Recurrent Spontaneous Stent Fracture in a Case of Takayasu Arteritis Treated Successfully with Supera Stent System
Desabandhu vinayakumar, Sherief Sulaiman* and Chakanalil Govindan Sajeev
Department of cardiology, Government medical college, Calicut, Kerala, India
Submission: February 20, 2018; Published: April 11, 2018
*Corresponding author: Sherief Sulaiman, Department of cardiology, Government medical college, Calicut, Kerala, India, Tel: 919562044472; Email: sherifmd.18@gmail.com
How to cite this article: Desabandhu V, Sherief S, Chakanalil GS. Recurrent Spontaneous Stent Fracture in a Case of Takayasu Arteritis Treated Successfully with Supera StentSystem. J Cardiol & Cardiovasc Ther 2018; 10(1): 555778. DOI: 10.19080/JOCCT.2018.10.555778
Abstract
Purpose: To report a case of recurrent spontaneous left subclavian stent fracture in a patient with Takayasu arteritis (TA). The patient subsequently had recurrent in-stent restenosis (ISR) which was treated successfully with Supera peripheral stent system.
Case report: A middle aged female with Takayasu arteritis with symptomatic left subclavian long segment occlusion underwent percutaneous transluminal angioplasty with stenting. Recurrent intraprocedural stent fracture and deformity was noted. Recurrence of symptoms was later treated successfully with Supera peripheral stent system.
Conclusion: Takayasu arteritis with long segment occlusions may yield poorly to balloon dilatation and may result in stent deformity. Stents with high radial force, like Supera, may result in better outcomes.
Keywords: Takayasu arteritis; Stent fracture; Supera; PTA
Introduction
Percutaneous transluminal angioplasty (PTA) is commonly performed in patients with Takayasu arteritis (TA) with symptomatic stenotic vascular lesions. TA commonly involves subclavian artery with a reported incidence of about 76%. The arterial involvement is contiguous in about 81% of cases [1]. Significant subclavian artery (SCA) lesions can cause severe upper limb claudication with restriction of activities. Symptomatic patients frequently undergo revascularization procedures. Percutaneous angioplasty with stenting is commonly performed as an alternative to surgical revascularization in these patients. Though the procedural success rate and long term outcomes of percutaneous revascularization are favourable for short segment stenotic lesions, intervention in long segment disease and occlusive lesions are frequently complicated by vascular dissection and restenosis over long term. Subclavian stent fracture is an infrequently reported complication of subclavian stenting. Stent fracture is more likely to occur in stiff arteries as seen in TA. Fractured stent struts predispose to in situ thrombosis and reappearance of symptoms. Occasionally stent fracture leads to pseudoaneurysm formation and subsequent vascular embolism [2].
Case Report
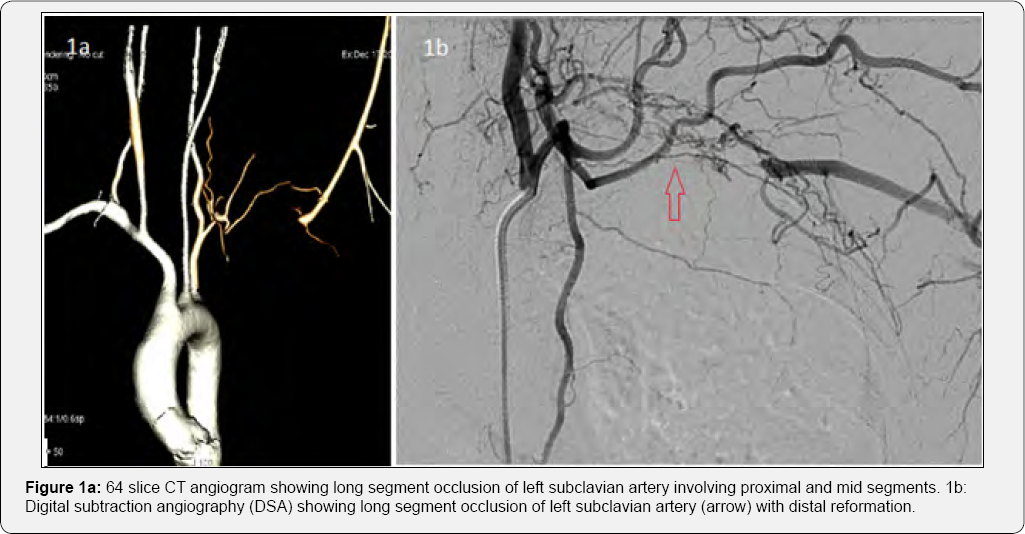
A 32 year old female presented with complaints of left upper limb (UL) claudication for a duration of 1 year with recent worsening of symptoms. The patient was evaluated before and was found to have feeble pulses in her left upper limb. Her CT angiogram revealed near total occlusion of second part of her left SCA. The acute phase reactants [Erythrocyte sedimentation rate (ESR) -94mm in first hour, C-Reactive protein (CRP)- 42mg/ dl] were found to be elevated. The patient was diagnosed to have type 1 Takayasu arteritis based on the angiographic involvement. The patient did not have any neurological manifestations. She was on maintenance dose of oral steroids. When she presented to our hospital, she did not have any constitutional symptoms. On examination, her left radial, brachial and subclavian pulses were absent without any ischemic ulcers or trophic changes in the limb. Her left arm BP was unrecordable while a BP of 100/76mmHg was recorded in her right arm. A 64 slice CT angiogram showed a long segment total occlusion of left SCA artery to a total length of about 7cm (Figure 1a). There was no evidence of active disease with the inflammatory markers (ESR, CRP) remaining within normal limits. An elective angioplasty with stenting of the occluded arteries was planned.
Technique
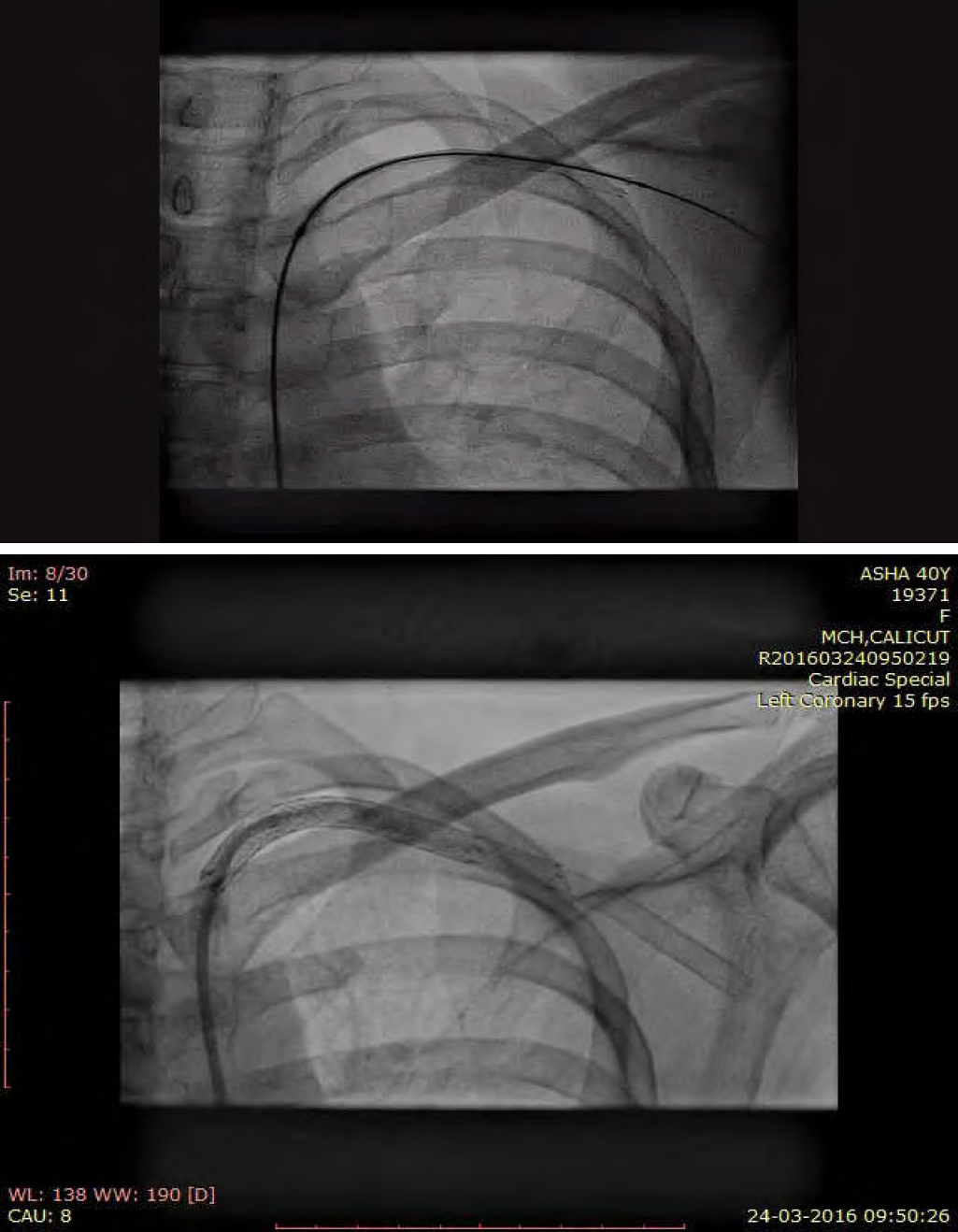
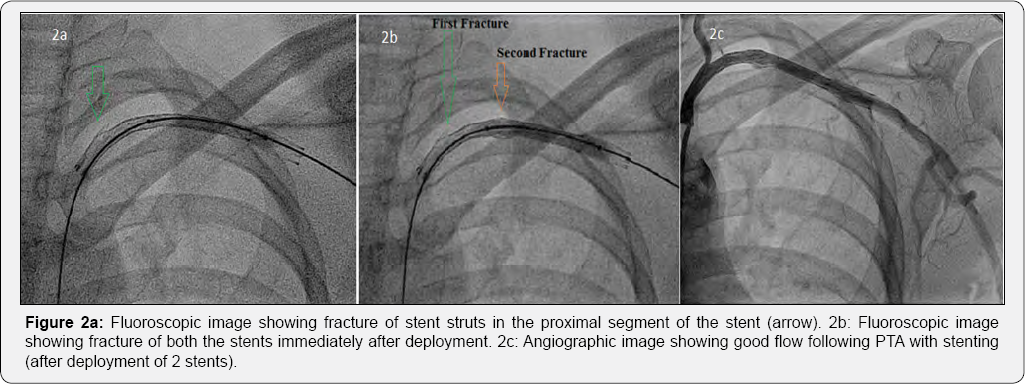
Under local infiltration anesthesia, right femoral artery was accessed percutaneously and secured with a 7F arterial sheath. A bolus of 5000IU of heparin was administered intravenously. Left subclavian artery (SCA) was selectively cannulated with a 6F Judkins right (JR) catheter. Selective SCA angiogram revealed a long segment total occlusion from second part of left SCA (Figure 1b). The lesion was crossed with a straight tip Terumo wire and a hydrophilic catheter (glidecath, Terumo interventional systems, NJ) was advanced over the wire. Injection distal to the occluded segment showed normal caliber vessels. The Terumo wire was reintroduced and advanced further to the distal left brachial artery followed by the glide catheter over the wire. The wire was exchanged with a stiff wire (Amplatz superstiff guide wire, Boston scientific, US) and the lesion was predilated with 6 x 40mm peripheral balloon catheter (Fox plus balloon, Abbott vascular, Switzerland) at 4atm. The lesion was hard and Digital subtraction angiography (DSA) after predilation showed inadequate dilatation of the diseased vessel. We decided to proceed with subclavian stenting. The 6 x 80mm self expanding stent (Absolute Pro, Abbott vascular, US) was tracked across the lesion and deployed. Immediately after deployment, we noticed the proximal portion of the stent sustained a fracture (type I stent fracture) (Figure 2a) (Video 1). The unyielded segments were post dilated with a 6 x 40mm peripheral balloon catheter (Fox plus balloon, Abbott vascular) at 8atm. A second self expanding stent (6 x 60mm Absolute Pro, Abbott vascular, US) was tracked into the previously stented segment across the fractured segment and deployed. Post dilatation was done with 6 x 40mm Fox plus balloon at 8atm. Immediately after post dilatation, the second stent also had a type I fracture in its mid segment (Figure 2b). However, the flow was re-established and there was no residual stenosis (Figure 2c). The procedure was completed and the patient was discharged after 48 hours with dual antiplatelets for one month followed by aspirin indefinitely. At 2 months follow up, the patient was asymptomatic. Her left UL pulses were palpable. Doppler evaluation showed triphasic flow in her left upper limb vessels. Check angiogram showed a patent stent. However, at 7 months after the procedure the patient returned with complaints of left UL claudication. Her left arm pulses were feeble. There was no evidence of reactivation of the disease. Diagnostic angiography revealed diffuse ISR of the SCA stent. She underwent balloon angioplasty with a low profile PTA balloon dilatation catheter (6x 40mm Advance balloon 14LP, Cook medical, US) at 6atm and was discharged. At 10 months follow up, she had recurrence of claudication. Doppler arterial study showed decreased flow across the SCA stent and monophasic flow in her left brachial artery. A 64 slice CT angiogram showed significant stenosis of the stented segment. The patient was not willing for surgical revascularization and was taken up for PTA with stenting. Selective injection of left SCA showed significant ISR (Figure 3a). The lesion was dilated with 6 x 80 Armada 35 balloon at 6atm. Thereafter, a 5 x 120mm Supera self expanding stent system (Abbott vascular, USA) was tracked and deployed across the lesion. Final injection showed good flow without any residual lesions (Figure 3b) (Video 2). At 15 months after stenting with Supera, the patient had no complaints of claudication. Her left UL pulses were well palpable. Doppler arterial study showed normal flow in her UL vessels (Figure 3c). Fluoroscopy showed no evidence of stent distortion. Her current medications include Aspirin 150mg OD, prednisolone 10mg OD.

Discussion
TA is highly resistant to endovascular treatment compared to atherosclerotic lesions. Percutaneous revascularization of SCA occlusions is technically more challenging compared to the excellent results with SCA stenosis. In a series of patients with TA undergoing PTA, the procedural success rate of total subclavian occlusion is 50% [3]. In the largest case series reported to date, the success rate of SCA stenting in occlusive disease is around 90% [4]. Since our patient had significant lifestyle limiting symptoms, revascularization procedure was necessary. Surgical revascularization of SCA is peformed by transthoracic surgical approach or extrathoracic bypass. In the current era, PTA may be favored over surgical intervention despite excellent long term outcomes with surgical revascularization [5]. Advantages of PTA over surgery include avoidance of general anesthesia, shorter healing times and length of hospital stay which can lead to significant cost savings per procedure [6]. However, the long term outcomes with subclavian stenting are less well defined. Several series have shown a higher incidence of restenosis (78%) with PTA especially in patients with TA [7]. After detailed discussion, our patient opted for PTA. Occlusive lesions in TA are commonly found during the quiescent phase and the vessels usually harbor dense scar tissue. These involved arteries are hard and stiff and are less likely to yield to balloon dilatation. Though stent fracture is not an uncommon complication, especially with calcified lesions, intraprocedural spontaneous recurrent stent fracture with self expanding stents is seldom reported. The various factors which may contribute to stent fractures include localised stiffness of the arterial wall, aggressive post-dilatation, the mechanical properties and solidity of the stent, post-deployment apposition defects and the length of the implanted stent. The fractured struts might embolise [8,9] or injure the vascular endothelium leading to in situ thrombosis, accelerated ISR or rarely perivascular hematoma and pseudoaneurysm formation [10]. The harder segments of the lesion might not yield adequately to balloon dilatation and the non-uniformity of the lesion post dilatation might cause a apposition defects on the stent leading to fracture. Whether the use of a less deformable stent like Supera in the first place could have prevented the strut fracture is unknown. Currently no large data on subclavian stenting with Supera exists. Balloon angioplasty alone has a little role to play in a case of ISR and it has a higher rate of restenosis compared to stenting. Since our patient had recurrence of symptoms within a short period of balloon angioplasty for ISR, we decided to stent the lesion, despite the fact that it would increase the metal load. Since our patient required stenting near the shoulder joint which has a wide range of movements, a stent with great flexibility was required. Supera is a self expanding interwoven nitinol stent used almost exclusively for superficial femoral or popliteal artery stenosis/occlusions. The experience of subclavian artery stenting with supera is limited. At 10 months after procedure, the patient is asymptomatic and the stent is patent. However, long term followup is needed to establish the superiority of Supera stent over other peripheral stent systems.
Conclusion
This case illustrates the uncommon occurrence of recurrent spontaneous stent fracture immediately following PTA with stenting in a case of TA. It also emphasizes the importance of cautious selection of patients for PTA based on lesion characteristics and the need for frequent followup following PTA. The assumption of superiority of Supera stent over other peripheral stents needs further data.
References
- Chung JW, Kim HC, Choi YH, Kim SJ, Lee W, et al. (2007) Patterns of aortic involvement in Takayasu arteritis and its clinical implications: evaluation with spiral computed tomography angiography. J Vasc Surg 45(5): 906-914.
- Math RS, Shankarappa RK, Dwarakaprasad R, Karur S, Bhairappa S, et al. (2011) Multiple fractures with pseudoaneurysm formation in a subclavian artery stent. Circulation 123: e602-e604.
- Sakaida H, Sakai N, Nagata I, Sakai H, Iihara K, et al. (2001) Stenting for the occlusive carotid and subclavian arteries in Takayasu arteritis. No Shinkei Geka 29(11): 1033-1041.
- Patel SN, White CJ, Collins TJ, Daniel GA, Jenkins JS, et al. (2008) Catheter-based treatment of the subclavian and in nominate arteries. Catheter Cardiovasc Interv 71(7): 963-968.
- Fields CE, Bower TC, Cooper LT, Hoskin T, Noel AA, et al. (2006) Takayasu's arteritis: Operative results and influence of disease activity. J Vasc Surg 43(1): 64-71.
- Takach TJ, Duncan JM, Livesay JJ, Krajcer Z, Cervera RD, et al. (2005) Brachiocephalic reconstruction II: operative and endovascular management of single-vessel disease. J Vasc Surg 42(1): 55-61.
- Maksimowicz-McKinnon K, Clark TM, Hoffman GS (2007) Limitations of therapy and a guarded prognosis in an American cohort of Takayasu arteritis patients. Arthritis Rheum 56(3): 1000-1009.
- Grasso C, Costanzo L, Tamburino C (2014) Subclavian transectional stent fracture and migration to the aortic carrefour: a case description of retrieval by snare system. Catheter Cardiovasc Interv 83(6): 10101013.
- Periard D, Haesler E, Hayoz D, Von Segesser LK, Qanadli SD (2008) Rupture and migration of an endovascular stent in the brachiocephalic trunk causing a vertebral steal syndrome. Cardiovasc Intervent Radiol 31(Suppl 2): S53-S56.
- Lee CE, Shaiful AY, Hanif H (2009) Subclavian Artery Stent Fracture. Med J Malaysia 64(4): 330-332.






























