A Study of Peripheral Blood Smear in Ne
Paramanantham PA1 and Maharaja P2
1Professor in NICU, SRM medical college hospital and research centre, India
2Research Scholar in Microbiology, SRM medical college hospital and research centre, India
Submission: March 09, 2018; Published: March 28, 2018
*Corresponding author: Paramanantham PA, Professor in NICU, SRM medical college hospital and research centre, Katankulathur, India,Email: paramanandham59@yahoo.com
How to cite this article: Paramanantham P, Maharaja P. A Study of Peripheral Blood Smear in Neonates. Mod Appl Bioequiv Availab. 2018; 3(4): 555618. DOI: 10.19080/MABB.2018.03.555618
Abstract
Objective: To study the variations in RBC, WBC, platelets, haemoglobin and nRBC in peripheral smear of neonates and to correlate with clinical findings.
Design: Prospective Descriptive Study
Methods: A total of 60 neonates was prospectively studied from june 2015 to august 2016. 1ml venous blood will be collected from new borns EDTA tubes. Peripheral smear will be studied according to standard operating procedure with a special emphasis on RBC, WBC, platelets, haemoglobin and nRBC counts the presents of band forms and toxic granules the peripheral smear will help diagnose septicemia. A performa containing the details of the patient and informed consent from the parents of the patient and institutional ethical committee clearance obtained for the present study.
Results: Mean weight varies from 1.2 to 3.9kgs with a mean of 2.80kg with SD 0.596 with a ratio of male 31 and female 29. Haemoglobin values varies from 6.1 to 22.8 with a mean of 15.25 and SD of 3.245. RBC values varies from 3.5 to 6.4 with mean and SD value of 4.615 and 0.645. WBC value varies from 6000 to 41300 with mean and SD value of 14383.3 and 6271.02. Platelet value varies from 3000 to 405000 with mean and SD value of 180353.33 and 88106.97. nRBC value varies from 0 to 120 with mean of 10.67 and SD value of 22.05.
Conclusion: nRBCs more than 10 per 100 WBCs is indicative of perinatal hypoxyia in neonates
Keywords: Peripheral smear; Neonatal nRBCs; Thrombocytopenia
Introduction
Peripheral blood smear examination provides information that cannot be obtained from automated cell counting. Hematological values in neonates differ significantly from those in older children and adults. Quantitative and qualitative differences are present as a reflection of the developmental changes during fetal hematopoiesis and so, correlate with gestational age. At birth, the hemoglobin, mean corpuscular volume, and WBC counts of term newborns are significantly higher than those of older children and adults and in preterm neonates the differences are even more pronounced. This review explores these differences and the major factors that account for them from the hematology laboratory standpoint. Early diagnosis of neonatal septicemia is a vexing problem because of its non specific clinical picture. Bacterial infection in the newborn still account for a considerable morbidity and mortality. This is because the newborn especially the premature are prone to serious infections by organisms and partly because the signs of these infections may be absent or minimal and hard to detect.Thus fatal septicemia may occur with little warning. Hence the timely diagnosis of sepsis in neonates is critical as the illness can be rapidly progressive and in some instances fatal.
A peripheral blood smear is a glass microscope slide coated on one side with a thin layer of venous blood. The slide is stained with Leishman's, and examined under a microscope. Microscopic examination of the peripheral blood is used to supplement the information provided by automated cell counter. However precise classification of abnormal cells requires a trained hematologist, a well-made peripheral blood smear, and a light microscope with good optical characteristics. This study was carried out with the objective of to study the variations in RBC, WBC, platelets, toxic granules in peripheral smear of neonates and to correlate with the clinical findings.
Materials & Methods
a) Place of Study: NICU, SRM Medical College Hospital & RC, Kattankulathur.
b) Duration of Study: June 15- September 16.
c) Study Design: Prospective Descriptive Study
d) Total No. of Cases: 60. All were Term neonates.
e) Inclusion criteria: All term neonates
f) Exclusion criteria: preterm neonates & those born with any congenital abnmomalies.
Procedure
Blood for examination is obtained by venepuncture and collected in EDTA vacutainers. Ethylene di amine tetra acetic acid (EDTA) is the anticoagulant preferred. The blood from the patient with EDTA tubes is Subjected to Sysmex-I Auto Analyser for automated cell counting. Blood smear was stained with Leishmann Stain due to easy feasibility and the staining methods done according to standard procedure.
The datas of newborn/s age, sex, mode of delivery, weight, APGAR score were entered in a separate proforma. The appropriate test were done according to the need like serum bilirubin, APGAR score, CRP, blood culture and glucose monitoring were done. The datas were analysed by descriptive analysis. The asphyxial neonates were staged for HIE by Sarnat [1,2].
Result
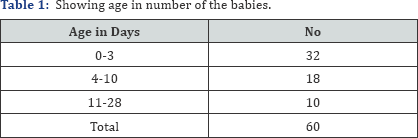
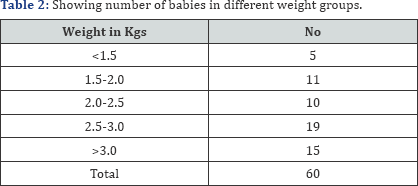
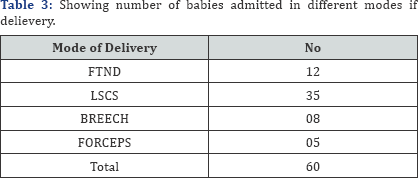
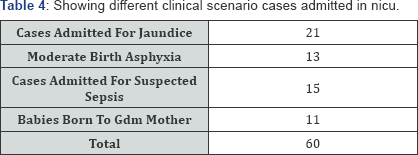
(Table 1-4) Total number of neonates studied were 60. All were term babies. Age of neonate varies from day 1 to day 28. Birth weight varies from 1.2 to 3.9kgs with a mean of 2.80kg with SD 0.596. 19 babies weighing from 2.5-3kgs. 32 babies were within 3 days of age. 35 babies were delivered by elective cesarian section. Out of 21 babies admitted for jaundice, 5 babies required phototherapy and the other babies bilirubin level below phototherapeutic range. Put of 13 babies born with moderate asphyxia. The asphyxial babies were staged for HIE 1. Only 1 baby had HIE-I stage (hyperalertness). Out of 15 suspected sepsis babies were done CRP. CRP and blood culture were negative in all suspected cases of sepsis. Only one baby showed toxic granules in peripheral blood smear. 11 born to gdm mothers were regularly glycemia was noted by glucometer reading till 72 hours of life. All results were normal. Neutophilic leucocytosis were indicative of sepsis. wbcs ranges from 600041300 with mean of sd 14383.3 and 6271.02. out of 13 babies delivered had moderate asphyixia which showed nrbc values from 0-120 with mean of 10.67 and sd of 22.05. in our study, all 13 asphyixial neonates showed nrbc more than 10 per 100 WBCs. The platelet count was more than 400000. The blood smear report were normal except for neutrophilic leukocytosis in 7 babies and 3 babies showed lymphocytic preponderance. All babies were discharged and advised to come for follow up for immunization and evaluation of increase in birth weight with occurence of infection.
Discussion
NRBCs are primarily produced in the fetal bone marrow in response to erythropoietin and are stored in the marrow as reticulocytes and mature erythrocytes. They are normally seen in the blood of neonates Ghosh [3]. as seen in non asphyxiated neonates below 10 nrbcs in our case. The levels of NRBCS per 100 white blood cells correlate with acute as well antepartum asphyxia and early neonatal outcome [4] Count of NRBCs per 100 WBCs is a simple marker for presence and assessment of severity of asphyxia as it is an early outcome and has a direct correlation with increased stress and infection [5]. as seen in 13 moderate asphyxiated neonates showed more than 10 nRBCs per 100wbcs in our case.
NRBC count is also a useful tool for prediction of brain damage and the expected course in hypoxic induced encephalopathy patients. Although NRBCS rarely circulate in older children, they are commonly seen in blood of neonates. In normal newborns less than 10 NRBC/100 WBC is within normal limit [6] Nucleated red blood cells are commonly seen in the blood of neonates. Wbc was seen 41,300. Any persistent increase in wbcs more than 2 5000 apart from sepsis to be evaluated for congenital leukemia, but the repeat wbc count showed decrease in 10 to less than 15,000 Risk factors like arrest of labour, prolonged rupture of membranes, eclampsia, prolonged labour and non- cephalic presentation are the important significant risk factors for perinatal asphyxia7 Clinically birth asphyxia presents as fetal distress, FHS>100/m or <160/m. Presence of meconium stained liquor and APGAR score will be less than 5 in these cases [7]. But APGAR score in 13 neonates were between 4 and 7 in our study.
Considering the fetal bone marrow response to hypoxia in utero, the elevated n-RBC/100 WBC count as the marker for not only perinatal asphyxia but also indicate developing Neurological sequalae [8,9] The number of NRBC/100 WBC is variable but is rarely greater than 10 in normal neonates [10-12] Early thrombocytopenia in Term/Preterm should prompt evaluation of sepsis, congenital viral infection or DIC Chaitanya [13] Presence of toxic granules and Howell Jolly bodies in the case of infection and should be proved by CRP and blood culture.
Microscopic exzmination of peripheral blood is used to supplement information provided by automated cell counters. Examination of peripheral smear is an inexpensive but powerful diagnostic tool in children and adults. It provides rapid, reliable access to information about a variety of hematological disorders. However the precise classification of abnormal cells requires a trained hematologist, a well made peripheral smear and a light microscope with good optical characteristics.
Conclusion
THE NRBCs count can be easily done in laboratory, which is commonly neglected by the clinicians. These NRBC count parameter can serve as simple and cost effective test in early diagnosis of perinatal asphyxia.
It will guide clinicians in instituting early treatment and adopting aggressive treatment whenever applicable, thus reducing the neonatal mortality and morbidity.
References
- Sarnat HB, Sarnat MS (1976) Neonatal encephalopathy following fetal distress. A clinical and electroencephalographic study. Arch Neurol 33(10): 696-705.
- Apgar V (1953) A proposal for a new method of evaluation of the newborn infant. Curr Res Anesth Analg 32(4): 260-267.
- Ghosh B, Mittal S, Kumar S, Dadhwal V (2003) Prediction of perinatal asphyxia with nucleated red blood cells in cord blood of newborns. Int J Gynaecol Obstet 81(3): 267-271.
- Boskabadi H, Maamouri G, Sadeghian MH, Ghayour-Mobarhan M, Heidarzade M, et al. (2010) Early diagnosis of perinatal asphyxia by nucleated red blood cell count: a case-control study. Arch Iran Med 13(4): 275-281.
- Phelan JP, Ahn MO, Korst LM, Martin GI (1995) Nucleated red blood cells: A marker for fetal asphyxia. Am J Obstetrics Gynecol 173(5): 1380-1384.
- Hermansen MC (2001) Nucleated red blood cells in the fetus and newborn. Arch Dis Child Fetal Neonatal Ed 84(3): F211-F215.
- Rehana M, Yasmeen M, Farrukh M, Shaikh NP, Rajar UD, et al. (2007) Risk factors of birth asphyxia. J Ayub Med Coll Abbottabad 19(3): 6771.
- O'Brien JR, Usher Rh, Manghan GB (1966) Causes of birth asphyxia and trauma. Journal of Canadian Medical Association 94(21): 1077-1086.
- Tungalag L, Gerelmaa Z (2014) Nucleated Red blood cell counts in asphyxiated newborns. Open Science Journal of Clinical Medicine 2(1): 33-38.
- Phelan JP, Ahn MO, Korst LM, Martin GI (1995) Nucleated red blood cells: a marker for fetal asphyxia? Am J Obstet Gynecol 173(5): 13801384.
- Philip AG, Tito AM (1989) Increased nucleated red blood cell counts in small for gestational age infants with very low birth weight. Am J Dis Child 143(2): 164-169.
- Mccarthy JM, Capullari T, Thompson Z, Zhu Y, Spellacy WN, et al. (2006) Umbilical cord nucleated red blood cell counts: normal values and the effect of labor. J Perinatol 26(2): 89-92.
- Chaitanya, Cravida, Mathew S, Sola-Visner M (2013) In Neonatal Thrombocytopenia. In: Cloherty JP [Ed.], In: (7th edn), In Manual of Neonatal Care, p. 578.






























