Abstract
Background: The complexity and increasing cost of health care creates challenges for hospitals to provide access to care [1-3]. Providing Mississippi with access to surgical care at the University of Mississippi Medical Center (UMMC) is vital. Due to the limited number of operating rooms (ORs), UMMC surgeons were unable to provide adequate access to surgical services for their patients. Due to the cost and time to build new ORs at UMMC, a surgical collaboration with a local, private community-based hospital, Merit Health Madison, offered a potentially viable option.
Methods: This mixed-methods study aimed to determine if the UMMC surgical collaboration with Merit Health Madison impacted the volume of
surgical services at both locations. Surgeons’ perceptions regarding the collaboration were also explored.
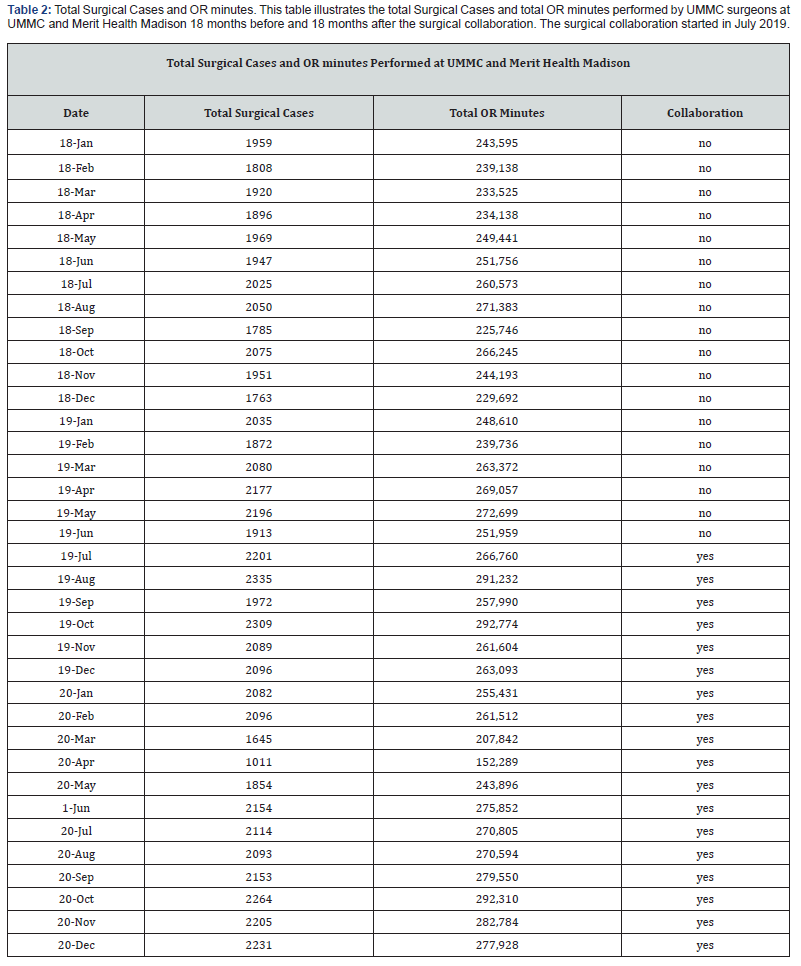
Results: The results indicated that UMMC surgeons were able to increase access to surgical services by performing 82 more monthly surgical
cases and having access to 23,198 more monthly OR minutes through this surgical collaboration. The study provided the qualitative categories of
convoluted access, collaborative felicity, and corroborated opportunities through the engaged participants’ semi-structured interviews.
Conclusion: This study showed that a surgical collaboration with Merit Health Madison improved UMMC surgeons’ ability to provide access to
surgical services. The results of this study suggest a viable path forward to increase access to surgical services through a surgical collaboration.
This study could serve as a guide for other academic medical centers considering potential surgical collaborations.
Keywords:Surgical Collaboration; Neurosurgery; Potential Solution; Surgeons’ Perceptions
Abbreviations:UMMC: University of Mississippi Medical Center; ORs: Operating Rooms; CBOs: Community-Based Organizations
Background
The rising complexity and cost of health care pose significant challenges for hospitals in providing accessible care [1-3]. Globally, five billion people lack access to affordable and safe surgical services [4]. Hospitals face the challenge of ensuring safe, affordable care through patient care coordination and collaborations with community-based organizations (CBOs) [5]. CBOs, defined as private, public, or nonprofit entities meeting community health needs, enhance care access and support research [6]. CBOs bridge researchers and communities through disseminating findings to improve outcomes and reduce disparities [7,8]. Collaboration lacks a universal definition, often causing confusion [9]. It involves social entities engaging in joint activities for mutual goals [9]. Cross-sector collaborations between public and private organizations address health determinants and disparities [10,11]. Effective collaboration requires coordinated knowledge sharing, especially in specialized fields, to achieve desired outcomes [12,13]. Collaborations with academic medical centers offer benefits like improved patient care coordination but face challenges [14].
The University of Mississippi Medical Center (UMMC), with
31 operating rooms (ORs) across its Jackson campus, faced
surgical capacity constraints. The State of Mississippi Health Care
Collaboration Act of 2017 allowed UMMC to form a collaboration
with Merit Health Madison in 2019, which leveraged underutilized
ORs at Merit Health [15]. Care coordination at this level can be
complex [16]. This surgical collaboration would require robust
patient care coordination. UMMC’s limited ORs restricted surgical
case volume, hindering patient access. Collaboration with Merit
Health Madison offered a potential solution. This mixed-methods
study evaluated the UMMC-Merit Health Madison collaboration’s
impact on surgical volume and explored surgeons’ perceptions.
The study aimed to answer the following questions:
a) Did the collaboration increase total surgical cases for
UMMC at both locations 18 months post-collaboration?
b) Did it increase total OR minutes for UMMC at both
locations 18 months post-collaboration?
c) What are UMMC surgeons’ perceptions of the
collaboration?
Methods
This mixed-methods study aimed to determine if the University of Mississippi Medical Center (UMMC) surgical collaboration with Merit Health Madison impacted the volume of surgical services at both locations. Surgeons’ perceptions regarding the collaboration were also explored.
Research Design
This explanatory sequential mixed-methods study, from January 2018 to December 2020, examined surgical case volume and explored the perceptions of eligible UMMC surgeons. The explanatory sequential mixed-methods study was selected to first collect phase one quantitative data and then collect phase two qualitative data to help explain the quantitative results [17].
Setting
University of Mississippi Medical Center’s main campus in
Jackson, Mississippi, is the state’s only academic medical center
and level one trauma center. The hospital was founded in 1955
and comprises 722 beds. The University of Mississippi Medical
Center’s main campus consists of three different hospitals
connected and located on the same campus. The three different
hospitals and corresponding number of operating rooms (ORs) at
UMMC are as follows:
I. Adult Hospital - 15 complex operating rooms (ORs) and
six ambulatory ORs
II. Sanderson Children’s Hospital - seven ORs
III. Winfred L. Wiser Hospital for Women and Infants – three
Ors
In 2019, UMMC performed 39,298 surgical procedures in all ORs. The adult hospital performed 29,905 surgical cases, Winfred L. Wiser Hospital for Women and Infants performed 1,646, and Children’s Hospital performed 7,747. Merit Health Madison is part of the Merit Health Network, which contains 10 hospitals. Merit Health Madison is a local, private, community-based hospital located in the suburb of Canton, Mississippi. Merit Health Madison is located 22 miles north of UMMC’s main campus in Jackson, MS. The 113,000 square foot hospital began serving Madison County in 2011 and is the county’s only hospital. Merit Health Madison has four ORs and one procedure room.
Participants and Sampling Methods
The target participants for this study were the UMMC surgeons who participated in the surgical collaboration with Merit Health Madison. University of Mississippi Medical Center surgeons who participated in the surgical collaboration include the specialties and sub-specialties of general, plastics, transplant, orthopedics, neurosurgery, and ear, nose, and throat. The researcher used a purposive sample, which included all UMMC surgeons who had performed surgical procedures at Merit Health Madison through the surgical collaboration. Targeted participants were invited to participate in the study utilizing a two-tier approach. Tier one participants were the UMMC surgeons who primarily performed surgeries at Merit Health Madison. Tier two participants were the UMMC surgeons who performed surgeries at Merit Health Madison, but less consistently.
Data Collection
Data collection took place in three phases:
a. In phase one, the researcher emailed the Chief
Perioperative Physician at UMMC requesting access to the
quantitative data regarding total surgical cases and total operating
room minutes.
b. In phase two, data collection involved in-depth
qualitative interviews to help explain phase one quantitative data
results. The researcher emailed the Chief Perioperative Physician
seeking permission to interview the eligible UMMC surgeons in a
two-tiered system. Also, the researcher requested a list of those
surgeons ‘ names and email addresses. After receiving permission
and the list of eligible surgeons, the researcher emailed the tier
one eligible surgeons requesting their participation in the study.
In phase three, the researcher emailed the Ambulatory Operations Director (AOD) requesting participation in the study.
Instrument Development
The semi-structured interview guide was developed and adopted by the researcher, as shown in (Table 1). For clarity, the interview guide contained seven open-ended questions, and the interview guide was used in pilot interviews with a small group of non-eligible UMMC surgeons. After pilot interviews, the interview guide combined two questions into one question based on feedback. Therefore, the final interview guide contained six open-ended questions. Each primary open-ended question was followed by prompts, and the responses of the participants guided further questioning.

Data Analysis
After completing phase one quantitative data collection, the researcher analyzed the data using IBM SPSS 26.0 statistics software. The researcher used an independent t-test to create a monthly comparison of the total surgical cases 18 months before and 18 months after the surgical collaboration. Also, the researcher used an independent t-test to create a monthly comparison of the total operating room minutes 18 months before and 18 months after the surgical collaboration. The level of significance was set at 0.05. P-value < 0.05 from the independent t-test indicated a significant difference between the total surgical cases and total operating room minutes before and after the collaboration. Within the independent t-test, Levene’s test was utilized. After completion of phase two qualitative data collection, the researcher used grounded theory to analyze the data. To analyze the qualitative data using grounded theory, an open coding process was conducted first to create concepts of the qualitative data set. Each participant interview transcript was reviewed line by line and coded by the researcher and a peer coder to represent the concept expressed by the participant. The codes were then organized into concept groups to allow the comparison process to become more manageable. The code concepts were then organized into categories. After open coding, the researcher utilized axial coding. Lastly, the researcher utilized selective coding. When the codes no longer produced any new categories, the data were considered saturated 17. After completion of phase three qualitative data collection, the interview with the AOD added depth since the AOD’s response was presented from an administrative standpoint. The findings of phase three were incorporated with established categories from phase two.
Ethical Considerations
The raw qualitative interviews and quantitative data collected remain confidential and will not be shared. Each participant’s interview transcripts were de-identified. Informed consent provided the study participants a thorough explanation of the study, the purpose of the study, potential risks and benefits, a guarantee of anonymity, selection of participants, and the right to participate or withdraw at any time.
Qualitative Findings
Three categories emerged: convoluted access, collaborative felicity, and corroborated opportunities. Convoluted access referred to how the participants generally perceived the ability to access surgical services in Mississippi. Some participants noted that in certain regions of the state, there might be adequate access to surgical services. Some participants asserted that the vast majority of the state had limited access to surgical services. Collaborative Felicity referred to how the participants perceived the surgical collaboration between UMMC and Merit Health Madison. All participants shared a common perception that the surgical collaboration between UMMC and Merit Health Madison was helpful. Also, all participants noted the collaboration to be beneficial. Corroborated Opportunities referred to participant perceptions regarding circumstances they encountered while operating in the surgical collaboration. The participants believed these shared perceptions of common circumstances could maintain and bolster future surgical collaborations. Corroborated Opportunities was broken down into two sub-categories: favorable facility findings and executive emendations. Favorable facility findings were patients having more surgical access, increased training opportunities for residents, and flexibility for surgeons through the introduction of additional ORs. Executive emendations were proposals that the surgeons felt hospital administrations could utilize to improve future collaborations. The executive emendations were that surgeons should be involved in the pre-collaboration stage to determine which surgical services would be involved in the collaboration, ensure the appropriate surgical equipment was available, and ensure ancillary services were available for the surgeries performed.
Discussion
The literature regarding surgical collaborations among health care facilities was lacking. This study brought forth initial research to fill the gap in the field of surgical collaboration among health care facilities. While this study revealed the perceptions of the engaged participants 18 months after the collaboration, future research should investigate the engaged participants’ perceptions at interval periods before the collaboration and throughout the collaboration. Future research should also investigate the financial perspective of increasing access to surgical services through a surgical collaboration.
Limitations of the Study
Limitations of this study were time constraints and access to data. First, the researcher was limited in the time frame in which the study was conducted. The researcher was limited in measuring change over a period of time of the UMMC surgeons’ perceptions participating in the surgical collaboration with Merit Health Madison. While the intentions of the researcher were to explore the perceptions of participants engaging in the surgical collaboration, the researcher cannot uphold that the participants’ perspectives did not change from the start of the collaboration to the time in which the researcher conducted the semi-structured interviews. Next, the researcher was limited in access to data of the surgical collaboration. The financial data relating to the surgical collaboration between UMMC and Merit Health Madison were considered in the study, but financial data were not readily accessible during the study’s time constraints.
Conclusion
This study investigated a surgical collaboration between an academic medical center and a local, private, community-based hospital. The study provided the quantitative results regarding total surgical cases and total OR minutes 18 months before and 18 months after a surgical collaboration. The study also provided the perceptions of UMMC surgeons participating in the surgical collaboration with Merit Health Madison. The results indicated that UMMC surgeons were able to increase access to surgical services through a surgical collaboration. The study provided a mean difference of 82 monthly surgical cases between pre-and post-collaboration. The study provided a mean difference of 23,198 total monthly OR minutes between pre-and post-collaboration. The study provided the qualitative categories of convoluted access, collaborative felicity, and corroborated opportunities through the engaged participants’ semi-structured interviews. The results of this study suggest a viable path forward to increase access to surgical services through a surgical collaboration. Finally, this study could serve as a guide for other academic medical centers considering potential surgical collaborations.
References
- Block DJ (2014) Revisiting the triple aim-Are we any closer to integrated health care? Physician Exec 40(1): 40-43.
- Shahly V, Kessler RC, Duncan I (2014) Worksite primary care clinics: A systematic review. Popul Health Manag 17(5): 306-315.
- Fox K, McCorkle R (2018) An employee-centered care model responds to the triple aim: Improving employee health. Workplace Health Saf 66(8): 373-383.
- Griswold DP, Makoka MH, Gunn WA, Johnson WD (2018) Essential surgery as a key component of primary health care: Reflections on the 40th anniversary of alma-ata. BMJ Glob Health 3(suppl 3): e000705.
- Bhatt J, Bathija P (2018) Ensuring access to quality health care in vulnerable communities. Acad Med 93(9): 1271-1275.
- Caldwell WB, Reyes AG, Rowe Z, Weinert J, Israel BA, et al. (2015) Community partner perspectives on benefits, challenges, facilitating factors, and lessons learned from community-based participatory research partnerships in Detroit. Prog Community Health Partnersh 9(2): 299-311.
- Adebayo OW, Salerno JP, Francillon V, Williams JR, et al. (2018) A systematic review of components of community-based organisation engagement. Health Soc Care Community 26(4): 474-484.
- Blakeney N, Michaels M, Green M (2015) Collaborative development of clinical trials education programs for African American community-based organizations. J Cancer Educ 30(2): 400-406.
- Bedwell WL, Wildman JL, DiazGranados D, Salazar M, Kramer WS, et al. (2012) Collaboration at work: An integrative multilevel conceptualization. Hum Resource Manag Rev 22: 128-145.
- Tung EL, Gunter KE, Bergeron NQ, Lindau ST, Chin MH, et al. (2018) Cross-Sector collaboration in the high-poverty setting: Qualitative results from a community-based diabetes intervention. Health Serv Res 53(5): 3416-3436.
- McCullough JM, Eisen-Cohen E, Lott B (2020) Barriers and facilitators to intraorganizational collaboration in public health: Relational coordination across public health services targeting individuals and populations. Health Care Manag Rev 45(1): 60-72.
- Hu L, Randel AE (2014) Knowledge sharing in teams: Social capital, extrinsic incentives, and team innovation. Group Organ Manag 39(2): 213-243.
- Berends H, Sydow J (2019) Process views on inter-organizational collaborations. Res Sociol Organ 64: 1-10.
- Ayers C, Arch J (2013) VA-Academic partnerships: challenges and rewards for new VA mental health investigators. J Ment Health 49(6): 709-713.
- (2017) Health Care Collaboration Act, Miss Code Ann 83-41-398.
- Izumi S, Barfield PA, Basin B (2018) Care coordination: Identifying and connecting the most appropriate care to the patients. Res Nurs Health 41(1): 49-56.
- Creswell JW, Creswell JD (2018) Research Design: Qualitative, quantitative, and mixed methods approach.






























