Every Little Helps
Anupama Barua* and David J O’Regan
Department of Cardiac surgery, Leeds Teaching Hospitals NHS Trust, UK
Submission: March 09, 2017; Published: April 11, 2017
*Corresponding author: Anupama Barua, Department of Cardiac surgery, Leeds Teaching Hospitals NHS Trust, E floor, Jubilee Wing, Leeds General Infirmary, Great George Street, Leeds, LS1 3EX, UK, Tel:00447944982375; Email:dmcanupama@hotmail.com
How to cite this article: Anupama B, David J O. Every Little Helps. J Cardiol & Cardiovasc Ther 2017; 4(3): 555640. DOI:10.19080/JOCCT.2017.04.555640
Introduction
The National Health Service (NHS) is facing an unprecedented financial burden. We have to save up to £22 billion over next five years. Some savings can be obtained by efficient working but the majority can be achieved by working ‘smartly’ and reducing wastage. Our advances in medicine are putting greater pressure on our finances and therefore we need to be more focussed to ensure that the precious resources of the NHS are utilised as effectively as possible.
A large proportion of expenditure found in surgery is in the theatre environment [1]. Although implants, suture materials and cardiopulmonary bypass machine are the primary contributors to cardiac surgery costs, standardization of the surgical process provides an opportunity to decrease waste and improve efficiency. Cardiac surgeons can focus on the usage of instruments in theatre and assess the implementation of cost-effective measures to utilise the resources effectively. Several authors reported that across four different surgical specialties, the number of surgical instruments used per case ranged from 13-25% of the instruments contained on a surgical tray [2-4].
We found that a large proportion of instruments used in the cardiac surgery tray are consistently unused. Revising surgical trays with fewer instruments can result in significant cost savings [5]. The number of instruments on the surgical tray can be reduced by methodically investigating the requirements of individual instrument without compromising the fundamental principles of surgery or conflicting the surgeon’s individual preference. The objective of the study was to identify the usage of instruments in common cardiac surgical tray and time utilised by the team in associated with processing unused instruments.
Methods
Study design
An observation study was conducted on surgical instruments in coronary artery bypass graft (CABG) trays. Data was collected from CABG operations over a period of four months. Four consultants in the unit were included in the study. Four caseswere observed in total from each consultant’s theatre lists. The time was calculated to count the instruments by the scrub nurse. It was repeated three times for different grades of nurses.
Results
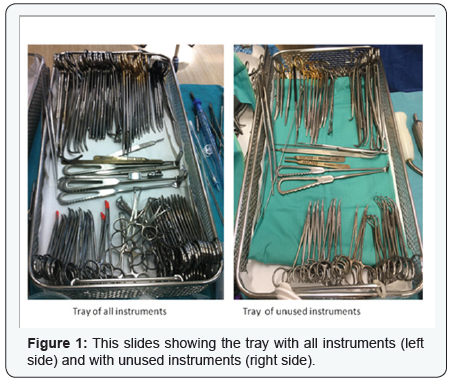
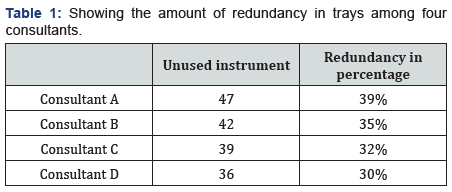
A coronary artery bypass graft tray contains 119 instruments (Figure 1). Forty seven instruments were unused by one consultant at the end of the procedure. The table shows the individual consultants’ usage of the instruments (Table 1).
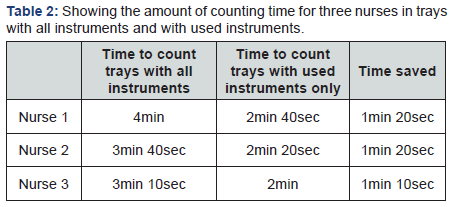
It took three to four minutes by the scrub nurse to calculate all instruments in the tray. After removing the unused instruments, the time was reduced to 2mins. It is worthwhile to mention that the scrub nurses count the number of instruments in every case three times (Table 2).
Discussion
From our experience, we found that instruments are rarely removed from the trays. More often instruments are added to the trays and that trays have become heavier over the years. One of the trays weighed approximately 6.4kg. After removal of redundant instruments, the weight was reduced to 5.2kg. Heavy trays, and the physical consequences of handling these trays may contribute to an increase in the dropout rate of employees.
Florijn EP [3] studied a dataset of 12 tray types in the Academic Medical Centre (AMC) in Amsterdam, and found that on average 21% of the instruments in the dataset were obsolete. In our study, overall utilisation of the tray was low with substantial redundancy ranges from 30-39%. Another consequence of sterilizing unused instruments is the deterioration of the quality of material. This leads to a shorter life of the instruments and quicker replacement of instruments, resulting in higher costs. Less utilised instruments can be identified and replaced by a process of individual packing to meet surgeon specific needs. Single instrument packing can be employed for infrequently used instruments with a shelf life of 96 weeks. It will reduce the unnecessary processing of instruments, improve employee safety and cost effective practice [6]. Removal of redundant instruments can be ensured by effective input and instruction from surgeons and scrub nurses. In addition to individual trays, specific surgical trays (e.g. sternotomy open and closure tray) could be considered for review in order to eliminate unwanted instruments with potential savings of time, resources and cutting wastage.
It is well established that excess time spent counting instruments significantly compromises case progression in the theatre [7]. Time savings should be considered from the starting point of the cleaning, disinfecting and counting of instruments in the sterilisation unit [7,8]. Furthermore, autoclaving for smaller trays results in reduced sterilisation time. This improves the total turnover time of trays. There is reduced chance of missing instruments when fewer instruments are in the tray. We have to consider human error in this sterilisation process [9]. Stockert et al. [10] noted that there was a 49% error rate for trays with greater than 40 instruments contrasted against an error rate of 13% for trays with 40 instruments or less.
Van Meter et al. [4] have reported that excess processing cost can be saved by removing unwanted instruments from surgical tray [5]. We estimated that the cost for sterilisation of unused instruments per tray is £3.00. Average 17,630 coronary artery bypass procedure was done in 2013 in UK, we can save upto17,630 X £3.00 =£52,890 [7]. If we apply similar principle in all cardiac surgery in 2013, the potential savings could be 36,134X £3.00=£108,402 in 2013 [11].
This simple concept can be applied to all surgical specialities. Here, we are looking for marginal gain. This small step in waste reduction and cost saving measures can make a considerable impact in the theatre management. This humble challenge should not be underestimated and can be translated into significant cost savings in the long term.
Limitations
Data was collected on only one surgical procedure in cardiac surgery. Usually, instruments are variable in different cases. The cost of individual packing of single instruments was not measured and compared with the set of instruments in the tray. We did not visit the sterilization suit and were not able to count the time spent to process the instruments over there.
Conclusion
This small study focuses on the advantages of small changes to reduce the cost and also to promote competency for utilising limited funding. Further research is warranted to investigate the efficiency of surgical processes for effective utilisation of precious resources in NHS.
References
- Siddharth V, Kumar S, Vij A, Gupta SK (2015) Cost Analysis of Operation Theatre Services at an Apex Tertiary Care Trauma Centre of India. Indian J Surg 77(Suppl 2): 530-535.
- Chin CJ, Sowerby LJ, John-Baptiste A, Rotenberg BW (2014) Reducing otolaryngology surgical inefficiency via assessment of tray redundancy. J Otolaryngol Head Neck Surg 43(1): 46.
- Florijn EP (2008) Optimisation of the distribution of surgical instruments over trays. Cost effectiveness and quality improvement of an operating theatre. Master thesis Industrial engineering and management. Logistical processes in healthcare. University of Twente, Enschede, The Netherlands.
- Van Meter MM, Adam RA (2016) Costs associated with instrument sterilization in gynecologic surgery. Am J Obstet Gynecol 215(5): 652.
- Lunardini D, Arington R, Canacari EG, Gamboa K, Wagner K, et al. (2014) Lean principles to optimize instrument utilization for spine surgery in an academic medical center: an opportunity to standardize, cut costs, and build a culture of improvement. Spine 39(20): 1714- 1717.
- Mhlaba JM, Stockert EW, Coronel M, Langerman AJ (2015) Surgical instrumentation: the true cost of instrument trays and a potential strategy for optimization. Journal of Hospital Administration 4(6): 82- 88.
- Kanich DG, Byrd JR (1996) How to increase efficiency in the operating room. Surgical Clinics 76(1): 161-173.
- Weinbroum AA, Ekstein P, Ezri T (2003) Efficiency of the operating room suite. Am J Surg 185(3): 244-250.
- Reason J (2000) Human error: models and management. BMJ 320(7237): 768-770.
- Stockert EW, Langerman A (2014) Assessing the magnitude and costs of intraoperative inefficiencies attributable to surgical instrument trays. J Am Coll Surg 219(4): 646-655.
- SCTS Blue Book Online - Cardiac Surgery Audit Data






























