Transcatheter Membranous Ventricular Septal Defect Closure, with Nit-Occlud PFM Device in One Working Group, Long-Term Follow up
Federico Borges Rodríguez1*, Angelo Sparano1, Yudith Robles1, Ernesto Urbano1, Manfred Hermanni1, Carlos Garcia1, Rosa Zabala2, Guillermo Villoria3, Roshec Bravo1, Ericson Ramirez1 and Carlos Troconis4
1Division of Pediatric Cardiology, Caracas Children’s Hospital, South America
2Division of Pediatric Cardiology, Cardiology Hospital Aragua, South America
3Division of Cardiology, CMDLT, South America
4Division of Cardiovascular Surgery, UCQNE, South America
Submission: October 04, 2016; Published: October 18, 2016
*Corresponding author: Federico Borges, Chief of the Division of Pediatric Cardiology, Caracas Children’s Hospital, Hospital de Niños J.M. de los Rios, Caracas, Venezuela, South America
How to cite this article: Angelo S, Yudith R, Ernesto U, Manfred H, Carlos G, et al. Transcatheter Membranous Ventricular Septal Defect Closure, with Nit-Occlud PFM Device in One Working Group, Long-Term Follow up. J Cardiol & Cardiovasc Ther. 2016; 1(4): 555567. DOI: 10.19080/JOCCT.2016.01.555567
Abstract
Objective: Goal of this work was to evaluate the safety and efficacy of transcatheter closure of ventricular septal defect (VSD) perimembranous (pVSD) with pfm device, Nit - Occlud, and long-term results. The VSD is the most common congenital heart disease being mostly membranous. Transcatheter percutaneous closure is a novel technique.
Material and methods: Between December 2004 and December 2013, 300 patients with VSD record were admitted to our study, previously admitted to the cath lab at our center for percutaneous treatment of its VSD with different types of devices. All patients were followed until December 2013, between 1 and 109 months. Cases closed with Devices pfm, Nit Occlud is therefore selected. There was thus obtained a sample of 59 cases, 5 cases were dismissed for having no full registration and review of 54 cases was performed. The age range 17 months to 16 years. The VSD type was treated perimembranous 100%. Sub Aortic 12, Sub tricuspid 27, Basal medium 5, and membranous muscle 5, not specified 5. pVSD aneurysm 51, 94.44%. VSD measures were between 1.5 and 16 mm, made by echocardiography or ventriculography. The successful placement of the device was 92.59%. The type of device used was Nit Occlud Coil VSD Le 35 cases, 64.81%, Nit Occlud PDA 19 cases, 35.18%. Complications were mostly minor; among the most relevant major complications was transitory hemolysis in 2 cases, 4%. There were no complete AV blocks between them.
Conclusion: Percutaneous closure of perimembranous VSD in experienced hands with Nit Occlud device of pfm can be performed safely and successfully with low morbidity and mortality. Long-term results are favorable, with the percutaneous closure of perimembranous VSD is a less invasive alternative and could be taken as first choice in the treatment of membranous ventricular septal defects.
Abbreviations: VSD: Ventricular Septal Defect; PVSD: Perimembranous Ventricular Septal Defect; MVSD: Muscular Ventricular Septal Defect; CAVB: Complete Atrio-Ventricular Blockade; QW: Quick Way; LV: Left Ventricule; RV: Right Ventricule; RS: Residual Shunt
Introduction
The Ventricular Septal Defect (VSD) is the most common congenital heart defect, and its variant perimembranous (perimembranous VSD) are the highest percentage of them, 70% [1-5]. Percutaneous closure of VSD is only approved in the literature for Muscular VSD (MVSD) [6-9], since in the perimembranous VSD Standard treatment is surgery with extracorporeal circulation [10-29] due to the high rate of complications reported in percutaneous procedures such as complete atrioventricular blockade (CAVB) [30]. Yet the Standard Surgical treatment has risks as CAVB 1.1%, Post Pericardectomy syndrome, residual shunts, besides being a more invasive method for the patient [10,17,29].
Cardiac Catheterization is an alternative to the VSD closure, tested as a method of first choice in closing muscle VSD [6-9] and exists as an alternative treatment in perimembranous VSD since the first reports of percutaneous VSD closure in 1988 [30-56]. This work demonstrates that the percutaneous method is a successful and low morbidity and mortality alternative in the procedure as well as in long-term Follow up of the VSD closure and specifically perimembranous VSD . In this paper perimembranous VSD closure with Nit Occlud device Coil reported. This work is a single working group with long-term follow up.
Materials and Method
Material
It was taken for analysis record of all patients diagnosed with VSD by the working group Hemodynamics Laboratory of Cardiology at Children’s Hospital J.M. Los Rios, Caracas, Venezuela, between December 2004 and December 2013 in a sample of 300 cases treated in the cath lab 59 cases treated with Coil Nit Occlud of pfm was selected, discarding 5 cases for not having complete records and 54 cases of membranous VSD closure with pfm Nit Occlud coil were processed.
Devices: The devices used were Nit - Occlud Brand , Spiral Coil Sistem, pfm house : NIT- Occlud VSD Le, NIT- Occluded PDA.
Method
All features of the technique, patients and pathology described , namely: Access Road: 2 options, the Retrograde, Quick Way (QW ) in which the catheter is passed from Left Ventricule (LV) to Right Ventricule (RV), the device first cone is deployed in the RV and then the second cone is displayed in the LV. Loop method in which the VSD is passed from the left ventricle is advanced with the right guide to a cavity as vena cava or pulmonary artery, the guide is captured and exposed outside the patient by establishing a Femoral Artery -vein loop, the transport catheter of the device progresses from the vein into the left cavities to the Aorta, specifically with Nit - Occluded Spiral Sistem, the device first cone is exposed in the Aorta, deployed at LV and then the second cone is displayed in the RV.
Patients studied and their characteristics: Total patients (p) with VSD, 54.
4.2.2 Gender: Female Dominance 57.4%.
4.2.3 Age: Between 17 months and 16 years.
4.2.4 Weight: Between 8 and 53 kg.
VSD type: Described in 54p, 54 Membranous, 100% (Table 1).
Symptoms such as fatigue, weight gain difficulty; medication used for heart failure; Echocardiographic findings: Qp/Qs ratio, AI/Ao ratio, radiological findings: Cardiomegaly, hyperflow or venous congestion. Assigning one point to each for a total of 5 [1-5,57,58].
VSD size: Measured by Trans- Thoracic Echocardiography, transesophageal echocardiography or catheterization. Range of 1.5 to 16 mm (Figures 1-3) (Tables 2-4).
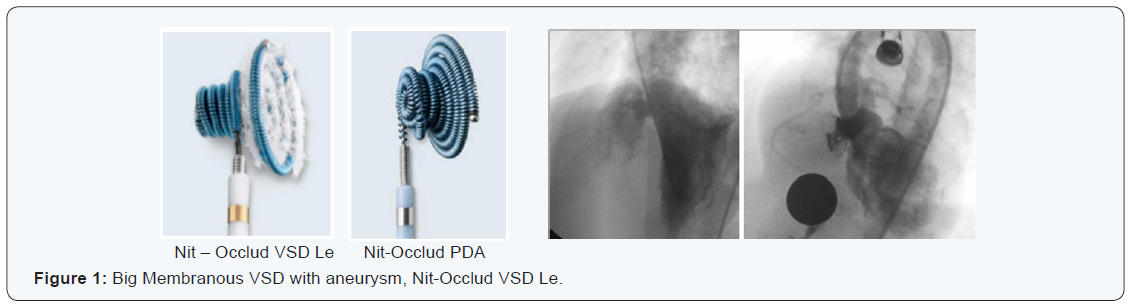
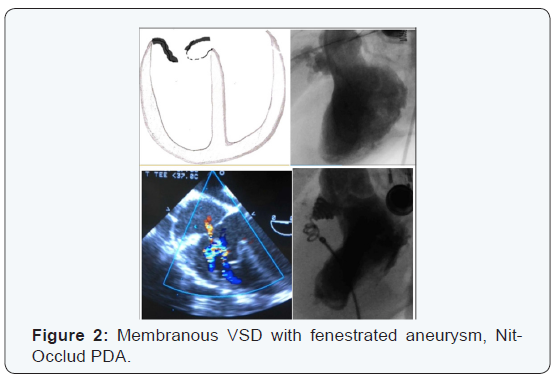
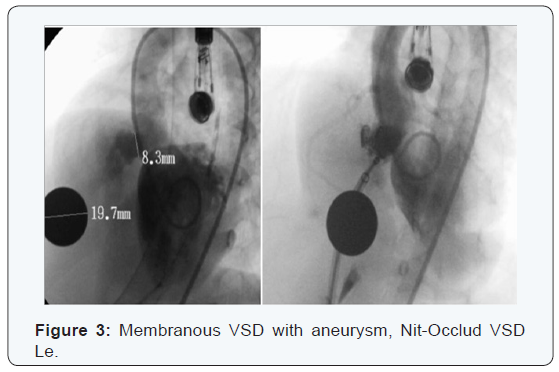
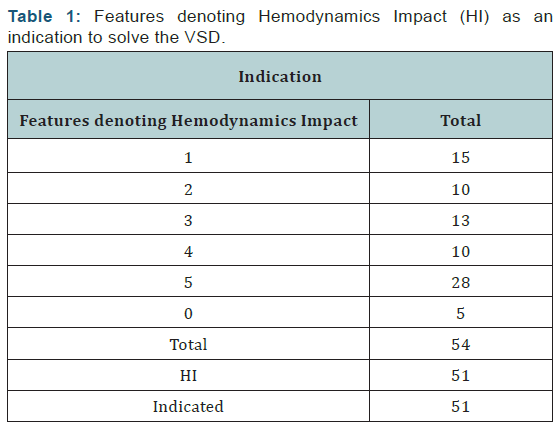
The percentage of patients with indication was 94.44 %.
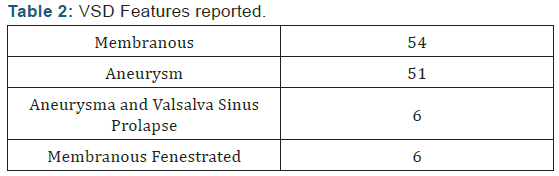
Membranous features: Described 54p, Aneurysm (Aneu) 51 p, 94.44 %;
Fenestrated 6p, 11.11 %; with Valsalva Sinus Prolapse (VSP) and Aneurysm 16p, 11.11 %.

Location of the membranous: Described 54p, 100% STr 27p, 50%; SAo 12p, 22.22%; 5p BM

Concomitant diseases, congenital heart disease or Acquired type
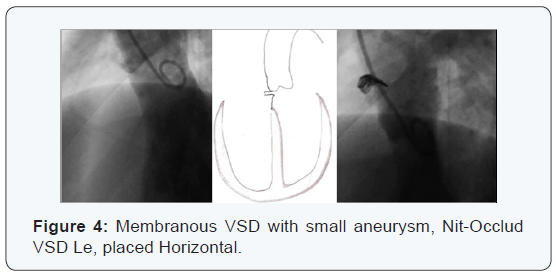
Total 9p, 17 %; 2 cases with PFO closed in the same procedure with Amplatzer PFO; 1 patient with Mild Pulmonary Stenosis dilated with balloon in the same procedure; 1 case with ASD ; 1 Case with ASD and PDA which failled closure the ASD with Hellex and failled Closure PDA with Nit Occlud PDA; 1 VSD previously closed with Nit Occlud VSD Le and residual VSD a new device Nit Occlud VSD Le was implanted; 1 VSD Closed Surgically with Residual VSD was closed with Nit Occlud VSD Le, 1 Case had been previously tried to close with Amplatzer and made a transient complete AV block so the catheterization was aborted, was closed with Nit Occlud VSD Le; 1 case with Mitral Stenosis and Mitral parachute (Figure 4).
Results
Procedure time
Heparin time was measured, Heparin was placed once VSD diagnosed by TEE or Catheterization, and was counted until the VSD was closed; and fluoroscopy time. Heparin average time was 36 minutes; fluoroscopy average time was 30 minutes.
Access Road
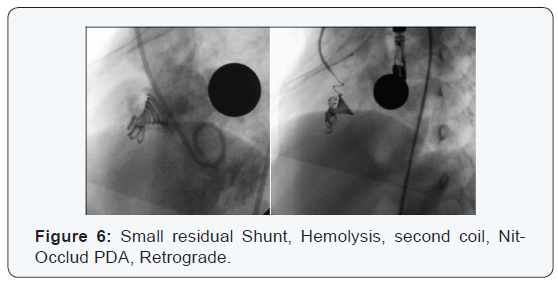
Only one case was closed Retrograde Quick Way from VI, residual restrictive VSD case presented Hemolysis and placed a PDA Nit Occlud to stop hemolysis (Figures 5 & 6).

Success of the procedure
It was considered:
- Succeeded: all VSD Closed
- Failed: all attempts to close VSD, crossing the VSD with the catheter without achieving close it
- Aborted: VSD that for some reason or feature is not trying to cross the VSD with the catheter.
- Successful: 50 cases, 92.59%;
- Failed: 3 cases, 5.55%;
- Aborted: 1 Case, 1.85%.
If we take into account the premise of not closing those present TCAVB in the procedure, the success rate is 94.33 %, 50 cases of 53 procedures.
The causes of failure were: 1 case migration to VD, being rescued; 1 case the device is jam when passing through the aortic valve, when achieve release it migrated to VD; 1 patient with ASD, PDA and VSD already closed with Nit Occlud VSD Le in the same procedure, in the process trying to close the PDA the device is hooked already placed migrating, being rescued later, the ASD was unsuccessfully tried to close with Hellex. The cause of Aborted: 1 case for transient AVB.
The results according to the characteristics of the VSD was assessed by type: Ratio VSD Size and Device size
The Nit - Occlud is recommended to oversize the bigger loop 2-4 mm relative to the opening of the VSD, ie , we take equal size to that dimension of the Loop least 4. Fulfilled with the approach of not overstate the device to seek to avoid the complication of permanent AVB to cause pacemaker, as also in some cases smaller devices were used to leave the device inside the aneurysm [48].
2nd device placed in the same patient: 2p, of 50 closed, 3.70%; ie, 1p Nit -Occlud VSD Le with Hemolysis solve placing the 2nd Coil Nit - Occlud PDA in the first week, (reported in hemolysis ). We report a late second case 1p perimembranous VSD STR withaneurysm of 10mm, closed with NIT-Occlud VSD Le 10x6, migrated into the aneurysm, with rsidual shunt for 3 years, was placed on the 2nd Nit VSD Le 12x6, stays with minimum residual shunt with minimum Hemodynamics Impact, then the 1st device found migrated and healed in right branch of the pulmonary artery, was attempted to remove it and failed (Figures 5 & 6).
Follow-up time: Between 1 month and 109 months.
Complications: Immediate
Residual shunt (RS)
Immediate in the catheterization, 20p of the 50p with device 40 %; of them 12p with Nit-Occlud VSD Le, 8p Nit-Occlud PDA,(This device is not designed for VSD closure and is not a fiber- Coil). At follow-up: still wit RS at 24 hour follow-up 11p 22%, all with VSD Le Nit Occlud. All Nit-Occlud PDA Shunt disappeared in 24 hours. Subsequently the RS disappeared one month 7p, 14 %; 5p more disappear on their follow-up to 2 months 2p,1p to 1 year, 2 years and 5 years respectively. Subtracting 2p 4% of the Nit-Occlud placed persists with minimal RS without Hemodynamics Impact at 9 years of follow up.
Transient hemolysis
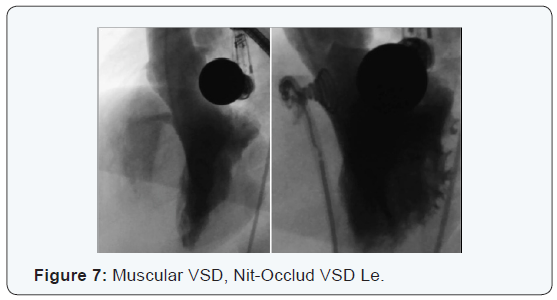
Starts in the first hours after catheterization, 2p of the 50 closed, 4%. 1p Nit-Occlud PDA of the 19p with Nit- Occlud PDA, 5.26 %, is spontaneously resolves the 2nd day, this tipe of device is no designed to VSD closure, hemolysis subsides spontaneously within 2 days. 1p Nit -Occlud VSD Le of the 35p with that tipe of device, 2.85 % with RS and hemolysis was placed a 2nd Coil Nit Occlud PDA quick Way a week latter and the RS and hemolysis disappeared in 5 days [52] (Figures 5-7).
Immediate Migration: Total 3p of the 54p, 5.55 %. They are rescued named in failed cases.
Migration remaining within the aneurysm: 2p migrated into the aneurysm, 4%, namely: 1p Nit-Occlud VSD Le migrated into the aneurysm (named in placing 2nd device on the same patient in long-term follow up); 1p with Nit-Occlud VSD Le migrating into the aneurysm with RS, removed in surgery at 7 years (named in Surgery).
No Progress transport pod RV to LV throught the VSD: 1p solved with Nit - Occlud PDA ASA Way, because the transport pod is 5F (Figure 2).
Migration in the follow up: 1p of the 50 placed 2%; NIT VSD Le migrated to 7 years (reported in 2nd placement device).
Rhythm disorders Transient immediately or in the follow up: 1 transient 1st grade AVB disappears immediately. 1 Transient right bundle branch Block disappears immediately.
Permanet Branch Block in the follow up: 1p of the 50 closed, 2 %; Hemiblock of the anterior subdivision of the left bundle branch Hiss in the follow up without Hemodynamics Impact, VSD STR aneurysm, Nit-Occlud VSD Le [51].
Surgery in the follow up: 1p, 2%. Nit-Occlud VSD Le migrates into the aneurysm, persisted with RS, at 4 of year follow-up showed thrombocytopenia classified as Marrow Aplasia meriting bone marrow transplant, thrombocytopenia persisted until the removal of the device and close the VSD for large RS to 7 years [31,59].
Discussion
High level of success in closing perimembranous VSD with Coil Nit Occlud. There were no CAVB including the following 9 years. Most complications were transient, 2p with residual shunting without hemodynamic impact to 9 years and only by large RS 1P and thrombocytopenia removed in surgery at age 7, 2% on follow up to 9 years [60-65].
Conclusion
Transcatheter closure of aneurysm perimembranous VSD with Nit Occlud Coil device has high chance of success with a low level of complications.
References
- Greech V (1998) Epidemiology and Diagnosis of Ventricular septal defect in Malta. Cardiol Young 8(3): 329-336.
- Lin MH, Wang NK, Hung KL, Shen CT (2001) Spontaneous closure of ventricular defect in the first year of life. J Formos Med Assoc 100(8): 539-542.
- Ruangritnamchai C, Khomsathit P, Pongpanich B (1993) Spontaneous Closure of small ventricular septal defect first six months of life. J Med Assoc Thai 76(2): 63-71.
- Turner SW, Hunter S, Willye JP (1999) The natural history of ventricular septal defect. Arch Dis Child 81(5): 413-416.
- Mehta AV, Chidamvam B (1992) Ventricular Septal Defect in the first year of life. Am J Cardiol 70(3): 364-366.
- Bridges ND, Perry SB, Keane JF, Goldstein SA, Mandell V, et al. (1991) Preoperative transcatheter closure of congenital muscular ventricular septal defects. N Engl J Med 324(19): 1312-1317.
- Zahid Amin, Xiaoping Gu, James M Berry, John L Bass, Jack L Titus, et al. (1999) New device for closure of muscular ventricular septal defects in a canine model. Circulation 100(3): 320-328.
- Thanopoulos BD, Tsaousis GS, Konstadopoulou GN, Zarayelyan AG, et al. (1999) Transcatheter closure of muscular ventricular septal defects with the amplatzer ventricular septal defect occluder: initial clinical applications in children. J Am Coll Cardiol 33(5): 1395-1399.
- Milind Chaudhari, Massimo Chessa, Oliver Stumper, Joseph V De Giovanni (2001) Transcatheter coil closure of muscular ventricular septal defects with Gianturco coils. Journal of Interventional Cardiology14(2): 165-168.
- Tucker EM, Pyles LA, Bass JL, Moller JH (2007) Permanent pacemaker for atriventricular conduction block after operative repair of perimembranous ventricular septal defect. J Am Coll Cardiol 50(12): 1196-1200.
- Mavroudis C, Backer CL, Jacobs JP (2003) Ventricular septal defect. Pediatric Cardiac Surgery (3rd edn.), Mosby, Inc pp. 298-320.
- Ross-Hesselink JW, Mejiboom FJ, Spitaels SE, Van Domberg R, Van Rijen EH, et al. (2004) Outcome of patients after surgical closure of ventricular septal defect at young age: longitudinal follow-up of 22-34 years. Eur Heart J 25(12): 1057-1062.
- Kitagawa T, Durham LA, Mosca RS, Bove EL (1998) Techniques and results in the management of multiple ventricular septal defects. J Thorac Cardiovasc Surg 115(4): 848-856.
- Wollenek G, Wyse R, Sullivan I, Elliot M, de Leval M, et al. (1996) Closure of muscular ventricular septal defects through a left ventriculotomy. Eur J Cardiothorac Surg 10(8): 595-598.
- Serraf A, Lacour-Gayet F, Bruniaux J, Ouaknine R, Losay J, Petit J, Binet JP, Planche C (1992) Surgical management of isolated multiple ventricular septal defects: logical approach in 130 cases. J Thorac Cardiovasc Surg 103(3): 347-342.
- Hobbins SM, Izukawa T, Radford DJ, Williams WG, Trusler GA (1979) Conduction disturbances after surgical correction of ventricular septal defect by the atrial approach. Br Heart J 41(3): 289-293
- Backer CL, Winters RC, Zales VR, Takami H, Muster AJ, et al. (1993) The restrictive muscular ventricular septal defect: how small is too small to close? Ann Thorac Surg 56(5): 1014-1019.
- Vázquez F, Mirabal R, González O, González A, Rodríguez O, et al. (2006) Resultados del tratamiento quirúrgico de la comunicación interventricular en pacientes pediátricos. Anales de Cirugía Cardíaca y Vascular 12(1): 28-33.
- Castañeda AR (1994) Ventricular Septal Defect. En: Cardiac Sugery of the Neonate and Infant. 1ra Ed, W.B. Saunders Company pp. 187-201.
- Kirklin JW (1993) Ventricular Septal Defect. En: Cardiac Surgery. 2da Ed, Churchill Livingstone Inc 749- 824.
- Fong XJ, Ho TF, Yip WC (2004) Signal-averaged electrocardiograms of children with ventricular septal defects before and after surgical repair. Ann Acad Med Singapore 33(5): 70-71.
- Kirklin JW (1983) Tratamiento Quirúrgico de la comunicación interventricular. En: Sabiston Jr DC. Cirugía Toráxica. 2da Ed. Ciudad Habana: Editorial Científico Técnica 1091-1108.
- De Leval M (1983) Ventricular Septal Defects. En: Stark J, de Leval M. Surgery for congenital heart defects. 1ra Ed. Grune Stratton, INC. 271- 84.
- Andersen HØ, de Leval MR, Tsang VT, Elliott MJ, Anderson RH, et al. (2006) Is complete heart block after surgical closure of ventricular septum defects still an issue? Ann Thorac Surg 82(3): 948-956.
- Rodríguez-Ortega F, Solís-Jiménez G, Jacobo Valdivieso E, Díaz G, Flores O, Espinosa O, et al. (2007) Cirujano General Vol. 29(2), Cirugía.






























