The Role of Corticosteroids in Pediatric Viral and Idiopathic Pericarditis
Vladislav A Vukomanovic1,2*, Sergej M Prijic1,2, Stasa D Krasic1, Sanja S Ninic1, Ruzica Z Bradaric3, Bojko B Bjelakovic4 and Dejan M Nesic2,5
1Department of Cardiology, Mother and Child Health Care Institute of Serbia “Dr.Vukan Cupic”; Belgrade, Serbia
2School of Medicine, University of Belgrade, Serbia
3Department of Pediatrics, Hospital “Sveti Vracevi” Bijeljina, Bosnia and Herzegovina
4 Clinic of Pediatrics - Clinical Center Nis; School of Medicine, University of Nis, Serbia
5 Institute of Medical Physiology “Rihard Burian”, Serbia
Submission: April 04, 2019; Published: April 18, 2019
*Corresponding author: Vladislav A Vukomanovic, Pediatric cardiologist, Mother and Child Health Care Institute of Serbia “Dr Vukan Cupic” R. Dakica St. 6-8, 11070 Belgrade, Serbia
How to cite this article:Vladislav AV, Sergej MP, Stasa DK, Sanja SN, Ruzica ZB, et al. The Role of Corticosteroids in Pediatric Viral and Idiopathic Pericarditis. J Cardiol & Cardiovasc Ther. 2019; 13(5): 555872. DOI: 10.19080/JOCCT.2019.13.555872
Abstract
Background: Recurrence of pericarditis (ROP) is the important complication of the acute pericarditis. The aim of the study was to analyse the influence of aetiology, clinical funding and treatment on outcome of acute pericarditis.
Materials and Methods:Data were retrospectively collected from medical records of patients treated from 2011 to 2017 at the tertiary referent heart center.
Results:Our investigation included 56 children. Recidivism was registered in 8/56 patients, 2/29 (7.41 %) treated with nonsteroidal anti-inflammatory drugs (NSAID) and 6/27 (28.57 %) treated with corticosteroids (CS) and NSAID. Independent risk factor for ROP were viral pericarditis (p = 0.01, OR 31.46), lack of myocardial affection (p = 0.03, OR 29.15), CS use (p = 0.02, OR 29.02) and ESR ≥ 50 mm/h (p = 0.03, OR 25.23). In 4/8 patients the first recurrence was treated with NSAID and colchicine, while treatment of 4/8 patients included CS. Children with ROP treated with CS had higher median number of recurrence (5, IQR: 2-15) than those treated with colchicine (0, IQR: 0-0.75).
Conclusion:Independent risk factors for recurrence are CS treatment, viral aetiology, pericarditis only and ESR ≥ 50 mm/h. Idiopathic acute pericarditis should be treated with NSAID. Colchicine and NSAID might be recommended in children with the first ROP.
Keywords: Childhood; Colchicine; Corticosteroid; Pericarditis; Treatment
Abbrevations: CS: Corticosteroids; NSAID: Nonsteroidal anti-inflammatory drugs; ROP: Recurrence of pericarditis; ESR: Erythrocytes Sedimentation Rate; CRP: C-Reactive Protein; CMR: Cardiac Magnetic Resonance
Introduction
Pericarditis is a common disease in children and the cause of 1-5% of chest pains in childhood [1]. Up to 80 - 90% of cases of pericarditis are either idiopathic or viral origin [2]. However, majority of cases with idiopathic acute pericarditis have unrecognized viral or immune aetiology [3-5]. Recurrent pericarditis is the important complication of the acute form of the disease. Nevertheless, unlike in adults, there is no consistent data on the incidence and aetiology of both acute and recurrent pericarditis in children. The incidence of recurrence is estimated to be 15-30% in adult patients [6]. The European Society of Cardiology has published recommendations and guidelines for pericarditis treatment in adults [7], but standardized therapy protocol for pericarditis in children is yet to be established [8]. There is still a doubt regarding the use of corticosteroids (CS), whereas recently published studies support the positive role of colchicine and anakinra in the treatment of pericarditis [9].
The aim of our study was to analyze the hypothesis that the treatment of acute pericarditis by using CS increases recurrence rate.
Methods
A retrospective study was carried out at the Mother and Child Health Care Institute of Serbia during the period from January 2011 to December 2017. The study included all children with idiopathic and viral pericarditis treated in our hospital. A lot of patients were admitted in the Institute 24 hours after the onset of the disease from regional secondary hospitals and primary Healthcare centres. Patients with other aetiology of the acute pericarditis were excluded from our investigation.
Pericarditis was diagnosed based on the existence of 2 out of 4 criteria: 1) chest pain, 2) changes in the electrocardiogram, 3) elevated level of the acute inflammation parameters (erythrocytes sedimentation rate (ESR), C-reactive protein (CRP), number of leucocytes), and 4) echocardiographic visualization of pericardial effusion [10]. Recurrence of pericarditis (ROP) is diagnosed with a documented first episode of acute pericarditis (index attack), a symptom-free interval of 4-6 weeks or longer and evidence of subsequent recurrence of pericarditis. The following parameters were analysed: gender, age, acute inflammatory parameters, levels of specific cardiac enzymes and proteins, echocardiographic findings and therapeutic protocol. Bacteriological testing (blood, throat and pericardial fluid culture) was carried out to determine the aetiology of the disease. Viral aetiology was based on the detection of the viral nucleic acids of the most common cardiotropic viruses with polymerase chain reaction (PCR) technique in blood, pericardial fluid, pharyngeal swab and stool. Idiopathic pericarditis was defined as virus negative and without specific origin after diagnostic workup.
Myocardial involvement was revealed by increased level of specific cardiac enzymes and proteins with or without decreased left ventricle contractility registered by echocardiography, as well as a funding of oedema in cardiac magnetic resonance (CMR) [11]. A diagnosis of myopericarditis was established in patients with signs and symptoms of acute pericarditis with elevated biomarkers of cardiac injury in blood with normal function of the left ventricle. On the other hand, perimyocarditis was diagnosed in children with acute pericarditis, elevated cardiac biomarkers and segmental or global changes in left ventricle contractility [11].
For the treatment of the acute pericarditis non-steroidal antiinflammatory drugs (NSAID) and CS were administered. Ibuprofen was the first-choice drug and was given at a dose of 30-40 mg/kg. Corticosteroids (Prednisone 0.5 - 2 mg/kg) were introduced in all patients with myocardial affection and in patients with bigger pericardial effusion diameter. Colchicine was used in all patients with ROP (0.5 mg twice daily) after 2015 because our previous data showed that CS use in ROP increased recurrence rate and also a new multicentre cohort study in children and adolescents showed that colchicine halved the recurrence risk [9].
Medications were stopped slowly and sequentially. Corticosteroids were discontinued first and the dose was decreased after the normalization of clinical and laboratory parameters. The next step was discontinuation of NSAID, while colchicine was stopped after several months to one year.
Corticosteroid-dependence was defined by the need of a continuous use in order to prevent disease relapses with a past experience of a disease flare in at least 2 attempts of corticosteroid tapering [12].
We divided the patients in groups with respect to aetiology, myocardial involvement, treatment and ROP appearance. Basic (descriptive) statistics included mean values, standard deviations, median and interquartile rang of monitored parameters. Furthermore, the difference in the distribution of certain features among the tested groups was determined using the χ2 or Fisher’s test. The normality of the distribution of numerical variables had been tested using the Shapiro Wilk and Kolmogorov Smirnov tests. The comparison between the groups was done using the Student T-test, ANOVA, Mann-Whitney test and Kruskal Wallis test. Binominal and multinomial logistic regression analysis were used to explain the relationship between dependent binary variable and independent variables. All statistical methods were significant if p value was ≤0.05. Data processing was done using statistical software SPSS 25.0 for Windows 10.
Results
From January 2011 to December 2017, 68 patients with acute pericarditis were treated in our hospital. The study included 56 patients with idiopathic and viral index attack - 41 boys (73.2%) and 15 girls (26.8%). The mean age of patients at the time of the onset of acute pericarditis was 12.31 3.21 years. ROP occurred in 8 patients (4 after idiopathic and 4 after viral acute pericarditis) with mean age of 13.44 ± 2.69 years – 12 boys (75%) and 4 girls (25%). The first recurrence occurred in average period of 6.7 ± 6.3 months after acute disease. Total recorded number of recurrence was 39 (2; IQR: 1-6). Mean time of the achieved remission (period from the last episode of pericarditis to the end of monitoring) was 26.3 months, whereas the maximal period of 48 months without relapses was achieved in three patients.
Aetiology
The aetiology of acute pericarditis and ROP are shown in Table 1. Idiopathic acute pericarditis was significantly the most common in our patients. The patient with the greatest number of relapses had no specific genetic finding for Familial Mediterranean fever and was classified into the idiopathic recurrent pericarditis group. In the group of patients with viral aetiology of the disease the most frequent was Adeno- and Epstein-Barr virus infection. Patients with viral pericarditis had six times more chances for ROP (n = 4/6, 66.6%) than those with idiopathic pericarditis (n = 4/46, 9%) (p = 0.02; OR 6.0; 95% CI = 2.72 - 36.78) as well as higher median number of recurrence (Figure 1).
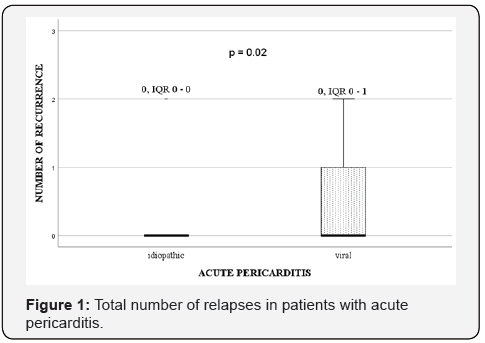
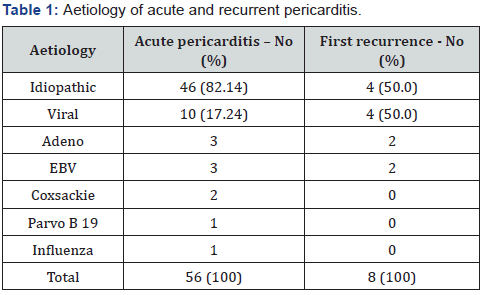
Abbreviations: EBV – Epstein – Barr virus, No – number
Multinomial logistic regression analysis has shown viral pericarditis (p = 0.01, OR 31.46; 95% CI 2.24 – 441.02), lack of concomitant myocardial affection (p = 0.03, OR 29.15; 95% CI = 1.39 – 609.37), CS use with NSID as treatment of acute pericarditis (p = 0.02, OR 29.02; 95% CI = 1.51 – 557.21) and ESR ≥ 50 mm/h (p = 0.03, OR 25.23; 95% CI 1.36 – 468.86) were independent risk factor for ROP (Table 2).
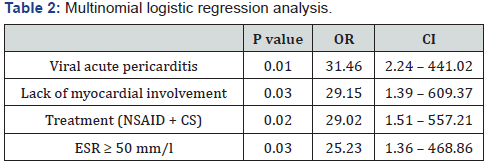
Abbreviations: NSAID – non steroid anti-inflammatory drug; CS – corticosteroids; ESR – erythrocyte sedimentation rate; OR – odds ratio; CI – confidence interval
Clinical findings
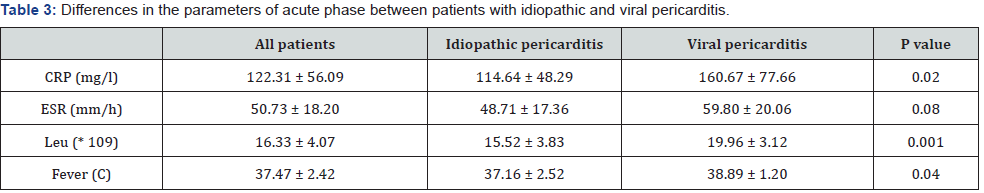
The difference between patients with idiopathic and viral index attack in laboratory parameters is presented in Table 3. At the admission mean effusion diameter was 10.52 ± 6.56 mm. Myocardial involvement was registered in 14 patients (8 patients with idiopathic and 6 with viral acute pericarditis). Perimyocarditis was established in 7/14 patients (4 children with idiopathic and 3 with viral index attack). Children with myocardial involvement had higher level of CRP than children with isolated pericardial affection (CRP - 160.50 ± 80.52 vs. 113.15 ± 41.14 mg/l, p = 0.008). Patients with perimyocarditis had higher value of CRP and ESR than those with myopericarditis (CRP 204.83 ± 73.60 vs. 105.30 ± 65.34 mg/l, p = 0.007; ESR 70.71 ± 15.68 vs. 46.43 ± 16.28 mm/h, p = 0.02). Also, CRP level, ESR and leucocytes (Leu) were statistically higher in patients with recurrent pericarditis than with acute disease (CRP -160.57 ± 83.63 vs. 116.62 ± 49.57 mg/l, p = 0.05; ESR - 72.0 ± 18.35 vs. 47.11 ± 15.67 mm/h, p < 0.001; Leu - 19.32 ± 5.30 vs. 15.82 ± 3.64 * 109/l, p = 0.02).
The average number of Leu was statistically significantly smaller in the first ROP than in index attack (p = 0.02).
Treatment
The treatment of acute pericarditis included either monotherapy with NSAID or the combination of NSAID and corticosteroids. An approximately equal number of patients received NSAID monotherapy (29/56 or 51.8%) and the combination of CS and NSAID (27/56 or 48.2%).
NSAID was often used in patients with idiopathic pericarditis (Table 4). Recurrence of the disease was frequently found in patients treated with the combination of NSAID and CS (6/27, 28.57 %) than in patients treated with NSAID only (2/29, 7.41 %) (p = 0.13). The trigger for recurrence was discontinuation of CS therapy in 5/8 patients. Median number of relapses in NSAID group was 0 (IQR: 0-0) and 0 (IQR: 0-1) in CS group (p = 0.08). Additionally, CS treatment was associated with higher recurrence rate (p = 0.03) and higher median number of relapses (p = 0.01) in children with idiopathic pericarditis, but none in patients with viral index attack (Table 3). CS use in patients with concomitant myocardial affection did not influence the ROP appearance (p = 0.38).
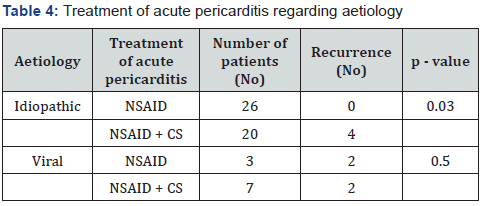
Abbreviations: NSAID – non steroid anti-inflammatory drug; CS – corticosteroids; No – number
Colchicine, NSAID and CS were used for treatment of the first ROP (Table 5). Among the eight patients with relapses, three did not have additional episodes. All patients without additional relapses were treated with the combination of colchicine and NSAID. Children with ROP treated with CS and NSAID had a bigger median number of additional relapses (5, IQR: 2 - 15) than those treated with colchicine and NSAID (0, IQR: 0 - 0.75) (p = 0.02). Additional relapses in CS patients appeared upon the discontinuation or reduction of steroids. Colchicine was added in therapy after several relapses in 2 patients treated with combination of NSAID and CS in the first recurrence. One of them had several ROPs after exclusion of colchicine and the other one has developed CS-depended pericarditis. Adverse events of colchicine (elevated level of transaminases and cytopenia) have not been registered during follow up period. Only two patients had nausea during the first week of drug intake.
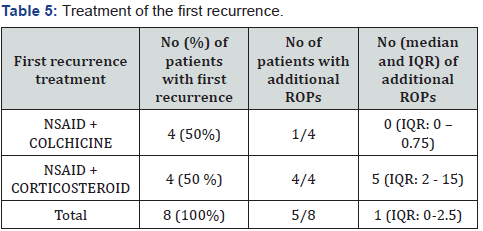
Abbreviations: NSAID – non steroid anti-inflammatory drug; No - number
Discussion
Aetiology
Thoracic chest pain has non-cardiac related origin in 97% of paediatrics patients. Regardless that thoracic pain is rarely associated with heart disease, pericarditis is the second cause of cardiac related chest pain in childhood [10]. In 70% of children, a specific aetiology of acute pericarditis cannot be detected and pericarditis is considered as idiopathic [4,7,13-15]. Idiopathic acute pericarditis is the most common in the United States and Western Europe [16]. Some investigators presumed that idiopathic index attack is post-viral [12,16], because the pathogenesis of idiopathic pericarditis is comparable to inflammatory diseases [3]. Brucato et al. [3] claimed that most cases of idiopathic pericarditis are viral in the index attacks, whereas recurrences are often due to too rapidly tapered drug regimen [3]. According to our study, laboratory analyses were statistically significantly different between children with viral and idiopathic index attack. The definitive diagnosis of putative viral agent requires the direct demonstration in the pericardial fluid or tissue but it is not routinely recommended [5]. The pericardiocentesis is routinely preformed in case of cardiac tamponed, purulent or neoplastic pericarditis [13]. On the other hand, it should be proposed as a second line of investigation when serological tests are negative and in the case of post-viral pericarditis, which does not resolve despite few weeks of anti-inflammatory treatment [17]. In our study, three patients underwent pericardiocentesis due to haemodynamic reasons. Molecular analysis (PCR) was preformed in those children and virus nucleic acids were uniformly negative. Gaaloul et al. [18] showed that PCR in blood and pericardial fluid were simultaneously positive in more than 60% of patients [18]. On the other hand, some authors claimed that detection of viral nucleic acid in pericardial fluid sample should be interpreted with caution when the agent has not been described previously [17].
Recurrent pericarditis is one of the complications of the disease. The etiopathogenesis of the recurrent pericarditis is presumed to be immune-mediated although 80-90% of cases remain idiopathic. Infectious, autoimmune and autoinflammatory pathways have been proposed as mechanisms involved. The interaction between aetiological agent, genetic factors and the immune system is responsible for the development of the disease. Then the same interactions with potential triggers may precipitate recurrences in predisposed individuals [4]. In our study, patients with viral acute pericarditis had six times bigger predisposition for recurrence. Also, those patients had higher level of acute phase reactants in the blood. It could be the aftermath of more extensive destruction of the pericardial tissue and expression of more antigens. Consequently, molecular mimicry or superantigens lead to autoinflammatory diseases. Recurrence might be developed due to re-infection [13].
Elevated CRP level was defined as one of the risk factors for unfavourable prognosis after acute pericarditis in adults [16]. In our study, the children with higher level of CRP frequently had ROP as well as children with higher ESR and Leu in blood. Also, according to our investigation ESR over 50 mm/h is an independent risk factor for recurrence.
Also, multinomial logistic regression analysis showed the lack of myocardial involvement and viral aetiology of the disease were independent risk factors for relapses. Earlier study in adult patients has also demonstrated that adult patients with myopericarditis or perimyocarditis had a lower recurrence rate than those with pericarditis only [11].
Treatment
Almost one half of our patients with acute pericarditis was treated with NSAID (ibuprofen), and the other half received combination of NSAID and CS. According to recommendations, patients were treated until clinical and laboratory findings (CRP) were normalized [19]. Some authors recommend that acute pericarditis can be treated with naproxen (10 mg/kg/day), and indomethacin (1-2 mg/kg/day) in severe cases [13]. Double blind study in single centre showed that ibuprofen and indomethacin had similar efficacy and both were more effective than placebo [20]. In our investigation only ibuprofen was used in the index attack. Corticosteroids are second line of therapy [10] and should be provided for connective tissue diseases, autoreactive or uremic pericarditis [21]. Imazio et al. administered CS in adulthood only in case of intolerance, contraindications or incomplete response to NSAID [11]. We introduced CS in more difficult cases, especially in patients with myocardial involvement with good result. Colchicine has been rarely administered in acute pericarditis in childhood. However, there is some evidence colchicine (together with NSAID) prevents relapse of the disease in more than 50% of adult patients if it is administrated for 3 months [13,22,23]. Mager et al. [24] concluded that the use of colchicine in addition to NSAID or aspirin for acute pericarditis in adulthood decreased recurrence rate by 37%, but without statistical significance [24].
Risks for unfavourable prognosis after acute pericarditis is defined in adults, but the definition of risks in childhood is lacking. According to Cremer at al. colchicine decreased the chance for recurrence. Quite the opposite, incomplete response to NSAID was related with unfavourable prognosis [22]. Missed viral aetiology may contribute to ROP, because corticosteroids could promote viral replication and thus prolong the treatment course [22]. In our study children with viral aetiology of the disease treated with NSAID and CS did not have higher recurrence rate than those treated only with NSAID (p = 0.63).
There are inconsistent data regarding prognostic role of CS treatment [22,24]. Few studies showed that CS treatment caries a risk for CS-dependent pericarditis [12], which is supported with our investigation. Corticosteroids can prevent symptoms and suppress inflammation, but their usage can increase the relapses rate two-fold [13,25,26]. In our study CS treatment increased chances for ROP 29.02 times. Our findings supported earlier study in adult population, which showed that usage of CS in treatment of pericarditis increases frequency of relapses. Also, pre-treatment with corticosteroids for the index attack and recurrent effusions may attenuate the efficacy of colchicine in preventing recurrent pericarditis [22, 27]. Also, according to a study by the Sackler Faculty of Medicine (Tel Aviv University) recurrence rate was growing when colchicine was administered in combination with CS for the treatment of acute pericarditis. However, CS is not indicated when CRP level is within normal limits [25]. Assolari et al. [28] suggested that CS should be included in case of autoimmune recurrent pericarditis and incomplete response to NSAID and colchicine, but only in combination with these drugs [28].
In our study, the first relapse of pericarditis was treated with NSAID and colchicine or CS and NSAID. All patients treated with CS and NSAID had additional ROPs over the period of 60 months and only one treated with colchicine and NSAID. Lower number of recurrence was demonstrated in groups of patients treated with colchicine than in group without colchicine (p = 0.02). Few investigations provided strong evidence for the favourable use of colchicine in adult patients with recurrent pericarditis, but data for paediatric patients are still missing [13,29]. Our results suggest that colchicine in combination with NSAID should be recommended as the treatment of choice for the first recurrence of idiopathic and viral pericarditis in childhood. Also, we showed that the treatment of recurrent pericarditis with colchicine was a safe and effective child therapy. However, Raatikka and al. concluded that colchicine did not decrease the number of relapses in children with recurrent pericarditis [25].
Anakinra can be used if recurrent pericarditis is refractory on NSAID, CS and colchicine. Role of the anakinra (IL-1 antagonist) is especially important in CS-dependent and colchicine-resistant pericarditis [12,22], antibody negative pericarditis followed by high levels of CRP, high fever, pleuropulmonary and systemic involvement [3]. Efficacy of anakinra was demonstrated in both adults and children, but in small series and with potential for recurrence after drug discontinuation [22].
The major limitations were collection of data from medical records and retrospective design. Also, the number of patients with recurrent pericarditis is insufficient for final conclusion, but we can suggest colchicine use in case of incomplete response to NSAID. Also, anakinra was not used in our study.
Independent risk factors for recurrence are viral aetiology, lack of concomitant myocardial affection, CS treatment of acute pericarditis and ESR ≥ 50 mm/h. Idiopathic index attack should be treated with NSAID, while CS use increases chances for ROP. On the other hand, CS use in patients with concomitant myocardial affection does not increase the risk for recurrence. However, CS should not be used in first ROP due to higher chances of additional relapses. Combination of colchicine and NSAID might be recommended as treatment of choice in patients with the first recurrence of pericarditis.
Each box shows the median and interquartile range (the box length). Outliers represent children with values more than 1.5 box lengths from the upper or lower edge of the box.
References
- Geggel RL (2004) Conditions leading to pediatric cardiology consultation in a tertiary academic hospital. Pediatrics 114(4): e409-e417.
- Dudzinski DM, Mak GS, Hung JW (2012) Pericardial diseases. Curr Probl Cardiol 37(3): 75-118.
- Brucato A, Valenti A, Maisch B (2017) Acute and Recurrent Pericarditis: Still
Idiopathic? J Am Coll Cardiol 69(22): 2775. - Imazio M (2014) Idiopathic recurrent pericarditis as an immune-mediated disease: current insights into pathogenesis and emerging treatment options. Expert Rev Clin Immunol 10(11): 1487-1492.
- Imazio M (2011) Pericarditis: Pathophysiology, Diagnosis, and Management. Curr Infect Dis Rep 13(4): 308-316.
- Ratnapalan S, Brown K, Benson L (2011) Children presenting with acute pericarditis to the emergency department. Pediatr Emerg Care 27(7): 581-585.
- Adler Y,Charron P, Imazio M, Badano L, Barón-Esquivias G, et al. (2015) 2015 ESC Guidelines for the diagnosis and management of pericardial diseases: The Task Force for the Diagnosis and Management of Pericardial Diseases of the European Society of Cardiology (ESC) Endorsed by: The European Association for Cardio-Thoracic Surgery (EACTS). Eur Heart J 36(42): 2921-2964.
- Alabed S, Pérez-Gaxiola G, Burls A (2016) Colchicine for children with pericarditis: systematic review of clinical studies. Arch Dis Child 101(10): 953-956.
- Imazio M, Brucato A, Pluymaekers N, Breda L, Calabri GB, et al. (2016) Recurrent pericarditis in children and adolescents: etiology, presentation, therapies, and out-comes. A multicenter cohort study. J Cardiovasc Med (Hagerstown)17(9): 707-712.
- Drossner DM, Hirsh DA, Sturm JJ, Mahle WT, Goo DJ, et al. (2011) Cardiac disease in pediatric patients presenting to a pediatric ED with chest pain. Am J Emerg Med 29(6): 632-638.
- Imazio M, Brucato A, Barbieri A, Ferroni F, Maestroni S, et al. (2013) Good prognosis for pericarditis with and without myocardial involvement: Results from multicentre prospective cohort study. Circulation 128(1): 42-49.
- Finetti M, Insalaco A, Cantarini L, Meini A, Breda L, et al. (2014) Long-Term Efficacy of Interleukin-1 Receptor Antagonist (Anakinra) in Corticosteroid-Dependent and Colchicine-Resistant Recurrent Pericarditis. Pediatr 164(6): 1425-1431.
- Gaspari S, Marsili M, Imazio M, Brucato A, Di Blasi Lo Cuccio C, et al. (2013) New insights in the pathogenesis and therapy of idiopathic recurrent pericarditis in children. Clin Exp Rheumatol 31(5): 788-794.
- Imazio M, Brucato A, Trinchero R, Spodick D, Adler Y (2009) Individualized therapy for
Expert Rev Cardiovasc Ther 7(8): 965-975. - Bolin EH, Tang X, Lang SM, Daily JA, Collins RT (2018) Characteristics of
Non-postoperative Pediatric Pericardial Effusion: A Multicenter
Retrospective Cohort Study from the Pediatric Health Information System
(PHIS). Pediatr Cardiol 39(2): 347-353. - Imazio M, Brucato A, Maestroni S, Cumetti D, Dominelli A, et al. (2011) Prevalence of C-reactive protein elevation and time course of normalization in acute pericarditis: implications for the diagnosis, therapy, and prognosis of pericarditis. Circulation 123(10): 1092-1097.
- Levy PY, Fournier PE, Charrel R, Metras D, Habib G, et al. (2006) Molecular analysis of pericardial fluid: a 7-year experience. Eur Heart J 27(16): 1942-1946.
- Gaaloul I, Riabi S, Harrath R, Hunter T, Hamda KB, et al. (2014) Coxsackievirus B detection in cases of myocarditis, myopericarditis, pericarditis and dilated cardiomyopathy in hospitalized patients. Mol Med Rep 10(6): 2811-2818.
- Horneffer PJ, Miller RH, Pearson TA, Rykiel MF, Reitz BA, et al. (1990) The effective treatment of postpericardiotomy syndrome after cardiac operations. A randomized placebo- controlled trial. J Thorac Cardiovasc Surg 100(2): 292-296.
- Maisch B, Seferovic PM, Ristic AD,Erbel R, Rienmüller R, et al. (2004) Task Force on the Diagnosis and Management of Pericardial Diseases of the European Society of Cardiology. Guidelines on the diagnosis and management of pericardial diseases executive summary. Eur Heart J 25(7): 587-610.
- Cremer PC, Kumar A, Kontzias A,Tan CD, Rodriguez ER, et al. (2016) Complicated Pericarditis: Understanding risk factors and pathophysiology to inform imaging and treatment. J Am Coll Cardiol 68(21): 2311-2328.
- Imazio M, Brucato A, Adler Y (2014) A randomized trial of colchicine for acute pericarditis. N Engl J Med 370(8): 781.
- Mager A, Talmor Y, Chezar Azzerad C, Iakobishvili Z, Porter A, et al. (2018) Does colchicine decrease the rate of recurrence of acute idiopathic pericarditis treated with glucocorticoids? J Cardiol 71(4): 409-413.
- Raatikka M, Pelkonen PM, Karjalainen J, Jokinen EV (2003) Recurrent pericarditis in children and adolescents: report of 15 cases. J Am Coll Cardiol 42(4): 759-764.
- Pepi M, Muratori M (2006) Echocardiography in the diagnosis and management of pericardial disease. J Cardiovasc Med (Hagerstown) 7(7): 533-544.
- Imazio M,Brucato A, Derosa FG, Lestuzzi C, Bombana E, et al. (2009) Aetiological diagnosis in acute and recurrent pericarditis: when and how. J Cardiovasc Med (Hagerstown) 10(3): 217-230.
- Artom G, Koren-Morag N, Spodick DH, Brucato A, Guindo J, et al. (2005) Pretreatment with corticosteroids attenuates the efficacy of colchicine in preventing recurrent pericarditis: a multi-centre all-case analysis. Eur Heart J 26(7): 723-727.
- Assolari A, Maestroni S, Cumetti D, Valenti A, Parisi F, et al. (2018) Clinical management and therapy of idiopathic recurrent pericarditis. Clinical Management Issues 12(1): 1-9.
- Imazio M, Belli R, Brucato A,Cemin R, Ferrua S, et al. (2014) Efficacy and safety of colchicine for treatment of multiple recurrences of pericarditis (CORP-2): a multicentre, double-blind, placebo-controlled, randomised trial. Lancet 383(9936): 2232-2237.






























