Recurrent Disc Prolapsed: Is the Endoscopic Approach Useful? Our Experience
Leonello Tacconi* and Paolo bobicchio
Neurosurgical unit, Azienda Universitaria Integrate, Trieste, Italy
Submission: February 04, 2018; Published: February 27, 2018
*Corresponding author: Leonello Tacconi, Neurosurgical Unit, Azienda Universitaria Integrate, Trieste, Italy, Email: leonello.tacconi@asuits.sanita.fvg.it
How to cite this article: Tacconi L and Bobicchio P. Recurrent Disc Prolapsed: Is the Endoscopic Approach Useful? Our Experience. Open Access J Neurol Neurosurg. 2018; 7(2): 555706. DOI: 10.19080/OAJNN.2018.07.555706.
Introduction
Surgery for lumbar disc prolapse either way is performed (by an open midline microdiscectomyor a MIS technique) has a recurrence rate which varies from 5% to 18% i and in the majority of cases ends with a new operation [1]. The standard surgical technique for a recurrent disc prolapse implies a minimal mount of bony removal and most important, it is generally necessary to work through a scar tissue in order to reach the offended nerve root. Therefore there is a higher possibility of complication like CSF leak, neurological deficits, mechanical instability and postoperative pain.
With the introduction of the endoscopic technique in the neurosurgical field, many surgeons have started to treat recurrent disc, already operated on by a standard microsurgical approach, with the use of the endoscope [2]. With this technique it is possible to reach the pathology via a "virgin route" avoiding the time consuming and the dangerous scar tissue dissection.
In our Unit we have started to implement the endoscope in disk prolapse in 2015 and only after we have overcome the learning curve phase we have applied this technique also for recurrent disc. We present our experience on 17 recurrent disc cases operated on by endoscopic technique. The results, complication, as well as our philosophy to approach recurrent lumbar disc will be discussed.
Material and Methods
From May 2016 to March 2017 we collected, prospectively, 17 patients who suffered from a recurrent disc prolapse and have undergone an endoscopic procedure for the recurrent disc. Nine patients had been operated in our Unit, the remaining elsewhere. The age population were between 23 and 78 years old with a sex ratio of 1.5 in favor of males The treated levels were L3-L4 in 2 cases; L4-L5 in 11 cases and L5-S1 in 4 cases (Table 1) . In all cases we performed a transforaminal route access, out of one where we used an interlaminar approach because of the disc fragment location (L5-S1 level). The recurrence of the disk happened with a median time of 8 months (range 3-15 months) from the first operation. All patients had filled up an ODI (Oswestry Disability Index) and a VAS (Visual Analogue Scale) before the operation and after 3, 6 and 9 months [3-6]. The age population were between 23 and 78years old with a sex ratio of 1.5 in favor of males The treated levels were L3-L4 in 2 cases; L4-L5 in 11 cases and L5-S1 in 4 cases (Table 1).
Results
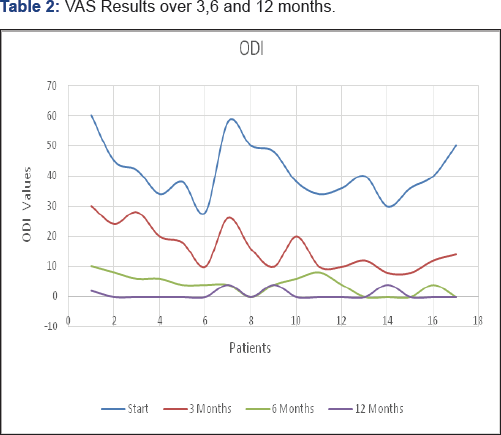
The pain improved in all cases as well as the quality of life and at a median follow up of 14 months (range 11-19 months) all the patients were pain free. Regarding the VAS values (Table 2) , from a median value of 5 (before the reoperation), it changed to a median value of 1,6 at 3 months; 1,2 at 6 months and 0,8 at 12 months (Table 2). If instead, we consider the ODI values they went from a median preoperative of 41,5% to a 16% at 3 months; 4% at 6 months and 1% at 12 months (Table 3).There were no long term complications. In the short term two patients woke up with painful paresthesie along the dermatomeric distribution of the operated nerve root. These symptoms improved within a few weeks. Two more patients had intraoperative evidence of small dural tear without any clinical signs or symptoms for postoperative CSF leakage.

Discussion
The recurrent rate of surgically treated disc prolapse, although small, is not negligible being around 6-9% [7-9] and many patients need a second operation. It is debatable regarding which approach to use: if reopen the previous scar or going paramedian in order to use a new route by muscles dilatation, like a MIS technique. However whatever route we use, once we reach the bony lamina we have to start to deal with the scar tissue formed as result of the previous operation. This can be very thick and hard to be removed and it is exactly during this phase it can happen to damage the dura or the nerve root. The main surgical concern of all surgeons, is to identify the affected nerve root as soon as possible. Generally, with the standard reoperation technique, the skin incision is a little longer as well as a bit wider the amount of bony removal in order to start the procedure from a point with normal anatomy. Then we move forward trough the scar till the nerve root and the recurrent disk's fragment are visualized. Sometime the excessive bony removal can create a situation where that segment of spine can become destabilized and it can further evolve to a clear mechanical instability with the necessity of a spinal fusion. If instead, we use a completely new route we could work in a normal anatomical situation. Further more if this route would put us directly and straightly in contact with the offended nerve root this would result in a much easier and faster procedure for the surgeon as well as for the patient with also less risk of complication. This is exactly what can be achieved, in our opinion, with the endoscopic transforaminal approach where we go from outside to inside. In this way we reach directly the interface between offended nerve root and disc prolapsed and we work below the scar tissue which very often does not need to be removed [2,3]. Also along this route it is possible to find some kind of scar tissue especially at the origin of the nerve root (shoulder) or along the nerve itself towards the foramen, but this scar is generally thinner and can be easily mobilized by dissection. On the other hand the scar tissue which develops, normally, laterally to the dural sac when we operate by a standard micro discectomy, is more abundant, adherent and difficult to be dissected apart. The philosophy we always use for disc prolapse is, if possible, to perform a transforaminal endoscopic approach for all disks located above L5/S1 [10]. Instead at this last level we prefer to use and endoscopic interlaminar approach because of the difficulty to reach the foramen in the presence of a high iliac crest (especially male patients) or in the case where the disc is pointing upwards (like in one of our case). In case of favorable anatomy (low iliac crest or with the prolapsed disc pointing downwards) a transforaminal L5-S1 route can become feasible. Naturally, when we use an interlaminar approach we do not eliminate the necessity to work through the scar, but this technique is certainly less invasive than an open procedure and requires a much less bony removal due to his better field of view. With experience it becomes easy to mobilize the scar also endoscopically by the use of specific surgical tools. Furthermore it is always possible to switch to an open procedure in case of intraoperative problems. As matter of fact in the first five cases of this series we had consented the patient for a possible conversion of the procedure from an endoscopic to an open one. Endoscopic lumbar discectomy can be performed also under epidural anesthesia [11] but we have preferred, for all seventeen cases, a general anesthesia, in the prone position without muscle relaxant in order to observe any nerve root stimulation. The length of surgery varied between 45 to 75 minutes and it was very similar to the time it takes to perform a first time lumbar endoscopic discectomy. The blood loss was negligible and all patients had been mobilized within 6 hours from the operation. We have observed also a less postoperative pain as well as a more rapid post-operative mobilization compared with the open procedure. Regarding the complication we had two cases of dura laceration without any clinical evidence or CSF leakage trough the skin incision. This is mainly due to the fact that this technique implies a muscles dilatation without cutting and so, once the working cannula is withdraw the tract automatically close up and it is very unlikely for the CSF to reach the surface. We had also a transient paresthesia along the dermatomeric distribution of the manipulated nerve root, which improved within a week.
Conclusion
The endoscopic procedure for recurrence disk prolapse is, in our opinion, a better technique when compared with the standard open microsdiscectomy or even a MIS technique. In our series it gave a good outcome with few complication and especially less postoperative pain thus also the return to normal life was faster [4]. Perhaps also the risk of iatrogenic mechanical instability might be minimized with this technique as well as the recurrent disk herniation. However our numbers are too small to give any conclusion.
References
- Hlubek RJ, Mundis GM Jr (2017) Treatment for recurrent lumbar disc herniation. Curr Rev Musculoskelet 10(4): 517-520.
- Shin KH, Chang HG, Rhee NK, Lim KS (2011) Revisional percutaneous full endoscopic disc surgery for recurrent herniation of previous open lumbar discectomy. Asian Spine J 5(1): 1-9.
- Choi KC, Kim JS, Ryu KS, Kang BU, Ahn Y, Lee SH (2013) Percutaneous endoscopic lumbar discectomy for L5-S1 disc herniation: transforaminal versus interlaminar approach. Pain Physician 16(6): 547-556.
- Leven D, Passias PG, Errico TJ, Lafage V, Bianco K, et al. (2015) Risk factors for reoperation in patients treated surgically for intervertebral disc herniation: a subanalysis of eight-year SPORT data. J Bone Joint Surg Am 97(16): 1316-1325
- Rasouli MR, Rahimi-Movaghar V, Shokraneh F, Moradi-Lakeh M, Chou R (2014) Minimally invasive discectomy versus microdiscectomy/ open discectomy for symptomaticlumbar disc herniation. Cochrane Database Syst Rev 4(9): CD010328.
- Fjeld O, Grotle M, Siewers V, Pedersen LM, Nilsen KB, et al. (2017) Prognostic factors for persistent leg-pain in patients hospitalized with acute sciatica. Spine (Phila Pa 1976) 42(5): E272-E279.
- Kim CH, Chung CK, Park CS, Choi B, Kim MJ, et al. (2013) Reoperation rate aftersurgery for lumbarherniatedintervertebral disc disease: nationwidecohortstudy. Spine (Phila Pa 1976). 38(7): 581-590.
- Malter AD, McNeney B, Loeser JD, Deyo RA (1998) 5-year reoperationratesafterdifferenttypes of lumbar spinesurgery. Spine (Phila Pa 1976). 23(7): 814-820.
- Fritzell P, Knutsson B, Sanden B, Stromqvist B, Hagg O (2015) Recurrent Versus PrimaryLumbar Disc HerniationSurgery: Patient-reported Outcomes in the Swedish Spine Register Swespine. Clin Orthop Relat Res 473(6): 1978-1984.
- Xie TH, Zeng JC, Li ZH, Wang L, Nie HF, Jiang HS, et al. (2017) Complications of lumbar disc herniation following full-endoscopicinter laminar lumbar discectomy: A large, single-center, retrospective study. Pain Physician 20(3):E379-E387.
- Albayrak S, Erol FS, Demirel I, Ayden O, Ucler N (2016) Lumbar disc surgery with epidural anesthesia: review of 700 Cases. Turk Neurosurg 26(3): 399-403.






























