Knee Arthrodesis: The Fate of the Contralateral Knee
Olivia J Bono*, Demetri M Economedes and James V Bono
Department of Orthopedic Surgery, New England Baptist Hospital, Boston, MA
Submission: June 01, 2018; Published: June 13, 2018
*Corresponding author: Olivia J Bono, Department of Orthopedic Surgery, New England Baptist Hospital, Boston, MA.
How to cite this article: Olivia J B, Demetri M E, James V B. Knee Arthrodesis: The Fate of the Contra Lateral Knee. Nov Tech Arthritis Bone Res. 2018; 3(1): 555604. DOI: 10.19080/NTAB.2018.03.555604
Abstract
Knee arthrodesis continues to be a common option for salvage in end-stage knee pathology. However, little is known of the morbidity within the contralateral knee and adjacent joints after undergoing this procedure. Arthrodesis is most commonly used in patients who have failed revision total knee arthroplasty secondary to sepsis. We retrospectively reviewed a consecutive series of sixteen patients who underwent knee arthrodesis for failed total knee arthroplasty, post-traumatic change, and irreparable extensor mechanism. Chart and radiograph review were conducted with an average follow-up of 7 years. Fifty-eight percent of patients followed for at least 6 months did experience contralateral knee symptoms, resulting in a 42% incidence of contralateral knee surgery following arthrodesis. Knee arthrodesis, performed as a salvage procedure, appears to enhance progression of pre-existing degenerative osteoarthritis.
Introduction
Knee arthrodesis is a common salvage solution for complications of total knee arthroplasty such as chronic infection. Septic total knee arthroplasty is the most common indication for arthrodesis [1]. Other indications include post-traumatic arthritis, ankylosis post infectious etiology such as tuberculosis or polio, neuropathic arthropathies and malignant lesions about the knee [1,2]. Currently, there are three methods of achieving knee arthrodesis [1,3]. External-fixation, initially championed by Charnley, has grown to include monoplanar, biplanar and circular frames. The latter, in using the Ilizarov method, offers the advantages of providing rigid fixation while still having the ability to adjust alignment during the fusion process and even simultaneously lengthen all during active infection [4]. Intramedullary fixation provides both long and short nail options, and its advantages include rigid fixation and early mobilization. Increased fusion rates have also been reported. The inherent advantage of compression plating, as has been described, is to provide rigid compression directly at the site of fusion without additional morbidity at distant sites [1,3]. Much has been described in terms of fusion rates and techniques [3]. However, there have been few studies that describe the outcomes and functional level of these patients. In contrast, much literature has been written with respect to long term outcome following hip arthrodesis. Several studies show the prevalence of pain in adjacent joints. Most commonly, lower back pain, ipsilateral knee and contralateral lower extremity pain demonstrate to be the most difficult symptoms the hip arthrodesis patient encounters [5,6]. The purpose of this study was to determine the effects of knee arthrodesis on the contralateral knee and to report the success of arthrodesis using intramedullary fixation.
Materials and Methods
We retrospectively reviewed a consecutive series of patients who underwent a knee arthrodesis procedure between 1994-2006. Sixteen patients were selected from the database of the senior author (JVB). There were an equal number of males and females in the cohort. The average age of the patient undergoing the procedure was 61.94 years, with the range being between 34-80 years of age. Mean follow-up was 36.5 months. Knee arthrodesis was performed in twelve patients (75%) as a salvage procedure for septic total knee arthroplasty. Eleven of these patients (91.67%) underwent knee arthrodesis after resection arthroplasty and antibiotic cement spacer placement. One patient (8.33%) had history of tibial plateau fracture treated with open reduction internal fixation and required gastrocnemius flap for skin coverage. The patient was later converted to total knee arthroplasty and tibial tubercle osteotomy was needed for exposure. The osteotomy site was found to be a primary site of osteomyelitis. Subsequent to the patient’s history and precarious skin envelope, arthrodesis was recommended. Of the remaining four patients (25%), two patients (12.5%) underwent the procedure for post-traumatic etiology, and two patients (12.5%) underwent arthrodesis for extensor mechanism disruption. One of these patients underwent revision total knee arthroplasty for infection and subsequently had extensor mechanism disruption. Another patient suffered a patellar dislocation post total knee arthroplasty. This necessitated extensor mechanism repair, which failed.
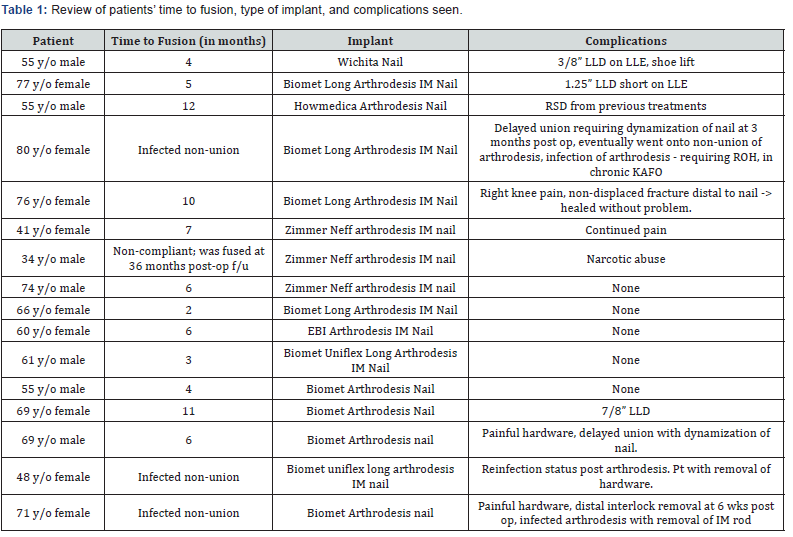
All patients underwent knee arthrodesis with intramedullary fixation. Five different prostheses were utilized for the procedure in our sixteen patient cohorts. They included the Biomet Uniflex Arthrodesis Nail, the Zimmer Neff Arthrodesis Nail, the Witchia Fusion Nail, the Howmedica Arthrodesis Nail and the EBI Arthodesis Nail (Table 1). Despite the variation of implants used, surgical technique remained consistent. Once the arthrotomy had been completed and the distal femur and proximal tibia had been debrided of any scar tissue or remaining cement spacer, both the tibial and femoral canals were sequentially reamed until isthmic fit was achieved. The component was then placed in an anterograde fashion. Proximal and distal interlocking screws were placed at the discretion of the senior surgeon. Postoperatively all patients were discharged from the hospital with instructions to remain toe-touch weight bearing on the ipsilateral lower extremity. At six weeks post-surgery, this was advanced to weight bearing as tolerated and use of assistive devices was discontinued unless there was contraindication or compromise of functional mobility. Routine follow-up was conducted at sixweeks, six months and one year post-operatively. Radiographs of the knee were obtained for evaluation of the arthrodesis. Charts were reviewed for evidence of patient complaints of back pain, contralateral knee and hip pain as well as ipsilateral hip and knee pain during their follow-up period. Time to fusion and complications were also extracted from the chart review. Radiographs were reviewed for evidence of osteoarthritis in the contralateral knee post-operatively in patients who had these films available.
Results
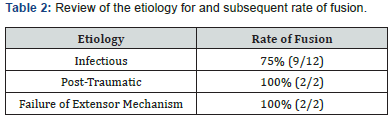
Of the sixteen patients in the cohort, fifteen complied with post-operative follow-up. Time to fusion, complications, implants used are documented in Table 1. These fifteen exhibited a fusion rate of 80%. Of these twelve successful fusions, eight (67%) were found to be radiographically fused at 6 months. The other four patients (33%) went on to delayed union, however all fused successfully within one year of the procedure. Average time to fusion of the cohort was 5.8 months. The one patient who was non-compliant with post-operative follow-up returned at 36 months, at which point was found to be radiographically and clinically fused. Table 2 documents the etiology leading to arthrodesis and the rates of fusion. Of those undergoing fusion secondaries to infectious etiology, 75% went on to fusion with the average time being 9.56 months. Twenty-five percent of the fusions performed for infection resulted in non-union and chronic osteomyelitis and underwent subsequent hardware removal. Patients undergoing knee arthrodesis secondary to post-traumatic osteoarthritis were found to have a fusion rate of 100%, although one patient did require 7 months for consolidation of the fusion. Failure of the extension mechanism leading to arthrodesis demonstrated an average fusion rate of 7.5 months. One of these patients was found to have delayed union, which later went on to fuse at 12 months.
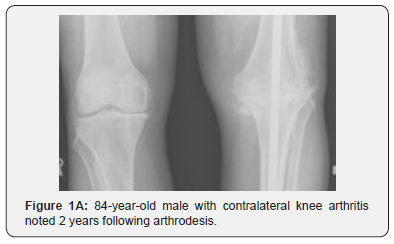
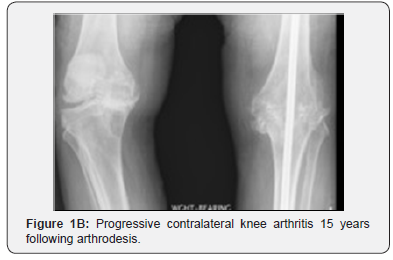
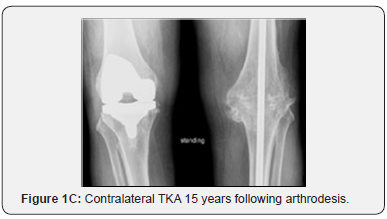
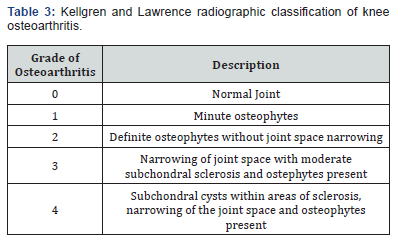
Average follow up of the study group (16 patients) was 7 years with a range from 6 months to 17 years. Four of the 16 patients had a replacement on the contralateral knee prior to arthrodesis. Of those four, one patient developed clinically significant instability in the contralateral knee replacement requiring revision total knee arthroplasty one year following arthrodesis. Twelve of the 16 patients had no prior surgery on the contralateral knee. Of these 12 patients, 8 had follow-up of 6 months or more. In this group of 8 patients with >6 months of follow up, 5 patients had preexisting DJD in the contralateral knee and 3 did not. Of the 5 patients with preexisting DJD in the contralateral knee, 4 patients went on to have surgery: 3 patients had knee replacement at 1 year, 4 years, and 15 years following arthrodesis of the contralateral knee, and one patient had arthroscopic debridement at 4 years. Of the 3 patients who did not have preexisting DJD of the contralateral knee, two patients developed pain from compensatory DJD. Clinically, contralateral knee symptoms developed in 58% (7/12) of the patients who had been followed for at least 6 months. Three of these seven patients required total knee arthroplasty (Figure 1A-1C), one required arthroscopic debridement, and one patient required revision TKA, resulting in a 42% (5/12) incidence of contralateral knee surgery following arthrodesis. Back pain was found to be present in 5 of 16 patients (31%) who underwent knee arthrodesis. All these patients experienced their back pain within 7 months of the procedure, with one complaining during the initial hospitalization for knee arthrodesis. Ipsilateral or contralateral hip pain was not present in any of the patients. Radiographs of nine of the sixteen patients were available for review. The classification of Kellgren and Lawrence, seen in Table 3, was used for radiographic analysis [7]. Two patients had total knee arthroplasty prior to fusion of the contralateral knee. One of these patients had radiographs at nine years postarthrodesis demonstrating no change of component position and minimal polyethylene wear. Three patients went on to total knee arthroplasty in the contralateral knee within 4 years of knee fusion. Two of these patients underwent arthroplasty at thirteen months post-arthrodesis, while the other waited until four years post-arthrodesis. All three demonstrated severe osteoarthritis in the contralateral knee either in pre-operative or at initial post-operative radiographs. Out of the remaining four patients who did not undergo contralateral knee arthroplasty, two demonstrated moderate osteoarthritic changes of the contralateral knee at one year and went on to severe changes by eight and fifteen years post-operatively, one demonstrated severe osteoarthritic changes of the contralateral knee at nine months post-fusion, and one demonstrated severe osteoarthritic changes of the contralateral knee on pre-operative films. Three patients demonstrated a significant leg length discrepancy measured to be 3/8”, 7/8”, and 1.25” respectively and were treated with shoe lifts. In three patients who went on to delay union, dynamization of the nail was conducted at six weeks in one patient, three months in another and five months in the last. Of these patients, one went on to radiographic and clinical signs of union, while the others went on to infected non-union.
Discussion
Total knee arthroplasty has continued to increase in prevalence over the past twenty years, with an exponential increase in primary total knee arthroplasty documented to be 166% over a 12-year period from 1990-2002 [8]. The number of revision total knee arthroplasties tripled during the same time period [8]. In 2007, Kurtz et al [9]. published an expected increase of 673% in primary total knee arthroplasties conducted in the United States by 2030 and a doubling of the total knee arthroplasty revisions by 2015. Although implants and technique have seen improvements over the same time period, there remain certain subsets of patients who require a salvage procedure such as arthrodesis to overcome the fate of failed attempts at joint reconstruction. Current indications for knee arthrodesis include septic total knee arthroplasty, post-traumatic arthritis, ankylosis post infectious etiology such as tuberculosis or polio, neuropathic arthropathies and malignant lesions about the knee [1,2]. Septic total knee arthroplasty continues to be the most common indication for arthrodesis, as was found to be the case in this study (Table 2).
Much has been previously described in terms of technique and fusion rates following knee arthrodesis [11-14]. However, few studies describe functional outcomes following the procedure. Benson et al [3] investigated this question and found that compared to a primary total knee arthroplasty-controlled cohort matched for gender and age, patients with knee arthrodesis had no difference in the following SF-36 categories: bodily pain, general health, vitality, social functioning, emotional role and mental health. They did however have significant differences in physical functioning, which is to be expected [10]. The purpose of this study was to determine the amount of contralateral knee symptomatology and pathology post knee arthrodesis. Secondarily, we attempted to determine the overall functional outcomes in these patients. This study demonstrated an overall rate of fusion in eighty percent of patients within 5.8 months of the procedure. Patients who underwent arthrodesis secondary to infectious etiology fused at a rate of seventy-five percent within about nine and a half months (9.56 months). Three patients in this subset went on to infected non-union and had all hardware removed. All patients undergoing arthrodesis for post-traumatic or extensor mechanism disruption fused successfully, although two of these exhibited a delayed union.
The data presented indicates that knee arthrodesis, performed as a salvage procedure, appears to enhance the progression of pre-existing degenerative osteoarthritis. Patients who exhibited osteoarthritis in the contralateral knee on initial post-operative radiographs progressed to severe osteoarthritis at one, four, and fifteen years post-operatively, and one patient underwent arthroscopic debridement as a temporizing measure. The data also indicates that arthrodesis enhances the onset of degenerative arthritis in the contralateral knee in two patients who did not exhibit osteoarthritis in the contralateral knee on initial post-operative radiographs. Our results suggest that contralateral knee symptoms developed in 58% (7/12) of the patients who had been followed for at least 6 months, resulting in a 42% incidence of contralateral knee surgery following arthrodesis. The primary weakness of this study is its small size and case series design. However, we feel it provides valuable insight and representation of the patient population undergoing such as procedure. We believe that a properly powered, multicenter study may yield similar results. The patient population in a salvage scenario often suffers from multiple comorbidities which compromises the ability for long term follow-up, although 5 patients had follow up > 10 years (10-17 years) Additionally, it would be beneficial for patients to undergo radiographic analysis at all follow-up intervals and extending the long-term follow-up to fifteen years.
This study demonstrates the presence pathologic advancement of degenerative osteoarthritis in the contralateral knee following arthrodesis in a select patient cohort. Arthrodesis of the knee creates adverse compensatory stresses on the contralateral knee which lead to symptoms in 58% of patients and the need for surgery in 42%.
References
- Somayaji HS, Tsaggerides P, Dowd GSE (2008) Knee arthrodesis. A review. The Knee 15: 247.
- Canale ST, Beaty JH (2008) Campbell’s Operative Orthopaedics. Mosby Elsevier, Philadelphia.
- Conway J, Mont M, Bezwada H (2004) Arthrodesis of the Knee. J Bone Joint Surg Am 86: 835.
- Spina M, Gualdrini G, Fosco M, Giunti A (2010) Knee arthrodesis with the Ilizarov external fixator as treatment for septic failure of knee arthroplasty. J Orthop Traumatol 11(2): 81.
- Schafroth MU, Blokzijl RJ, Haverkamp D, Maas M, Marti R (2010) The long-term fate of the hip arthrodesis: does it remain a valid procedure for selected cases in the 21st century? International Orthopaedics (SICOT) 34: 805.
- Beaule P, Matta J, Mast J (2002) Hip arthrodesis:current indications and techniques. J Am Acad Orthop Surg 10(4): 249.
- Kellgren J, Lawrence J (1957) Radiologic Assessment of osteoarthritis. Ann Rheum Dis 16(4): 494.
- Kurtz S, Mowat F, Ong K, Chan N, Lau E, et al. (2005) Prevalence of Primary and Revision Total Hip and Knee Arthroplasty in the United States from 1990 to 2002. J Bone Joint Surg Am 87(7): 1487-1497.
- Kurtz S, Ong K, Lau E, Mowat F, Halpern M (2007) Projections of Primary and Revision Hip and Knee Arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am 89(4): 780.
- Benson E, Resine S, Lewis CG (1998) Functional Outcome of Arthrodesis for Failed Total Knee Arthroplasty. Orthopedics 21: 875.
- Talmo C, Bono J, Figgie M, Sculco T, Laskin R, et al. (2007) Intramedullary Arthrodesis of the Knee in the Treatment of Sepsis After TKR. HSS Journal 3(1): 83-88.
- Bono J, Talmo C, Windsor R (2009) Arthrodesis of the Knee: Indication and Treatment Options, Techniques in Knee Surgery 8(4): 212-215.
- Bono J, Sherman P, Windsor R, Laskin R, Sculco T, et al. (2009) Intramedullary Arthrodesis after Failed Septic Total Knee Arthroplasty. Techniques in Knee Surgery 8(4): 216-224.
- Wellman S, Bono J (2009) Knee Fusion with External Fixation. Techniques in Knee Surgery 8(4): 235-238.






























