Neuromuscular Electrical Stimulation and Spinal Segmental Stabilization in Individuals with Non-Specific Low Back Pain- Randomized Clinical Trial
Fernanda da Silva Tori, Alberito Rodrigo de Carvalho, Carlos Eduardo Albuquerque, Gabriela Taborda and Gladson Ricardo Flor Bertolini1*
Gladson Ricardo Flor Bertolini, Universitaria St, Brazil
Submission: May 04, 2021; Published: June 11, 2021
*Corresponding author: Gladson Ricardo Flor Bertolini, Universitaria St. 2069, Cascavel, Paraná, Brazil
How to cite this article: Tori F S, Carvalho A R, Albuquerque C E, Taborda G, Bertolini G R F. Neuromuscular Electrical Stimulation and Spinal Segmental Stabilization in Individuals with Non-Specific Low Back Pain- Randomized Clinical Trial. J Yoga & Physio. 2021; 8(5): 555749. DOI:10.19080/JYP.2021.08.555749
Abstract
The objective of this study was to verify the results of neuromuscular electrical stimulation (NMES) associated with central stabilization exercises in individuals with chronic nonspecific low back pain, taking as parameters the pain and trophism of the multifidus muscle. Methods: 40 volunteers were recruited and distributed in the placebo group, electrostimulation, stabilization exercise and therapeutic association. Pain was analyzed by visual analogue scale and McGill’s questionnaire, and trophism was analyzed by ultrasound images. The therapeutic protocol consisted of three therapies per week over 4 weeks, independent of the group, with pre-protocol and end-of-protocol evaluations. Results: Significant differences were observed in pain quantification with reduction for the group that performed stabilization exercises, however, there were no differences for trophism. Conclusion: It is concluded that the use of stabilization exercises produced good results for the reduction of pain in individuals with chronic nonspecific low back pain.
Keywords: Low back pain; Muscle strength; Exercise therapy; Electric stimulation therapy
Introduction
Low back pain (LBP) is a musculoskeletal dysfunction, multifactorial and high incidence [1]. The lifetime incidence is estimated to be around 84% [2], and given this magnitude, it is possible to compare the costs of LBP with cardiovascular disease, depression, and diabetes, in addition to resulting in disability and absence from work [3]. LBP causes functional disability that can go on for years of life [4]. Besides affecting physical aspects, it also affects psychological and emotional factors, resulting in personal and social losses, with a reduction in the individual’s quality of life [5]. Among the types of LBP, the nonspecific type stands out, which is characterized precisely by not being attributed a known cause, representing from 90 to 95% of cases [4] Musculoskeletal disorders of the lumbar spine are an important public health problem, with the need for intervention strategies to control this morbidity [6]. Conservative treatments have shown to be effective in recovery aspects, besides having a lower cost when compared to invasive treatments [7].
LBP has shown a high relationship with changes in muscle strength [8,9]. The impairment of muscle function can come from fatigue, due to excessive overload generated in the intervertebral discs, capsules, and ligaments, causing deformities of these, and leading to pain [10]. Specifically, atrophy of the multifidus is related to nonspecific LBP, and exercise therapy aimed at strengthening this muscle group is fundamental for clinical treatment [11].
Exercise therapy is recommended by European guidelines as the first line of treatment, in addition to potentially a faster recovery and generating less disability [12]. Spinal segmental stabilization exercises focus on strengthening the core muscles, that is, internal and external obliques, transverse abdominals, multifidus, erector spinae, and rectus abdominals, which control the lumbar pelvic complex [13]. They are intended to provide neuromuscular control to obtain lumbar stabilization, from the nervous and muscular systems, generating protection for the spine from the improvement in the activation pattern of the trunk muscles, thus reducing pain and disability [14].
In addition to therapeutic exercises, there are electrotherapeutic resources that can help increase muscle strength, such as neuromuscular electrical stimulation (NMES), which aims to produce muscle contraction from the stimulation of motor neurons. In clinical practice, it is accompanied by the main objective of strengthening weakened muscles, besides the recovery and preservation of function in case of immobility or reduced activity [15]. However, studies evaluating its use in conjunction with kinesiotherapy in cases of low back pain are still needed. Thus, the present study aimed to verify the results of NMES associated with central stabilization exercises in individuals with chronic nonspecific LBP, using pain and trophism as parameters.
Methods
This is a cross-sectional, descriptive, quantitative, doubleblind study. Each group was composed of 10 individuals, totaling 40 participants. The research was carried out at the Physical Rehabilitation Center (CRF) of the Universidad Estadual do Oeste do Paraná, after approval by the Research Ethics Committee of Univest (no. 2.748.221).The sample was randomized (https:// www.graphpad.com/quickcalcs/randomize1/) into four groups, being the control group (CG) that received no intervention; NMES group (NMES); isometric exercises of the core muscle group associated with the placebo NMES (Exer); FES group associated with isometric exercises of the core muscles (NMES+Exer). This sample size was calculated by the program G*Power 3.1.9.7, with an effect size of 0.3, α=0.05, 95% power, 4 groups, 2 measurements.
The research participants were volunteers who reported nonspecific low back pain [15] for at least 3 months, aged between 18 and 30 years, who signed the informed consent form. The exclusion criteria were pregnant women, LBP due to a diagnosis that did not fit as nonspecific, trauma, neoplasms, inflammatory diseases, surgical procedures on the spine, cardiac pacemaker, altered sensitivity, or any other contraindication related to the use of electrostimulation.
The individuals answered an anamnesis and quantified the intensity of pain by means of the Visual Analog Scale (VAS), in which the patient quantifies from 0 to 10 the pain score, being 0 no pain, 1 to 3 mild pain, 4 to 7 moderate pain and 8 to 10 severe pain [16,17]. Pain characteristics were assessed by McGill’s scale that qualitatively and quantitatively detects items grouped into four groups (sensory, affective, evaluative and miscellaneous) and 20 subcategories, the higher the score, the more intense is the [18]. Transverse section of the multifidus muscle was analyzed bilaterally with an ultrasonic transducer (Shimadzu SDU 450 xl, Columbia, USA), 7.5MHz linear B-mode, positioned laterally to the spinous process of L3, water-soluble gel was used for better visualization. During the measurement, the patient was positioned in the ventral decubitus and the upper limbs arranged beside the body, feet outside the stretcher, at each end of expiration the image was collected, so as not to influence the images collected [19] Assessment occurred before the start of the therapeutic protocol (EV1) and after 4 weeks of intervention (EV2).
For the NMES group, the intervention was performed with the Neurodyn device (Ibramed), with a frequency of 50Hz, phase duration of 300μs, the cycle was composed of up and down times of 1s, on 8s, and off 10s, during 10minutes per therapy, over 4 weeks, 3 procedures per week were performed, with intervals. The electrodes used were made of silicone rubber (2x4cm), positioned on the paravertebral region (bilateral) from L1 to L5, with 2cm lateral distance to the spinous process. The intensity of the current was increased until a muscle contraction felt on palpation was produced.
The isometric exercises consisted of a plank on the ground in a prone position. Abdominal exercises in the dorsal decubitus with the Swiss ball situated in the lumbar region, performing the movement of trunk flexion with the upper limbs extended. In prone position with the Swiss ball in the abdominal region, the participant lifted the lower and upper limbs, alternating them. Bridge in dorsal decubitus with the Swiss ball in the foot region, performing hip extension. The participants had to keep for 10seconds in 3 sets of 8 repetitions.
Data were analyzed in SPSS 20.0 program, using the test for generalized mixed models and LSD post-test, the accepted significance level was 5%. Effect size was also assessed by Hedges’ h, based on the first assessment for a given group, and classified as: <0.2: trivial; 0.2-0.5: small; 0.5-0.8: moderate; >0.8: large (https://www.estimationstats.com/#/).
Results
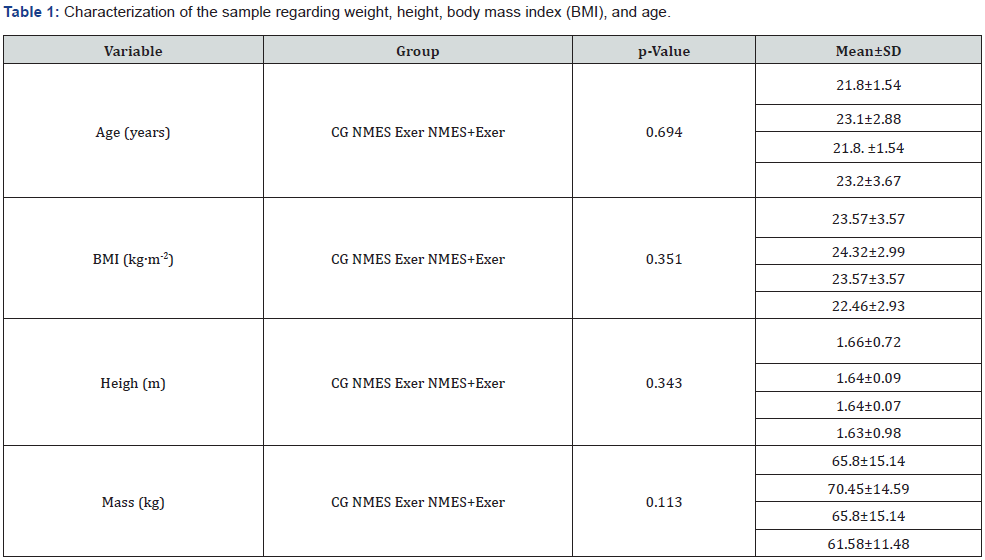
The sample presented homogeneous characteristics regarding anthropometric aspects (Table 1). For pain intensity assessed by the VAS scale, there were significant differences when comparing groups (p<0.001), evaluations (p<0.001) and interaction of factors (p=0.002). In EV1 there were no differences between groups, but for EV2, CG was significantly higher than NMES, Exer and NMES+Exer (p<0.001); still NMES was higher than NMES+Exer (p=0.039). In intra-group comparisons, only CG had no difference between EV1 and EV2 (p=0.576), with a 42% reduction for NMES (p=0.001), 58% for Exer (p<0.001), and 66% for NMES+Exer (p<0.001). For the effect sizes, only CG showed values considered small, for the other groups they were considered large (Table 2).
For the McGill pain questionnaire, there were again differences between groups (p<0.001), evaluations (p<0.001), and interaction of factors (p=0.044). For EV1, there were no differences between groups, but for EV2, CG showed higher scores than NMES (p=0.017), Exer (p<0.001) and NMES+Exer (p<0.001); NMES also showed higher values than NMES+Exer (p=0.012). In the intragroup comparison, CG and NMES showed no significant differences (p=0.711 and p=0.056, respectively), whereas Exer showed a 56% reduction (p=0.009) and NMES+Exer a 76% reduction (p=0.001). Effect sizes were trivial for CG, moderate for NMES, and large for the other two groups (Table 2). For the thickness of the multifidus, there was a difference between groups (p=0.005), with GFES+EX showing higher values than the other groups (CG - p=0.023; GFES - p=0.003; GEX - p=0.001). There was also a difference between evaluations, with an increase in trophism in AV2 (p=0.029); but there was no interaction of the factors (p=0.064). Effect sizes were trivial for GC and NMES, small for NMES+Exer and large for Exer (Table 2).

Discussion
In this study, segmental spinal stabilization trainings associated with functional electrical stimulation were performed, aiming at reducing chronic nonspecific LBP, and it was observed that the main factor that led to the reduction of pain in patients was the use of active exercises that strengthen the stabilizing muscles.
The stability of the lumbar spine is given in osteoligamentous structures and trunk muscles. The movements performed during activities of daily living generate loads on these structures of the spine, which, if unprotected, becomes vulnerable and generate pain. To provide adequate stability to the spine and avoid overload injuries, it is necessary in order to contract the stabilizing muscles [1].
The deep muscles of the trunk present alterations in individuals with LBP, especially the transverse abdominous and multífidus. The contraction occurs in a slow and delayed manner, with deficiency in the activation time and muscular atrophy, which leads to muscular inhibition and replacement by fat, causing the muscle to lose its stabilizing function. For this reason, stabilization exercises that improve strength, endurance, and neuromuscular control generate a reduction in chronic LBP [20]. The intensity of pain was evaluated by VAS, with a lower score in the final evaluation when compared to the initial evaluation in the groups that performed spinal segmental stabilization, when compared to the CG, which corroborates the results of other studies that also used central stabilization, demonstrating that central stabilization exercises reduce pain in individuals with chronic LBP [12,21-23]quality of life and functional capacity”,”type”:”article-journal”,”volume”:”17”},”uri s”:[“http://www.mendeley.com/documents/?uuid=a18db685- 2d51-4d75-bbd1-43b3cfc637fe”,”http://www.mendeley. c o m / d o c u m e n t s / ? u u i d = 6 7 e 0 b 2 b 1 - 3 9 d 1 - 4 1 6 9 - b d c 8 - 4cfa1d032f34”]},{“id”:”ITEM-2”,”itemData”:{“DOI”:”10.1017/CB O9781107415324.004”,”ISBN”:”9788578110796”,”ISSN”:”1098- 6596”,”PMID”:”25246403”,”abstract”:”Predicting the binding mode of flexible polypeptides to proteins is an important task that falls outside the domain of applicability of most small molecule and protein−protein docking tools. Here, we test the small molecule flexible ligand docking program Glide on a set of 19 non- α-helical peptides and systematically improve pose prediction accuracy by enhancing Glide sampling for flexible polypeptides. In addition, scoring of the poses was improved by post-processing with physics-based implicit solvent MM- GBSA calculations. Using the best RMSD among the top 10 scoring poses as a metric, the success rate (RMSD ≤ 2.0 Å for the interface backbone atoms.
The use of spinal segmental stabilization is an option with evidence for the reduction of nonspecific LBP, and to quantify the level of analgesia, scales such as VAS and McGill’s questionnaire can be used, which aims to verify the quality of pain. In the present study there was a significant difference in relation to McGill. The groups that performed vertebral segmental stabilization presented a lower final score when compared to the control group and the NMES group [23,24]”type”:”article-journal”,”volume”:”27”},”ur is”:[“http://www.mendeley.com/documents/?uuid=7cb6f3ef- 9c6f-4dba-9526-8437a01cece5”,”http://www.mendeley. c o m / d o c u m e n t s / ? u u i d = 0 0 9 7 c d d 5 - d 4 5 c - 4 d f c - 8 2 4 0 - 4be89c746746”]},{“id”:”ITEM-2”,”itemData”:{“ISSN”:”1981- 6855”,”abstract”:”pain, such as in the improvement of functional capacity. This improvement follows the principles of neuromuscular training of deep muscles of the lumbar spine, increasing vertebral stability. A dor lombar ou lombalgia é considerada um problema de saúde pública, sendo responsável por um grande número de pessoas que sofrem afastamento do trabalho e realizam consultas médicas, considerada também a principal causa de procura por atendimento fisioterapêutico em todo mundo. Segundo a IASP (Associação Internacional de Estudo da Dor. The McGill scale consist of four subgroups, which are sensory, affective, evaluative and miscellaneous. Within each subgroup there are descriptors that are synonyms among themselves, others that seem synonymous, but vary in intensity or may still have minimal but important differences for the people who are trying to classify pain [25].
Individuals with non-specific LBP generally present atrophy of the multifidus muscles, and it is possible to evaluate the crosssection by means of diagnostic ultrasound equipment, considered of excellent reliability to measure these muscles [11]. The present study performed the measurement at the level of L3 in the initial and final evaluations of the participants. A significant difference was observed in the final evaluation with cross-sectional gain, and the group that performed exercises associated with NMES presented higher values than the other three groups, however, there was no interaction of factors, and for this group the effect size was moderate. Only the group that performed exercises associated with the placebo NMES showed a large effect size, small for the association group and for the other two groups it was considered trivial. In the present study, the use of NMES did not contribute to the increase of trophism, since in the final evaluation there was no significant difference, i.e., only the isometric exercise was important for this to occur. A possible explanation for the fact that electrical stimulation did not fulfill its role of helping to strengthen the muscles may have been the fact that the frequency used did not produce tetanic stimulation of the multífidus [26], however according to Baek et al. [27]50, and 80 Hz. Ultrasound images of the LM, TrA, OI, and obliquus externus (OE such frequency can also be used for these muscles.
The results of this study should be analyzed keeping in mind limitations, such as: the period of 4 weeks may have been insufficient to obtain advantages for electrostimulation, as well as the intensity used in electrostimulation could have been more intense, there were no follow-up measures to evaluate the longterm effects.
Conclusion
We conclude that isometric exercise aimed at strengthening the stabilizing muscles of the lumbar spine reduces chronic nonspecific low back pain, but functional electrical stimulation was not an adjuvant factor.
References
- Silveira AP de B, Nagel LZ, Pereira DD, Morita ÂK, Spinoso DH, et al. (2018) Efeito imediato de uma sessão de treinamento do método Pilates sobre o padrão de cocontração dos músculos estabilizadores do tronco em indivíduos com e sem dor lombar crônica inespecífica. Fisioter e Pesqui 25(2): 173-181.
- Hildebrandt J, Ursin H, Mannion A, Airaksinen O, Brox JI, et al. (2006) Chapter 4: European guidelines for the management of chronic nonspecific low back pain. Eur Spine J Suppl 2(Suppl 2): S192-300.
- Nabavi N, Bandpei MAM, Mosallanezhad Z, Rahgoza M, Jaberzadeh S (2018) The effect of 2 different exercise programs on pain intensity and muscle dimensions in patients with chronic low back pain : a randomized controlled trial. J Manipulative Physiol Ther 41(2): 102-110.
- Butts R, Dunning J, Pavkovich R, Mettille J, Mourad F (2017) Conservative management of temporomandibular dysfunction: A literature review with implications for clinical practice guidelines (Narrative review part 2). J Bodyw Mov Ther 21(3): 541-548.
- Nascimento JM, Stefane T, Napoleão AA, Hortense P (2015) Alternative therapeutic methods for disability management in chronic low back pain. Rev Min Enferm 19(1): 195-203.
- Antunes RS, Macedo BG, Amaral T da S, Gomes H de A, Pereira LSM, et al. (2013) Dor, cinesiofobia e qualidade de Vida em pacientes com lombalgia crônica e depressã Acta Ortopédica Bras 21(1): 27-9.
- Anandani G, Shetty GM, Bafna S, Narula N, Gandhi A (2015) Effectiveness of device-based therapy for conservative management of low back pain. J Phys Ther Sci 27(7): 2139-2141.
- da Silva RA, Vieira ER, Cabrera M, Altimari LR, Aguiar AF, et al. (2015 ) Back muscle fatigue of younger and older adults with and without chronic low back pain using two protocols: A case-control study. J Electromyogr Kinesiol 25(6):928-936.
- Gondhalekar GA, Kumar SP, Eapen C, Mahale A (2016) Reliability and validity of standing back extension test for detecting motor control impairment in subjects with low back pain. J Clin Diagnostic Res JCDR 10(1): KC07-11.
- Abboud J, Nougarou F, Descarreaux M (2016) Muscle activity adaptations to spinal tissue creep in the presence of muscle fatigue. PLoS One 11(2): 1-14.
- Goubert D, Van Oosterwijck J, Meeus M, Danneels L (2016) Structural changes of lumbar muscles in non-specific low back pain. Pain Physician 19(7): E985-E1000.
- Akhtar MW, Karimi H, Gillani SA (2017) Effectiveness of core stabilization exercises and routine exercise therapy in the management of pain in chronic nonspecific low back pain: A randomized controlled clinical trial. Pakistan J Med Sci 33(4): 1002-1006.
- Zheng Y, Ke S, Lin C, Li X, Liu C, et al. (2019) Effect of core stability training monitored by rehabilitative ultrasound image and surface electromyogram in local core muscles of healthy people. Pain Res Manag
- Chung S, Lee J, Yoon J (2013) Effects of stabilization exercise using a ball on mutifidus cross-sectional area in patients with chronic low back pain. J Sport Sci Med 12(3):533-541.
- Bohórquez IJR, Souza MN de, Pino AV (2013) Influência de parâmetros da estimulação elétrica funcional na contração concêntrica do quadríceps. Rev Bras Eng Biomédica 29(2):153-65.
- Boonstra AM, Schiphorst HR, Reneman MF, Posthumus JB, Stewart RE (2008) Reliability and validity of the visual analogue scale for disability in patients with chronic musculoskeletal pain. J Rehabil Res 31(2): 165-169.
- Barbosa IM, Sales DS, Oliveira LM de S, Sampaio DV, Milhome AG (2016) Pain in onco-hematologic patients and its association with analgesia. Rev Dor 17(3): 178-182.
- França FR, Burke TN, Hanada ES, Marques AP (2010) Segmental stabilization and muscular strengthening in chronic low back pain - a comparative study. Clin Sci 65(10): 1013-1017.
- Teyhen DS, Rieger JL, Westrick RB, Miller AC, Molloy JM, et al. (2008) Changes in deep abdominal muscle thickness during common trunk-strengthening exercises using ultrasound imaging. J Orthop Sport Phys Ther 38(10): 596-605.
- Volpato CP, Fernandes SW, Carvalho NAA, Freitas DG (2012) Exercícios de estabilização segmentar lombar na lombalgia: revisão sisemática da literatura / The effectiveness of lumbar segmental stabilizing exercises in low back pain: a systematic review. Arq Med Hosp Fac Cienc Med St Casa São Paulo. 57(1): 35-40.
- Arins MR, Murara N, Bottamedi X, Ramos J dos S, Woellner SS, et al. (2016) Physiotherapeutic treatment schedule for chronic low back pain: influence on pain, quality of life and functional capacity. Rev Dor 17(3): 192-196.
- Kobill AF de M, Silveira AL de A, Lima AI, Paidosz A, Siqueira AF, et al. (2017) Influência da estabilização segmentar core na dor e funcionalidade da coluna lombar. Fisioter Bras 8(2): 148-153.
- Ferreira JN dos S, Oliveira AS (2015) Estabilização segmentar vertebral em pacientes com lombalgia crônica: revisão da literatura. Corpus Sci 11(2): 24-32.
- Chang WD, Lin HY, Lai PT (2015) Core strength training for patients with chronic low back pain. J Phys Ther Sci 27(3): 619-622.
- Pimenta CA, Teixeiro MJ (1996) Questionário de dor McGill: proposta de adaptação para a língua Portuguesa. Rev da Esc Enferm da USP 30(3): 473-483.
- Gonçalves M, Silva Barbosa FS (2005) Analysis of strength and resistance parameters of the lumbar spinae erector muscles during isometric exercise at different effort levels. Rev Bras Med do Esporte 11(2): 109-114.
- Baek SO, Ahn SH, Jones R, Cho HK, Jung GS, et al. (2014) Activations of deep lumbar stabilizing muscles by transcutaneous neuromuscular electrical stimulation of lumbar paraspinal regions. Ann Rehabil Med 38(4): 506-513.






























