Zero Percent Inappropriate Rates for Percutaneous Coronary Intervention are Achievable and Sustainable at One Year with a Multifaceted Quality Improvement Initiative
Lyndon C Box*, Karen Dey RN and Robert L Duerr
St. Luke’s Idaho Cardiology Associates, West Valley Medical Center, USA
Submission: June 28, 2016; Published: July 15, 2016
*Corresponding author: Lyndon Box, West Valley Cardiology, 1906 Fairview Avenue Suite 230 Boise, ID 83605, St. Luke’s Idaho Cardiology Associates, West Valley Medical Center, Caldwell, Boise, ID, USA, Tel:904-612-2630; Email:lyndoncbox@outlook.com
How to cite this article: Lyndon CB, Karen D RN, Robert LD. Zero Percent Inappropriate Rates for Percutaneous Coronary Intervention are Achievable and Sustainable at One Year with a Multifaceted Quality Improvement Initiative. J Cardiol & Cardiovasc Ther. 2016; 1(3): 555562. DOI: 10.19080/JOCCT.2016.01.555562
Abstract
Introduction: Appropriate Use Criteria Scores for percutaneous intervention (AUC-PCI) are being used to evaluate appropriateness of procedures performed by hospitals and interventional cardiologists. Effective strategies for improving AUC-PCI scores are needed.
Methods: We reviewed all inappropriate for one year. Multiple interventions targeting the root causes were implemented. We then evaluated the subsequent percentage change for AUC scores, prior stress imaging, non-obstructive disease and PCI volume.
Results: From 2012 Quarter 2- 2013 Quarter 1 (2012Q2-2013Q1) the inappropriate PCI rate was 1.7%; Following the intervention, there were 0.0% inappropriate PCI for one year. PCI volume increased by 5.35%; stress testing increased by 5.1% and the rate of non-obstructive disease increased by 1.5%.
Conclusion: Our experience demonstrates that 0.0% inappropriate PCI rates are not only achievable, but can be sustained for one year. Secondarily, there was an increase in stress testing and PCI volume without a change in the rate of non-obstructive disease.
Abbreviations: AUC-PCI: Appropriate Use Criteria Scores for Percutaneous Intervention; PCI: Percutaneous Coronary Intervention; NCDR: National Cardiovascular Data Registry; ACS: Acute Coronary Syndrome; SCAI-QIT: Society for Cardiac Angiography and Interventions Quality Improvement Toolkit; CCS: Canadian Cardiovascular Society; CABG: Coronary Artery Bypass Grafting; EMR: Electronic Medical Record
Introduction
With the realization that overutilization of medical services is a critical economic and public health concern, numerous initiatives have been developed to address the problem. Due to its widespread use, reducing the frequency of Percutaneous Coronary Intervention (PCI) has been suggested as a goal [1]. The American College of Cardiology has been supportive of efforts to reduce overutilization of PCI in situations where there is limited evidence of benefit. The Appropriate Use Criteria for percutaneous coronary intervention (AUC-PCI) were released in 2009 and revised in 2012 to guide clinical decisions [2]. To support utilization of AUC-PCI as a quality metric, the National Cardiovascular Data Registry (NCDR) provides AUC-PCI scores in benchmarked feedback reporting. Both private and public scrutiny has caused AUC-PCI to quickly become an important performance measure [1,3-5].
The 2012 AUC-PCI guideline divides indications into three primary categories: Appropriate, Uncertain and Inappropriate. The NCDR registry institutional outcomes report benchmarks the percentage of each category relative to other institutions and all registry patients. Reports are provided for all PCI patients, those with acute coronary syndrome (ACS) and those without ACS (Non-ACS).
There are numerous challenges to improving AUC scores. Foremost are the multiple potential causes. These include documentation deficiencies, errors in data abstraction and variability in clinical practice [6-8]. To achieve rapid improvement, we implemented multiple interventions in parallel. This contrast with the traditional cyclic model of performance improvement where the problem is identified, a single intervention is planned, implemented and the results analyzed prior to planning the next intervention.
Methods
To identify causes for inappropriate PCIs specific to our institution, the NCDR individual fallout reporting feature was utilized to identify all inappropriate cases for the second quarter of 2012 through the first quarter of 2013(2012Q2-2013Q1). The project physician lead (L. Box) reviewed all relevant documentation. The root cause was identified and entered into an excel spreadsheet. To develop interventions, we reviewed recommendations from the Society for Cardiac Angiography and Interventions Quality Improvement Toolkit (SCAI-QIT) webinar “Navigating the New 2012 Revascularization Appropriate Use Criteria” [9], presentations [10], the NCDR quality improvement for Institutions website and the Accreditation for Cardiovascular Excellence Cath/PCI standards [11].
Additional solutions were identified through discussion with all involved providers. The interventions were initiated beginning in July 2013 and were fully operational by the end of 2013Q4. Presently there is no established standard rate of each category (A, U and I). The NCDR registry provides reports the 50th percentile and 90th percentile for all participants for comparison. We therefore targeted the 90th percentile performance level as our goal. To better understand the impact on practice patterns, we pre-specified PCI volume, the rate of pre-procedure stress testing and the rate of negative angiograms as metrics but without set targets.
A secondary review was conducted to evaluate the accuracy of documentation specifically related to Non-ACS PCI. Documentation related to the indication for all outpatient coronary angiograms for 2013Q1 was reviewed. A determination of the validity of the stated indication based on the supporting documentation was made in each case. The key variables as entered into the Cath-PCI registry were then checked against the documentation to confirm that documentation and data abstraction was accurate.
Results
During 2012Q2-2013Q1, there were 12 cases scored I. Of these, 7 were classified as ACS cases and 5 as Non-ACS. Guided by the reviewer’s findings two primary causes were identified:
- Physician clinical decision
- Documentation and abstraction.
The second category reflected the difficulty with clearly discerning the primary indication and clinical history at the time of abstraction. In general problems with documentation also lead to inaccurate data abstraction. Therefore, documentation and abstraction problems were merged into a single cause. The initial review findings are presented in (Table 1).
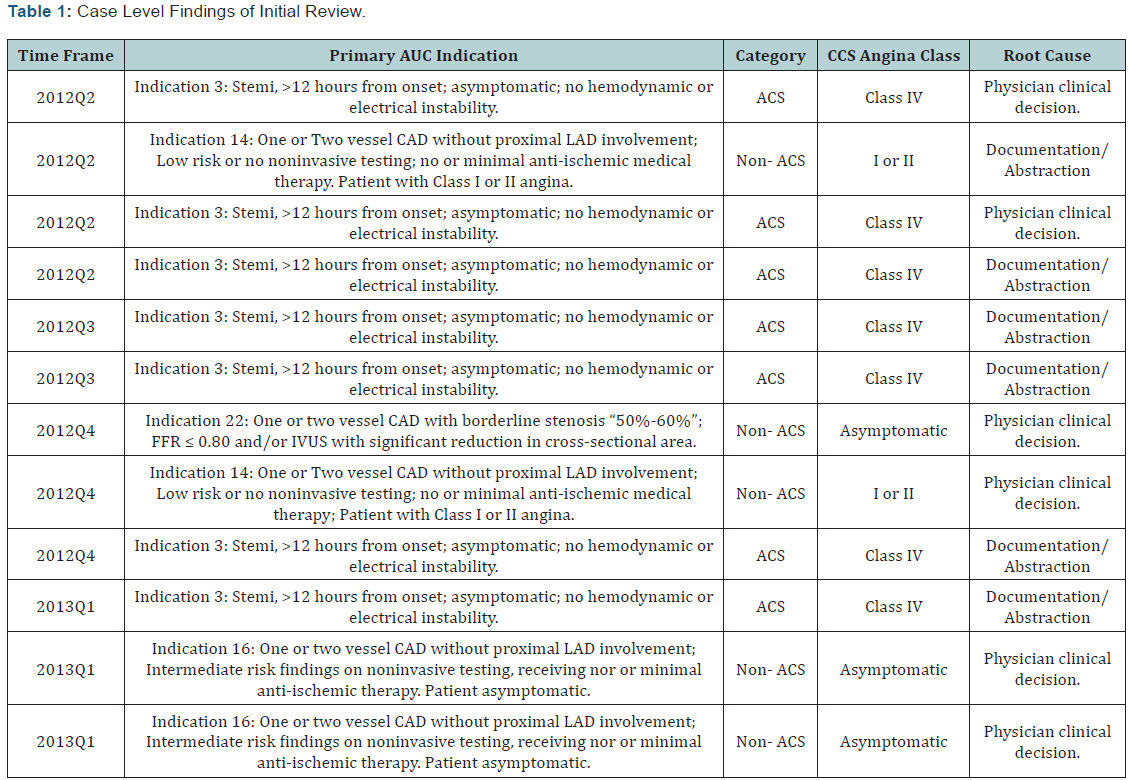
Guided by the chart review findings, we selected multiple possible interventions for improving performance. These interventions are listed in (Table 2). A recurring theme across these interventions was improving documentation of the key variables for determination of AUC: the Canadian Cardiovascular Society (CCS) Angina Classification, the number of anti-anginal medications, noninvasive testing results with a risk estimate and a prior history of coronary artery bypass grafting (CABG) [12].
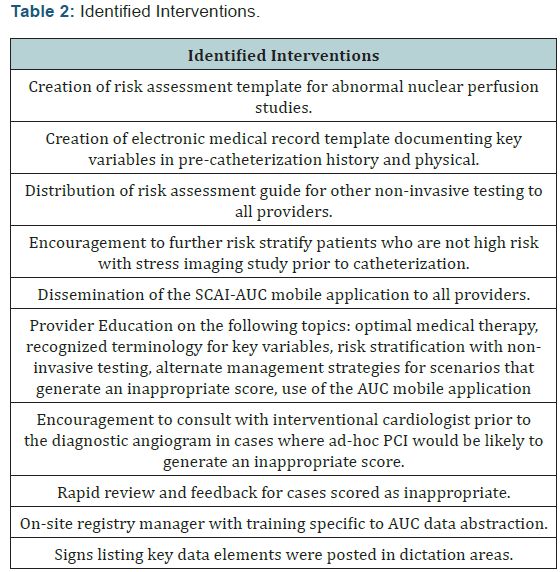
This was addressed not only with templates but also with provider education regarding the data element definitions and usage of proper terminology. Education on all interventions was provided at conferences and physician meetings. To improve the data abstraction process, a new position was created for an onsite data registry manager. Previously, data abstraction was done offsite. The position was filled by an RN with catheterization laboratory experience (K. Dey). During orientation, the manager was instructed on the abstraction process relevant to AUC. An additional challenge identified in discussions was the hybrid medical record system within our institution. The outpatient setting utilized the EPIC electronic medical record (EMR) system while the inpatient setting used paper charts with dictation. To address this, signage regarding documentation of the key data elements was placed in all inpatient areas frequently used by physicians for dictation. All interventions were operational by the close of 2013Q4 and the project was officially launched as part of a divisional grand rounds presentation in December, 2013.
Data Analysis and Statistical Methods
The results of our intervention were assessed by performance on the NCDR Institutional Outcomes Report. Our focus was the change in the percentage of inappropriate cases as well as the absolute goal of exceeding a 90th percentile performance level. The additional metrics of volume, rate of stress testing and rate of negative angiograms were reported as percentages without prespecified targets.
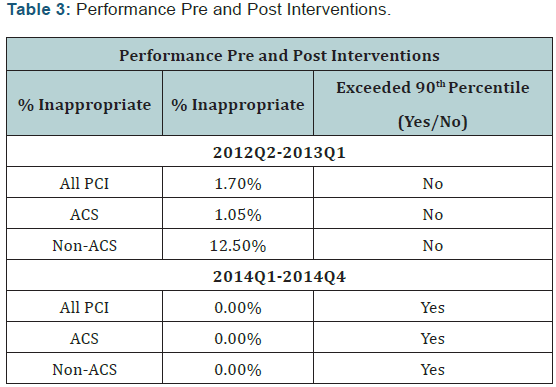
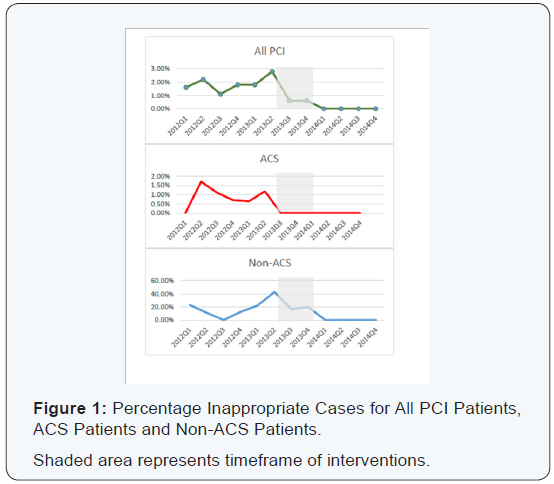
At one year, the rate of inappropriate interventions across all categories was 0.00%, thus meeting the 90th percentile target for each category at one full year post interventions (2014Q1- 2014Q4) (Table 3). During the implementation phase, 2013Q2 data had been submitted but was not available. The interventions were in varying stages of implementation for 2013Q3-Q4. The trajectory of improvement is presented in (Figure 1) depicting the quarterly inappropriate score for 2012Q1-2014Q4. The number of PCI procedures increased by 5.3%. The percentage of patients with a stress or imaging study increased by 5.1%. The percentage of patients with non-obstructive CAD increased by 1.5% (Table 3). Secondary chart review of all elective cases demonstrated 100% consistency of the stated indication for the procedure with the supporting documentation. The documentation was also 100% consistent with the data entry of key variables into the Cath-PCI registry by the registry manager.
Recent works in this area show the new echocardiographic methods such as strain rate and speckle tracking echocardiography to enable easier, more objective and more accurate analysis of the minimum, initial changes in the function of the right heart, which will greatly contribute to an easier and more precise diagnosis and improved treatment of heart diseases in children.
Discussion
Since the introduction of PCI AUC in 2009, hospitals and physicians have struggled with implementation. One challenge is the lack of an acceptable threshold. It is not intended that AUC scores be 100% Appropriate or 0% Inappropriate [12]. At the hospital level, AUC scores have been shown to have a wide variation [13,14]. The NCDR registry allows benchmarking against other institutions with a reported inappropriate 50th percentile for ACS of 0% and Non-ACS of 13.5% for the 2014Q1- Q4. Patient level analysis of NCDR data for July 1, 2009 and September 20, 2010 demonstrated inappropriate ratings of 1.1% for ACS and 11.6% for Non-ACS [15]. Data from other registries have found similar rates. Analysis of PCIs performed in the state of Washington during 2010 found inappropriate ratings 1% for ACS and 17% for Non-ACS [13]. Examination of the New York State PCI registry found 14% of Non-ACS PCI scored inappropriate [16]. In the highly controlled environment of the courage trial, the numbers were much lower with retrospective analysis finding only 5.1% of interventions inappropriate [17].
Our experience demonstrates that a 0% rate of inappropriate is both achievable and sustainable. There have been prior reports of successful quality improvement initiatives for AUC scores. Utilization of the SCAI AUC application was reported by both Chen & Jackson [18,19] as an effective tool for improving AUC scores. Provider education has also been reported as effective [20]. A multifaceted approach was described by Beauvallet et al. & Wong et al. [6,21] but they did not achieve the same degree of improvement nor did they report sustained improvement over one year.
Our efforts included the active involvement of a physician lead and strong engagement of all interventional cardiologists within our institution. Many potentially inappropriate PCIs were avoided by informal consultations prior to angiography. Timely communication between the registry manager and providers through feedback reports rapidly improved both documentation and abstraction. Having a dedicated registry manager on site facilitated this process.
Most of our interventions were voluntary. However, the use of templates for reporting stress test risk results and for preprocedure documentation of key variables were adopted by the division as mandatory. These requirements are likely to have the greatest impact on AUC performance improvement [9-13]. Use of the SCAI AUC application was optional but it was adopted by many providers. The educational intervention addressed variations in clinical management leading to inappropriate scores. Group discussion of alternative management strategies for common inappropriate scenarios reinforced didactic education and increased provider comfort.
There were likely other factors beyond the interventions contributing to the low inappropriate rate. It has been reported that regional practice patterns of lower utilization predicts lower scores [22]. In fact this study was conducted in an area with lower rates of PCI utilization. The Dartmouth Atlas reported 4.4 inpatient PCI procedures per 1000 medicare beneficiaries for the state of Idaho in 2012, which is at the 10th percentile [23]. Our lower than average rate of negative angiograms (Table 3), higher symptom burden, greater use of two anti-anginal agents and percentage of high risk stress tests suggests a conservative management approach across providers. In particular, our negative angiogram rate suggests good patient selection [24].
Critics of AUC have suggested that procedures based on sound clinical judgment may be deemed inappropriate by AUC criteria [25]. This raises the concern that patients might be denied needed care due to concern over performing an inappropriate procedure. This was not a clinical study and therefore we cannot exclude this possibility, however, there were no anecdotal reports to support this concern. Analysis of the courage trial data suggests that such events would be infrequent [17]. A possible interpretation of our success is that documentation did not accurately reflect the true clinical scenario. Our secondary analysis of all cases for 2013Q1 argues against this possibility.
To verify the validity of this review, the documentation and abstraction process was also discussed with the NCDR staff and it was felt that our methods were sound. Physicians were educated on utilization of terminology that was consistent with the NCDR data dictionary, but were explicitly instructed against intentionally misrepresenting the clinical facts to avoid inappropriate scores. There has been widespread speculation that overutilization of PCI is driven in part by economic concerns and that implementation of AUC would decrease the number of PCIs being performed [8]. During this initiative, PCI volumes actually increased. While this may have been due to multiple factors, it certainly does not support the claim that AUC will reduce the number of interventions.
Conclusion
Given that providers were encouraged to increase utilization of noninvasive testing prior to coronary angiography, it is not surprising that the percentage of noninvasive testing increased. Interestingly, this did not change the frequency of nonobstructive disease found at the time of angiography. This could be interpreted both as a sign that needed care was still being delivered or alternatively, that the utility of noninvasive testing in the evaluation of ischemic coronary artery disease is lower than current perception. The most likely interpretation is that given the conservative practice style already in existence within our group, the increase in stress testing had a minimal impact. It does raise the concern that broad implementation of AUC may actually increase cost while not improving care beyond what can be achieved with sound clinical judgment.
Limitations
Limitations of this study include the study design, which was a single center observational study. We cannot make any conclusive statements regarding the clinical effects of our interventions. Future studies regarding the clinical impact of very low inappropriate AUC scores need to be conducted in a prospective, randomized trial. However, given the current available evidence, we do believe it is reasonable for institutions to target the lowest inappropriate AUC scores possible. This report provides an overview of a successful multifaceted approach to reach this goal.
References
- Commission TJ (2013) Proceedings from the National Summit on Overuse.
- Patel MR, Dehmer GJ, Hirshfeld JW, Smith PK, Spertus JA (2012) ACCF/ SCAI/STS/AATS/AHA/ASNC/HFSA/SCCT 2012 Appropriate use criteria for coronary revascularization focused update: a report of the American College of Cardiology Foundation Appropriate Use Criteria Task Force, Society for Cardiovascular Angiography and In. J Am Coll Cardiol 59(9): 857-881.
- Forum NQ. Percutaneous Coronary Intervention (PCI): Comprehensive Documentation of Indications for PCI. Cardiovascular Measures.
- Allen M (2012) To Stent or Not to Stent, That is the Question. ProPublica.
- Dougherty SSG (2015) Are Doctors Exposing Patients to Unnecessary Cardiac Procedures? US News World Rep.
- Beauvallet SR, Cogan J, Seto TB, Spies C (2014) Improving Documentation and Guideline Awareness Increases Compliance with Appropriate Use Criteria in the PCI Population. Poster Present NCDR 2014 Annu Meet.
- Bsn KV, Heart T, Baylor H (2014) Shifting Appropriate Use Criteria Ratings for Coronary Revascularization from Uncertain to Appropriate : A Clinical Documentation Project.
- Behnke LM, Solis A, Shulman SA, Skoufalos A (2013) A Targeted Approach to Reducing Overutilization: Use of Percutaneous Coronary Intervention in Stable Coronary Artery Disease. Popul Health Manag 16(3): 164-168.
- Ho, Kalon KL Dehmer GJ (2012) Navigating the New 2012 Revascularization Appropriate Use Criteria.
- Patel MR (2013) Highlights of the Appropriateness Use Criteria, and How to Apply Them in Daily Practice. In: Society for Cardiac Angiography and Interventions Scientific Sessions.
- ACE: Accreditation for Cardiovascular Excellence. ACE Cath/PCI Standards. 2013: 1-24.
- Fitzgerald S (2012) NCDR Carth PCIv4 AUC Companion Guide. Am Coll Cardiol.
- Bradley SM, Maynard C, Bryson CL (2012) Appropriateness of Percutaneous Coronary Interventions in Washington State. Circ Cardiovasc Qual Outcomes 5(4): 445-453.
- Bradley SM, Chan PS, Spertus JA, Kennedy KF, Douglas PS, et al. (2012) Hospital Percutaneous Coronary Intervention Appropriateness and In-Hospital Procedural Outcomes: Insights from the NCDR. Circ Cardiovasc Qual Outcomes 5(3): 290-297.
- Chan PS, Patel MR, Klein LW, Krone RJ, Dehmer GJ, et al. (2011) Appropriateness of Percutaneous Coronary Intervention. J Am Med Assoc 306(1): 53-61.
- Hannan EL, Cozzens K, Samadashvili Z, Walford G, Jacobs AK, et al. (2012) Appropriateness of coronary revascularization for patients without acute coronary syndromes. J Am Coll Cardiol 59(21): 1870- 1876.
- Bradley SM, Chan PS, Hartigan PM, Weintraub WS, Nallamothu BK, et al. (2015) Validation of the Appropriate Use Criteria for Percutaneous Coronary Intervention in Patients With Stable Coronary Artery Disease ( from the COURAGE Trial ). Am J Cardiol 116(2): 167-173.
- Chen, SK Kalon, KL Gannon, S Thyagarajan, B Chakrabarti, AK Potter, et al. (2014) C-062 Utility of a Real-Time Appropriate Use Criteria Decision Support Tool for Percutaneous Coronary Interventions in Non-Acute Coronary Syndrome. Catheter Cardiovasc Interv 83(1): S163.
- Jackson, Nanette Kirk J (2014) C-075 Incoporating the SCAI-QIT Appropriate Use Criteria Application into the Electronic Documentation Process. Catheter Cardiovasc Interv 83(1): S173.
- Kahlon, Kumar T, Kline M, Scott L, Berger E, et al. (2014) O-08 Successful Prevention of Inappropriate Cardiac Catheterizations by an Educational and Screening Prgoram in a Rural Tertiary Cardiac Referral Center. Catheter Cardiovasc Interv 85(2): S122.
- Wong B, Estrada S (2014) Process Improvement to Meet Appropriate Use Criteria (AUC) for Elective Patients in the National Cardiovascular Data Registry (NCDR) CathPCI Registry. In: NCDR Annual Meeting 2014.
- Thomas MP, Parzynski CS, Curtis JP, et al. (2015) Percutaneous Coronary Intervention Utilization and Appropriateness across the United States. PLoS One 10(9): e0138251.
- Institute TD. The Dartmouth Atlas of Health Care.
- Douglas PS, Patel MR, Bailey SR Dai D, Kaltenbach L, et al. (2011) Hospital Variability in the Rate of Finding Obstructive Coronary Artery Disease at Elective, Diagnostic Coronary Angiography. J Am Coll Cardiol 58(8): 801-809.
- Marso SP, Teirstein PS, Kereiakes DJ, Moses J, Lasala J, et al. (2012) Percutaneous coronary intervention use in the United States: Defining measures of appropriateness. JACC Cardiovasc Interv 5(2): 229-235.






























