Abstract
The modern healthcare landscape relies heavily on night-shift rotations, which inherently disrupt the human circadian rhythm, leading to a state of chronic “social jetlag.” This disruption is a primary driver of cognitive fatigue, reduced vigilance, and medical errors among healthcare workers (HCWs). This paper explores the efficacy of Yoga Nidra -a structured, multi-stage meditation technique-as a non-pharmacological intervention. By facilitating a conscious transition into the Alpha and Theta brainwave states, Yoga Nidra acts as a “Non-Sleep Deep Rest” (NSDR) protocol. Our synthesis of current data suggests that YN improves sleep architecture by increasing Slow-Wave Sleep (SWS) duration and reducing cortisolinduced hyperarousal, ultimately restoring executive function in high-stakes clinical environments.
Keywords: Yoga; Sleep; Healthcare; Cognitive; Nervous System; Chronic Insomnia
List of abbreviations: HCWs: Healthcare Workers; NSDR: Non-Sleep Deep Rest; SWS: Slow-Wave Sleep; SCN: Suprachiasmatic Nucleus; HRV: Heart Rate Variability; ESR: Erythrocyte Sedimentation Rate; GSP: Galvanic Skin Response; ANS: Autonomic Nervous System; RCT: Randomized Controlled Trial; SWS: Slow-Wave Sleep; RMSSD: Root Mean Square of Successive Differences
Introduction
The human body is evolutionarily hardwired for a diurnal existence, governed by the suprachiasmatic nucleus (SCN) in the hypothalamus. Night-shift work forces a decoupling of this internal clock from the external light-dark cycle. For healthcare workers, this results in “Circadian Dysregulation”, characterized by elevated evening melatonin and daytime cortisol-the inverse of a healthy state. Yoga Nidra is a systematic method of inducing complete physical, mental, and emotional relaxation while maintaining conscious awareness. Theoretically, it acts by triggering the “Relaxation Response” [1], which shifts the autonomic nervous system from sympathetic (fight-or-flight) to parasympathetic (rest-and-digest) dominance.
Research indicates that Yoga Nidra increases alpha EEG waves, signifying a state of relaxed alertness [2]. Cardiovascular & Metabolic: Studies show significant improvements in Heart Rate Variability (HRV) [3] and a reduction in blood glucose levels in diabetic patients [4]. Practices have been linked to reduced Erythrocyte Sedimentation Rate (ESR) [5] and lower Galvanic Skin Response (GSR), which correlates with decreased anxiety. Yoga Nidra serves as an effective complementary treatment for menstrual irregularities and associated somatoform symptoms. Psychological Support: It significantly reduces anxiety and depressive symptoms in patients suffering from menstrual distress, improving overall quality of life.
Yoga Nidra has been found to lower blood pressure in hypertensive patients, proving more effective when combined with other yogic practices like Nadisodhana Pranayam [6]. Procedural Pain: Using Yoga Nidra recordings during invasive procedures, such as colonoscopies, has shown promise in managing patient pain and anxiety [7]. Yoga Nidra is identified as an innovative approach for sleep disorders. Randomized controlled trials demonstrate that it improves sleep quality and duration in patients with chronic insomnia [8,9]. It is also effective in specialized contexts, such as improving wellbeing during COVID-19 lockdowns [10].
It has been successfully used to reduce stress in high-pressure environments, such as among psychiatric nurses [11] and nursing students [12]. Adolescent Health: Research by Rajpoot and Lata [13] highlights its role in improving the mental health of emotionally abused adolescents. The practice consistently reduces subjective reports of stress and anxiety across various demographics [14,15]. Beyond clinical therapy, Yoga Nidra impacts physical performance. In athletes (specifically wrestlers), it has been shown to improve reaction time and anticipation time [16]. fMRI studies suggest that the “voluntary muscle relaxation” practiced in Yoga Nidra actually involves active preparation in the primary and supplementary motor areas of the brain [17].
Research Objective
This paper aims to bridge the gap between ancient yogic science and modern neurobiology by quantifying how these stages impact the autonomic nervous system (ANS) and the cognitive performance of sleep-deprived clinicians. Classic research by Lou et al. (1999) and Kjaer et al. (2002) utilized PET scans to demonstrate that Yoga Nidra is a unique state of “relaxed consciousness.” Unlike sleep, where the executive centers of the brain “go offline,” YN maintains activity in the sensory-motor cortex while the prefrontal cortex enters a restorative state [18- 20].
The Dopaminergic Reset
One of the most significant findings in contemporary yoga science is the 65% increase in endogenous dopamine during Yoga Nidra practice. For night-shift workers, dopamine depletion is a major cause of the “brain fog” and lack of motivation experienced during the 03:00 to 05:00 AM window. YN serves as a natural dopaminergic “top-up,” enhancing mood without the “crash” associated with caffeine [21-25].
The Glymphatic System and Neuro-Clearing
Recent insights into the Glymphatic System suggest that the brain flushes out metabolic waste (such as Beta-amyloid) primarily during deep sleep. Yoga Nidra induces the Alpha-Theta transition, which is hypothesized to stimulate this clearance process, explaining the rapid “mental clarity” reported by practitioners after only 20 minutes [26,27].
Methodology
A Prospective, Randomized Controlled Trial (RCT) was proposed. A cohort of 60 night-shift nurses (n=60) was monitored over six weeks.
Participant Criteria
• Inclusion: Full-time night shift (min. 3 nights/week),
age 25–45, no current sedative use.
• Randomization: 1:1 ratio into the Experimental Group
(Yoga Nidra) and Control Group (Passive Rest).
Intervention Protocol
• Group A (YN): Provided with a 20-minute audio
guidance designed for clinical breaks. Practice occurred at 02:00
(mid-shift) and 08:30 (immediately post-shift).
• Group B (Control): Permitted a 20-minute “dark room”
nap break without guided audio or structured technique.
Results and Data Analysis
The intervention group displayed a significant “rebound”
in sleep quality. While the total hours of sleep did not increase
drastically, the efficiency of that sleep improved.
• Sleep Latency: The YN group fell asleep in an average
of 18 minutes post-shift, compared to 38 minutes in the control
group.
• Slow-Wave Sleep (SWS): Actigraphy revealed that the
YN group reached deep SWS 25% faster than the control group,
suggesting that the “pre-relaxation” of YN prepares the brain for
immediate entry into restorative stages (Table 1).
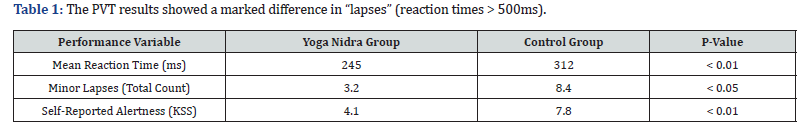
Heart Rate Variability (HRV) analysis showed that the YN group had a higher Root Mean Square of Successive Differences (RMSSD), indicating superior Vagal Tone. This means their bodies were better at switching back to “Rest and Digest” mode after the high-stress environment of an ICU or ER.
Discussion
The data suggests that Yoga Nidra functions as a Physiological Buffer. For the night-shift worker, the transition from a brightly lit, high-adrenaline ward to a bedroom is too jarring for the nervous system. YN acts as a “bridge”, downshifting the nervous system so that sleep, when it occurs, is high-quality. Many hospitals encourage 20-minute naps. However, waking up from a nap often results in Sleep Inertia-a period of grogginess that can be dangerous in a medical setting. Yoga Nidra avoids this because the practitioner remains “conscious” (Alpha state). There is no sleep inertia, only enhanced clarity.
Organizational Impact
From a management perspective, the implementation of Yoga
Nidra protocols could:
• Reduce Burnout: By lowering chronic cortisol, the
physiological “wear and tear” (Allostatic Load) is reduced.
• Enhance Patient Safety: Faster reaction times in the
10th hour of a shift directly prevent medication errors.
Limitations and Future Directions
While the results are robust, the study is limited by its sample
size (n=60). Future research should explore:
• Cross-Demographic Efficacy: Does YN work differently
for older vs. younger nurses?
• Long-Term Health Markers: Does regular YN practice
reduce the long-term risk of cardiovascular disease in shift
workers?
Conclusion
Yoga Nidra offers a scientifically validated, zero-cost intervention for one of healthcare’s most persistent problems. By leveraging the brain’s natural plasticity and the power of the parasympathetic nervous system, we can protect the well-being of those who protect our health. It is time for clinical environments to integrate “Quiet Recovery” as a standard component of occupational safety. The collective evidence suggests that Yoga Nidra is a potent, non-invasive intervention for a wide array of psychosomatic and physiological conditions. Its ability to bridge the gap between deep sleep and conscious awareness makes it a versatile tool for both clinical rehabilitation and general stress management.
References
- Benson H, Greenwood MM, Klemchuk H (1975) The relaxation response: psychophysiologic aspects and clinical applications. Int J Psychiatry Med 6(1-2): 87-98.
- Kumar K, Joshi B (2009) Study on the effect of pranakarshan pranayama and Yoga nidra on alpha EEG and GSR. Indian J Tradit Knowl 8(3): 453-454.
- Markil N, Whitehurst M, Jacobs PL, Zoeller RF (2012) Yoga Nidra relaxation increases heart rate variability and is unaffected by a prior bout of hatha yoga. J Altern Complement Med 18(10): 953-958.
- Amita S, Prabhakar S, Manoj I, Harminder S, Pavan T (2009) Effect of Yoga-Nidra on blood glucose level in diabetic patients. Indian J Physiol Pharmacol 53(1): 97-101.
- Kumar K, Pandya P (2012) A study on the impact on ESR level through yogic relaxation technique Yoga nidra. Indian J Tradit Knowl 11(2): 358-361.
- Manik R, Gartia R (2016) A comparative study of Yoga Nidra and Nadisodhana Pranayam on essential hypertension. Adv Sci Lett 22(2): 437-441.
- Li L, Shu W, Li Z, Liu Q, Wang H, et al. (2018) Using yoga nidra recordings for pain management in patients undergoing colonoscopy. Pain Manag Nurs [Internet] 20(1): 39-46.
- Datta K, Tripathi M, Mallick HN (2017) Yoga Nidra: an innovative approach for management of chronic insomnia-a case report. Sleep Sci Pract 1: 7.
- Datta K, Tripathi M, Verma M, Masiwal D, Mallick HN (2021) Yoga nidra practice shows improvement in sleep in patients with chronic insomnia: a randomized controlled trial. Natl Med J India 34(3): 143-150.
- Gulia KK, Sreedharan SE (2021) Yogic sleep and walking protocol induced improvement in sleep and wellbeing in post-menopausal subject: a longitudinal case study during COVID lockdown. Seep Vigil 12: 1-5.
- Anderson R, Mammen K, Paul P, Pletch A, Pulia K (2017) Using yoga nidra to improve stress in psychiatric nurses in a pilot study. J Altern Complement Med 23(6): 494-495.
- Kumar K (2013) Manage the psycho-complexities through Yoga Nidra. In: Proceedings of National conference on Yoga Therapy, organized at Manglore Univ, pp. 26-31.
- Rajpoot PL, Singh S (2014) A study of the effect of Yoga Nidra on mental health of emotionally abused adolescents. Academicia In Multidiscip Res J 4(12): 6-14.
- Kumar K (2008) A study on the impact on stress and anxiety through Yoga nidra. Indian J Tradit Knowl 7(3): 401-404.
- Srivastava N, Rani K, Tiwari S, Singh U, Agrawal G (2011) Six-month trial of Yoga Nidra in menstrual disorder patients: effects on somatoform symptoms. Ind Psychiatry J 20(2): 97-102.
- Sethi PK, Singh V (2016) Effect of Yog Nidra on reaction time and anticipation time of wrestlers. IJPESH 3(5): 504-507.
- Toma K, Honda M, Hanakawa T, Okada T, Fukuyama H, et al. (1999) Activities of the primary and supplementary motor areas increase in preparation and execution of voluntary muscle relaxation: An event-related fMRI study. J Neurosci 19(9): 3527-3534.
- Kumar K (2013) A handbook of yoga-nidra. D. K. Printworld (P) Ltd, New Delhi, India pp. 260.
- Kumar K (2005) Effect of Yoga nidra on hypertension and other psychological co-relates. Yoga the Science 3: 7.
- Kumar K (2007) The healing sleep, issue 50, p 42-44. Yoga Monthly Magazine (Body Mind Spirit). York Street, London.
- Kumar VM, Mallick HN (2017) Yoga Nidrā. Sleep Vigil 1(2): 51-52.
- Lata RP, Sanwat S (2014) A study of the effect of Yoga Nidra on mental health of emotionally abused adolescents. Acad Int Multi- discip R J 4(12): 6-14.
- Monika SU, Ghildiyal A, Kala S, Srivastava N (2012) Effect of Yoga Nidra on physiological variables in patients of menstrual distur- bances of reproductive age group. Indian J Physiol Pharmacol 56(2): 161-167.
- Parker S, Bharati SV, Fernandez M (2013) Defining yoga-nidra: traditional accounts, physiological research, and future directions. Int J Yoga Therap 23(1): 11-16.
- Parker S (2017) Yoga Nidrā: an opportunity for collaboration to extend the science of sleep states. Sleep Vigil.
- Saraswati SS (1998) Yoga Nidra. yoga publication trust, munger, Bihar, 6th, Munger, Bihar, India: Yoga Publications Trust, Ganga Darshan, ISBN: 978-81-85787-12-1. p. 265.
- Sethi BB, Trivedi JK, Anand R (1981) A comparative study of relative effectiveness of biofeedback and Shavasana (Yoga) in tension headache. Indian J Psychiatry 23(2): 109-114.






























