Incidence, Recurrence and Complications after Facial Skin Cancer Excision: Retrospective Analysis of Multi-Institutional Experiences
Yasser Helm Ali*, Ahmad Taha and Abd EL Nasser Khallaf
Department of Plastic Surgery, Al-Azhar University, Egypt
Submission: March 07, 2018; Published: March 26, 2018
*Corresponding author: Yasser Helmy Ali, Assistant professor of plastic and burn surgery. Faculty of Medicine, Al-Azhar University, Nasercity, Cairo, Egypt-6th of October city- central road- Al-fateh towers-Doctors’ tower No 6-3RD Floor-above AUDI Bank, Egypt, Tel: 002-01004406331; Fax: 002-02-38376114; Email: dryasserhelmy@gmail.com; dryasserhelmy@azhar.edu.eg
How to cite this article: Yasser Helm Ali, Ahmad Taha, Abd EL Nasser Khallaf. Incidence, Recurrence and Complications after Facial Skin Cancer Excision: Retrospective Analysis of Multi-Institutional Experiences. J Head Neck Spine Surg. 2018; 2(4): 555594. DOI: 10.19080/JHNSS.2018.02.555594
Abstract
Objectives: Skin cancer varies in incidence according to Geography, sun exposure, genetic predilection, skin type and many other factors. Definite treatment of skin cancer requires multidisciplinary approach. Surgery is usually giving a strong hand in skin cancer management regardless to the size of the lesion. This study is designed to evaluate the incidence, recurrence and complications in patients, who had undergone facial skin cancer excision then reconstruction.
Material and Methods: Retro analysis review was conducted for the complications that had happened in patients who were having facial skin cancer and underwent excision then reconstruction. Of 254 cases, 54, 25 and 175 cases were submitted to direct skin closure, skin grafts and local facial flap reconstruction respectively
Results: The total reconstructive surgery complications in this study were in 16 cases of254 (appx. 6.3% of the study). Most of surgical reconstructions are carried out by local facial flaps with good outcomes. Total skin cancer recurrences had been reported in 5 cases (appx. 2.5% of the study).
Conclusion: Incidence of skin cancer in sunny countries like Egypt, where there is a cumulative effect of the sun, moves towards nonmelanoma skin cancer. Local skin cancer recurrence in these series is about 2.4%. Different surgical reconstructive modalities areused, including direct simple closure of the wound, skin grafting and local facial flaps. The commonly used flaps for face reconstruction after excision of skin cancer, in this study, are advancement flaps, naso-labial flaps and forehead flaps with the same survival potentiality.
Keywords: Skin cancer; Reconstruction; Complications; Recurrence
Introduction
The most common facial skin cancers are Melanoma, basal cell carcinoma and squamous cell carcinoma [1,2]. Different incidences are recorded according geographical and genetic factors. Surgery has an important role in treatment of facial cancer [3]. Surgical reconstructive options are usually available and different according to many parameters as the defect size and site, patient general condition and surgeon’s experience caliber.
Materials and Methods
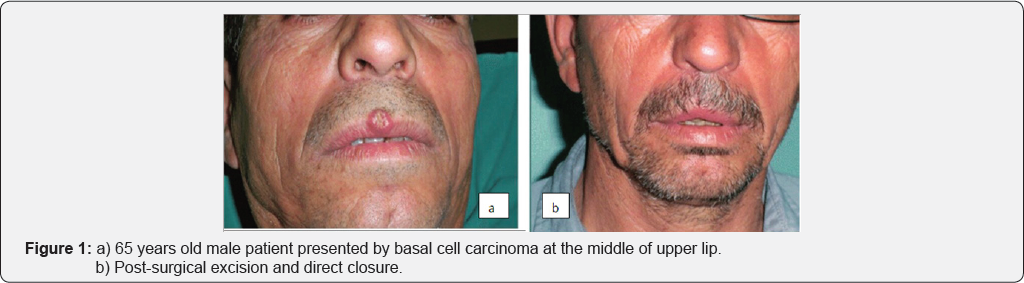
Retro review analysis was conducted for the complications that happened to patients who were having facial skin cancer and underwent excision then reconstruction. The study was included through multi institutional data and analyzed regards surgical complications. 254 patients were included in the study during the period from January 2014-2017. 254 cases were managed by surgical excision and included in the study. Small defects less than 2cm*3cm were closed directly in 54 cases, after lesion excision (Figure 1a & 1b). Larger post-surgical defects were closed by skin grafts (Figure 2a & 2b) or local skin flaps (Figure 3a & 3b) in 25 and 175 case respectively. Flap reconstruction was achieved by one of the three commonly used local facial flaps [3]. Advancement flaps by one of its different patterns, transposition or rotational flaps and Nasolabial flaps were proceeded in 80, 10, 52 case respectively.
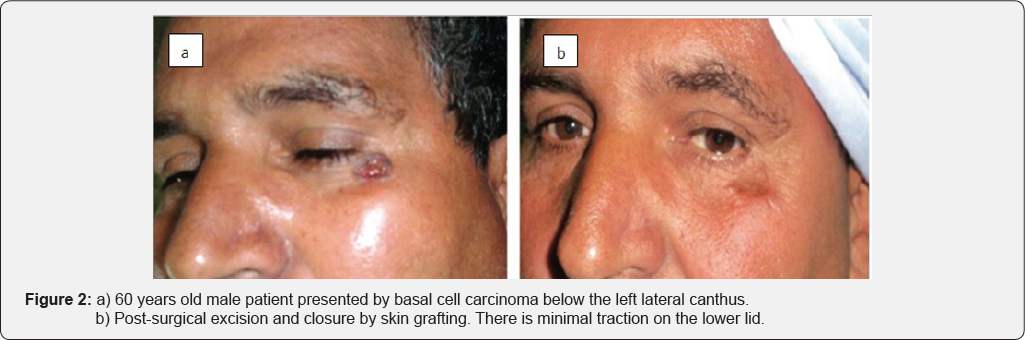
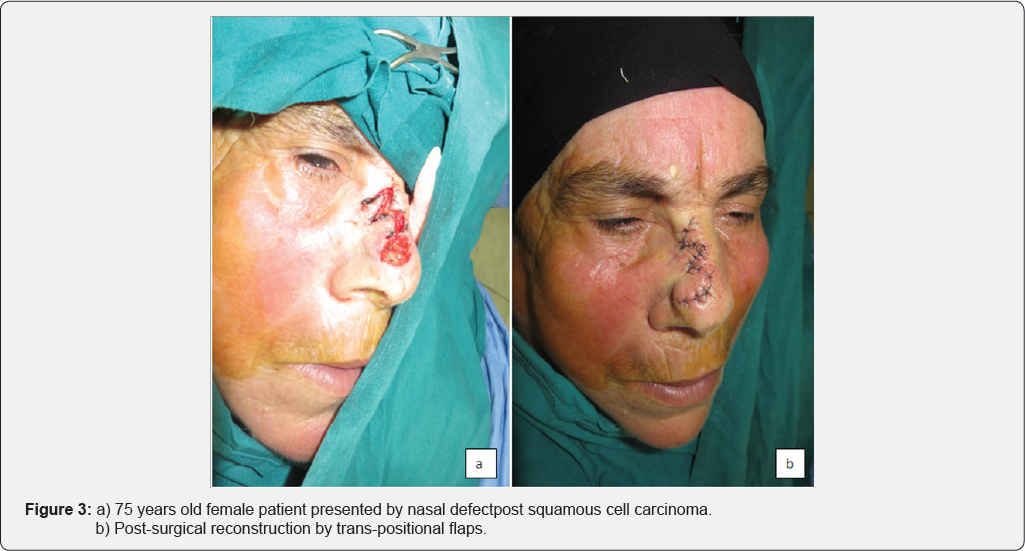
Facial cancer was distributed in different incidence presentations in facial areas; 81 case in the nose, 35 case in upper lip, 19 case in lower lip, 24 case in check inferior and medial to lateral canthus, 21 case inferior and lateral to medial canthus, 23 case at forehead, 14 case at scalp area, 22 case at the mandibular margin and 15 case at pre-auricular area. Sentinel and draining lymph nodes were free by clinical examination and investigations.
Of 254 patients were presented by skin cancer in the face, 205 were due to basal cell origin, 45 were due to squamous cell and other non-melanoma cancers. Only 4 cases of skin cancer in the study were due to melanoma. Average patients' age is ranged from 35-75 with mean age of 55 years. Male patients were 159 and 95 were females, aged from 35-75 year. Multi-centric data were collected from Sayed Galal, Al-Hussein, Nasser Institute and AL-Harm hospitals, Cairo, Egypt. Informed consent for surgery, any possible complications and photography were signed by each patient. Study was approved by my institutional ethical committee.
Results
The total incidence, of reconstructive surgery complications, is 16of 254 (app 6.3%.of the study). The Complications have been varied in different presentations according to type of reconstructive surgery. Of 54 cases were closed directly, 2 cases showed recurrence within two years postoperative. Of 25 cases were reconstructed by skin grafting, one case howed retraction of the lateral canthus with minimal scleral show (Figure 3) and another case has recurrence of squamous cell cancer after 3 months of surgery. Of 175 cases were treated by local facial flap reconstruction, 11 cases were complicated by flap dehiscence. Flap dehiscence underwent in 8 patients, who were reconstructed by advancement flap, 2 were reconstructed by naso-labial flaps and one case was reconstructed by median forehead flap.
Although all flaps have sensationally survived without major wound healing complications, but edge dehiscence has been recorded in 11 cases of 175 have been reconstructed by flaps. Total skin cancer a recurrence was reported in 5 cases (appx 2.5% of the study). Of 5 cases of recurrence, 3 were due to recurrent squamous cell cancer and 2 were due to recurrent basal cell carcinoma. All recurrent cases were re-operated with immediate reconstruction after frozen section biopsy.
Discussion
Surgical closure after facial skin cancer excision is one of the main pillars in the treatment of small sized facial lesions in head and neck. However surgical reconstruction is the first line in treatment of large sized facial skin cancer. In most cases, surgery should be done upon two stages, first one is excision and the second one is reconstruction or wider excision, based on histological clearance about lateral and deep resection margins and sometimes after intraoperative frozen section assessment
[4].
These facts are correlated with this study, when surgery was the mainstay in definite treatment. Large lesion more than 2 cm x 3cm defiantly needs post excision reconstruction. Reports about histological incidence of skin cancer are ranging from 75-80% incidence of non-melanoma skin cancer, according to skin cancer institute in North America and cancer journal respectively [5,6]. In this study the incidence of non-melanoma skin cancer in head and neck is 98.8%. Basal cell carcinoma has 80.7%, while squamous cell carcinoma has 18.1% of the skin cancer incidence in our study, while it is 22% in other worldwide statistics.
According to Cleveland clinic [7] center for continuous education, they state that; new skin cancers will be basal cell origin in about 80%, (BCC), squamous cell carcinoma in 16%, and Melanoma in 4%. This slightly differs from this study report regards BCC and SCC. Although it is higher more than double folds, regards Melanoma incidence.
This could be explained by the predisposing factor; sun exposure, which has been mostly cumulative in non-melanoma skin cancer and has been an acute exposure in melanoma one. So residents of sunny countries, theoretically, where they are cumulatively exposed to sun and more vulnerable for nonmelanoma skin cancer. Contradicted to this peoples who lives in non-sunny countries, when exposed acutely to the sun anywhere, they are at a risk to develop melanoma.
Meticulous surgery, facial units understanding, relaxing skin tension lines and proper choice and design of the flap are important factors in successful reconstruction after tumor excision from the face. Facial flap surgery is an old finding in the Indian civilization [8], and it has been considered an early whispering of reconstructive surgery in modern western literatures. In this study, three types of flaps with their variant designs were used in 175 cases to reconstruct defects after skin cancer excision from the face. Advancement flaps have showed better aesthetic outcome than nasolabial and forehead flaps, although all flaps have showed sensational survival.
This study reported 6.3% total incidence of reconstructive surgery complications. Small defects are usually closed directly if submitted to surgery [9]. Direct skin closure has incidence of 0.5%, while skin grafting has showed 0.25%, but the two options are not applicable for large lesions and when the lesion is present in special areas as medial canthus, lateral canthus, and facial angles and when there is a bone or cartilaginous exposure. Of 175 cases were treated by local facial flap reconstruction, 11 cases were complicated by flap dehiscence. 8 cases were reconstructed by advancement flap, 2 were reconstructed by nasolabial flaps and one case was reconstructed by median forehead flap. Flap complication reported also 6.3% higher than another study; it was 4.6% in Rao JK & Shende KS study [3]. Facial Flaps outcomes were extensively discussed in another author's article [10].
This study has showed the total skin cancer a recurrence is 5 of 254 cases, (appx 2.5% of the total cases) and they were subjected for reconstructive ladder. These results of recurrence are lower than those recorded by Marri, et al. study [11] which is 4.2%. This study is concerning facial skin cancer in face and scalp only, not the deep cancers in head and neck as the study carried out by Raj et al. in 2017 [12].
Recurrence occurred in 5 cases, 3 were due to recurrent squamous cell cancer and 2 were due to recurrent basal cell carcinoma. Aesthetic outcome is more satisfactory when advancement flaps were used.
Conclusion
The incidence of skin cancer in face and scalp, at sunny countries like Egypt, where there is cumulative effect of the sun is higher towards non- melanoma skin cancer. Small skin cancer is easy to be reconstructed after excision either by direct closure, skin graft or local facial flaps. Larger lesions need definite flap reconstruction after excision. The commonly used flaps for face reconstruction after excision of skin cancer, in this study are; advancement flaps, nasolabial flaps and forehead flaps with same survival potentiality. However Aesthetic outcome is more satisfactory when advancement flaps are used. Local skin cancer recurrence in these series is about 2.4%.
References
- Miller DL, Weinstock MA (1994) Non-melanoma skin cancer in the United States: Incidence. J Am Acad Dermatol 30(5): 774-778.
- Kwon KH, Lee DG, Koo SH, Jo MS, Shin H, et al. (2012) Usefulness of V-Y advancement flap for defects after skin tumor excision. Arch Plast Surg 39(6): 619-625.
- Rao JK, Shende KS (2016) Overview of local flaps of the face for reconstruction of cutaneous malignancies: Single institutional experience of seventy cases. J Cutan Aesthet Surg 9(4): 220-225.
- Helmy Y, Taha A, Farahat SE, Yousef M (2014) Frozen Section Biopsy Reliability for Immediate Reconstruction after Tumors Excisionrom the Face. Egypt J Plast Reconstr Surg 38(2): 171-175.
- Lomas A, Leonardi-Bee J, Bath-Hextall F (2012) A systematic review of worldwide incidence of nonmelanoma skin cancer. Br J Dermatol 166(5): 1069-1080.
- (2018) American cancer society statistics.
- Tung R, Vidimos A (2009) Nonmelanoma Skin Cancer
- Correa BJ, Weathers WM, Wolfswinkel EM, Thornton JF (2013) The forehead flap: the gold standard of nasal soft tissue reconstruction. Semin Plast Surg 27(2): 96-103.
- Belmahi A, El Mazouz S, Gharib NE, Bencheikh R, Ouazzani S (2003) The bilobed flap: A very efficient method in aesthetic reconstruction of small skin defects at the alar and tipregions of the nose. Ann Chir Plast Esthet 48(4): 211-215.
- Helmy Y, Taha A, Abd EL-Nasser Khallaf, Abd El-Fattah Al-Sheikh (2017) Survival and aesthetic outcome of local flaps used for reconstruction of face defects after excision of skin malignancies: Multi-institutional experience of 175 cases. International Journal of Current Research in Medical Sciences 3(5-2): 129-137.
- Chren MM, Torres JS, Stuart SE, Bertenthal D, Labrador RJ, et al. (2011) Recurrence after treatment of nonmelanoma skin cancer: a prospective cohort study. Arch Dermatol 147(5): 540-546.
- Nagarkar R, Wagh A, Kokane G, Patil M, Markanday A (2017) Incidence and prognostic factors in distant metastasis from primary head and neck cancer-an institutional experience. J Head Neck Spine Surg J 1(5): 001-004.






























