Combined Endo-Epicardial Approach and Scar Dechanneling Ablation in Arrhythmogenic Right Ventricular Cardiomyopathy
Pedro A Sousa1*, Nuno Cortez-Dias2, João de Sousa2, Luís Elvas1 and Lino Gonçalves1,3
1Pacing & Electrophysiology Unit, Cardiology Department, Coimbra’s Hospital and University Center, Coimbra, Portugal
2Invasive Arrhythmia Unit, Cardiology Department, Santa Maria Hospital and University Center, Lisboa, Portugal
3ICBR, Faculty of Medicine, University of Coimbra, Coimbra, Portugal
Submission: July 15, 2021; Published: August 17, 2021
*Corresponding author: Pedro A Sousa, Pacing & Electrophysiology Unit, Cardiology Department Coimbra’s Hospital and University Center, Coimbra, Portugal
How to cite this article: Pedro A S, Nuno C-D, João d S, Luís E, Lino G. Combined Endo-Epicardial Approach and Scar Dechanneling Ablation in Arrhythmogenic Right Ventricular Cardiomyopathy. J Cardiol & Cardiovasc Ther. 2021; 17(2): 555957. DOI: 10.19080/JOCCT.2021.17.555957
Abstract
A 47-year-old male diagnosed with Arrhythomogenic Right Ventricular Cardiomyopathy (ARVC) was referred for ablation due to recurrent ventricular tachycardia. Using the CARTO® 3 V6 system, both endocardial and epicardial voltage maps were acquired revealing an extensive epicardial scar with abundant local abnormal ventricular activities (LAVA) in distribution compatible with conducting channels. Epicardial scar dechanneling ablation allowed abolition of all LAVA’s. This case highlights the advantage of a combined endo-epicardial approach as a first-line therapy for ARVC, as well as of scar dechanneling ablation, which allowed elimination of all LAVA’s with a lesser extensive ablation.
Keywords: Ventricular tachycardia; Epicardial ablation; Arrhythmogenic right ventricular cardiomyopathy; Scar dechannelling ablation
Keywords: ARVC: Arrhythomogenic Right Ventricular Cardiomyopathy; LAVA: Local Abnormal Ventricular Activities; RV: Right Ventricle
Introduction
A 47-year-old male diagnosed with Arrhythomogenic Right Ventricular Cardiomyopathy (ARVC) was referred for ablation due to recurrent ventricular tachycardia with appropriate shocks despite optimized therapy with amiodarone and mexiletine.
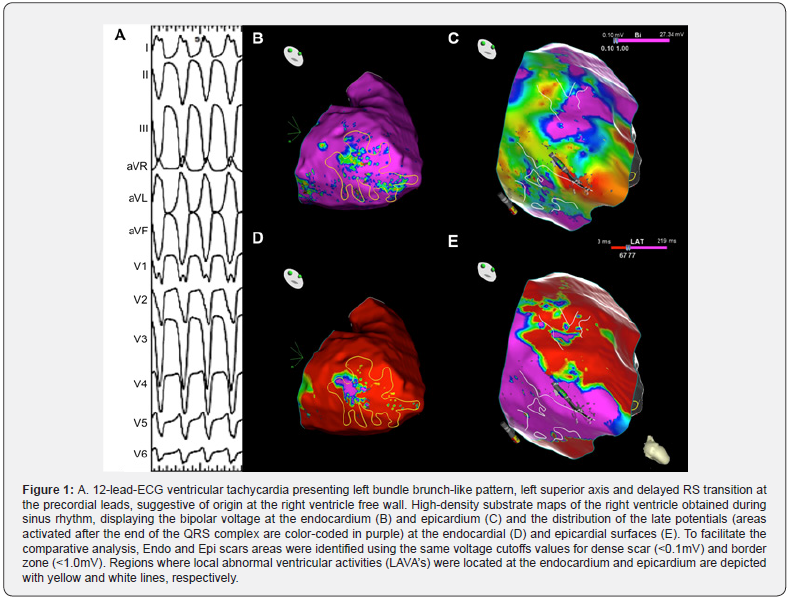
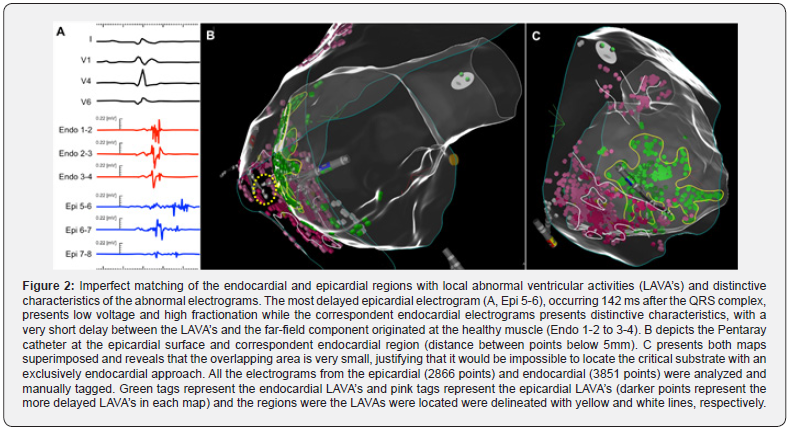
The procedure was performed under general anesthesia with continuous invasive arterial blood pressure monitoring. Programmed right ventricular (RV) stimulation induced a non-tolerated ventricular tachycardia (Figure 1-A) that required termination by overdrive pacing. Using the CARTO 3 V6 system (Biosense-Webster, Irvine, CA, USA), an endocardial high-density substrate voltage map of the RV (Figure 1-B and D) was obtained during stable sinus rhythm and a limited area with local abnormal ventricular activities (LAVAs) was identified at the mid-ventricular portion of the free wall. Since ARVC is typically associated with a more extensive epicardial arrhythmogenic substrate, a percutaneous subxyphoid access to the pericardial space was performed. The substrate epicardial map revealed a wider area of scar with abundant LAVAs in distribution compatible with conducting channels (pathways of orthodromically activated sites inside the scar – Figure 1-C and E), poorly matching the location of the endocardial regions with suspicious electrograms (Figure 2). Epicardial ablation of the anomalous conducting channels was performed. After ablation, VT was non-inducible with up to 4 extrastimuli from 2 different endocardial sites and the substrate map documented abolition of all LAVA’s.
This case highlights the advantage of a combined endo-epicardial approach as a first-line therapy, since ARVC typically presents a wider epicardial substrate, and of scar dechanneling ablation, which allowed elimination of all LAVA’s with a lesser extensive ablation.