Transthoracic Echocardiographic Guidance for Percutaneous Patent Ductus Arteriosus Closure in Pediatric Patients
Mashail Binobaidan*, Mohammed Al Issa, Ahmad Alonazi and Jassim Abdulhameed
Department of Pediatric cardiology division, Prince Sultan Cardiac Center, Riyadh, Saudi Arabia
Submission: December 07, 2016; Published: December 15, 2016
*Corresponding author: Mashail Binobaidan, Prince Sultan Cardiac Center, Riyadh, Saudi Arabia, King Abdulaziz Street, P.O Box 396162, Riyadh 11375, Saudi Arabia
How to cite this article: Mashail B, Mohammed A I, Ahmad A, Jassim A. Transthoracic Echocardiographic Guidance for Percutaneous Patent Ductus Arteriosus Closure in Pediatric Patients. J Cardiol & Cardiovasc Ther 2016; 2(3): 555590. DOI: 10.19080/JOCCT.2016.02.555590
Abstract
Background:: Patent ductus arteriosus (PDA) is a common congenital cardiac disorder; the treatment of choice is fluoroscopy-guided transcatheter occlusion. Closure of PDA under transesophageal echocardiography (TEE) with Trans aortic imaging guidance was studied in adult patients. In pediatric patients, transthoracic echocardiography (TTE) provides excellent images for PDA and may replace fluoroscopy as an imaging tool to guide PDA closure.
Purpose: The goal was to study the feasibility of device closure under TTE guidance in patients who are not candidates for transfer to the cardiac catheterization laboratory or in those with contraindications for contrast and/or radiation applications.
Methods: Eighteen patients (7 males, median age 7 months, median weight 8 kg) underwent TTE guidance device closure of PDA from July 2013 to May 2015. Conscious sedation was used in 17 patients-one patient was sick and ventilated in the intensive care unit. The antegrade approach with partial fluoroscopy was used in eight patients, and the retrograde approach without fluoroscopy in 10 patients.
Results: The median procedure time was 30 minutes (13-45 min). The median fluoroscopy time was 2.2 minutes (0-13 min). The PDA size was small in 13 cases and moderate in five subjects. Immediate successful closure was achieved in 17 patients. One patient had device emobilization after the release of the device during the retrograde approach. The device was successfully retrieved under fluoroscopy.
Conclusion: Transcatheter PDA device closure under TTE guidance is feasible and recommended in selected patients and can replace fluoroscopy.
Keywords: Transthoracic echocardiography; Patent ductus arteriosus; Fluoroscopy; Pediatric; Congenital; Device closure
Abbreviations: PDA: Patent Ductus Arteriosus; TEE: Transesophageal Echocardiography; TTE: Transthoracic Echocardiography; AVP2: Amplatzer Vascular Plug type 2; MPA: Main Pulmonary Artery; ADOS: Amplatzer Duct Occluder additional Size; ADO II: Amplatzer Duct Occluder type II
Introduction
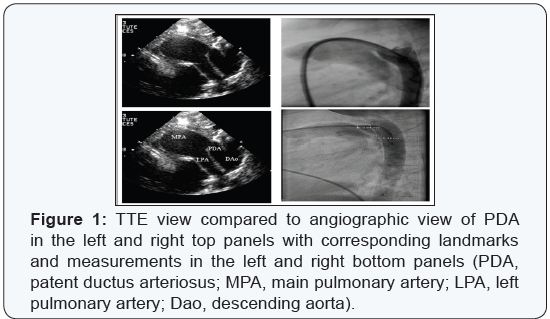
Transcatheter closure of patent ductus arteriosus (PDA) under fluoroscopy guidance is the method of choice in pediatric subjects over the last four decades (Figure 1). However, there is an urgent need for alternative imaging methods in patients with contraindications to fluoroscopy.
Transthoracic echocardiography (TTE) is already used for guidance of secudum atrial septal defect closure [1,2]. In addition, this method was successfully used to guide many other procedures. This makes it an attractive tool, especially in pediatric patients, where TTE provides excellent images for PDA (Figure 1).
In adult patients with PDA, transesophageal echocardiography (TEE) with transaortic imaging is an important alternative and offers good image quality [3]. However, it is disfavored in pediatric patients because of the need for general anesthesia. Nevertheless, a few reports described TTE as a tool to monitor PDA closure before, during, and after the procedure [4-9]. We describe our experience in using TTE to guide the transcatheter closure of PDA with and without fluoroscopy.
Methods
Patient selection
A total of 18 patients (7 males) underwent TTE guidance device closure of PDA between July 2013 and May 2015 at Prince Sultan Cardiac Center. The median age of patients was 7 months (range 4-23 months) and the median weight was 8 kg (range 3.2–11 kg). All patients received a detailed echocardiographic evaluation of the duct morphology as part of the institutional protocol using broadband 3-8 MHZ (AEPEC, Philips, USA/ Holland) and 5-12 MHZ frequency transducers. The duct diameter was measured in a high parasternal long-axial view at the insertion of PDA to the pulmonary artery. The measurements were based on zoomed two-dimensional echocardiographic images and not on the color Doppler jets width. Because this measurement varies with different phases of the cardiac cycle, the maximum measurement diameter at the level of pulmonary artery insertion was reported as the narrowest diameter (duct diameter) and the widest diameter at the aortic side was reported as ampulla and the length of the duct is the distance between ampulla and PDA-MPA junction (Figures 2 ).
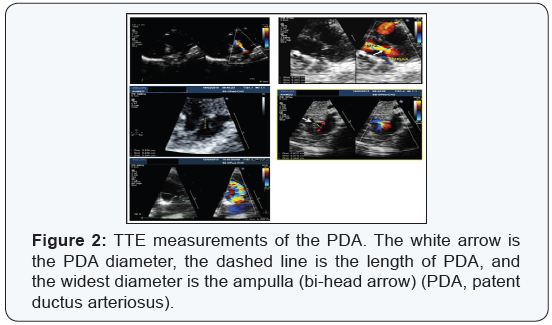
The ductal ampulla or the diverticulum was defined in the high parasternal long-axis view or in the supra-sternal longaxis view. The ductal ampulla was considered adequate if its maximal dimension in the long axis view was greater than twice the measured ductal diameter. Careful 2-D and Doppler imaging of the pulmonary artery branch origins was also routinely performed. Multiple and repeated measurements were collected and the most concordant value was reported.
Antegrade approach for transcatheter PDA closure
In the cardiac catheter laboratory, the femoral vein (in seven patients) and the jugular vein (in one patient) were accessed with a 5F sheath. The end and side hole catheter was used to check the hemodynamics and to approach the PDA under fluoroscopy guidance, followed by crossing the PDA via a soft 0.035-inch exchange length Terumo wire (Terumo Corp., Tokyo, Japan). The catheter was then replaced with a long sheath (size 5 or 6F). The devices were then deployed under TTE guidance (Figure 3).
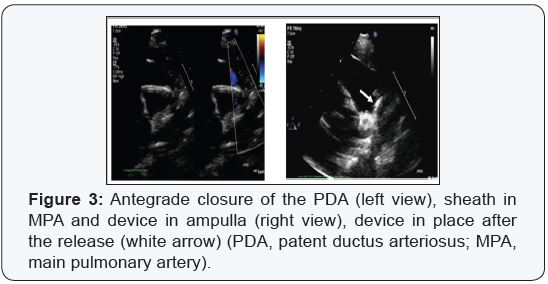
We used the following devices: Amplatzer duct occluder type I (ADO I, ST. Jude Medical corp. , St. Paul, Minnesota, USA ), Occlutech (Occlutech, Jena, Germany), and Amplatzer vascular plug type 2 (AVP2, ST. Jude Medical corp. , St.Paul, Minnesota. The disc was released in the ampulla and then pulled until the rest of the device seen in the main pulmonary artery (MPA) under 2D and color doppler transthoracic echocardiography guidance, followed by complete release of the device with no need for contrast angiography or arterial access.
Retrograde approach for transcatheter PDA closure
In the catheter laboratory, the femoral artery was accessed in 10 patients who have small to moderate PDA using a 4F short sheath to cross the PDA via a 4F end hole catheter. A 4F long sheath then has replaced the catheter over a soft 0.035 exchange length Terumo wire (Terumo Corp., Tokyou, Japan). followed by device implantation. We used the following devices: Amplatzer duct occluder additional size (ADOS, ST. Jude Medical corp. , St. Paul, Minnesota, USA), Amplatzer duct occluder type II (ADO II, ST. Jude Medical corp. , St. Paul, Minnesota, USA ), and AVP2 ( ST. Jude Medical corp. , St. Paul, Minnesota, USA ).

This procedure consists of the release of the first disc in the main pulmonary artery, followed by pulling the sheath with the device toward the PDA and aorta. The disc is then fixed against the PDA and the rest of the device is released in the ampulla. This was visualized with color Doppler ultrasonography, and a waggle movement was applied to ensure device stability. The device position and shape was reassessed after the release-all under TTE guidance (Figure 4). The contrast angiography or fluoroscopy was not necessary. However, a femoral venous line was secured with a 20G needle (Vygon, Aachen, Germany) for the emergencies.
Device Embolization
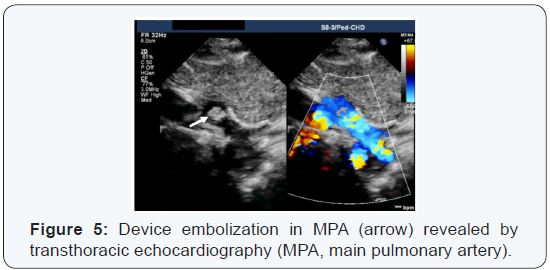
One patient was assessed before the procedure for a retrograde approach with the PDA device; the pre- and intraprocedural measurements were consistent with the use of a 4×4 ADOS. However, after the device release, it was embolized immediately in the main pulmonary artery (Figure 5). Therefore, fluoroscopy was used to define the exact location of the device. A short sheath was inserted in the femoral vein, which was then replaced with a long sheath for the device retrieval. The procedure was very successful and uneventful. Finally, a 6×4 ADO I was used for ante grade closure of the PDA under fluoroscopy guidance (total fluoroscopy time was 13 min).
Results
All procedures were performed under conscious sedation except for one patient who was ventilated in the intensive care unit before the procedure. Two patients had chronic renal impairment and two patients showed the relapse of leukemia. The median procedure time was 30 min (range 13-45 min) and median fluoroscopy time was 2.2 min (range 0-3 min), except for one patient, in whom the device embolized (this consumed 13 min because of the retrieval of the device and re-implantation of a second one under fluoroscopy guidance). We found small PDAs in 13 subjects and moderate PDAs in five. Immediate successful closure was achieved in all subjects except one. Complete closure was documented by color Doppler ultrasonography on the second day before discharge (patients’ characteristics were shown in the following Table 1).
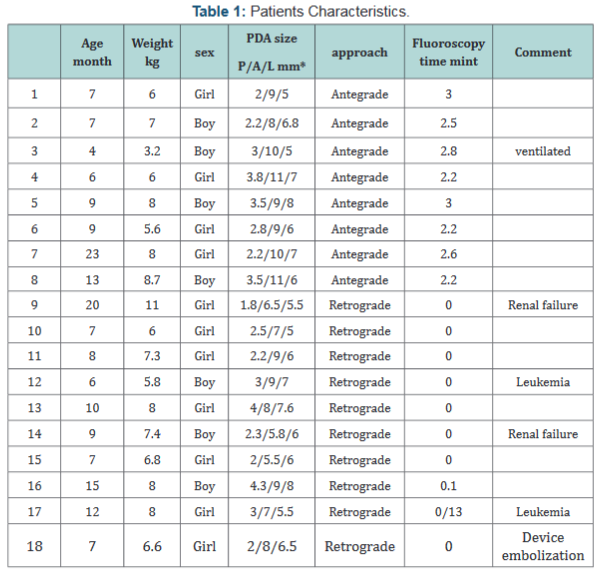
Different devices were used according to the approach, size, and shape of the PDA. However, the ADO I and ADO II, Occlutech duct occluder device and AVP2 were mainly used with the antegrade approach. The ADOS, ADO II, and AVP2 were used in the retrograde approach, because of the availability of two discs in these devices, which allow the release of one disc in the MPA and the other in the ampulla. No immediate or early complications were found in 17 patients.
Discussion
Transcatheter closure of PDA is routinely performed under fluoroscopic guidance. However, alternative methods of guidance are recognized and applied worldwide. The use of TTE to guide atrial septal defect secundum closure suggests that it can also be used in other congenital heart defects [1,2]. The 3-D echocardiography was more accurate than 2-D echocardiography in determining the length and the location of the PDA ampulla. However, the use of 3-D echocardiography to assess the small vascular structures (e.g., PDA) in children with rapid heart rates are still of limited clinical value [10]. TEE can be an alternative with good image quality, but it is primary applied in adult population and animals. It is disfavored in pediatric populations because of the need for general anesthesia [3]. TEE monitoring played an important role in PDA ligation and assessed residual blood flow. It also monitored the pulmonary artery and the aortic valve [11].
Retrograde imaging with the 8F intracardiac echocardiographic catheter (Acu Nav, Acuson-Siemens, Mountain View, CA, USA) from the femoral artery into the descending aorta can be used for anatomical characterization and sizing of the PDA in adults [12]. Transaortic phased-array imaging can effectively assist the percutaneous PDA device closure. This may reduce procedure time, limit radiation exposure, and lower the amount of contrast agent administered [13]. In pediatric populations, transcatheter PDA closure under fluoroscopy guidance has been preferred for the last 40 years [14]. However, a study reported in 2007 the use of TTE for transcatheter PDA closurein neonates [4]. The success of this method [5] suggested that it could replace fluoroscopy and guide this procedure at least in some situations when the patients are too sick for the cardiac catheter laboratory, are at high risk, or have contraindications for contrast angiography or / and radiation [6-8].
Baykan et al. [9] described percutaneous PDA closure via ADO I using the femoral venous access without the need for arterial access or contrast angiography. They deployed the devices under TTE guidance, and this technique can be used in patients whose femoral artery could not be accessed or if the access is impossible / contraindicated [9]. In our study, we used the same classification of PDA size as reported by Rao [14]. We used both femoral veins and arteries to access the PDA with different approaches as described above. We found that TTE images were very helpful in guiding the device deployment. With more experience, we found that even the course of the catheter and the sheath could be visualized via TTE. The challenges in visualizing the catheter course inside the cardiac structure by TTE motivated our use of arterial access to cross the PDA via a straight course from the aorta.
The TTE-based PDA measurements (diameter, length, and ampulla) were feasible. Previous fluoroscopy procedures showed that TTE is largely comparable to angiography measurements with a difference of 0.5-0.8 mm. We used the average of multiple measurements from different images in the presence of at least two image readers during the procedure. We used devices that were 2 mm larger than the maximum diameter of the narrowest end of PDA, at the opening into the MPA.
It is difficult to explain the reasons for device embolization. However retrospective review of the patient’s images suggests some theories behind the embolization:
- The second disc of the device might be partially released in the MPA. Because it is short arterial duct it was difficult to realize the protrusion of the second disc.
- The PDA size was larger than what we measured.
- There is possibility that the PDA is a stretchable type and the size might be changed with the catheter and sheath manipulation.
- It might be that both discs were released in the MPA due to the presence of short PDA. Howevers, we managed to retrieve the device and close the PDA with a larger device under fluoroscopy guidance, which made the procedure longer.
This is the limitation for the success of the procedure in the current time.
Conclusion
Transcatheter PDA closure guided by TTE is a feasible and very promising method as an alternative to fluoroscopy. In the future, certain patients may be helped with this approach. More clinical experience will further improve the technique and minimize the embolization rate. While visualization of the embolized device is feasible, the retrieval of the device needs fluoroscopy at least in the present time.
Acknowledgment
I would like to thank all the pediatric catheter laboratory team in PSCC for their assistance and contribution in the team work to provide the best care to the patients.
Ethical Standards
All study participants provided informed consent, and the study design was approved by the appropriate ethics review board.
References
- Gui-Shuang Li, Hai-De Li, Jie Yang, Wen-Quan Zhang, Zong-Shen Hou, et al. (2012) Feasibility and safety of transthoracic echocardiographyguided transcatheter closure of atrial septal defects with deficient superior-anterior rims. PLoS ONE 7(12): e51117.
- Bartakian S, El-Said HG, Printz B, Moore JW (2013) Prospective randomized trial of transthoracic echocardiography versus transesophageal echocardiography for assessment and guidance of transcatheter closure of atrial septal defects in children using the Amplatzer septal occluder. JACC Cardiovasc Interv 6(9): 974-980.
- Porciello F, Caivano D, Giorgi ME, Knafelz P, Rishniw M, et al. (2014) Transesophageal echocardiography as the sole guidance for occlusion of patent ductus arteriosus using a canine ductal occluder in dogs. J Vet Intern Med 28(5): 1504-1512.
- Roberts P, Adwani S, Archer N, Wilson N (2007) Catheter closure of the arterial duct in preterm infants. Arch Dis Child Fetal Neonatal Ed 92(4): F248-F250.
- Bentham J, Meur S, Hudsmith L, Archer N, Wilson N (2011) Echocardiographically guided catheter closure of arterial ducts in small preterm infants on the neonatal intensive care unit. Catheter Cardiovasc Interv 77(3): 409-415.
- Chen W, Yan X, Huang Y, Sun X, Zhong L, et al. (2015) Transthoracic echocardiography as an alternative major guidance to angiography during transcatheter closure of patent ductus arteriosus: technical feasibility and clinical relevance. Pediatr Cardiol 36(1): 14-19.
- Jesús María Damsky Barbosa, J. Alonso, A. de Dios (2015) PDA closure in a very low-weight premature infant with ADO II device. Neonatology Today 10: 1-5.
- Zhan EM, Nevin P, Simmon C, Garg R (2015) A novel technique for transcatheter patent ductus arteriosus closure in extremely preterm infants using commercially available technology. Cathet Cardiovasc Interv 85(2): 240-248.
- Baykan A, Narin N, Özyurt A, Argun M, Pamukçu Ö, et al. (2015) Do we need a femoral artery route for transvenous PDA closure in children with ADO-I? Anatol J Cardiol 15(3): 242-247.
- Alaa Roushdy, Azza El Fiky, Dina Ezz el Din (2012) Visualization of patent ductus arteriosus using real-time three-dimensional echocardiogram: Comparative study with 2D echocardiogram and angiography. J Saudi Heart Assoc 24(3): 177-186.
- Song H, Liu F, Dian K, Liu J (2010) Intraoperative transesophageal echocardiography-guided patent ductus arteriosus ligation in an asymptomatic nonbacterial endocarditis patient. Anesth Analg 111(4): 878-880.
- Beyer RW, Bier AJ (2009) Ultrasonic guidance for percutaneous closure of patent ductus arteriosus in an adult. J Invasive Cardiol 21(8): E141-E144.
- Eur J Echocardiogr (2011) Device closure of patent ductus arteriosus: optimal guidance by transaortic phased-array imaging. Eur Heart J Cardiovasc Imaging 12(2): E9.
- Rao PS (2007) Percutaneous closure of patent ductus arteriosus: state of the art. J Invasive Cardiol 19(7): 299-302.






























