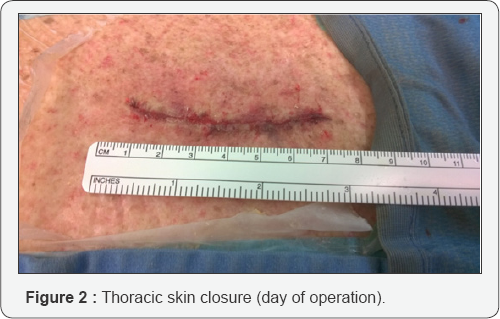
Regarding the number of complications these were very few: only 4 (0.8%) and certainly they were well below the general standard infection rate. One was a 67 year old male with a history of diabetes mellitus, who underwent a microsurgical removal of a right L5-S1 disk prolapsed. The surgery was uneventful and the patients was discharged home in 2 days. Six weeks later he came back because his wife had noticed a 1cm opening in the cranial portion of the wound which was also red and slightly swollen. We put him on oral antibiotics for a week and 14 days later the wound was perfectly closed. The third complication was about a 75 year old man who underwent a L4 laminectomy for a central canal stenosis. The surgical procedure was uneventful and the patient was discharged home 4 days later. After 5 weeks the wound became reddish and tense. Two days later the wound started to secret. Blood labs revealed an increasing of the C-reactive protein and slight elevated white cells count. MR imaging were compatible with a superficial infection. The patient was reopened, the wound washed out and the skin was again glued. This patient was discharged home 8 day later. At the latest follow up he is fine with a nice surgical scar. The last complication was an ugly hypertrophic neck scar which improved almost to a satisfactory one at 12 months having had many laser treatments (Figure 1 & 2).
Conclusion
Although this study, is not a randomized controlled one, it may point to the fact that CNA is effective for standard skin closure for spinal surgical wounds, it carries an acceptable percentage of complication and is very well accepted by the patients. At 12 months follow up also the cosmetic results are extremely beautiful. Naturally we do not know yet if it can also be used safely for longer wound like procedures for spinal imbalance or scoliosis. Probably in these case a tighter and carefully subcutaneous layer must be achieved.
References
- Refojo MF, Dohlman CH, Ahmad B, Carroll JM, Allen JC (1968) Evaluation of Adhesives for Corneal Surgery. Archives of Ophthalmology 80(5): 645-656.
- Romero I, Malta JNS, Silva C, Mimica LJ, Soong K, et al. (2009) Antibacterial properties of cyanoacrylate tissue adhesive: Does the polymerization reaction play a role? Indian Journal of Ophthalmology [Internet]. 57(5): 341-344.
- Quinn JV, Osmond MH, Yurack JA, Moir PJ (1995) N-2- Butylcyanoacrylate: risk of bacterial contamination with an appraisal of its antimicrobial effects. The Journal of international medical research 13(4): 581-585.
- Chibbaro S, Tacconi L (2009) Use of skin glue versus traditional wound closure methods in brain surgery: A prospective, randomized, controlled study. Journal of Clinical Neuroscience 16(4): 535-539.
- 5. Sabol F, Vasilenko T, Novotny M, Tomori Z, Bobrov N, et al. (2010) Intradermal running sutures versus 3M Vetbond tissue adhesive for wound closure in rodents: a biomechanicl and histological study. 45(3-4): 321-326.
- Shapiro AJ (2001) Tensile strength of wound closure with cyanoacrylate glue. American Surg: 67(11): 1113-1115.
- Sultan A, Mohamed A (2017) Efficacy and safety of using n-butyl cyanoacrylate in cranial fixation following trauma and other pathologies. Turk Neurosurg (1): 1-5.
- Toriumi DM, O'Grady K, Desai D, Bagal A (1998) Use of octyl-2- cyanoacrylate for skin closure in facial plastic surgery. Plast Reconstr Surg 102(6): 2209-2219.
- Gennari R, Rotmensz N, Ballardini B, Scevola S, Perego E, et al. (2004) A prospective, randomized, controlled clinical trial of tissue adhesive (2-octylcyanoacrylate) versus standard wound closure in breast surgery. Surgery 136(3): 593-599.
- Greene D, Koch JR, Goode RL (1999) Efficacy of Octyl-2-Cyanoacrylate tissue glue in blepharoplasty. Arch Facial Plast Surg 1(4): 292-296.
- Jallali N, Haji A, Watson CJE (2004) A prospective randomized trial comparing 2-Octyl Cyanoacrylate to conventional suturing in closure of laparoscopic cholecystectomy incisions. J Laparoendosc Adv Surg Tech 14(4): 209-211.
- Maartense S, Bemelman WA, Dunker MS, de Lint C, Pierik EGJM, et al. (2002) Randomized study of the effectiveness of closing laparoscopic trocar wounds with octylcyanoacrylate, adhesive papertape or poliglecaprone. Br J Surg 89(11): 1370-1375.
- Matin SF (2003) Prospective randomized trial of skin adhesive versus sutures for closure of 217 laparoscopic port-site incisions. J Am Coll Surg 196(6): 845-853.
- Ong CCP, Jacobsen AS, Joseph VT (2002) Comparing wound closure using tissue glue versus subcuticular suture for pediatric surgical incisions: A prospective, randomised trial. Pediatric surgery international 18(5-6): 553-555.
- Petratos PB, Rucker GB, Soslow RA, Felsen D, Poppas DP (2002) Evaluation of octylcyanoacrylate for wound repair of clinical circumcision and human skin incisional healing in a nude rat model. J Urol 167(2 I): 677-679.
- Rosin D, Rosenthal RJ, Kuriansky J, Brasesco O, Shabtai M, et al. (2001) Closure of laparoscopic trocar site wounds with cyanoacrylate tissue glue: a simple technical solution. Journal of laparoendoscopic & advanced surgical techniques Part A [Internet] 11(3): 157-159.
- Sebesta MJ, Bishoff JT (2003) Octylcyanoacrylate skin closure in laparoscopy. J Endourol 17(10): 899-903.
- Singer AJ, Quinn JV, Clark RE, Hollander JE (2002) Closure of lacerations and incisions with octylcyanoacrylate: A multicenter randomized controlled trial. Surgery 131(3): 270-276.
- Howard BM, Eshraghi SR, Holland CM, Refai D (2014) Octyl- cyanoacrylate skin adhesive is effective for wound closure in posterior spinal surgery without increased risk of wound complications. Clin Neurol Neurosurg 125: 137-142.
- Wachter D, Bruckel A, Stein M, Oertel MF, Christophis P, et al. (2010) 2-Octyl-cyanoacrylate for wound closure in cervical and lumbar spinal surgery. Neurosurgical Review 33(4): 483-489.
- Wang MY, Levy ML, Mittler MA, Liu CY, Johnston S, et al. (1999) A prospective analysis of the use of octylcyanoacrylate tissue adhesive for wound closure in pediatric neurosurgery. Pediatric Neurosurgery 30(4): 186-188.
- Ando M, Tamaki T, Yoshida M, Sasaki S, Toge Y, et al. (2014) Surgical site infection in spinal surgery: A comparative study between 2-octyl- cyanoacrylate and staples for wound closure. European Spine Journal 23(4): 854-862.
- Eymann R, Kiefer M (2010) Glue instead of stitches: a minor change of the operative technique with a serious impact on the shunt infection rate. Acta Neurochir Suppl 106: 87-89.






























