Surgical Treatment of High-Grade Dysplastic Spondylolisthesis and Co-Existent Spinal Scoliosis in One Patient
Peng Li, Haoping Zhang, Kainan Zhang and Junwei Li*
Institute of Spinal Deformity, The First Affiliated Hospital of Zhengzhou University, China
Submission: December 04, 2017; Published: February 12, 2018
*Corresponding author: Junwei Li, Professor, Chief, Institute of Spinal Deformity, The first affiliated hospital of Zhengzhou University, Zhengzhou 450000, Henan province, PR China, Tel: +86-135-924 77-837; Fax: +86-0371-6697-1120; Email: lijunweizz@126.com
How to cite this article: Peng L, Haoping Z, Kainan Z, Junwei L. Surgical Treatment of High-Grade Dysplastic Spondylolisthesis and Co-Existent Spinal Scoliosis in One Patient. Open Access J Neurol Neurosurg. 2018; 7(1): 555702. DOI: 10.19080/OAJNN.2018.07.555702.
Highlights
A. Spinal scoliosis and high-grade dysplastic spondylolis thesis could be treated separately.
B. It was safe to observe the scoliosis even it progressed in short time.
C. Anatomic reduction could be achieved by enough sacral dome osteotomy and wide decompression.
Introduction
Treatment of high-grade dysplastic spondylolisthesis have been reported massively [1], while when concomitant with spinal scoliosis, it was still debated on how to treat these deformities best according to the literature. We report our experience in treatment of one case of high-grade dysplastic spondylolisthesis concomitant with spinal scoliosis.
Case Report
A girl at the age of 9 years became aware of mild low back pain, and high-grade dysplastic L5 spondylolisthesis (Meyerding grade III) was found by a local doctor. One year later in December, 2015, the girl visited our department with the complaints of significant low back pain and crouch gait. Progressed spondylolisthesis (Meyerding grade IV) and co-existent spinal scoliosis was detected by X-ray examination (Figure 1A-1D).
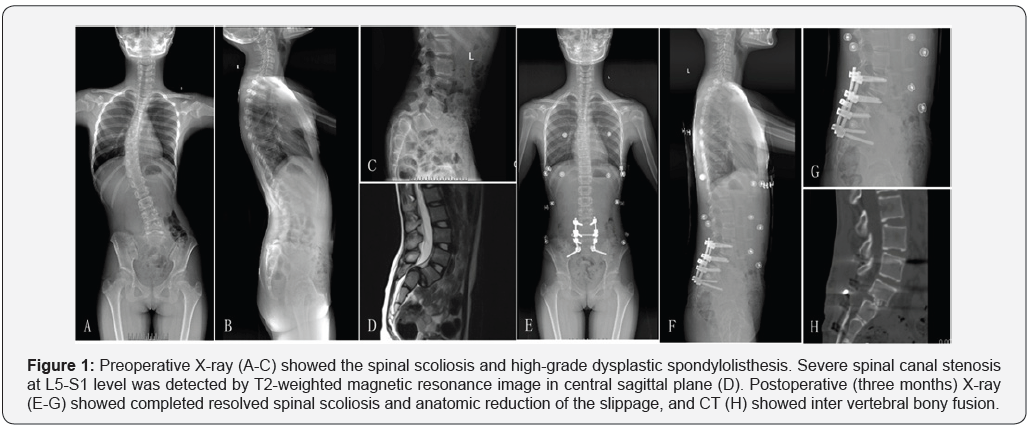
The physical findings included positive straight leg raising test at 50° on left side and 60° on right side. Both extensor and flexor hallucis longus muscle strength were grade III on left side and grade IV on right side. No bladder and rectal dysfunction were oberserved. Visual pain scale (0-10) was 7.
The radiographic parameters were analyzed based on X-ray examination and included the thoracic main curve of 44.61° in coronal plane, coronal balance of -25.28mm, sagittal balance of -10.95mm, 84.40% slippage, lumbar lordosis angle (LLA) of 81.24°, lumbosacral angle (LSA) of -41.49°, pelvic incidence (PI) of 42.51°, pelvic tilt (PT) of 30.50°, and sacral slope (SS) of 12.01°.
Considering the spinal scoliosis progressed within one year, we made the decision to treat the spondylolisthesis surgically, but observe the spinal scoliosis. The surgical technique was described as following. A longitudinal incision was made in lumbosacral region under prone position, bilateral L5/S1 facet joint were exposed laterally. In order to acquire reliable screw purchase, L4-S1 pedicle screws and S2-Alar-IIiac (S2AI) screw were used, S1 pedicle screws were inserted bicortically. After removal of lamina L5 and bilateral L5/S1 facet joint, ligamenta flava between L4/5 and L5/S1 were excised to expose dura mater. Sufficient decompression was performed from inside the spinal canal to the extraforaminal aera by excising scar tissue and osteolytic factors. Following the courses of bilateral L5 nerve roots, the nerve was found lied below the bulging part of annulus fibrosus, special care was taken to excise the bulging part to expose L5 roots, and then the L5/S1 disc was excised bilaterally between L5 and S1 roots.
The osteotomy of the sacral dome was performed bilaterally using osteotomes in an antero-medial direction. Lordosis contoured rods were fixed to the S1 and S2AI screws, and L4 and L5 screws were sequentially reduced to the fixed rod, in this process the slipped L5 was gradually reduced to the osteotomised surface of S1. Special care was taken to avoid any distraction, bilateral L5 roots were detected frequently during the process of reduction to make sure they were not stretched, further soft tissue release and shortening osteotomy using highspeed drill were also used to relieve the tension of L5 roots, correction of the lumbosacral kyphosis was verified using lateral fluoroscopy. After fully reduction was reached, the intervertebral height was measured and two cervical intervertebral spacer (polyetheretherketone cage, 12x7mm) filled with autogenous bone were installed side by side. Posterolateral fusion using autogenous bone was also performed. The tension of L5 roots was detected and no compression along the courses of L5 roots was verified before closing.
After surgery, transient weaker extensor hallucis longus muscle strength (grade II) was found in left side, which was recovered to grade IV three months later, there was no neurological deficit were found in right side. Spinal scoliosis was disappeared three months after surgery, clinical symptom and radiographic parameters were also significantly improved (Figure 1E-1H). Pain scale was improved to 1, main curve in coronal plane to 3.93°, coronal balance to -4.06mm, sagittal balance to 35.38mm, slippage to 0%, LLA to 30.65°, LSA to 3.46°, PI to 40.80°, PT to 16.91°, and SS to 23.89°. These results retained until the latest follow-up.
Discussion
It was reported that spinal scoliosis could be associated with spondylolisthesis, recent studies tend to consider these two pathologies be treated separately, except the scoliosis curve progressed over time [2]. The case we presented here had concomitant high-grade dysplastic spondylolisthesis (HGDS) and scoliosis, the scoliosis curve progressed with the spondylolisthesis in one year to more than 40°, we made the decision to surgically treat the spondylolisthesis and leave the scoliosis for observation. Interestingly, the scoliosis curve was fully resolved three months after surgery. The concrete mechanism of spinal scoliosis in this case was not fully known, but we believed that correction of lumbosacral kyphosis had positive effect on improvement of overall coronal and sagittal profile of the spine.
Surgical treatment was commonly recommended to prevent the progression of HGDS [1], while injury to L5 root in the reduction process was still a major concern [3]. It was growing consent that the priority of reduction of HGDS was restoration of lumbosacral lordosis, not complete correction of the deformity. While anatomic correction would provide the benefits of superior biomechanics and improved intervertebral bony fusion. Sacral dome resection as shortening osteotomy was recommended during reduction process, which could reduce neurological complications [4], while it was unclarified that how much osteotomy would be best. In this case, the thickness of osteotomy could be re-adjusted according to the tension of L5 roots during the reduction process, if the tension of nerve root was high, highspeed drill would be used for further osteotomy parallel to the surface. Furthermore, wide decompression of the nerve root by clear the scar or soft tissue around L5 root far lateral from the foramen would be also important to reduce neurological complications. Transient left L5 neurological dysfunction was observed in this case maybe due to the irritation of nerve root during manipulation, because the symptom recovered three months later.
The length of fusion segment, monosegment versus L4-S1, was still debated [4,5]. We believed that the number of screw insertion lied on if the surgeon felt the screw purchase was strong enough, the concrete advantage or disadvantage still need longer follow-up. In this case, sacral dome osteotomy affected the length of S1 screw, and the S2AI screws were used.
Conclusion
When concomitant with spinal scoliosis, HGDS could be treated separately, even the curve progress in short time, it was still safe to observe. Enough sacral dome osteotomy and wide decompression of the nerve root could achieve anatomic reduction and reduce neurological complications.
References
- Crawford CH, Larson AN, Gates M, Bess RS, Guillaume TJ, et al. (2017) Current Evidence Regarding the Treatment of Pediatric Lumbar Spondylolisthesis: A Report From the Scoliosis Research Society Evidence Based Medicine Committee. Spine Deform 5(5): 284-302.
- Crostelli M, Mazza O (2013) AIS and spondylolisthesis. Eur Spine J 22(Suppl 2): S172-S184.
- Smith MD, Bohlman HH (1990) Spondylolisthesis treated by a singlestage operation combining decompression with in situ posterolateral and anterior fusion. An analysis of eleven patients who had long-term follow-up. J Bone Joint Surg Am 72(3): 415-421.
- Min K, Liebscher T, Rothenfluh D (2012) Sacral dome resection and single-stage posterior reduction in the treatment of high-grade high dysplastic spondylolisthesis in adolescents and young adults. Eur Spine J 21(Suppl 6): S785-S791.
- Mizuno K, Mikami Y, Nagae M, Tonomura H, Ikeda T, et al. (2014) Instrumented reduction and monosegmental fusion for Meyerding Grade IV developmental spondylolisthesis: a report of 3 cases. Medicine (Baltimore) 93(29): e244.






























