Parental and Physician Perceptions of Medical Marijuana in the Pediatric Setting
Celina ML Caetano1, Michael W Powell1, Rebecca Clark2, Danielle Chenard3 and Sharon R Smith1,2,3*
1Department of Emergency Medicine, University of Connecticut, USA
2Department of Emergency Medicine, International Children’s Advisory Network, USA
3Department of Emergency Medicine, Connecticut Children’s, USA
Submission:June 14, 2019; Published:July 03, 2019
*Corresponding author:Sharon R Smith, Department of Emergency Medicine, Connecticut Children’s Medical Center, 282 Washington Street, Hartford CT, USA
How to cite this article:Celina ML C, Michael W P, Rebecca C, et al. Parental and Physician Perceptions of Medical Marijuana in the Pediatric Setting. J Complement Med Alt Healthcare. 2019; 9(5): 555772. DOI:10.19080/JCMAH.2019.09.555772
Table of Contents Summary
This is the first survey analyzing both parental and physician perceptions and concerns regarding medical marijuana use in children receiving treatment.
What’s Known on This Subject
Evidence continues to emerge that supports the use of medical marijuana as a therapeutic adjunct. Despite increasing research and acceptance of medical marijuana for adults, a stigma endures surrounding the study and use of medical marijuana in children.
What This Study Adds
This study describes parental and pediatricians’ attitudes and beliefs surrounding medical marijuana use in children. Results demonstrate general acceptance and expand on details that may improve future research on medical marijuana for pediatric patients.
Abstract
Objective: The past decades have seen several political and sociological debates regarding the legalization of medical marijuana as studies discover novel treatment benefits. In the pediatric setting, these discussions involve both parents and physicians. This study sought to identify factors that may influence the parents’ and physicians’ perceptions on medical marijuana use for children; and to determine any stigmas and concerns with its use. Methods: A prospective survey using a 5-point Likert scale was administered using convenience sampling of guardians with children receiving care in the pediatric emergency department, physicians working in the pediatric hospital, and providers attending the 2016 Pediatric Academic Societies Conference. Results: 319 parents and 287 physicians participated in this study. The majority of parents were female (69.3%), white (44.2%) and 35-44 years (34.2%). The majority of physicians were female (57.1%), white (58.5%), and 25-34 years (30.7%). Parents and physicians agreed or somewhat agreed that medical marijuana should be legalized for children, and agreement increased if scientific evidence proved that medical marijuana could relieve symptoms of a condition. More physicians (55.6%) than parents (33.1%) viewed marijuana to be addictive. Both groups agreed that administration of treatment should be as a food product or pill/liquid over inhalation, and the psychological effects of marijuana are more concerning than the physical. Television news programs were the primary source for information regarding medical marijuana. Conclusion: Physicians and parents moderately agree that medical marijuana should be legalized for children receiving treatment and additional factors, such as the media, can influence this perception.
Introduction
The history of marijuana in the United States has been defined by strict regulatory and prohibitory policies. A review of this historical background reveals how political agendas, social apprehension, and scientific misconceptions have been the basis for the continuous regulation of the drug, rather than medical research or clinical trials. Currently, marijuana remains a Schedule I controlled substance, despite the legality for its medical use in 29 states and the District of Columbia [1]. Several prominent medical associations, such as the American Medical Association and American Society of Addiction Medicine, have been hesitant to publicly support the legalization of medical marijuana despite evidence of potential benefits [2]. Such hesitations and the schedule I classification have made it challenging for further research to be conducted. Specifically, the U.S. Drug Enforcement Administration (DEA) and the National Institute on Drug Abuse (NIDA) complicate investigators’ ability to obtain the proper licenses required for marijuana research and commonly denies applications for necessary supplies [3].
The purpose of the current study is to identify important factors that influence parental and pediatricians’ perceptions of medical marijuana for pediatric patients. It is posited that identifying these factors will be the first step in addressing social stigma surrounding pediatric medical marijuana use. This study examines demographic factors, the ways in which parents and pediatricians receive their information about medical marijuana, and their overall acceptance or concerns with the legality of medical marijuana in both adult and pediatric populations. Knowing what is acceptable to parents and pediatricians and any stigma or concerns may assist in changing the current legal and regulatory conditions. Future research efforts are necessary to scientifically evaluate the potential therapeutic risks and benefits of medical marijuana.
Patients and Methods
University undergraduates developed a questionnaire that contained two sections: demographic questions (Appendix A) and perception of medical marijuana questions (Appendix B). In the perception section, parents and physicians were first asked how often they hear about medical marijuana and from what sources they receive most of their information about medical marijuana. Both groups then responded on a 5-point Likert scale (i.e. strongly agree, agree, neutral, disagree, or strongly disagree) to ten statements about the use of medical marijuana. Data is presented as agree (combining strongly agree and agree), neutral, and disagree (combining disagree and strongly disagree) Finally, the groups responded on a second Likert scale to items related to their concern about potential risks or benefits of medical marijuana use. The survey design was approved by the Institutional Review Board (IRB).
The research team first administered the survey to a convenience sample of parents that had a child currently receiving care in the Pediatric Emergency Department (PED) and spoke English. Research assistants explained the purpose of the research and the survey procedure. Subjects were made aware of their rights to abstain or withdraw from the survey and that completion of the questionnaire implied their consent for participation. Data collection for parents began in November 2015 and was completed in April 2016. Data was imported into a Qualtrics database, and the software was used for statistical analysis. Qualtrics is a HIPAA compliant database that allows for real-time updates of completed surveys and automatic transfer of survey responses to a database
English-speaking physicians were administered the survey in one of two manners. The first was through an emailed link to the electronically uploaded survey on the Qualtrics database, an online database service. Qualtrics survey links were emailed to all the pediatricians (residents, fellows and faculty), along with a short cover letter explaining the purpose and aims of the study and disclosing contact information of the study’s authors. Prior to answering survey questions on the Qualtrics platform, pediatricians were prompted with a consent form explaining that their responses would be completely confidential, would not affect their position at the medical center, and there were no risks/benefits attached to the study. An initial email was sent to all physicians at the medical center. The following week(s), the email was resent to increase participation. The physician survey was also administered to an additional population of physicians in attendance at the 2016 Pediatric Academic Society (PAS) Conference in Baltimore, Maryland. The data for this study combined responses from both groups of pediatricians.
Both surveys were written to be neutral with respect to biases regarding medical marijuana. The primary objective of the survey was to assess parents’ and physicians’ current perceptions about medical marijuana. It was not meant to educate parents or physicians about the potential therapeutic benefits of the substance or any potential risks
Results
A total of 319 parents completed the questionnaire. The study population was 69.3% female, 66.5% between the ages of 25 to 44, and 44.2% White/Caucasian, 32.6% Hispanic or Latino, 15.7% Black or African American, 0.9% Asian and 6.6% other. The population was composed of 27.0% college graduates, 22.2% high school graduates (no further education), 21.9% subjects who completed some college, 12.4% trade/vocational school graduates, 8.9% post-graduates, 4.8% subjects having completed some high school, and 2.9% subjects having completed some post-graduate work. Approximately 31.3% of the subjects had children with chronic conditions. The chronic diseases reported included asthma (22.1%), other (7.9%), diabetes (1.9%), cerebral palsy (1.3%), Crohn’s disease (0.9%), sicklecell disease (0.9%), epilepsy (0.6%), cancer (0.3%), multiple sclerosis (0.3%) and Cytophagic histiocytic panniculitis (0.3%). Demographic data for the general population of parents with children receiving care in the PED at our hospital was similar to the subject population of this study. The average decline rate for each survey item was 2.2%. A total of 287 physicians completed the questionnaire. The physician population was 57.1% female, 57.2% between the ages of 25 to 44, and 58.5% White/Caucasian, 9.4% Hispanic or Latino, 2.4% Black or African American, 23.0% Asian and 6.6% other. Physicians surveyed were pediatricians either from Connecticut Children’s Medical Center through the emailed survey, or in attendance at the 2016 Pediatric Academic Society Conference.
Six of the survey items produced statistically significant data upon comparison of physician and parental perception responses. The following summary regards those six items only. A plurality (45.4%) of the physicians supported the legalization of medical marijuana for children, whereas parental support was much more varied, with only 35.6% in support. Medical marijuana delivered via food product or pill/liquid was more acceptable to parents and physicians (both groups with 50% or more support for either category) than inhalation (36.0% and 26.6%, respectively). Additionally, both parents (64.0%) and physicians (72.4%) were more concerned about psychological effects than the physical effects, 59.4% and 62.9% respectively. Most physicians (55.6%) believed marijuana to be addictive, whereas parents do not have consensus (33.1%). Four survey items-questions about legality for adults, consideration of a food product, and concern about physical effects-did not produce statistically significant responses between parents and physicians
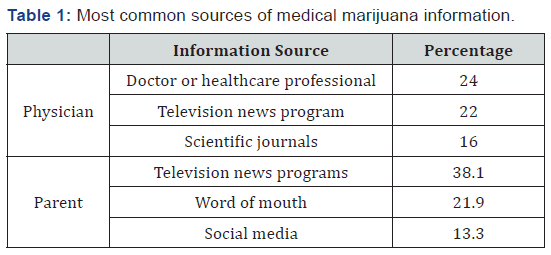
The most prominent source of information regarding medical marijuana used by physicians was doctor or healthcare professional (24.0%), followed by televisions news programs (22.0%) and scientific journals (16.0%). For parents, the most used source for information was television news programs (38.1%), followed by word of mouth (21.9%) and social media (13.3%).
Discussion
This study specifically investigated the influences on parental and physician perceptions about medical marijuana use in pediatrics. The results indicate that both parents and pediatricians accept medical marijuana as a potential therapeutic agent when asked if its use should be legal. However, when repetitioned after saying medical marijuana was scientifically proven to be beneficial, a majority of parents (63.4%) and pediatricians (73.1%) agreed they would consider treating their child or patient with it. This significant difference in responses may be attributed to the exposure an individual has to a situation where a child may need medical marijuana. Anorexia and nausea associated with cancer treatment is a situation where medical marijuana is frequently employed to provide relief. In a recent study, over 90% of pediatric oncologists were willing to treat their patients with medical marijuana if it would be beneficial [4]. Parents may be less likely than a physician to encounter a situation where medical marijuana use in pediatrics is of concern. Thus, a pediatrician may be more likely to witness the outcome of prescribing medical marijuana to a child and could then be more willing to endorse its use when scientifically proven as beneficial.
The concern of the psychological/behavioral effects on children using medical marijuana was high in both groups, and significantly more prominent in pediatricians (72.4%) than parents (64.0%). Several longitudinal and twin studies have demonstrated that marijuana use can impact brain development and neuropsychological functioning when taken as an adolescent, while other studies show no significant cognitive delays accredited to marijuana use [5,6]. It is important to note that much of the published data available detail the benefits and harms of marijuana in children when used recreationally and unsupervised or examine the role of medical marijuana in research reports for the drug’s clinical applications [7-10]. This is a key distinction as medical marijuana is prescribed by a physician and utilized for specific purposes. This lack of a clear conclusion as to the effects of medical marijuana on the cognitive development on children may account for the increased concern for its use in both groups.
In this study, both parents and pediatricians were in agreement that if medical marijuana was to be administered to pediatric patients, it should not be via inhalation, but rather as a food product or in a pill/liquid. The consensus among individuals on the dangers of inhaling fumes may be attributable to the extensive literature on the harms of smoke to the lungs [11,12]. However, this survey did not differentiate between inhaled marijuana from an asthma-type inhaler and from directly smoking it—a difference that could impact participants’ response. Other factors to explain the agreement include the alterations of the hedonic effect after inhalation and the potentiation of it as a gateway drug [13].
This study also reveals a significant difference of opinion in regard to the addictive nature of marijuana. The majority of physicians agreed that marijuana is addictive (55.6%), while parents (33.1%) have less of a consensus. Although several studies have shown marijuana to have addictive properties, its use in the medical setting has proven to tamper the need for administration of other, more addictive, treatment options (such as prescription opioids) [14,15]. A possible explanation for these observations may be due to the source where information regarding medical marijuana is received. This study found that parents (38.1%) are more likely than pediatricians (22.0%) to turn to television news programs for information regarding medical marijuana. An in-depth analysis over the past two decades revealed that the media preferences the negative impact marijuana has (psychotic episodes, hallucinations, incriminations for possession) and neglects to mention the medical uses and benefits. Providing a limited amount of information may skew perceptions of the substance, hindering an unbiased decision for its use in the pediatric medical setting to be made.
Conclusion
Parents and physicians believe that medical marijuana use in pediatrics may benefit the child/patient receiving care but share differences of opinion in the psychological implications and modes of administration. As well, parents and physicians turn to television news outlets for information on medical marijuana, highlighting the role that the media can have on future sociological and political opinion. Future research looking at the potential of television news programs over other information sources to manipulate one’s opinion regarding medical marijuana in pediatrics would provide further knowledge on the issue.
Acknowledgement
We would like to thank the Undergraduate Research Assistance Program and the students for their assistance and support of this survey
Conflict of Interest
The authors have no conflicts of interest relevant to this article to disclose
References
- Wang GS, Hoyte C, Roosevelt G, Heard K (2019) The Continued Impact of Marijuana Legalization on Unintentional Pediatric Exposures in Colorado. Clin Pediatr (Phila) 58(1): 114-116.
- Wilkinson ST, Yarnell S, Radhakrishnan R, Ball SA, D’Souza DC (2016) Marijuana Legalization: Impact on Physicians and Public Health. Annu Rev Med 67: 453-466.
- Cohen PJ (2010) Medical Marijuana 2010: It’s Time to Fix the Regulatory Vacuum. J Law Med Ethics 38(3): 654-666.
- Ananth P, Ma C, Al Sayegh H (2018) Provider Perspectives on Use of Medical Marijuana in Children with Cancer. Pediatrics 141(1): e20170559.
- Meier MH, Caspi A, Ambler A (2012) Persistent cannabis users show neuropsychological decline from childhood to midlife. Proc Natl Acad Sci USA 109(40): E2657- E2664.
- Jackson NJ, Isen JD, Khoddam R (2016) Impact of adolescent marijuana use on intelligence: Results from two longitudinal twin studies. Proc Natl Acad Sci USA 113(5): E500-E508.
- https://medicalmarijuana.procon.org/
- Kim H, Kim SH (2018) Framing marijuana: How U.S. newspapers frame marijuana legalization stories (1995-2014). Prev Med reports 11: 196-201.
- Primack BA, Kraemer KL, Fine MJ, Dalton MA (2009) Media Exposure and Marijuana and Alcohol Use Among Adolescents. Subst Use Misuse 44(5): 722-739.
- Mc Ginty EE, Samples H, Bandara SN, Saloner B, Bachhuber MA, et al. (2016) The emerging public discourse on state legalization of marijuana for recreational use in the US: Analysis of news media coverage, 2010-2014. Prev Med (Baltim) 90: 114-120.
- Moir D, Rickert WS, Levasseur G (2008) A Comparison of Mainstream and Sidestream Marijuana and Tobacco Cigarette Smoke Produced under Two Machine Smoking Conditions. Chem Res Toxicol 21(2): 494-502.
- Department of Health U, Services H, for Disease Control C, Center for Chronic Disease Prevention N, Promotion H, on Smoking O. Executive Summary (The Health Consequences of Smoking-50 Years of Progress: A Report of the Surgeon General).
- Should Medical Cannabis Administered by Inhalation Be Allowed for Hospitalized Patients? Can J Hosp Pharm 71(3): 211-214.
- Hasin DS, Saha TD, Kerridge BT (2015) Prevalence of Marijuana Use Disorders in the United States Between 2001-2002 and 2012-2013. JAMA psychiatry 72(12): 1235-1242.
- Bruce D, Brady JP, Foster E, Shattell M (2018) Preferences for Medical Marijuana over Prescription Medications Among Persons Living with Chronic Conditions: Alternative, Complementary, and Tapering Uses. J Altern Complement Med 24(2): 146-153.






























