Aortopulmonary Window Closure Using the Amplatzer ASD Device
Ghaderian Mehdi1 and Hosseinzadeh Mohsen2*
1Assistant professor of Pediatric Cardiology, Department of Pediatric Cardiology, Isfahan University of Medical Sciences, Iran
2Department of pediatric cardiology, Isfahan University of Medical Sciences, Isfahan, Iran
Submission: December 22, 2016; Published: January 09, 2017
*Corresponding author: Hosseinzadeh Mohsen, Department of pediatric cardiology, Isfahan University of Medical Sciences, Isfahan, Iran, Email: drmhz.ped@gmail.com
How to cite this article: Ghaderian M, Hosseinzadeh M. Aortopulmonary Window Closure Using the Amplatzer ASD Device. J Cardiol & Cardiovasc Ther 2017; 2(5): 555598.. DOI: 10.19080/JOCCT.2017.02.555598
Abstract
One of the relatively rare cardiac malformations is aortopulmonary window. We report a 12-year-old boy with a mod size aortopulmonary window who presented with an asymptomatic cardiac murmur and in whom catheter device closure was successfully developed with an Amplatzer ASD Cardio fix.
Keywords: Aortopulmonary window; catheter device occlusion; Amplatzer ASD closure
Introduction
One of the relatively rare cardiac malformations is aortopulmonary window (APW), or aortopulmonary septal defect that accounts for 0.1% to 0.6% of all cases of congenital heart disease. It was first described by Elliotson nearly two centuries ago [1,2]. This abnormality is characterized by an malformed communication between the ascending aorta and the pulmonary shaft or the right pulmonary artery [3]. The clinical manifestations of APW are not characteristic, but many of patients have the futures of a large left to right shunt. The cases with large APW usually have symptoms and signs of pulmonary hypertension and congestive heart failure in the neonatal period. Severe hypertension of pulmonary vascularity can occur in the first months of life [4].
Closure of the aortopulmonary window defect in all patients is essential as soon as possible. The classical treatment of the defect is surgical closure and the median sternotomy and cardiopulmonary bypass was recommending [2]. Current outcomes of early repair of APW are excellent, including infants with complex associated cardiac lesions [5]. Several case reports have been demonstrated recently about transcatheter device occlusion of both native and postoperative residual defects. Nowadays, several suitable devices include Amplatzer Duct Occluder I and II, Amplatzer Septal Occluder or ventricular septal defect closure device are used [6]. We report the use of Amplatzer ASD Cardiofixdevice, which was originally designed for closure of atrial septal defect, for closure of aortopulmonary window.
Case Report
A 12-year-old boy presented with an asymptomatic cardiac murmur. He has no cyanosis with full pulses, normal S1, loud S2 and a continuous murmur grade 3/6 in upper left sternal border. He had a bounding pulse in physical exam. Chest x-ray showed mild cardiomegaly and increased peripheral blood flow. Echocardiography confirmed a moderate aortopulmonary window and mild pulmonary hypertension. There were no associated cardiac anomalies. Right and left cardiac catheterizations were performed under generalized anesthesia and standard protocol. The course of arterial catheter passed from femoral artery into descending aorta, ascending aorta and then into pulmonary artery via APW respectively.
At catheterization he had mild increased pulmonary arterial pressures (50/40 mmHg, mean = 45 mmHg) and the QP/QS was 2.5. Aorta angiogram showed opacification of pulmonary artery from an APW. Sizing of APW was performed by 20*40mm Numed- Boston USA sizing balloon that showed a moderate aortopulmonary window, 7mm in size in the ascending aorta, away from the aortic valve and coronary arteries (Figure 1).

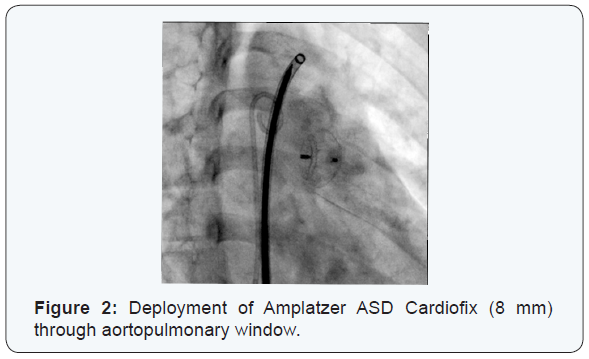
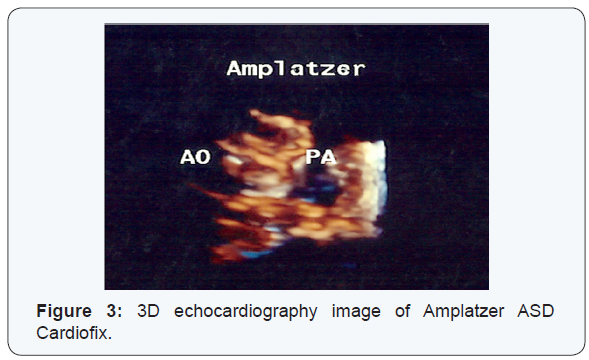
After passing delivery system through APW, Amplatzer ASD Cardiofix (8 mm) was deployed, successfully (Figure 2 & 3). After them mean PA pressure was decreased from 45 to 24 mmHg. Echocardiography and ascending aorta angiogram after deployment of device showed no residual APW. He was discharged from hospital after 2 days. At follow-up 2years later, the serial echocardiogram showed no leak through the window.
Discussion
In large aortopulmonary windows, for anatomical reason, the choice of treatment is surgery, but there are essential risks. So, other lower risk procedures should be considered [6]. The first using of transcatheter closure of an APW was described by Stamato et al. They using a modified double umbrella occlude system in a 3 years old child [7]. Tulloh and Rigby also using transcatheter umbrella closure of an APW in a child with 6-month-old by a Rash kind double umbrella system [8] Other investigators also describe trans catheter closure of APW by using an Amplatzer Duct Occlude device [6,9-11]..
The device selection may be a preference of operator and also related to the space available in the main pulmonary artery, so the devices with two disks are probably better than the device with a disk only on the aortic side. Yet, Amplatzer Duct Occluder (ADO I) has been used to closure of APW, although the device come out into the pulmonary artery. Alternatively, the Amplatzer muscular ventricular septal defect occludes or ASO may be better than ADO, or devices with similarly shaped available from several other manufacturers [3].
Because of the device design, the device may be deployed from the aortic side hence; a small delivery catheter is required for it. Noonan and et.al believe that in young children, the venous approach is preferable [6]. PremSekar, R et.al showed that the use of the internal jugular vein can be an alternative approach to device closure of APW in patients with occluded femoral veins [12]. Our patient was older child who had moderate size APW accordingly, we preferred to use the Amplatzer ASD device (size: 8 mm) and deployed it from the aortic side.
Conclusion
Most patients with APW develop severe clinical symptoms such as congestive heart failure or pulmonary hypertension. Early surgical closure or device employment is indicated as soon as the diagnosis is established. Nonsurgical technique is possible for closure of small aortopulmonary windows, and the range of Amplatzer devices exhibit the several options for operators.
References
- Soares AM, Atik E, Cortêz TM, Albuquerque AM, Castro CP, et al. (1999) Aortopulmonary window. Clinical and surgical assessment of 18 cases. Arq Bras Cardiol 73(1): 59-74.
- Taggart NW, Qureshi MY (2016) Patient ductus arterosus and aortopulmonary window. Moss and Adams’Heart Disease In Infants, Children, and Adolescents Including the Fetus and Young Adult. 1. 9 ed. Philadelphia: Lippincott Williams & Wilkins 803-819.
- Qureshi SA (2015) Patent ductus arteriosus (PDA): Aortopulmonary window. In: Sievert H, Qureshi SA, Wilson N, Hijazi ZM, editors. Interventions in Structural, Valvular, and Congenital Heart Disease. 2 ed. Boca Raton, London, New York: Taylor & Francis Group 637-644.
- Mehdi Ghaderian (2012) Aortopulmonary window in infants. Heart views 13(3): 103-106.
- Alsoufi B, Schlosser B, McCracken C, Kogon B, Kanter K, et al. (2016) Current Outcomes of Surgical Management of Aortopulmonary Window and Associated Cardiac Lesions. Ann Thorac Surg 102(2): 608-614.
- Noonan PM, Desai T, Degiovanni JV (2013) Closure of an aortopulmonary window using the Amplatzer Duct Occluder II. Pediatr Cardiol 34(3): 712-714.
- Stamato T, Benson LN, Smallhorn JF, Freedom RM (1995) Transcatheter closure of an aortopulmonary window with a modified double umbrella occluder system. Cathet Cardiovasc Diagn 35(2): 165-167.
- Tulloh RM, Rigby ML (1997) Transcatheter umbrella closure of aortopulmonary window. Heart 77(5): 479-480.
- Atiq M, Rashid N, Kazmi KA, Qureshi SA (2003) Closure of aortopulmonary window with amplatzer duct occluder device. Pediatr Cardiol 24(3): 298-299.
- Naik GD, Chandra VS, Shenoy A, Isaac BC, Shetty GG, et al. (2003) Transcatheter closure of aortopulmonary window using Amplatzer device. Catheter Cardiovasc Interv 59(3): 402-405.
- Sangeetha Viswanathan, Balu Vaidyanathan, R Krishna Kumar (2007) Transcatheter closure of the aortopulmonary window in a symptomatic infant using the Amplatzer ductal occluder. Heart 93(12): 1519.
- R. Prem Sekar, P.R. Bhima Shankar, Kotturathu Mamman Cherian (2012) Transcatheter closure of a residual aortopulmonary window through internal jugular vein access. Indian Heart J 64(5): 521-523.






























