Medication Assessment and Pharmacy Intervention Guideline to Reduce Fall Risk on Medical Floors at a Community Hospital in the USA
Alaa Abdullah Alhubaishi*
Department of Pharmacy Practice, Princess Nora University, Saudi Arabia
Submission: March 05, 2018; Published: March 12, 2018
*Corresponding author: Alaa Abdullah Alhubaishi, Department of Pharmacy Practice, Princess Nora University, Riyadh Airport Road, Narjes Neighborhood, Former Pharmacy Practice Resident, Hallmark Health System (HHS) Inc Medford, MA, USA, Email: aaalhubaishi@pnu.edu.sa
How to cite this article: Alaa Abdullah A. Medication Assessment and Pharmacy Intervention Guideline to Reduce Fall Risk on Medical Floors at a Community Hospital in the USA. Mod Appl Bioequiv Availab. 2018; 3(3): 555611. DOI: 10.19080/MABB.2018.03.555611
Abstract
Background: Falls in hospitalized patients have received a lot of attention in recent years. A fall may result in an injury that can add to overall healthcare costs. Evidence exists about the specific medication classes that increase patient's risk of falling. However, the common fall assessment tools used in most hospitals do not factor in patient's medications as a variable. The purpose of this study is to identify high risk patients by utilizing a medication fall risk assessment tool and to make recommendations to mitigate falls.
Method: This was a prospective chart review study. The control group included any patients who scored ≥6 points according to medication fall risk assessment tool (N=685). While the experimental group included any patients who scored ≥6 points according to medication assessment tool and had a pharmacy intervention (N=71). If a patient score ≥6 points (high risk) then, a pharmacist would intervene using the developed medication algorithms for safer alternative.
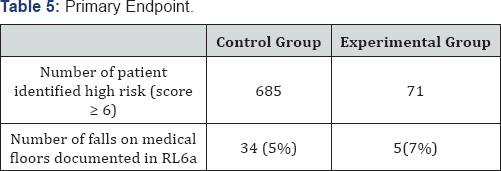
Results: The primary end point occurred in 34 patients out of 685(5%) in pre implementation group verses 5 patients out of 71(7%) in postimplementation. The primary end point was not statistically significant at p < 0.05.
Conclusion: This study may provide an effective tool based on medications for mitigating falls although the results were inconclusive. Preventing falls in hospitals should be a combined effort including physicians, pharmacist, and nurses.
Keywords: Pharmacy; Medications; Falls; Intervention; Morse fall scale
Abbreviations: HHS: Hallmark Health System; MFS: Morse Fall Scale; ADR: Adverse Drug Reaction; RL6: Comprehensive Event Reporting System; MWH: Melrose Wakefield Hospital; LMH: Lawrence Memorial Hospital
Introduction
Falls in hospitalized patients have received a lot of attention in recent years. A fall may result in an injury that can add to overall healthcare costs. Fall injuries are one of the most expensive medical conditions. In Saudi Arabia, researches continue to recommend reducing fall's incidence among health care institutions by recognizing patient's risk factors [1]. Many identified risk factors contribute to falls on medical floors; these may include age, female gender, chronic diseases, falls history, vision or mobility impairment, alcohol and multiple medication use [2]. Evidence exists about the specific medication classes that increase patient's risk of falling. There is an increase awareness of the impact of some medications on increasing the risk of falls, therefore the guideline for prevention of falls in older persons (American geriatrics society, American academy of orthopedic surgeons panel on falls prevention) states that "patients who have fallen should have their medications reviewed and altered or stopped, as appropriate, in light of their risk of future falls " Although falls are often multifactorial, the risk of falls can be reduced by addressing any underlining factors that are modifiable [3]. The exact number of falls caused by medication is not known because falls are not officially recognized in the adverse drug reaction (ADR) reporting. However, modification of a patient's medication regimen is one possible method of reducing the risk of falls on medical floors. A number of fall assessment tools are readily available to identify adults with fall risk factors [4]. At Hallmark Health System (HHS), a two community hospital system, the fall assessment tool used by nurses is Morse Fall Scale (MFS). The Morse Fall Scale is a rapid and simple method of assessing a patient's likelihood of falling which consists of six variables (Table 1). A score of 0-24 is interrupted as low risk, a score of 25-44 is moderate risk and a score of 45 or higher is high risk. Each level of risk had a list of precautions in order to reduce the risk of falling.
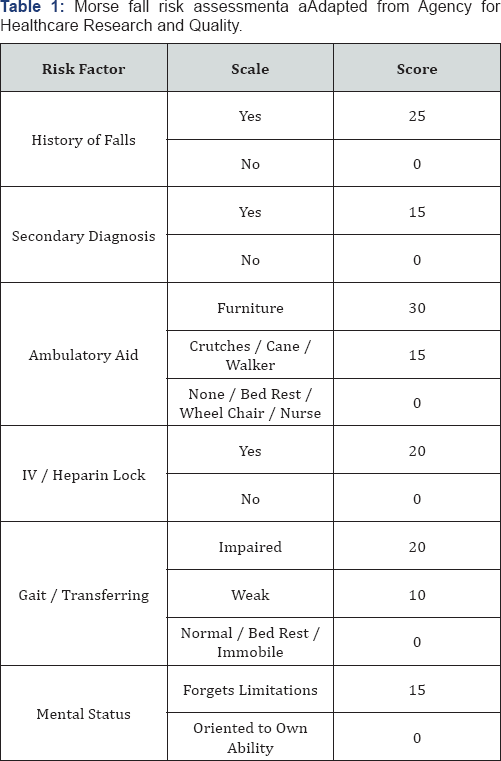
The MFS is used widely in acute care settings, both in the hospital and long term care inpatient settings. In developing countries such as Riyadh region, Saudi Arabia MFS is not common practice yet. MFS does not factor in medications that the patient is on as a variable in determining the total score. The purpose of this research is to reduce the rate of falls by identifying the patients who are at high risk to fall based on their medication administration profile during their hospital stay. Besides using MFS to assess patient's likelihood of falling, pharmacy was supporting by screening and recognizing high risk patients using a different assessment tool known as
Medication fall risk score [3]. This tool is developed for pharmacist to identify medication-related risk factors for falls in hospitalized patients. This tool was published in Agency for Healthcare Research and Quality with the permission of Beasley B, Patatanian E (Table 2).
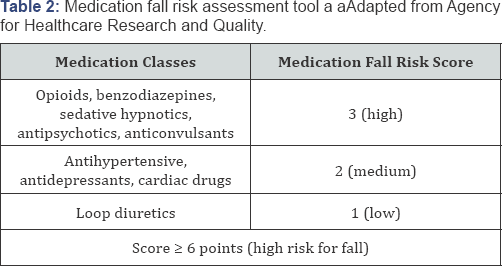
Methods
Study design
This study was approved by the Institutional Review Board and the Pharmacy and Therapeutics Committee at HHS. The study was conducted within two location centers, a 340-bed community hospital-based health system located north of Boston (Melrose-Wakefield Hospital and Lawrence Memorial Hospital). This was a prospective chart review study. The historical control group included patients who scored ≥6 according to medication fall risk assessment tool for the period of 60 days pre- implementation (September 1st to October 31st 2016) while the experimental group included patients who scored ≥6 and had a pharmacy intervention around falls in the period of 60 days post- implementation ( February 15th to April 15th 2017).
Study population
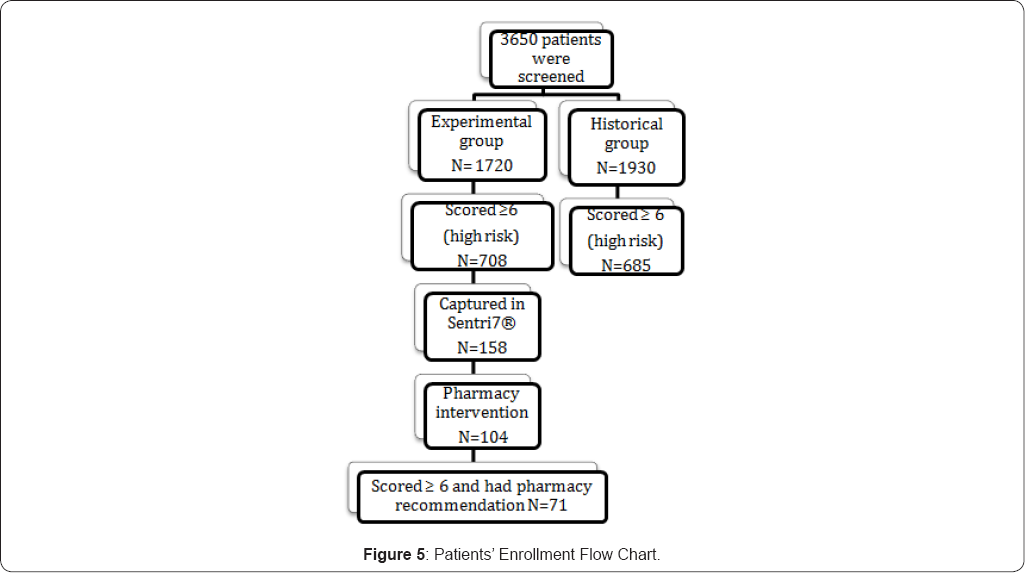
Using pharmacy electronic software system, a search was conducted to collect any patient on any medication listed in the medication fall risk assessment tool. A total of 3650 patients were screened (1930 patients in control group vs 1720 patients in experimental group) Eligible patients in historical control group were patients on medical floors of HHS who were identified as high risk to fall that scored ≥6 on the medication fall risk assessment tool (N=685 patients). The experimental group included patients scored ≥6 and had a pharmacy intervention (N=71). Patient demographics is listed in (Table 3). Emergency department, labor and delivery, and maternity patient or patients that scored < 6 were excluded from this study
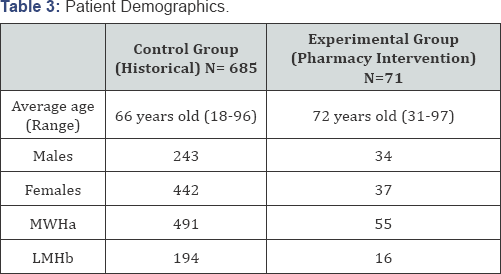
aMWH: Melrose -Wakefield Hospital
bLMH: Lawrence Memorial Hospital
Intervention
aRL6: comprehensive, easy-to-use event reporting system
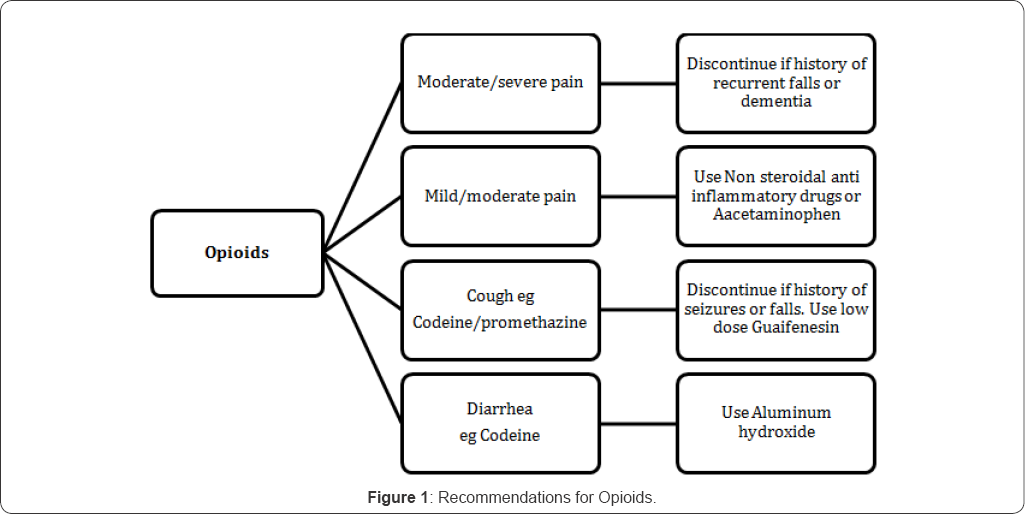
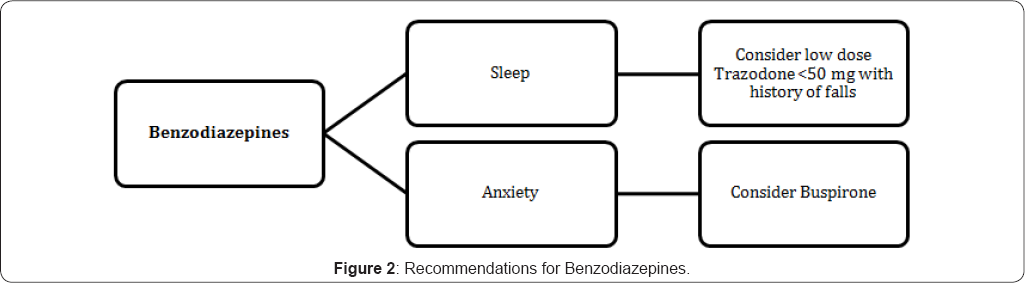
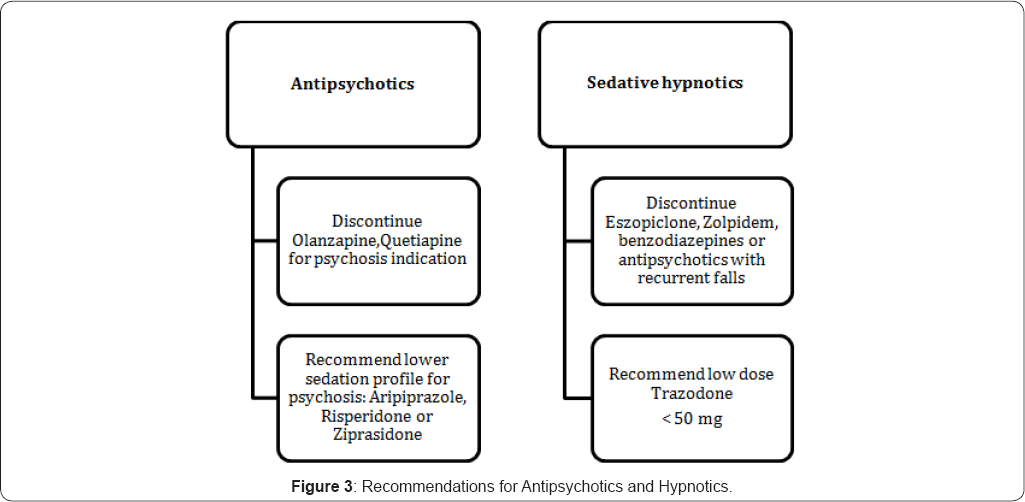
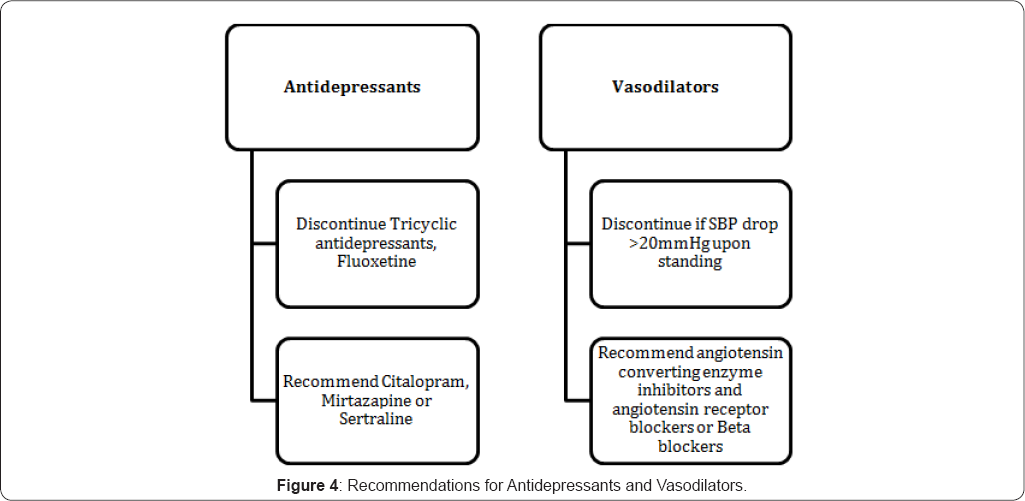
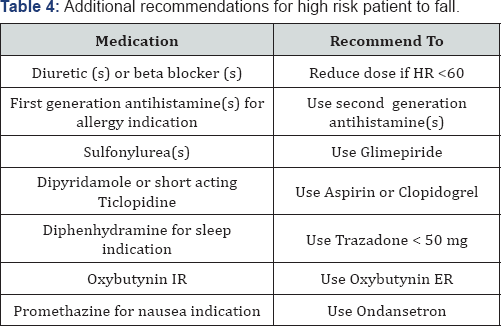
The literature was reviewed to develop a list of high- risk medications that have been associated with falls. The medication algorithms were developed in an effort to guide pharmacist recommendations on safer alternatives. The bases for development of algorithms were clinical literature. There were six developed algorithms for specific medication classes which are associated with increased risk of falls. These include: opioids, benzodiazepine, antipsychotics, sedatives hypnotics, antidepressants, and vasodilators. (Figure 1-4) and additional recommendations for high risk patients (Table 4 & 5). The detailed pharmacy intervention guide was available as a policy for the pharmacy staff. The pharmacy pharmaco- surveillance software (Sentri7®) was set up to capture any patient on at least one medication from the medication classes listed in the medication fall risk assessment tool (Table 2). Once the patient was captured in sentri7®, the pharmacist would calculate a score by adding up the points for every medication identified in the medication fall risk assessment tool. If the patient was taking more than one medication in a particular risk category, the score was calculated by (risk level score) x (number of medications in that risk level category) [3]. Patient(s) was at high risk to falls when they scored ≥6. Due to lack of literature data, not all the high risk medication classes mentioned in the medication fall risk assessment tool had a developed algorithm [5-7]. When patient (s) score>6, pharmacist will contact the physician for appropriate recommendations based on the medication algorithms.
The general goal was to identify high risk patients and provide a safer alternative medication or apply more fall precautions. In fact, pharmacist were not only screening medications but also evaluating other factors in order to make an appropriate recommendation such as patient's age, vital signs, history of falls, etc. For example if the physician did not accept recommendations for patient's safety such as patient cannot tolerate new medications or health condition is not stable, then pharmacist contacted patient's nurse to upgrade MFS precautions risk to the next risk category [8].
Endpoints
The primary endpoint was the number of falls on medical floors. The secondary endpoint was the average number of pharmacy recommendations per patient. These categorical variable endpoints were evaluated using Chi-Square test at the level of significance α= 0.05.
Results
The primary end point occurred in 34 of 685 patients (5%) in control group verses 5 of 71 patients (7%) in the experimental group (Table 5). The primary end point was not statistically significant at p<0.05. The average number of pharmacy interventions was 0.97 with a total of 69 recommendations for the 71 patients identified as high risk (97%). Recommendations vary between upgrading MFS precautions, recommending safer alternative per developed algorithms, or no changes due to unstable health condition.
Discussion
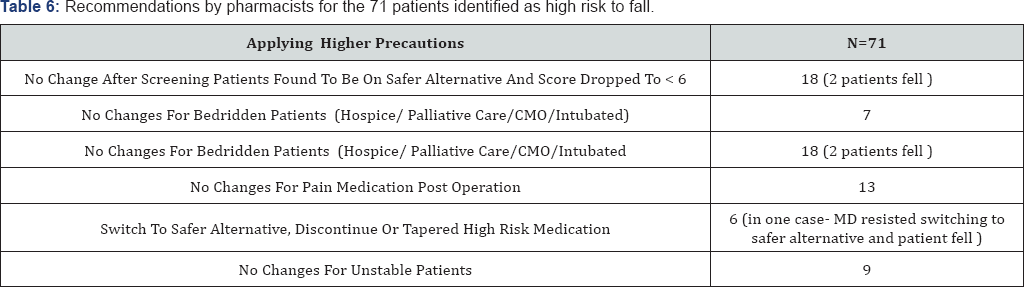
The medication fall risk assessment tool and the pharmacy guideline to reduce risk of falls on medical floor policy was implemented for 60 days. Sentri7® captured 158 patients during that time period and the pharmacist screened 104 patients only (Figure 5). This was one of the challenges that faced this intervention. Pharmacy staff shortages and time related issue limited the number of patients that were included in this period. 71 patients out of 104 scored ≥6 (qualified as high risk). Of those patients, there were 5 patients which fell despite the pharmacist recommendations. Two patients fell after placing higher precautions by nurses and two other patients fell in which the pharmacist did not recommend any changes to their medications given the fact that they were bedridden, while one patient fell after physician rejected a change to one of the high risk medications (Table 6). These interventions were performed by certified pharmacists, pharmacy residents, and pharmacy interns.
Conclusion
This study is the first of a kind conducted in a community hospital setting to the best of author's knowledge. Other studies around preventing falls by screening medications are done in a different health setting. There was no significant difference in the rate of falls pre and post implementation of the medication fall risk assessment tool and guideline policy. For future studies, preventing falls should be a combined effort including physicians, pharmacist and nurses. In some measure, our study suffers from considerable limitations such as physician resistant to switch to a safer alternative, and lack of education to nurses therefore; there was no documentation in nurse's note about pharmacy recommendation to apply higher precautions. Overall, pharmacists found this policy challenging to fit in their present of other clinical interventions assigned due to staffing challenges. The study needed ~ 2000 patients in each group to achieve 80% power which might have been achieved if the study period were to be extended. We can conclude that screening medications and identifying patients as high risk in a hospital setting was hard to implement. Although, similar kind of intervention was applied in different health setting, with favorable outcome of the role of pharmacist in screening patient's medications and recommending safer alternatives. For future direction, implementing MFS with medication fall risk assessment tool as a combination to assess patient's risk of fall on medical floors might result in better outcome.
Acknowledgment
I would like to acknowledge the following people for providing invaluable support: Nicole Clark, Pharm D, MHA, BCPS; Ruchit Marfatia, Pharm D, MSCR, BCPS, BCCCP.
References
- (2012) The Prediction of Falls Among older people in Saudi Arabia. Journal of American Science 8(6): 692-700.
- (2016) The Centers for Disease Control and Prevention. Important Facts about Falls, USA.
- Beasley B, Patatanian E (2009) Development and Implementation of a Pharmacy Fall Prevention Program. Hospital Pharmacy 44(12): 10951102.
- Rojas-Fernandez CH, Seymour N, Brown SG (2014) Helping pharmacists to reduce fall risk in long-term care: a clinical tool to facilitate the medication review process. Can Pharm J (Ott) 147(3): 171-178.
- Jong DMR, Elst VDM, Hartholt KA (2013) Drug-related falls in older patients: implicated drugs, consequences, and possible prevention strategies. Ther Adv Drug Saf 4(4): 147-154.
- Bulat T, Castle SC, Rutledge M, Quigley P (2008) Clinical practice algorithms: Medication management to reduce fall risk in the elderly- Part 3, benzodiazepines, cardiovascular agents, and antidepressants. J Am Acad Nurse Pract 20(2): 55-62.
- (2016) NHS Cumbria Stopp start toolkit supporting medication review.
- DiPiro JT, Talbert RL, Yee GC, Matzke GR, Wells BG, et al. (2014) Pharmacotherapy: A Pathophysiologic Approach, 9e. Access pharmacy, USA.






























