CCBs and Neuroprotection: A Genuine Benefit
Leandro Bueno Bergantin* and Afonso Caricati-Neto
Department of Pharmacology, Universidade Federal de Sao Paulo (UNIFESP), Brazil
Submission: February 27, 2017; Published: March 14, 2017
*Corresponding author: Leandro Bueno Bergantin, Laboratory of Autonomic and Cardiovascular Pharmacology, Department of Pharmacology, Escola Paulista de Medicina, Universidade Federal de Sao Paulo (UNIFESP), Rua Pedro de Toledo, 669 - Vila Clementino, Sao Paulo - SP, Brazil, Tel: 55 11 5576-4973; 04039-032; Email: leanbio39@yahoo.com.br
How to cite this article: Leandro B B, Afonso C. CCBs and Neuroprotection: A Genuine Benefit. J of Pharmacol & Clin Res. 2017; 2(3): 555589. DOI: 10.19080/JPCR.2017.02.555589
Abstract
It has been almost 4 years since we revealed the explanation for the enigma of the so-called "calcium paradox”. Interestingly, this discovery initiated decades ago when numerous clinical studies have reported that use of L-type Ca2+ channel blockers (CCBs) by hypertensive patients decreased arterial pressure, but produced typical symptoms of sympathetic hyperactivity, such as tachycardia and increment of catecholamine plasma levels. Despite these adverse effects of CCBs have been initially attributed to adjust reflex of arterial pressure, during almost four decades this enigmatic phenomenon (the so-called "calcium paradox") remained unclear. In 2013, through an ingenious experiment, we discovered that this phenomenon was resulting of increment of transmitter release from sympathetic neurons, and adrenal chromaffin cells, stimulated by CCBs due to its interference on the Ca2+/cAMP signalling interaction. In this way, our discovery of the role of Ca2+/cAMP intracellular signalling interaction in the neurotransmitter release, and neuronal death triggered by cytosolic Ca2+ overload, opened novel adventures for the development of new pharmacological strategies more effective for the treatment of neurological and psychiatric disorders resulting of neurotransmitter release deficit, and neuronal death. These novel concepts have been extensively documented in several cited international papers of our own authorship (Bergantin and Caricati-Neto), and in an international book.
Keywords: Ca2+cAMP Signalling Interaction; Calcium Paradox; Neurological/Psychiatric Disorders
Abbreviations: CCBs: Ca2+ channel blockers; ACs: Adenylyl Cyclases; PDEs: Phosphodiesterases; ER: Endoplasmic Reticulum
Introduction
The notion of stimulus-secretion coupling to explain neurotransmitters and hormones release has been resulted from ingenious experiments performed by Douglas and Rubin in the 1960s [1]. Complementing their concepts, Baker and Knight revealed in 1970's that a rise in the cytosolic Ca2+ concentration ([Ca2+]c) is an elementary requirement to trigger transmitter release [2]. Indeed, the definite demonstration of a direct relationship between neurotransmitter release and increase in [Ca2+]c derived from the fundamental experiments performed by the Nobel laureate Erwin Neher [3]. More recently, many results have shown that cAMP increases neurotransmitter release at many synapses in autonomic nervous system of vertebrate, including sympathetic neurons [4]. Although the cellular mechanisms involved in these enhancer effects of cAMP on the release of neurotransmitters and hormones are under debate, the evidences indicate that this important intracellular messenger modulates signalling pathways mediated by Ca2+ involved in the regulation of neurotransmitter, and hormones release.
The Ca2+/cAMP signalling interaction as a universally- operated concept
The interaction between the intracellular signalling pathways mediated by Ca2+ and cAMP, named Ca2+/cAMP signalling interaction, has been widely studied in different cell types and tissues. This nowadays accepted concept assumes that this interaction results in synergistic actions of these intracellular messengers on cell functions regulated by adenylyl cyclases (ACs), and phosphodiesterases (PDEs) [5-8]. The Ca2+/cAMP signalling interaction has particularly been extensively studied at the endoplasmic reticulum (ER) Ca2+ channels, such as Ca2+ channels regulated by ryanodine receptors (RyR) [5-8]. Our own experiments established that Ca2+/cAMP signalling interaction play a key role in the regulation of neurotransmitter release from neurons and neuroendocrine cells [5-8]. Then, dysfunctions of cellular homeostasis of Ca2+ and/or cAMP in these cells could result in the dysregulation of Ca2+/cAMP signalling interaction, and could be a novel therapeutic goal for medicines.
CCBs and neuroprotection: a genuine benefit
Indeed, several medical studies have been evidencing that acute and chronic use of L-type Ca2+ channel blockers (CCBs) in the antihypertensive therapy, such as nifedipine and verapamil, decreased peripheral vascular resistance and arterial pressure arterial, but produced typical symptoms of sympathetic hyperactivity such as tachycardia, and increment of catecholamine plasma levels [9]. Despite these adverse effects of CCBs have been initially attributed to adjust reflex of arterial pressure, during almost four decades the cellular and molecular mechanisms involved this enigmatic phenomenon named "calcium paradox" remained without additional explanation.
In 2013, through an ingenious experiment, we discovered that the "calcium paradox" phenomenon was resulting of increment of transmitter release from sympathetic neurons, and adrenal chromaffin cells, stimulated by CCBs due to its interference on the Ca2+/cAMP signalling interaction [6]. Using isolated tissues richly innervated by sympathetic nerves (rat vas deferens) to exclude the influence of adjusting reflex, we showed that neurogenic responses of the vas deferens were completely inhibited by L-type CCBs in high concentrations (>1 μmol/L), but unpredictably, and paradoxically, potentiated in concentrations below 1 μmol/L, characterized by sympathetic hyperactivity induced by CCBs [10-12].
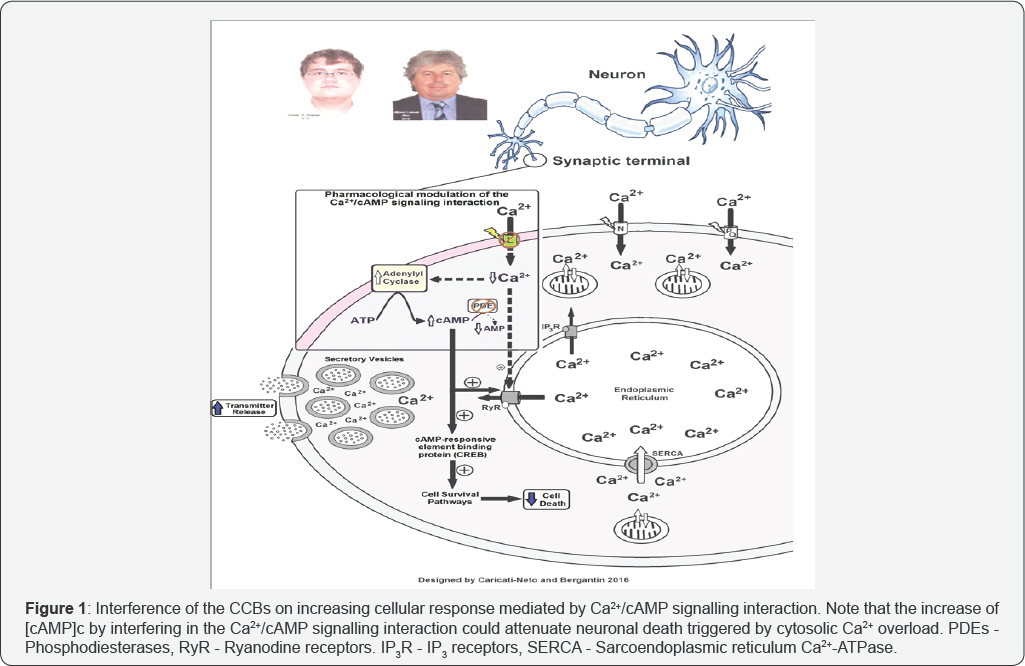
Our studies showed that this paradoxical sympathetic hyperactivity is caused by increment of neurotransmitter release from sympathetic neurons produced by L-type CCBs due to its interference on the Ca2+/cAMP signalling interaction [5-8] (Figure 1). In addition, several studies have showed that increase of cytosolic cAMP concentration ([cAMP]c) stimulates neuroprotective response [13,14]. In this way, increase of [cAMP]c by interfering in the Ca2+/cAMP signalling interaction could attenuate neuronal death triggered by cytosolic Ca2+ overload [5-8]. Then, the pharmacological handling of the Ca2+/ cAMP signalling interaction produced by combination of the L-type CCBs used in the antihypertensive therapy, and [cAMP] c enhancer compounds used in the anti-depressive therapy such as rolipram, could be a new pharmacological strategy for enhancing neurotransmission in neurological and psychiatric disorders resulting of neurotransmitter release deficit, and/or neuronal death [5-8]. Indeed, it was showed that the treatment with L-type CCBs reduces motor symptoms, and attenuates progressive neuronal death in animal model of degenerative disease, suggesting that L-type CCBs are potentially viable neuroprotective agents [15].
In addition, a 10-year follow-up study (2000 to 2010), involving 82,107 hypertensive patients of more than 60 years of age, showed that use of L-type CCBs reduced blood pressure and risk of dementia in hypertensive patients, suggesting that these drugs could be clinically used to treat Alzheimer's disease [16]Supportive findings for the neuroprotective effects of CCBs have been demonstrated in 1,241 elderly hypertensive patients with memory impairment [17]. The use of CCBs decreased the risk of cognitive impairment, and Alzheimer's disease, independently of blood pressure levels, when compared to patients not receiving CCBs [17]. These findings reinforced the idea that attenuation of cytosolic Ca2+ overload produced by L-type CCBs due to blockade of Ca2+ influx through L-type VACC could be an excellent pharmacological strategy to attenuate, or prevent, neuronal death in neurodegenerative diseases. These findings could open a new avenue for the drug development more effective and safer for the treatment of Alzheimer's diseases [18-24].
Conclusion
CCBsand neuroprotection: a genuinebenefit.Pharmacological handling of the Ca2+/cAMP signalling interaction could be a more efficient and safer therapeutic strategy for stimulating neurotransmission compromised by neurotransmitter release deficit, and attenuating neuronal death.
Disclosure Statement
Caricati-Neto and Bergantin thank the continued financial support from CAPES, CNPq and FAPESP (Bergantin's Postdoctoral Fellowship FAPESP #2014/10274-3). The authors also thank Elsevier - "author use": Reuse of portions or extracts from the article in other works - https://www.elsevier.com/data/assets/pdffile/0007/55654/AuthorUserRights.pdf.
References
- Douglas WW, Rubin RP (1961) The role of calcium in the secretory response of the adrenal medulla to acetylcholine. J Physiol 159: 40-57.
- Baker PF, Knight DE (1978) Calcium-dependent exocytosis in bovine adrenal medullary cells with leaky plasma membranes. Nature 276(5688): 620-622.
- Neher E, Zucker RS (1993) Multiple calcium-dependent processes related to secretion in bovine chromaffin cells. Neuron 10(1): 21-30.
- Chern YJ, Kim KT, Slakey LL, Westhead EW (1988) Adenosine receptors activate adenylate cyclase and enhance secretion from bovine adrenal chromaffin cells in the presence of forskolin. J Neurochem 50(5): 14841493.
- Afonso Caricati-Neto, Antonio G Garcia, Leandro Bueno Bergantin (2015) Pharmacological implications of the Ca2+/cAMP signalling interaction: from risk for antihypertensive therapy to potential beneficial for neurological and psychiatric disorders. Pharmacology Research & Perspectives 3(5): e00181.
- Bergantin LB, Souza CF, Ferreira RM, Smaili SS, Jurkiewicz NH, et al. (2013) Novel model for "calcium paradox" in sympathetic transmission of smooth muscles: role of cyclic AMP pathway. Cell Calcium 54(3): 202-212.
- Leandro Bueno Bergantin, Aron Jurkiewicz, Antonio G Garcia, Afonso Caricati-neto (2015) A Calcium Paradox in the Context of Neurotransmission. Journal of Pharmacy and Pharmacology 3: 253261.
- Leandro Bueno Bergantin, Afonso Caricati-Neto (2016) Challenges for the pharmacological treatment of neurological and psychiatric disorders: Implications of the Ca2+/cAMP intracellular signalling interaction. European Journal of Pharmacology 788: 255-260.
- Grossman E, Messerli FH (1998) Effect of calcium antagonists on sympathetic activity. Eur Heart J : F27-F31.
- Kreye VA, Luth JB (1975) Proceedings: verapamil-induced phasic contractions of the isolated rat vas deferens. Naunyn Schmiedebergs Arch Pharmacol 287: R43.
- AM French, NC Scott (1981) A comparison of the effects of nifedipine and verapamil on rat vas deferens. Br J Pharmacol 73(2): 321-323.
- Moritoki H, Iwamoto T, Kanaya J, Maeshiba Y, Ishida Y, et al. (1987) Verapamil enhances the non-adrenergic twitch response of rat vas deferens. Eur J Pharmacol 140(1): 75-83.
- Sommer N, Loschmann PA, Northoff GH, Weller M, Steinbrecher A, et al. (1995) The antidepressant rolipram suppresses cytokine production and prevents autoimmune encephalomyelitis. Nat Med 1(3):244-248.
- Xiao L, O'Callaghan JP, O'Donnell JM (2011) Effects of repeated treatment with phosphodiesterase-4 inhibitors on cAMP signaling, hippocampal cell proliferation, and behavior in the forced-swim test. J Pharmacol Exp Ther 338(2): 641-647.
- Ilijic E, Guzman JN, Surmeier DJ (2011) The L-type channel antagonist isradipine is neuroprotective in a mouse model of Parkinson's disease. Neurobiol Dis 43(2): 364-371.
- Wu CL, Wen SH (2016) A 10-year follow-up study of the association between calcium channel blocker use and the risk of dementia in elderly hypertensive patients. Medicine (Baltimore) 95(32): e4593.
- Hanon O, Pequignot R, Seux ML, Lenoir H, Bune A, et al. (2006) Relationship between antihypertensive drug therapy and cognitive function in elderly hypertensive patients with memory complaints. J Hypertens 24(10): 2101-2107.
- Leandro Bueno Bergantin, Afonso Caricati-Neto (2016) Insight from "Calcium Paradox" due to Ca2+/cAMP Interaction: Novel Pharmacological Strategies for the Treatment of Depression. International Archives of Clinical Pharmacology 2(1).
- Bergantin LB, Caricati-Neto A (2016) Novel Insights for Therapy of Parkinson's disease: Pharmacological Modulation of the Ca2+/cAMP Signalling Interaction. Austin Neurol & Neurosci 1(2): 1009.
- Leandro Bueno Bergantin, Afonso Caricati-neto (2016) Recent advances in pharmacotherapy of neurological and psychiatric disorders promoted by discovery of the role of Ca2+/cAMP signaling interaction in the neurotransmission and neuroprotection. Adv Pharmac J 1(3): 66-70.
- Bergantin LB, Caricati-Neto A (2016) From discovering "calcium paradox" to Ca2+/cAMP interaction: Impact in human health and disease. Scholars' Press, USA, 108p.
- Afonso Caricati-neto, Leandro Bueno Bergantin (2016) New therapeutic strategy of Alzheimer's and Parkinson's diseases: Pharmacological modulation of neural Ca2+/cAMP intracellular signaling interaction. Asian Journal of Pharmacy and Pharmacology 2(6): 136-143.
- Afonso Caricati-neto, Leandro Bueno Bergantin (2016) Impact of interaction of Ca2+ /cAMP Intracellular Signalling Pathways in Clinical Pharmacology and Translational Medicine. Clinical Pharmacology and Translational Medicine p. 1-4.
- Bergantin LB, Caricati-Neto A (2016) Challenges for the Pharmacological Treatment of Dementia: Implications of the Ca2+ / cAMP Intracellular Signalling Interaction. Eur J Pharmacol 788: 255260.






























