Becker’s Nevus and Shagreen Patch: Extraordinary Cutaneous Association with Neurofibromatosis in Two Successive Generation
Manisha Nijhawan, Savita Agrawal, Virendra N Sehgal*, Manmohan Bagri, Subhash Bishnoi and Shivi Nijhawan
Department of Skin, Mahatma Gandhi medical College and Hospital, India
Submission: February 02, 2019; Published: August 28, 2019
*Corresponding author: Virendra N Sehgal, Dermato Venerology (Skin/VD) Center, Sehgal Nursing Home, India
How to cite this article: Manisha Nijhawan, Savita Agrawal, Virendra N Sehga, Manmohan Bagri, Subhash Bishnoi, Shivi Nijhawan. Becker’s Nevus and Shagreen Patch: Extraordinary Cutaneous Association with Neurofibromatosis in Two Successive Generation. JOJ Dermatol & Cosmet. 2019; 1(5): 555575.
Abstract
Neurofibromatosis type 1 or Von Recklinghausen disease is an autosomal dominant condition, manifested by overgrowth of nervous tissue and skin discoloration. Becker’s nevus is a benign cutaneous hemartomatous disorder. Shagreen patch is a connective tissue nevus seen in 20-50% cases of tuberous sclerosis. However, the association between becker’s nevus with neurofibromatosis is rare and a very few cases have been reported in literature. Its association with shagreen patch has not been reported yet. We are reporting a case in which father is having shagreen patch along with neurofibromatosis whereas son is having large becker’s nevus with neurofibromatosis. This unique association in two successive generation has never been reported before in literature.
Keywords: Shagreen patch; Becker’s nevus; Plexiform neurofibroma
Introduction
Neurofibromatosis (NF) is an autosomal dominant disorder, which primarily affect the growth of neural tissue which is derived from neural crest [1]. NF1 gene is located at chromosome 17q11.2. [2,3]. Its clinical presentation may vary from benign café-au-lait macules to malignant degeneration of plexiform neurofibromas. Becker’s nevus is a benign cutaneous hemartomatous disorder, which is characterized by large hyperpigmented macule with irregular border and hypertrichosis [4]. While Shagreen patch is a connective tissue nevus, present as firm to rubbery irregular skin colour plaque, most commonly found in lumbosacral region [5].
It is reported to be present in 20-50% cases of tuberous sclerosis but no case is so far reported with NF1. Association of Becker’s nevus with NF is extremely rare and only a few case reports [6] are thus far available following literature survey. A rare association of NF1 with Shagreen patch in father and NF1 with becker’s nevus in his son is being reported for the first time to the best of literature survey.
Case Study
Case 1:
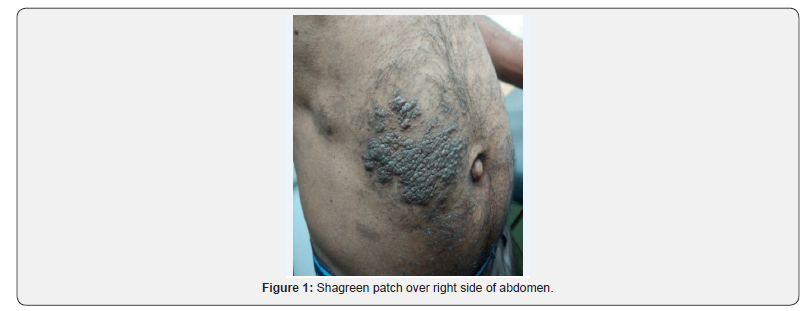
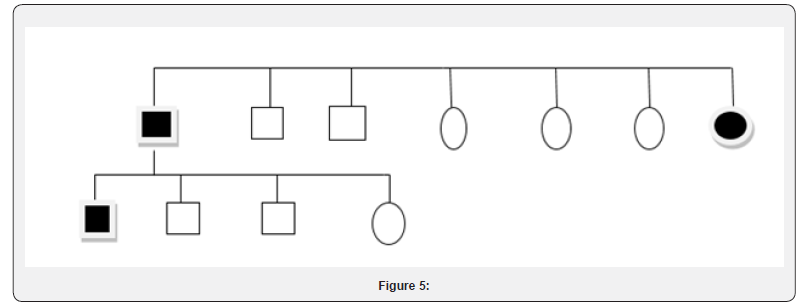
A 50 years old man, presented with a single large asymptomatic pigmented lesion, occupying right lower abdomen, the shagreen patch. In addition, history of multiple asymptomatic discrete small raised lesions over the back was affirmative. However, there was neither history of discomfort/ pain in the abdomen nor altered bowel habit, anorexia and weight loss. A similar history could be elicited in father, sister and his son, In all 13 family member of two generation were scanned for the purpose of whom only 4 were found afflicted (vide supra) with the disease, while remaining 9 including 3 of his own children were unaffected depicting in the adjoining pedigree diagram. In addition, had Becker’s nevus, the precise details of which form the narrative of the second case.
Examination of the skin surface showed, a single hyperpigmented plaque of the size of 8x10cm it was non homogenous / irregular with well-defined borders, the shagreen patch. The plaque was non-tender, prominently located on the right lower abdomen Figure 1. In addition, café-au-lait macules of 1×2cm-4×2cm of skin color, non-tender multiple accompanied by a few flesh color nodules distributed, bilaterally were located Figure 2. Dermatoscopic finding of plaque showed reddish brown strands on ridges of skin lines. Linear strands were found to be studded with regularly spaced white dots. General physical examination was apparently normal.
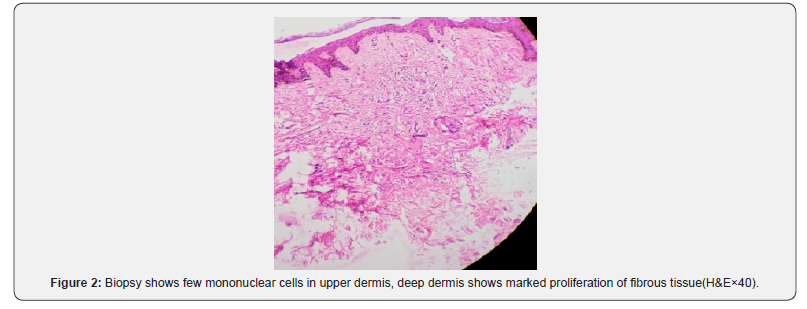
Hemotoxyllin & eosin (H&E) stained section prepared from skin biopsy of representative lesions of shagreen patch depicting mild to moderate hyperkeratosis prominent granular cell layer acanthosis representing uniform elongation of rete-ridges, whereas H & E Stained section from plaque reveled a few mononuclear cells in upper dermis, while deep dermis showed marked proliferation of fibrous tissue with crossing bundles of fibrous band Figure 2.
Case 2:
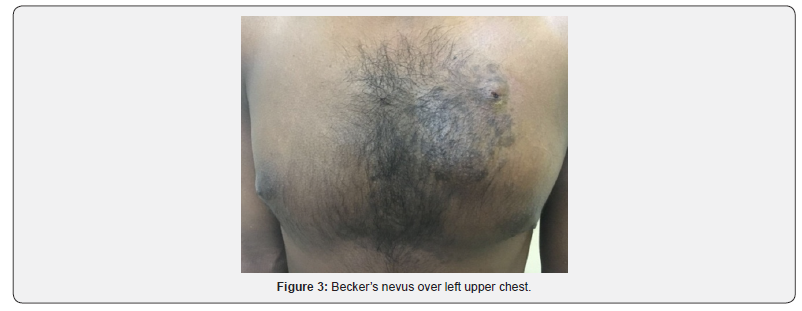
A 24-year-old son of the Ist case presented with complaint of large, dark brownish colored raised lesion, over the left upper chest for the past 3 years. No history of chest pain, breathlessness or any other systemic complains. History of similar lesion in his grandfather and father was present as shown in above pedigree. On cutaneous examination a large brown to black colored patch measuring 40×20cm in size with irregular border and increased coarse terminal hairs was seen over upper left chest Figure 3. There were two large illdefined masses of size 20×10cm over left upper back and 10×5cm over right lower leg with a bag of worm feeling on palpation was present. On further examination, Multiple CALMs over trunk and left axillary freckling was present. General, physical and systemic examinations were apparently normal. There were no neurological, musculoskeletal and bony deformity. Slit lamp examination showed lisch nodules at 4’ o clock and 10’o clock position. Dermatoscopic finding of patch revealed focal hypopigmentation, hair follicle, perifollicular hypopigmentation and vessels suggesting of becker’s nevus.
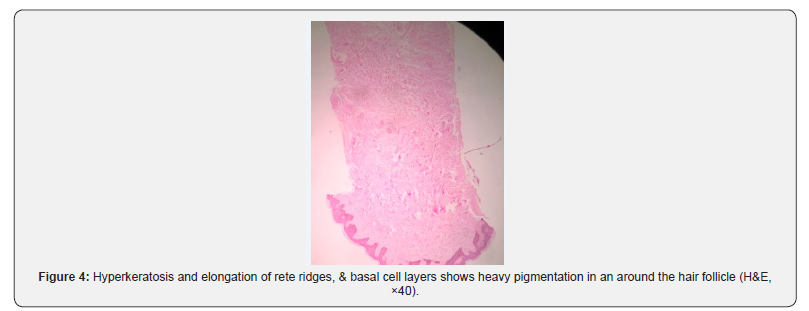
Histopathology of patch shows mild hyperkeratosis and elongation of rete ridges. The basal layers show heavy pigmentation, an increase in melanin pigment in the basal cell layer. Besides, prominence of pigmentation in an around the hair follicle Figure 4 was explicit. Routine blood investigation, X-ray chest, USG-whole abdomen was normal. On clinicopathologic correlation, diagnosis of becker’s nevus was made. Diagnosis of neurofibromatosis was made on basis of clinical criteria (Figure 5 & 6).
Discussion
Neurofibromatosis type 1 also known as Von Recklinghausen’s [1] disease, consider as a rare autosomal dominant condition affecting 1 in 3000 individuals worldwide. NF1 is a disorder of single gene-neurofibromin gene, which is located at chromosome 17q11.2. [2]. This gene is a large, spanning 350 kilobase of genomic DNA and contain 60 exons [2]. This protein has both structural and functional similarity to guanosine triphosphate-related proteins which serve as a negative regulator of ras oncogene, through a GTPase activating protein (GAP), which is essential for NF1 associated tumorigenesis [6]. In neurocutaneous tissues, loss of function mutations results in increased Ras activity, causing increased proliferation and tumorigenesis. In this men and women are equally affected with about 100 % penetrance of disease, about 50% of NF1 case are due to new mutations. Diagnostic criteria were developed by National Institute of Health consensus conference [7] in 1987 and refined by a second conference in 1997. Which is based on certain clinical criteria as follows (Table 1).
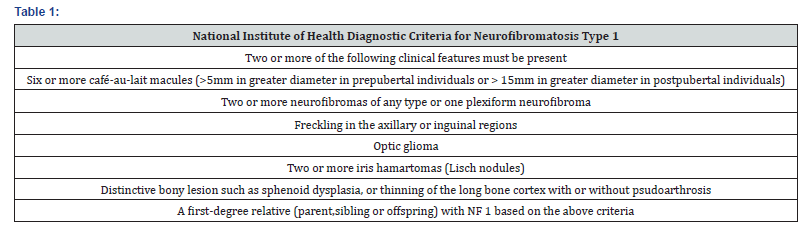
a) In case 1-Father fulfilling three criteria out of these as first degree relative, six or more CALMs, two or more neurofibroma.
b) In case 2-Son showing plexiform neurofibroma over upper back and right lower leg, bilateral lisch nodules, axillary freckling in left axilla, six or more CALMs.
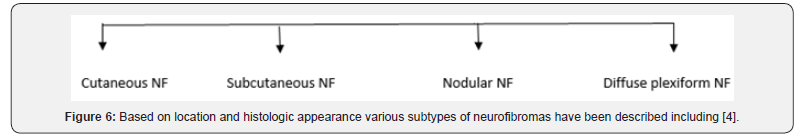
Cutaneous and subcutaneous NF arise from distal end of nerve and localized to cutaneous and subcutaneous skin layers respectively. Nodular NF arise from proximal nerve root and growing within organs. Diffuse plexiform NF involves long segments of multiple nerves [8]. Among these plexiform variants is a major cause of morbidity and disfigurement. About 20-44% individual with NF1 develop this variant.8 It may develop at birth or later in life as it is a slow growing tumor. It has 20% risk for malignant degeneration into peripheral nerve sheath tumor [8]. No specific treatment for this variant exists, beside surgical resection. Pirfenidone, an antifibrotic agent, has been shown to decrease the size of neurofibroma by up to 15% in a minority of patients, but in 24months follow up these results were not sustained. Thalidomide, a tumor necrosis factor-alpha inhibitor was also tested but gave poor result. Treatment for this variant is complete surgical excision of malignant peripheral sheath tumor with palliative chemotherapy but with surgical excision, a recurrence rate of 20% has been reported [6].
Becker’s had the distinction of formed a narrative of pigmented nevi including becker’s [9] nevus in the year 1949 also known as Becker’s melanosis, Pigmented hairy epidermal nevus [5]. It is suggested to follow a predominant inheritance pattern, means always occurs sporadically. It is a benign, focal cutaneous hemartoma, characterized by hyperpigmented macule with well-defined but irregular margins and presented with hypertrichosis. It is mostly present over upper trunk with prevalence of around 0.5% in population observed in French study [5]. There may be possibility of androgenic stimulation in its pathogenesis as it appears during puberty, there is increase number of terminal hairs and acne vulgaris and high male to female ratio and rarely associated with accessory scrotal and breast hypoplasia. Becker’s nevus syndrome is an association of Becker’s nevus with mammary hypoplasia, scoliosis or any other skin, muscle or skeletal alteration [8]. Various cutaneous association occurs including intradermal nevis, malignant melanoma, leiomyoma, lymphangioma and acneform eruptions. In microscopic examination, there is normal numbers of melanocytes, and increased levels of melanin in the basal epidermal layer. The epidermis shows acanthotic with variable hyperkeratosis and elongation of the rete ridges and dermis shows an increased number of arrector pili muscles which makes it difficult to differentiate from the related smooth muscle hamartoma [10]. The patient had no mammary hypoplasia or muscular or bone deformity. Only a few cases of Becker’s nevus with neurofibromatosis had been reported in the literature mostly with NF1, as both are hemartomatous proliferative disorders with increased expression of steroid hormone receptors. In future large sample size and molecular study will help to understand this association [5]. For becker’s nevus therapeutic intervention is because of cosmetic purpose. Long –pulsed alexandrite laser, Q-switch [11], Nd:YAG laser therapy has been used for treatment of both hypertrichosis and hyperpigmentation.
Shagreen patch first described by Hallopean and leredde in 1895, lesions frequency increase with age. First appeared at age of puberty and reported in 20-50% cases of tuberous sclerosis [3]. It is a connective tissue nevus which appeared as firm to rubberyirregular plaque commonly present over back, buttocks, thigh and nape of neck. Histopathology shows normal band of superficial dermis and irregular arranged collagen present in deeper dermis, also some other variant shows hamartomous proliferation of collagen bundles throughout dermis layer. In literature we were unable to find any previous reports showing two unusual association becker’s nevus and shagreen patch in two successive generation, may be this is the first case which must to be reported.
References
- Smeeing DPJ, Briet JP, Van KCS, Segers MM, Verleisdonk EJ, et al. (2018) Factors associated with wound- and implant-related complications after surgical treatment of ankle fractures. J Foot Ankle Surg 57(5): 942- 947.
- Mu Y, Edwards JR, Horan TC, Berrios-Torres SI, Fridkin SK (2011) Improving risk-adjusted measures of surgical site information for the National Healthcare Safety Network. Infect Control Hosp Epidemiol 32(10): 970-986.
- (2006) Health Protection Agency. Surveillance of Surgical Site Infection in England: October 1997-September 2005. London: Health Protection Agency
- Daneman N, Lu H, Redelmeier DA (2010) Discharge after discharge: Predicting surgical site infections after patients leave hospital. J Hosp Infect 75(3): 188-194.
- Delgado-Rodriguez M, Gomez-Ortega A, Sillero-Arenas M, Llorca J (2001) Epidemiology of surgical-site infections diagnosed after hospital discharge: A prospective cohort study. Infect Control Hosp Epidemiol 22(1): 24-30.
- Gibson A, Tevis S, Kennedy G (2014) Readmission after delayed diagnosis of surgical site infection: A focus on prevention using the American College of Surgeons National Surgical Quality Improvement Program. Am J Surg 207(6): 832-839.
- Gheorghe A, Moran G, Duffy H (2015) Health utility values associated with surgical site infection: A systematic review. Value Health 18(8): 1126-1137.
- Kaye KS, Anderson DJ, Sloane R (2009) The effect of surgical site infection on older operative patients. J Am Geriatr Soc 57(1): 46-54.






























