An Aggravation of Type II Diabetes Mellitus with Relapse of Lower Respiratory Tract Infection: A Case Study
Likhita Kolli*
M.A.M. College of Pharmacy, Kesanupalli, Narasaraopet, Guntur district, Andhra Pradesh, India
Submission: September 14, 2017; Published: September 19, 2017
*Corresponding author: Likhita kolli, M.A.M. College of Pharmacy, Kesanupalli, Narasaraopet, Guntur district, Andhra Pradesh, India,Tel: 8106094879; Email: likhitakolli.pharmd@gmail.com
How to cite this article: Likhita K. An Aggravation of Type Ii Diabetes Mellitus with Relapse of Lower Respiratory Tract Infection: A Case Study. J of Pharmacol & Clin Res. 2017; 3(5): 555621. DOI: 10.19080/JPCR.2017.03.555621
Abstract
Diabetes mellitus is a metabolic disorder characterized by insulin resistance. Lower respiratory tract infections (LRTIs) have become a common problem for Indians to visit general practitioner. It is a clearly known fact that attack of infections in Diabetic patients is common due to deprivation of immune system and altered inflammatory responses. Hence patients with diabetes have an elevated risk of developing lower respiratory tract infections (LRTIs). However, until now, clinicians have not had the tools to assess individual risks. Studies and observations showing a high risk of infections in diabetics exist as this topic is still being debated upon. Abnormal lung function and glucose intolerance, insulin resistance, type 2 diabetes have been proposed to be interrelated. The present case study includes a 66yr old woman who is a known case of Type II DM with hypertension. The patient had developed pneumonia 6 months ago which was suspected to be a complication of diabetes. Upon treatment it was subsided. At present she had a relapse of LRTI which is still not finally diagnosed. In addition, her ECG was found to be abnormal. The point of interest is that her fasting blood levels were elevated after a respiratory attack. This study is being reported to state that diabetes alone doesn't develop infections but relapse of pulmonary infections due to its improper management could lead to elevation of diabetic risks and complications. This study has raised a point that improper treatment of LRTI could lead to diabetic complications even under proper glycemic management and further development of cardiovascular problems will be supported. Clinicians and dialectologists must focus that elevation of previous infections or incidence of new infections would increase the therapeutic regimen for hyperglycemia and hence causes patient noncompliance to therapy.
Keywords: Diabetes Mellitus; Lower Respiratory tract infections; Hypertension; Inflammatory responses; Relapse; Diabetic complications; Patient noncompliance
Abbreviations: DM: Diabetes Mellitus, PAD: Peripheral Artery Disease, CHF: Congestive Heart Failure, CHD: Congenital Heart Defect, MI: Myocardial Infarction, BMJ: British Medical Journal, LRTI: Lower Respiratory Tract Infection, BMI: Body Mass Index, FBS: Fasting Blood Sugar, PPBS: Post Prandial Blood Sugar, BBF: Before Break Fast, OD: Once Daily, BD: Twice Daily, TID: Thrice Daily, BP: Blood Pressure, RR: Respiratory Rate, PR: Pulse Rate, SpO2: Percentage saturation of oxygen, ECG: Electrocardiogram, PFT: Pulmonary Function Test, CXR: Chest X-ray, GRBS: Generalized Random Blood Sugar, FEV1: Forced Expiratory Volume 1
Introduction
Diabetes mellitus (DM) is a group of common metabolic disorders that have the phenotype of hyperglycemia. Genetical inheritance and environmental exposure together result in distinct types of DM. Depending on the etiology of the DM, factors contributing to disease include reduced insulin secretion, decreased glucose utilization, and increased glucose production which can be simply stated as development of insulin esistance. The metabolic imbalance associated with DM causes secondary pathophysiologic changes in different organ systems that thrust a massive destructive burden on the patient's quality of life [1].Insulin resistance and abnormal insulin secretion are central to the development of type 2 DM. Although the primary cause is disputable, most studies support the view that insulin resistance antecedes an insulin secretary defect but that diabetes develops only when insulin secretion becomes scanty.
Cardiovascular attacks are observed in individuals with type 1or type 2 DM. The Framingham Heart Study disclosed a notice able increase in PAD, CHF, CHD, MI, and sudden death (risk increase from one- to fivefold) in patients with DM. The American Heart Association has stated DM as a "CHD risk equivalent" since many patients is prone to it. In addition to these complications, attack of infectious diseases has become a major problem to the clinicians during their management. Findings from the study, published in British Medical Journal (BMJ), indicate that patients who are suffering with LRTI along with diabetes may require intensified care in order to reduce their risk of death. Although some studies state there is a link between hyperglycemia and mortality from LRTI, results from other studies show no clear association [2]. The predisposition for infection may also be based on conditions that interfere with normal clearance mechanisms and on disturbance of pulmonary immune cell function. Several aspects of immunity such aspolymorphonuclear Leukocyte function (i.e. leukocyte adherence, chemotaxis and phagocytosis) and bactericidal activity of serum are depressed in patients with diabetes [3].
Hyperglycemia impairs a wide range of functions in neutrophils and monocytes. This is particularly important in limiting invasion by pyogenic and other bacteria. The presence of healthy microcirculation is essential to certain infectious insults. Inversion in the function of capillary endothelium, the rigidity of red blood corpuscles and changes in the oxygen dissociation curve that occur as a result of chronic hyperglycemia are factors which affect the person's ability to fight infections. Hence it is not surprise that patients with longstanding diabetes are at a greater risk or prone to infections. The reduced oxygen supply to tissue as a result of microvascular changes make them vulnerable to the infections by anaerobic microorganisms which grow best under such conditions [4].
Poor glycemic control is a common denominator in individuals with these infections. But the present case study had an inverse impact on patient. Patient has been receiving therapy for diabetes since 7 years under which it must be under proper control. Conversely the patient had an elevation of glycemia. The underlying cause was unknown. Upon investigation, we came to know that LRTI was left improperly treated. We know that diabetes brings about lot of metabolic disturbances inside the body. They are weight loss, ketoacidosis and inter current illnesses. An interdependence of these factors lead to release of stress hormones. Here, the inter current illnesses are nothing but infections. These stress hormones like cortisol, catechol amines and growth hormones oppose the action of insulin and hence causes an elevated and aggressive hyperglycemia than it existed earlier.
This can precipitate an acute exacerbation of insulin resistance and insulin deficiency, and result in more severe hyperglycemia and dehydration [5]. The improper management of diabetes causes attack of infectious diseases whereas the improper management of infections can also cause elevation of diabetes. This statement is being supported by the present case study. Other works support that improper control of diabetes causes complications, both micro vascular and macro vascular. This case supports both statements i.e. improper therapeutic management of LRTI has led to its relapse along with aggravation of glycemic levels and outcome of new cardiovascular complications. An abnormal ECG with unconfirmed diagnosis is supportive to this. Our main objective is to observe the elevation and depression of glycemic levels with respect to the therapeutic management and identification of new clinical concerns for a better management of diabetes and LRTI having a preexisting hypertension (Figure 1).
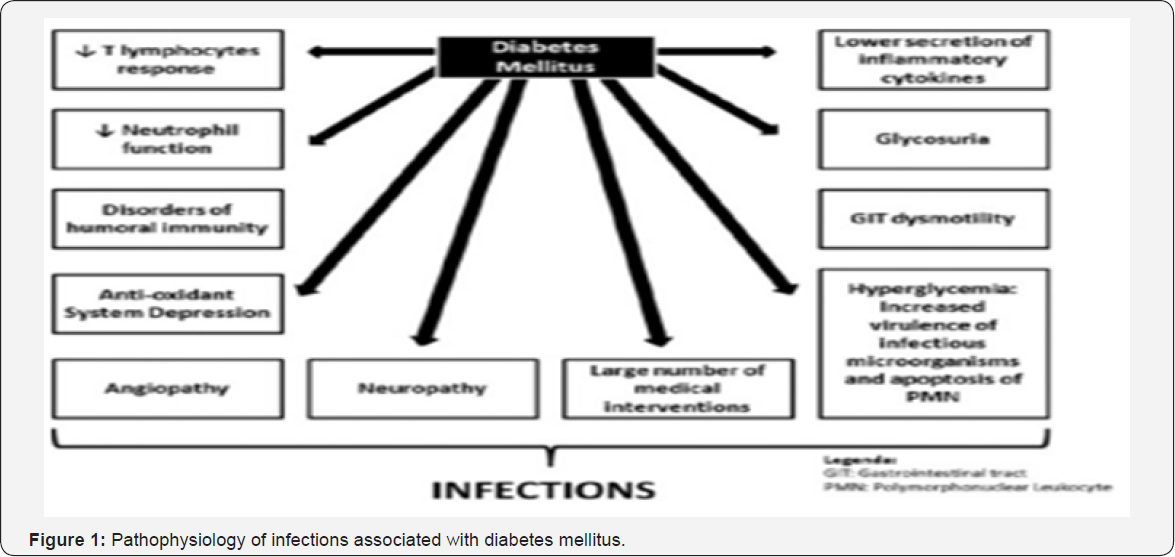
Case Report
Mrs. VG is a 66yr old patient admitted to general ward. She has an average BMI of 23.2kg/m2. She was admitted on 2/25 with chief complaints of burning sensation of feet and hands with generalized weakness and constipation. She had an additional complaint of right shoulder pain. Her systemic examination revealed irregular breath sounds with creps in right lung infrascapular region. She had an elevation of FBS with 177mg/ dL and PPBS with 275mg/dL. The patient was reported to be a known case of type 2 diabetes mellitus and hypertension since 7 years. She was advised for admission but left home the after physician consultation. She was given medication for a week days. Her prescription included Tab. Levofloxacin 500mg/OD, Syrup Ambroxol 10ml/BD, Tab. Monteleukast + Levocetirizine OD, Duolin Rotacap BD (Salbutamol 200mcg + Ipratropium 40mcg) and Aerocort Rotacap BD (Salbutamol 200mcg + Beclomethasone Dipropionate 100mcg).
Mrs. VG has reported to the general ward again on 3/3 with same complaints. Her history of present illness was reported to be burning sensation of feet and hands since one week, generalized weakness with uneasiness in upper abdomen and thoracic region. She complained of nausea, anorexia, insomnia and increased frequency of micturition. Being a known case of Type 2 Diabetes Mellitus and hypertension, she reported that she had an attack of pneumonia 4 months ago for which she used Duolin rotacaps BD (Salbutamol 200mcg + Ipratropium 40mcg). She was immediately admitted as In-patient.
Her Past Medication History included Tab. Metformin 500mg/OD(BBF) for DM and Tab. Losartan potassium 25mg/ OD for hypertension. The medication reported was being used since 5 months and earlier medication was not known, stating that she was under medication since 7 years. Her socioeconomic status was weak and worked as a farmer for 2-3 years in the past. Her vitals were normal(BP 120/80mmHg, PR 90bpm, RR 22bpm, Temperature 98.3°F, SpO2 98%) and system examination revealed abnormal breath sounds with B/L creps in infrascapular region. Her GRBS was 159mg/dL.
On 3/3 further investigations were performed. It included ECG, PFT and CXR. ECG: HR-100, Sinus Tachycardia, Left atrial enlargement, Non-specific T abnormalities. Finally reported as abnormal ECG with unconfirmed diagnosis. PFT: FEV1- 28% predicted. Pre-test:- FEV1 25.6%. Post-test:- FEV1 3.0%. It was interpreted as Very Severe Obstruction.
CXR: PA View, white dense mass in the upper lobe of left lung, NON HOMOGENOUS OPACITY. Final diagnosis was given as a known case of Type II DM with Hypertension and LRTI under observation. On day 1 i.e. 3/3, she was treated with Inj. Levofloxacin 500mg/IV/OD, Inj. Ondansetron 4mg IV/TID, Inj. Rabeprazole 20mg/IV/OD, Inj. Diclofenac 75mg/3ml IM/STAT, Tab. Monteleukast + Levocetirizine OD, Tab. Glimepiride + Metformin 0.5mg + 500mg OD(BBF) and Tab. Zolpidem 10mg/ OD (9PM). She was advised for FBS and PPBS investigation. She was under continuous fluid input of NS and RL with 100ml/hr infusion rate. Her vitals were normal throughout the day.
On day 2 i.e. 3/4, her vitals were stable. Lab investigations revealed FBS - 141mg/dL, PPBS - 196mg/dL. Rests of the vitals were normal. The dose of glimepiride was increased to 1mg. In the evening, the patient had uneasiness in the upper abdominal and thoracic region. Upon further examination, her treatment plan was modified by adding Duolin Rotacap BD (Salbutamol 200mcg + Ipratropium 40mcg) and Aerocort Rotacap BD (Salbutamol 200mcg + Beclomethasone Dipropionate 100mcg).
On day 3 i.e. 3/5, no fresh complaints were stated. Same treatment was continued. She was discharged in the evening. Her medications to home included Tab. Levofloxacin 500mg/ OD, Tab. Monteleukast + Levocetirizine OD, Duolin Rotacap BD (Salbutamol 200mcg + Ipratropium 40mcg) and Aerocort Rotacap BD (Salbutamol 200mcg+Beclomethasone Dipropionate 100mcg), Tab. Glimepiride + Metformin 1mg + 500mg OD(BBF), Tab. Pantoprazole 40mg OD (6AM), Tab. Telmisartan 20mg OD, Tab. Zolpidem 10mg/OD (9PM) and Syrup Lactulose 10ml/ SOS. Review after 10 days at general medicine department was advised.
Results and Discussion
Right from the beginning, the patient was complaining about burning sensation of feet and hands, generalized weakness and uneasiness in the upper abdomen and thoracic region. Of all these, her problem of uneasiness indicates toward a lower respiratory tract infection. It is supported by signs of inflammation and infection like burning sensation. Her past complaint of pneumonia was improperly treated with rotacaps which is not sufficient to prevent its relapse as well as her noncompliance to those rotacaps was reported which indicate towards an aggravation of the condition.
Symptoms like anorexia, nausea, insomnia and increased frequency of micturition indicate that she is suffering with some metabolic disorder. Her past history shows her status of diabetes and hypertension. In such conditions, the entire symptom logy would indicate towards her imbalanced condition of diabetes. This suspicion is supported by her abnormal FBS and PPBS levels with 177mg/dL and 275mg/dl respectively. Though the patient was given a prescription for suspected LRTI and continuity of her past medication for diabetes and hypertension, she was again admitted to hospital indicating that her treatment plan was improper.
Her revisit to hospital proved to be worth full since it made the physician to advice ECG, PFT and CXR. ECG revealed sinus tachycardia which can be expected to be a complication of diabetes. But the PFT and CXR revealed a very severe obstruction indicating a strong LRTI. Her therapeutic plan was changed which followed the guidelines of diabetic and LRTI treatment. Surprisingly, hypertension was left untreated which resulted in an increase of BP from 110/80mmhg on day 2 to 140/90mmhg on day 3. Though it can be considered as a normal value for such an age group, a sudden alteration in value must be taken into consideration. Coming to the aggravation of diabetes in relation to the relapse of LRTI, the following points must be considered.
a) In the past 7 years, the patient has never complained of elevated sugar levels since she has been under continuous medication.
b) Due to improper observation, lack of sanitation, occupational exposure to farm dust and reduced immune response due to diabetes [4-9], the patient had an attack of pneumonia. She was treated only with a Duolin Rotacap BD (Salbutamol 200mcg + Ipratropium 40mcg), which would reduce the obstruction but doesn't control the infection, has led to its relapse after four months.
c) Upon comparison of these two conditions, one can strongly say that pneumonia was not properly managed. These inter current illnesses result in development of stress conditions which further led to excessive hyperglycemia than earlier. That's the reason for elevation of sugar levels even under treatment with metformin. This condition led to change in diabetic medication to Tab. Glimepiride + Metformin 0.5mg + 500mg OD(BBF) and was again finally modified to Tab. Glimepiride + Metformin 1mg + 500mg OD(BBF) on day 3.
d) When the patient was given Tab. Levofloxacin 500mg/ OD, Tab. Monteleukast + Levocetirizine OD, Duolin Rotacap BD (Salbutamol 200mcg + Ipratropium 40mcg) and Aerocort Rotacap BD (Salbutamol 200mcg+Beclomethasone Dipropionate 100mcg), she has shown an improvement in condition. B/L creps were not heard and uneasiness was reduced by day 3.
e) Development of stress condition and its impact on diabetes is also supported by her anxiety which resulted as insomnia and hence was given Tab. Zolpidem 10mg/OD (9PM).
f) No strong evidence or systematic review or metaanalyses is available to support the aggravation diabetes due to relapse of LRTI, clinicians need to focus on the point that there is an inter-relationship between diabetes and infections [2]. A continuous examination of the infectious state of diabetic patients is compulsory to avoid further complications. Physicians must concentrate that a diabetic patient must be monitored for abnormalities in cardiovascular system, nervous system, immune system, renal system etc. All the micro vascular and macro vascular complications lead to alterations in immune system. Hence a parallel observation of hygiene and its management would help the patient improve his health related quality of life.
Interventions
I. Improper use of levocetirizine + monteleukast combination where rotacaps along with levofloxacin is enough for management of LRTI.
II. Hypertension was left untreated which caused to an elevation in blood pressure on day 3 of hospitalization.
III. Though sinus tachycardia was reported by ECG, no change in treatment plan was made.
IV. Using two rotacaps consisting of same combination would cause drug duplication. It is necessary to subside any one medication.
References
- Dan L Longo, Anthony S Fauci, Dennis L Kasper, Stephen L Hauser, J Larry Jameson, et al. (2012) Harrison's principles of internal medicine (18th edn), The McGraw-Hill Companies, Inc., New York, USA.
- Grace Rattue (2012) Pneumonia Patients with High Glucose Levels at Greater Risk of Death, Medical news today, USA.
- Dutt J, Dabhi LA (2014) Study of pneumonia in diabetic patients. Int J Med Sci Public Health 3: 974-976.
- Spomenka Ljubic, Ayyasamy Balachandran, Ivana Pavlic-Renar, Ante Barada, Zeljko Metelko (2004) Pulmonary infections in diabetes mellitus. Diabetologia Croatica 33(4): 115-124.
- Brian R Walker, Nicki R Colledge, Stuart H Ralston, Ian D Penman (2014) , Churchill Livingstone Elsevier, New York, USA, pp. 806.
- Juliana Casqueiro, Janine Casqueiro, Cresio Alves (2012) Infections in patients with diabetes mellitus: A review of pathogenesis, Indian J Endocrinol Metab 16(Suppl1): S27-S36.
- Miquel Falguera, Ricard Pifarre, Antonio Martin, Anas Sheikh, Anna Moreno (2005) Etiology and Outcome of Community Acquired Pneumonia in Patients With Diabetes Mellitus, chest 128(5): 32333239.
- Martins M, Boavida JM, Raposo JF, et al. (2016) Diabetes hinders community acquired pneumonia outcomes in hospitalized patients. BMJ Open Diabetes Research and Care 4(1): e000181.
- Shruthi Bettegowda, Vimala Sheshadri Iyengar, Varun Gosain, Vikas Govind Naik, Spandana Vuyyuru, et al. (20014) Clinical profile and Spectrum of Infections in Type 2 Diabetes Mellitus Patients: A Retrospective Study from Rural Tertiary Care Hospital of South Karnataka, India. Sch J App Med Sci 2(6G): 3331-3336.






























